 In the long-run, health information technology (HIT) will improve the quality of health care, according to 73% of U.S. physicians. However, about the same number (7 in 10 physicians) believe that the ROI on health IT is inflated and that implementing EHRs will cost more, not less.
In the long-run, health information technology (HIT) will improve the quality of health care, according to 73% of U.S. physicians. However, about the same number (7 in 10 physicians) believe that the ROI on health IT is inflated and that implementing EHRs will cost more, not less.
Still, market forces from health insurance plans, payers and consumers are driving health IT adoption, according to Deloitte’s survey report, Physician adoption of health information technology: implications for medical practice leaders and business partners.
Electronic health records (EHR) adoption and meeting meaningful use (MU) Stage 1 criteria appears strongly related to the size of a physician practice: 82% of large practices with 10 or more physicians have an EHR system that meets MU Stage 1 requirements, compared with 31 % of solo practitioners. Furthermore, among solo practitioners, 45% do not have plans to adopt an EHR that meets MU. Underlying this solo practice data point is that these doctors are more likely to be cynical about the potential for HIT’s positive impact, Deloitte’s survey finds.
The major barrier preventing doctors from adopting EHRs is…surprise, surprise…the upfront costs of adoption.
For physicians who currently use an EHR that meets MU Stage 1, there are several main benefits derived from HIT:
- Faster and more accurate billing for services, among 74% of the high-EHR users
- Time savings via ePrescribing, 67%
- Improved communication and care coordination capabilities due to interoperability, 67%
- Clinical benefit due to immediately available data, 59%
- Cost saving by no longer managing and storing paper records, 59%
- Patient care improvement through clinic guideline prompts and faster lab results, 56^
- Practice/worksite efficiency increase, 53%
- Patient opportunity to submit information to their health record, 41%.
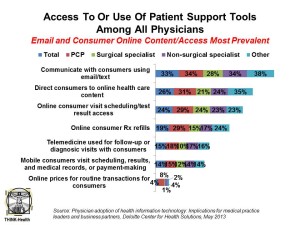
It is early days for physicians’ adoption of patient support tools, shown in the table. The most common support tool between doctors and patients is the use of email/texts, among 33%, followed by directing consumers to online health content (26%), enabling consumers to schedule online or access tests (24%), online consumer Rx refills (19%), telemedicine used for follow-up or diagnostic visits (15%), and mobile enablement of consumer tasks (e.g., test access, EHR access, payments).
While transparency is seen as a key tool for empowering health care consumers, only 4% of physicians overall post online prices for routine transactions.
Deloitte surveyed 613 doctors, including 146 PCPs, 142 surgical specialists, 197 non-surgical specialists, and 128 other physicians (e.g., pathology, occupational medicine, public health and prevention, and others not specified).
Health Populi’s Hot Points: In this BYOD era of mass physician adoption of mobile platforms — iPhones and iPads, especially — the Deloitte survey finds that 57% of physicians aren’t tapping into these technologies for clinical uses like accessing EHRs, eRx, and communicating with their medical colleagues. Other studies, however, are more sanguine about physicians’ use of mHealth tools.
In this survey, doctors who do not use mHealth platforms say the main barriers are the fact that their workplaces do not provide and are unwilling to use personal devices, among 44% of non-mHealth adopters; concerns about patient privacy, for 29%; and lack of suitability for the physician’s needs, cited by 26% of doctors.
Several big ideas come out of this study:
- Notwithstanding the future promise of the HITECH incentive, the up-front cost outlay of an EHR continues to be a barrier for late-adopting solo practitioners. Given that there are very low-cost models of EHRs in the marketplace, this raises a question of whether these physicians would ever adopt even an EHR offered on a “freemium” basis. In future surveys of doctors, it could be worthwhile to ask that “will you ever adopt” question.
- The BYOD movement seen in other vertical markets (e.g., business, education) may not be as pronounced in health care among physicians. Other studies, however, have noted BYOD among doctors, so this issue requires further study.
- Patients/consumers want more access to health care data and tools, especially from their trusted physicians. However, there is a chasm here that needs addressing. Perhaps better aligning payment for quality and patient satisfaction will further move this needle.
On a methodological note, only about 10% of physicians polled were primary care doctors (PCPs). However, there are over 200,000 PCPs in the U.S., equal to roughly one-third of doctors. This study might have under-accounted for PCP experience with EHRs.




 Interviewed live on BNN Bloomberg (Canada) on the market for GLP-1 drugs for weight loss and their impact on both the health care system and consumer goods and services -- notably, food, nutrition, retail health, gyms, and other sectors.
Interviewed live on BNN Bloomberg (Canada) on the market for GLP-1 drugs for weight loss and their impact on both the health care system and consumer goods and services -- notably, food, nutrition, retail health, gyms, and other sectors. Thank you, Feedspot, for
Thank you, Feedspot, for  As you may know, I have been splitting work- and living-time between the U.S. and the E.U., most recently living in and working from Brussels. In the month of September 2024, I'll be splitting time between London and other parts of the U.K., and Italy where I'll be working with clients on consumer health, self-care and home care focused on food-as-medicine, digital health, business and scenario planning for the future...
As you may know, I have been splitting work- and living-time between the U.S. and the E.U., most recently living in and working from Brussels. In the month of September 2024, I'll be splitting time between London and other parts of the U.K., and Italy where I'll be working with clients on consumer health, self-care and home care focused on food-as-medicine, digital health, business and scenario planning for the future...