For Healthcare Costs, Geography is Destiny
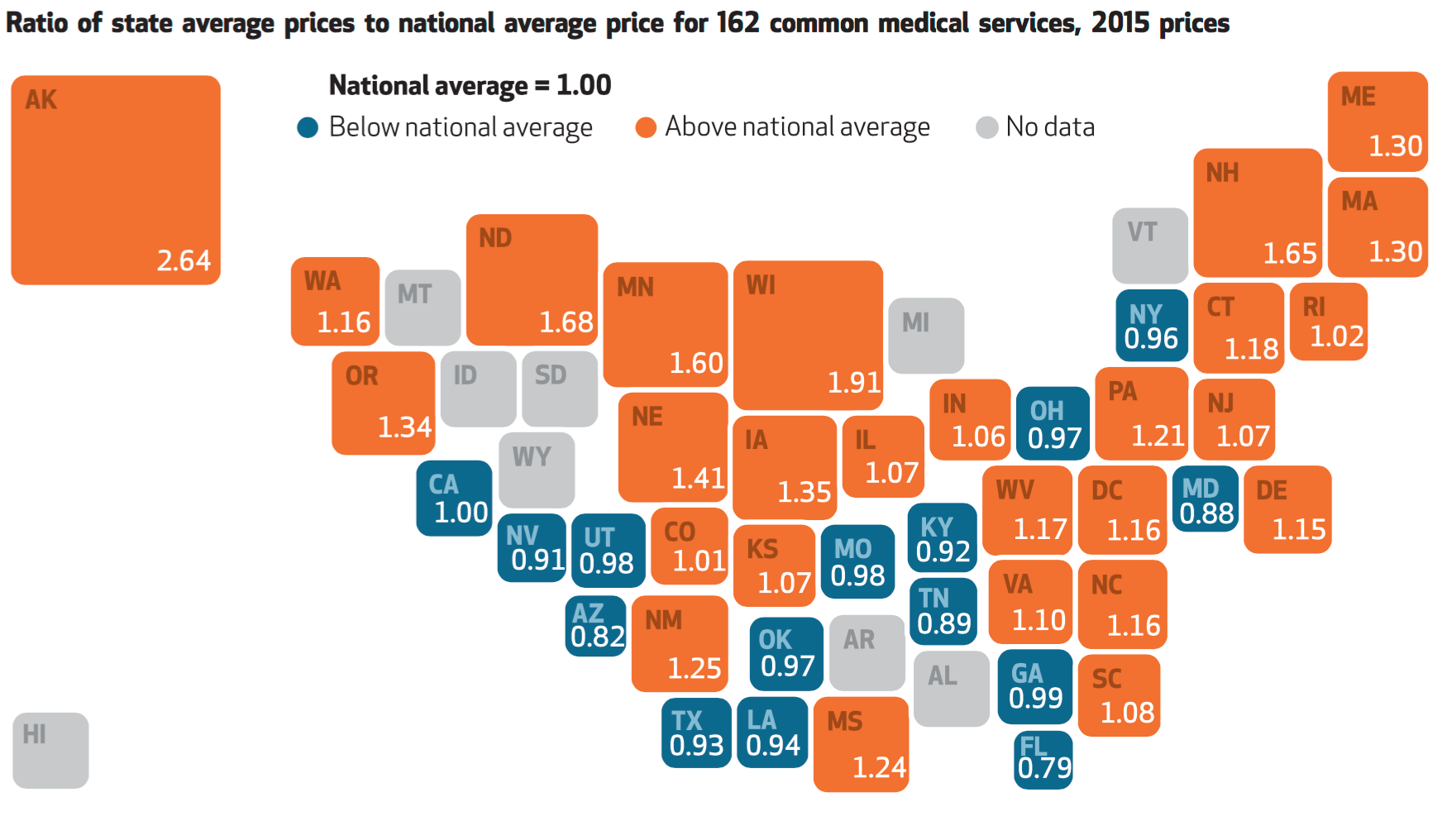
Where you live in America determines what you might pay for healthcare. In this health economic scenario, as Napoleon is rumored to have said, “geography is destiny.” If you’re searching for low-cost health care, Ohio may just be your state of choice. The map illustrates these health care disparities across the U.S. in 2015, when the price of a single service could vary by more than 200% between one state and another: say, Alaska versus Arizona, or Wisconsin compared to Florida. Even within states, like Ohio, the average price of a pregnancy ultrasound in Cleveland ran nearly three times that received in
Withings Inside: Nokia’s Digital Health Vision
The first health news I read this morning in my Google Alerts was a press release explaining that Nokia planned to acquire Withings for EU170 (about $190mm). As an early adopter and devoted user of the Withings Smart Body Analyzer, I took this news quite personally. “What will Nokia be doing with my beloved Withings?” I asked myself via Twitter early this morning. As if on cue, a public relations pro with whom I’ve been collegial for many years contacted me to see if I’d like to talk with the Founder and CEO of Withings, Cédric Hutchings, and Ramzi Haidamus,
Digital Health Update from Silicon Valley Bank

Who better than a financial services institution based in Silicon Valley to assess the state of digital health? Few organizations are better situated, geographically and sector-wise, than SVB Analytics, a division of Silicon Valley Bank based in, yes, Silicon Valley (Santa Clara, to pinpoint). The group’s report, Digital Health: Opportunities for Advancing Healthcare, provides an up-to-date landscape on the convergence of healthcare and technology. SVB Analytics defines digital health as “solutions that use digital technology to improve patients’ health outcomes and/or reduce the cost of healthcare.” The report provides context for the digital health market in terms of health care costs,
Control Drug Costs and Regulate Pharma, Most Older Americans Say
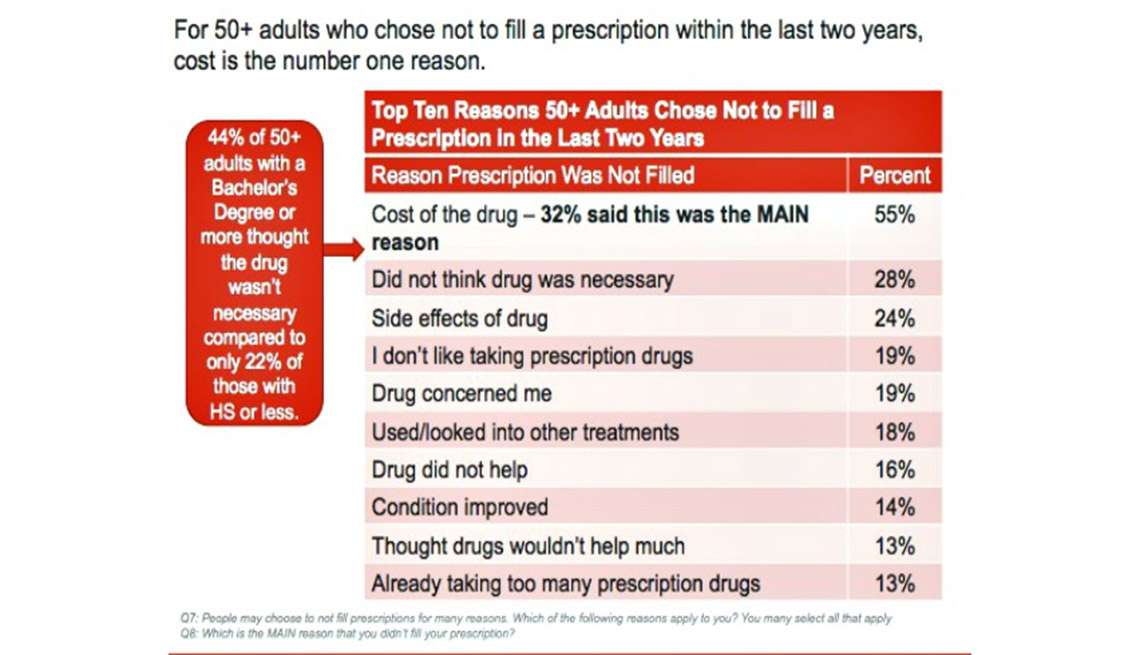
The top reason people in America over 50 don’t fill a prescription is the cost of the drug, according to the AARP 2015 Survey on Prescription Drugs. Eight in 10 people 50+ think the cost of prescription drugs is too high, and 4 in 10 are concerned about their ability to afford their medications. Thus, nearly all people over 50 think it’s important for politicians (especially presidential candidates) to control Rx drug costs. Older consumers are connecting dots between the cost of their medications and direct-to-consumer prescription drug advertising: 88% of the 50+ population who have seen or heard drug
Money, Stress and Health: The American Worker’s Trifecta
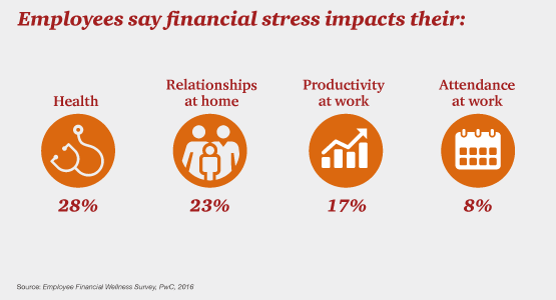
Financial stress impacts health, relationships, and work productivity and attendance for employees in the U.S. It’s the American worker’s trifecta, a way of life for a growing proportion of people in the U.S. PwC’s 2016 Employee Financial Wellness Survey for 2016 illustrates the reality of fiscally-challenged working women and men that’s a national epidemic. Some of the signs of the financial un-wellness malaise are that, in 2016: 40% of employees find it difficult to meet their household expenses on time each month 51% of employees consistently carry balances on their credit cards (with a large increase here among Baby Boomers
The Hospital of the Future Won’t Be a Hospital At All
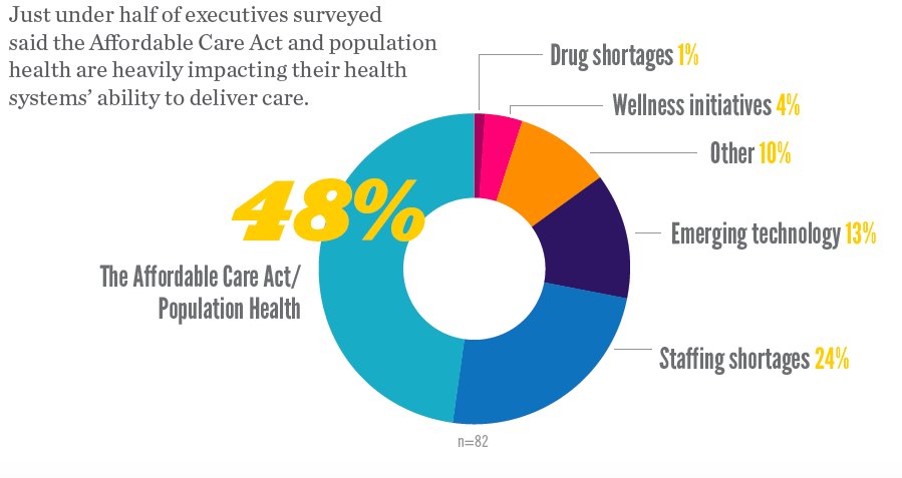
In the future, a hospital won’t be a hospital at all, according to 9 in 10 hospital executives who occupy the c-suite polled in Premier’s Spring 2016 Economic Outlook. Among factors impacting their ability to deliver health care, population health and the ACA were the top concerns among one-half of hospital executives. 1 in 4 hospital CxOs think that staffing shortages have the biggest impact on care delivery, and 13% see emerging tech heavily impacting care delivery. Technology is the top area of capital investment planned over the next 12 months, noted by 84% of hospital execs in the survey.
Financial Wellness Declines In US, Even As Economy Improves
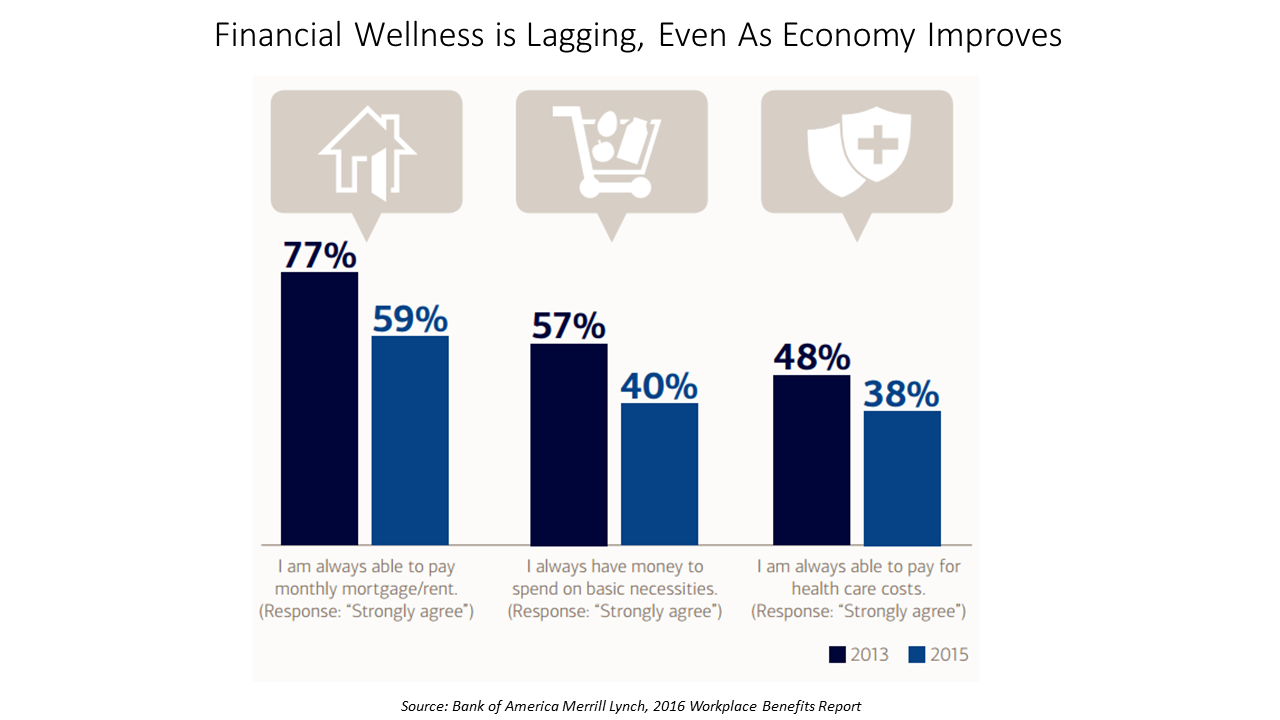
American workers are feeling financial stress and uncertainty, struggling with health care costs, and seeking support for managing finances. 75% of employees feel financially insecure, with 60% feeling stressed about their financial situation, according to the 2016 Workplace Benefits Report, based on consumer research conducted by Bank of America Merrill Lynch. The overall feeling of financial wellness fell between 2013 and 2015. 75% of U.S. workers don’t feel secure (34% “not very secure” and 41% “not at all secure”), with the proportion of workers identifying as “not at all secure” growing from 31% to 41%. Financial wellness was defined for this
Expect Double-Digit Rx Cost Growth to 2020 – Implications for Oncology
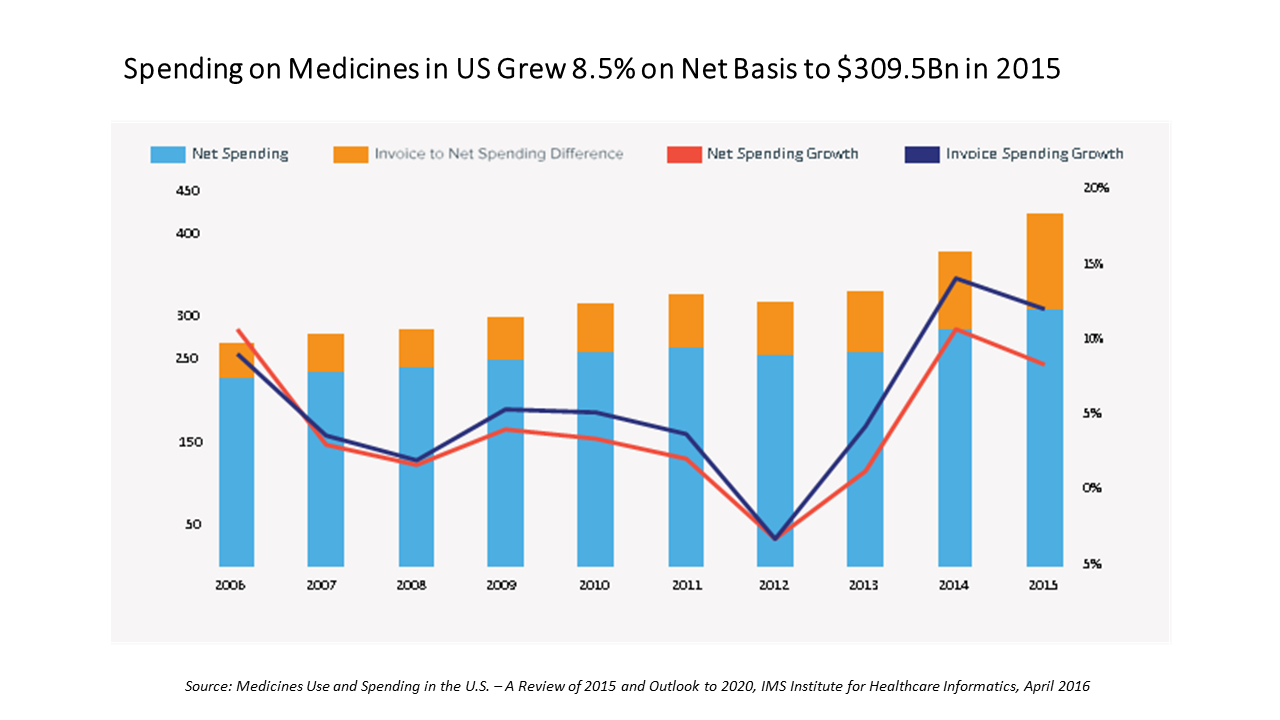
In the U.S., spending on prescription medicines reached $425 bn in 2015, a 12% increase over 2014. For context, that Rx spending comprised about 14% of the American healthcare spend (based on roughly $3 trillion reported in the National Health Expenditure Accounts in 2014). We can expect double-digit prescription drug cost growth over the next five years, according to forecasts in Medicines Use and Spending in the U.S. – A Review of 2015 and Outlook to 2020 from IMS Institute of Healthcare Informatics. The biggest cost growth driver is specialty medicines, which accounted for $151 bn of the total Rx spend
Digitizing Self-Healthcare with Google, Pfizer, Under Armour, Walgreens and WebMD
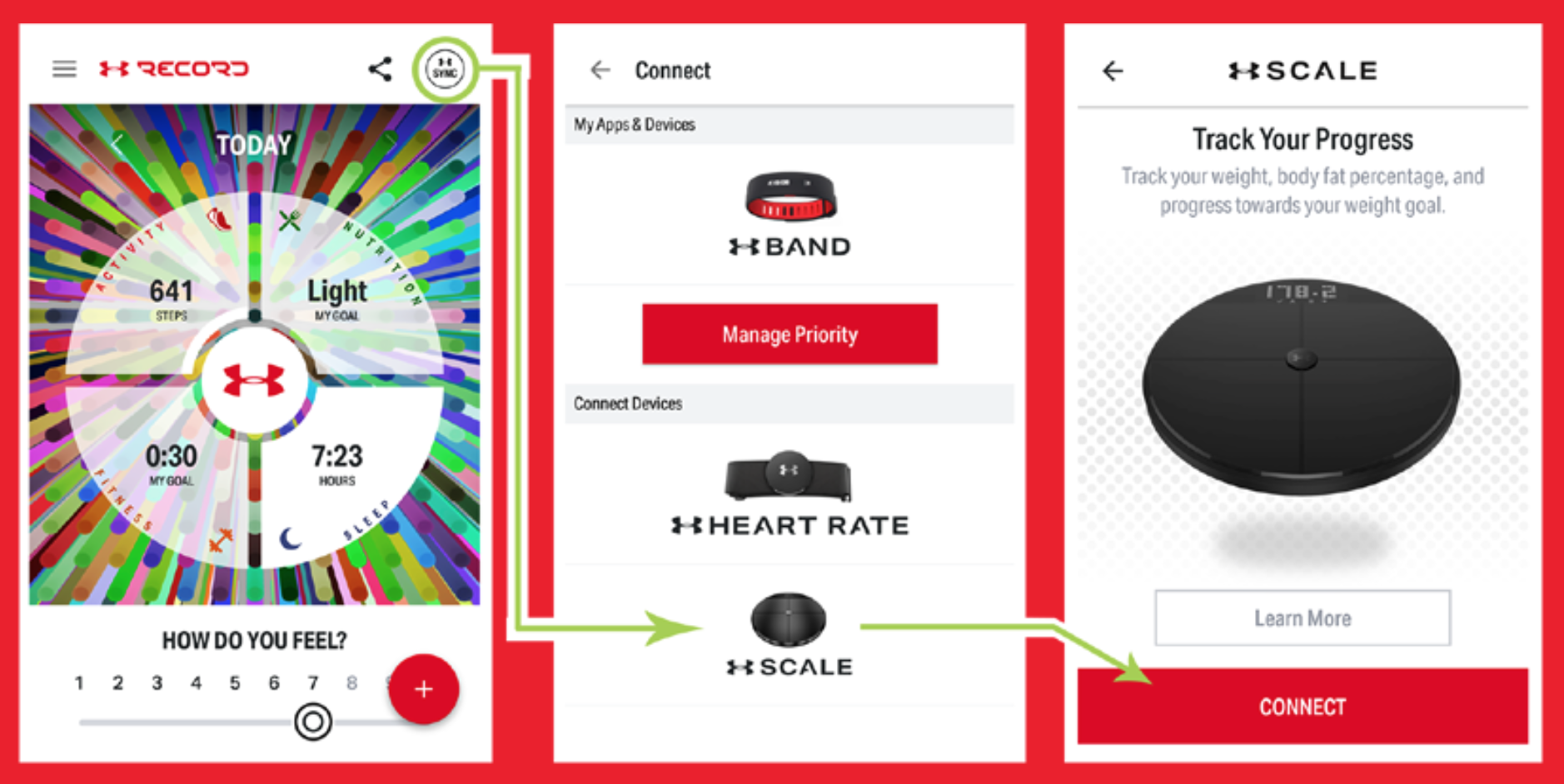
How can digital technologies enable self-healthcare in novel ways? This was the theme of a meeting sponsored by Pfizer Consumer Healthcare and hosted by Google, with the title, “Advancing Consumer Health through New Technology and Next Generation OTC Healthcare” held on 12th April 2016 at Google offices in Manhattan’s Chelsea neighborhood. Pharmaceutical brand drugs switching to over-the-counter packaged goods, the Cellscope Otoscope used by parents checking their young children’s earaches, connected shoes and earbuds for athletic enhancement, and omni-channel retail shopping….these are a few of the signals we see emerging to enable consumers’ to drive healthy behaviors, wellness and self-healthcare. Speakers
Generation Gaps in Health Benefit Engagement

Older workers and retirees in the U.S. are most pleased with their healthcare experiences and have the fewest problems accessing services and benefits. But, “younger workers [are] least comfortable navigating U.S. healthcare system,” which is the title of a press release summarizing results of a survey conducted among 1,536 U.S. adults by the Harris Poll for Accolade in September 2015. Results of this Accolade Consumer Healthcare Experience Index poll were published on April 12, 2016. Accolade, a healthcare concierge company serving employers, insurers and health systems, studied the experiences of people covered by health insurance to learn about the differences across age
Paper and Fax, Not EHRs or Portals, Are Popular for Health Data Sharing
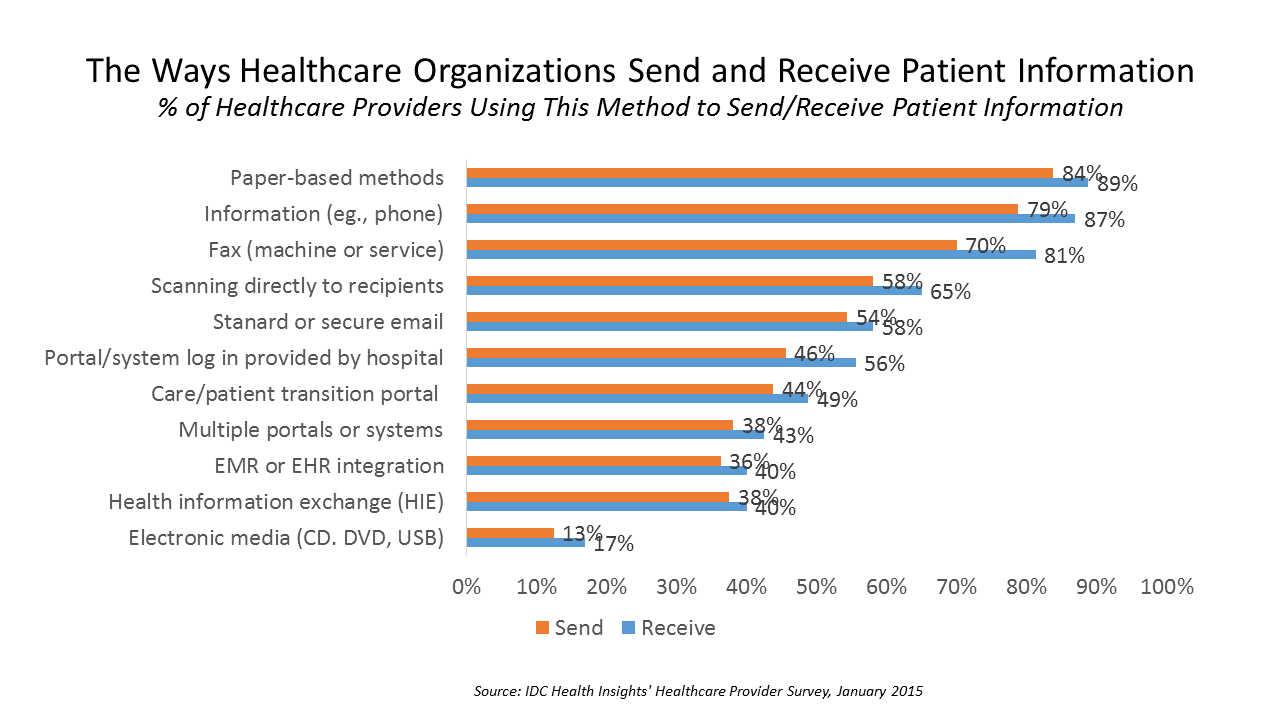
Faxing in health care ranks higher in patient data information sharing than using secure email, online portals, health information exchange (HIE), or leveraging electronic health records. Welcome to the American healthcare system in 2016, as described in a market spotlight published by IDC, The Rocky Road to Information Sharing in the Health System. IDC’s survey research among healthcare providers forecasts the “rocky road” to information sharing. That rocky road is built for medical errors, duplication of services, greater healthcare costs, and continued health il-literacy for many patients. “The holy grail of interoperability — lower-cost, better-quality care with an improved experience for
Patient Engagement – Secret In The Healthcare Sauce

Patient engagement is the new imperative in health care, writes Editor-in-chief Alan Weil in his introduction to the April 2016 issue of Health Affairs. It is appropriate and right that Judith Hibbard of the University of Oregon served as the theme adviser for the issue: she’s the innovator of the Patient Activation Measure and has frequently published her research in Health Affairs. Her own bottom-line: that the higher the patient activation, the less health care costs the health plan. (See a recent post on her research here on Health Populi). This issue of Health Affairs is a comprehensive primer on the
It’s World Health Day: Stay Super, Act Local

April 7 is World Health Day, and the World Health Organization (WHO) has named #diabetes the big public health challenge for 2016. What’s striking about this year’s World Health Day is the “Stay Super” public health ad campaign that WHO has developed featuring figures of super-people. THINK: Superman and Wonderwoman meet Doctors Welby, Kildare, and McDreamy. I’ve included several of the posters in the blog today to show how engaging health messaging works well when it works. The materials can be downloaded at this link. This week also saw the publication of America’s Health Rankings, spotlighting the impact of unhealthy behaviors.
Healthcare Vs New Entrants: A $1.5 T Problem
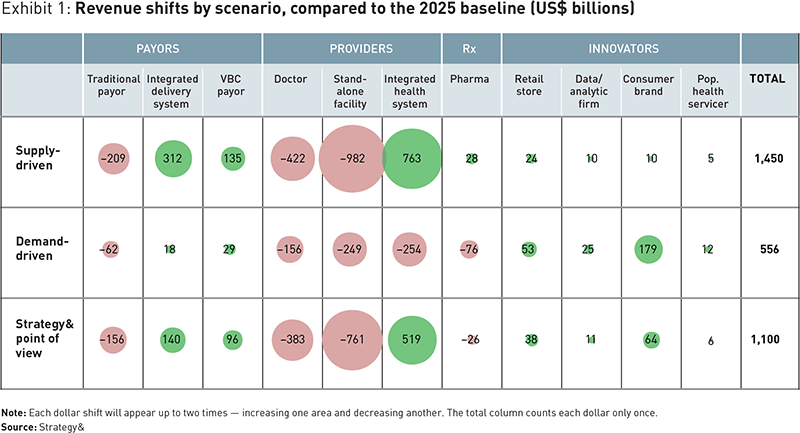
There’s an annual $1.5 trillion in revenues for the legacy healthcare system at stake by 2025, at risk of transferring to new entrants keen to please consumers, streamline physician practices, and provide new-new health insurance plans. A team from PwC has characterized this challenge in their strategy+business article, The Coming $1.5 Trillion Shift in Healthcare. Based on their survey of healthcare industry stakeholders and analyzing their economic model, the PwC team developed three scenarios about the 2025 healthcare market in the U.S. These are supply-driven, demand-driven, and equilibrium. The exhibit details each of these possible futures across various industry stakeholder
Cost Comes Before “My Doctor” In Picking Health Insurance
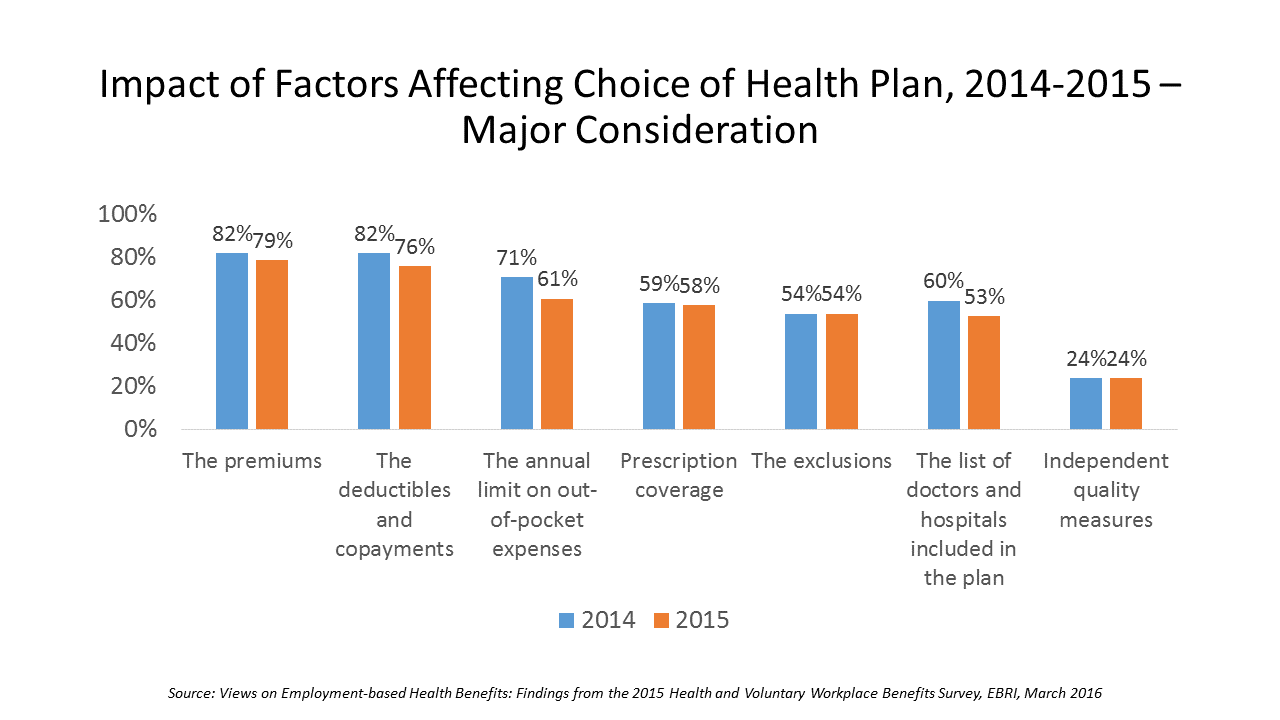
Consumers are extremely price-sensitive when it comes to shopping for health insurance. The cost of health insurance premiums, deductibles and copays, prescription drug coverage and out-of-pocket expenses rank higher in the minds of health insurance shoppers than the list of doctors and hospitals included in a health plan for health consumers in 2015. The Employee Benefit Research Institute (EBRI) surveyed 1,500 workers in the U.S. ages 21-64 for their views on workers’ satisfaction with health care in America. The results of this study are compiled in EBRI’s March 2016 issue of Notes, Views on Employment-based Health Benefits: Findings from the 2015 Health
Honoring the Doctor-Patient Relationship
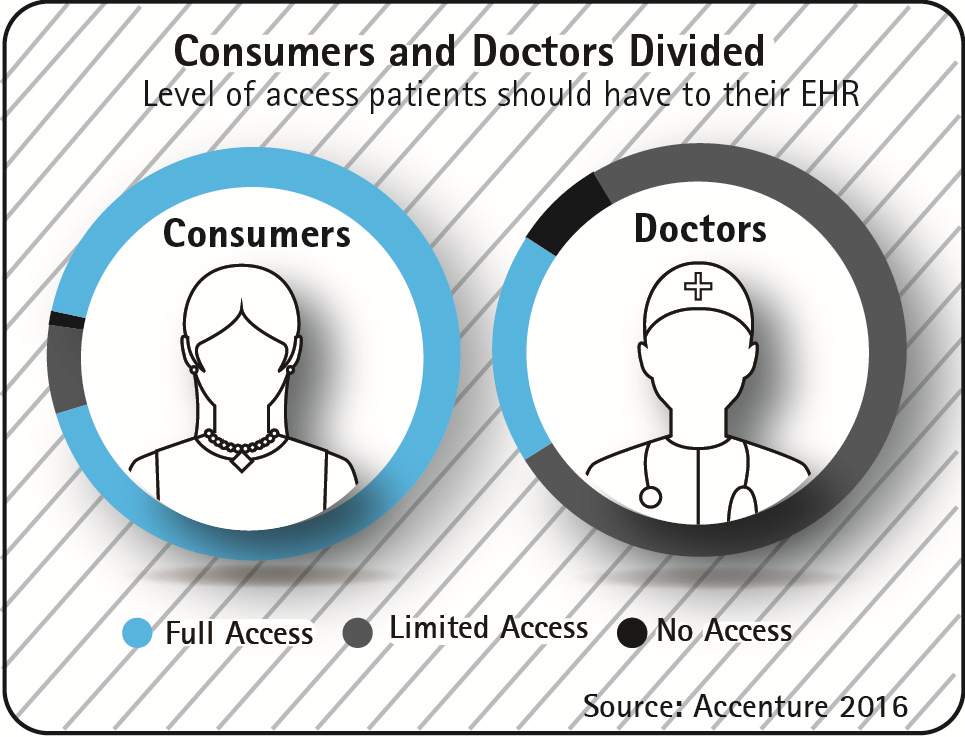
March 30 this week was National Doctors Day, which was proclaimed a national celebration by President George Bush in 1991. But as I’ve written through this week here on Health Populi, doctors may enjoy prestige on the outside, but they’re hurting on the inside — both economically in medical/business practices, and emotionally in their personal career-lives. Patients tend to like, even love, their personal physicians based on years of consumer polls on the topic (usually themed, “love my own doctor, hate the health care system”). But physicians and their patients aren’t on the same page, literally, when it comes





 I'm in amazing company here with other #digitalhealth innovators, thinkers and doers. Thank you to Cristian Cortez Fernandez and Zallud for this recognition; I'm grateful.
I'm in amazing company here with other #digitalhealth innovators, thinkers and doers. Thank you to Cristian Cortez Fernandez and Zallud for this recognition; I'm grateful. Jane was named as a member of the AHIP 2024 Advisory Board, joining some valued colleagues to prepare for the challenges and opportunities facing health plans, systems, and other industry stakeholders.
Jane was named as a member of the AHIP 2024 Advisory Board, joining some valued colleagues to prepare for the challenges and opportunities facing health plans, systems, and other industry stakeholders.  Join Jane at AHIP's annual meeting in Las Vegas: I'll be speaking, moderating a panel, and providing thought leadership on health consumers and bolstering equity, empowerment, and self-care.
Join Jane at AHIP's annual meeting in Las Vegas: I'll be speaking, moderating a panel, and providing thought leadership on health consumers and bolstering equity, empowerment, and self-care.