AI Is Expanding Healthcare Access, Enabling Clinician Wellbeing, and Preparing Proactive Patients – The Philips Future Health Index 2026

AI is already transforming healthcare delivery for clinicians, patients, and their clinical partnerships, we learn in The Philips Future Health Index 2026. For this year’s annual futures report, Philips conducted two surveys among 2,011 healthcare professionals and 20,085 patients, spanning ten countries and fielded between February and April 2026. AI adoption among healthcare providers and patients in this early phase is showing benefits translating into greater productivity, clinician well-being, improved data workflows, and expanded access and capacity for clinicians to see more patients. Health systems the
What $37,824 Can Buy You in the U.S. in 2026: a VW SUV, a Year of College Tuition, or Healthcare for a Family of 4

If you had an extra $38K to spend, what would be on your list? If you’re a parent of a college-aged son or daughter, paying for college would be a lovely idea. If you’re in need of a new car, then that money could get you a mid-sized SUV. If you valued being covered by a health plan through your employer, then you’d be sharing in that cost to the tune of over $14,000 for your family of 4, based on the annual forecast in the 2026 Milliman Medical Index. The actuaries and health
The Side Effects of Debt and Financial Stress Add Up to a Public Health Crisis in America

Financial stress and debt take are now an American public health problem, we realize in the report, Rising debt is taking a toll on Americans’ financial and mental health from the Achieve Center for Consumer Insights. A joint survey conducted by Achieve and Money.com assessed the fiscal health perspectives of 2,000 U.S. consumers ages 18 and over, fielded in February 2026. This first chart from the study report arrays various “side effects” of Americans dealing with financial stress and debt, most commonly feelings of fatigue and low energy, stress-eating, delayed decision
Will AI Make Our Minds Feel Like Boiling Frogs, Be Borrowed, or Inspire Agency and Joy? Learning from John Nosta

Like gas and healthcare prices crowding out other spending, the topic of “AI” can crowd out other issues in our email inboxes, LinkedIn and other social media channels, and local and national concerns. Getting my head into John Nosta’s new book, The Borrowed Mind: Reclaiming Human Thought in the Age of AI, could not have come at a better time given AI’s growing presence in my own brain, work conversations, and local political discussions in our community and state. After one read-through, I let John know I would need to do a
Will GLP-1s Shift the Actuarial Curves for Life Expectancy? Swiss Re Models the Scenarios

The growing adoption of GLP-1 medications has already begun to transform society and industry sectors, along with helping many patients effectively deal with managing diabetes and obesity, and other conditions. There is growing evidence that this group of medicines is also bending the actuarial curves for life expectancy, we learn in the report, The future of metabolic health and weight loss drugs from Swiss Re. In the report, Swiss Re shares the company’s vision of metabolic health, a graphic for which is shown here. The company (smartly) takes a broad ecosystem view
The Blurring of Consumer Brands and Healthcare – HealthConsuming Goes Mainstream, Ipsos Reports

As people have taken on self-agency for their health and health care decisions, two sides of a coin are responding to market forces to meet health-inspired consumers where they are, and where they want to “be:” consumer brands on one side of that coin, and healthcare companies on the other, we learn in the report Consumer Brands Are Becoming Healthcare’s Next Leader from Lauren Berry at Ipsos. Lauren points to four converging forces shaping the blur of consumer goods firms and healthcare stakeholders like providers and life science companies:
The Cost of Confusion with U.S. Healthcare – a deja vu of The Temptations’ “Ball of Confusion”
A new survey from RevSpring, a healthcare payments company, measures consumers’ feelings of friction with healthcare in America — where people feel frustration “at every level,” the topline reads. The title of the paper, The Cost of Confusion: How Friction Shapes the Healthcare Experience, reminded me of one of my favorite songs from Motown growing up, “Ball of Confusion.” This Temptations hit was written by the great Motown songwriters, Norman Whitfield and Barrett Strong (who interestingly and to the point of this post, recorded the first hit single for Motown, the fabulous song “Money [That’s What I Want],” in 1960).
Gas ‘n Healthcare ‘n Groceries: U.S. Voters’ Cost-of-Living Concerns Will Inspire Them to Vote in the Midterms in the Latest KFF Health Tracking Poll

The cost of health care will have a major impact on U.S. voters’ midterm voting decisions in November 2026, most Americans expressed in the April 2026 KFF Health Tracking poll. Kaiser Family Foundation surveyed 1,343 U.S. adults in April 2026 to assess peoples’ views on health care costs and their influence on voting behavior forward-looking to the midterm elections to be held on 3rd November 2026. The first chart quantifies that overall 55% of U.S. voters say health care costs will have a “major impact,” and another 33% say health costs will
Most Brands Speak to Women As If They Are Men: Learning from Hidden Women, Health Marketing Insights from 8th Day

Are women “seen?” And how do they see themselves compared with how companies see them — marketers, leaders, and any enterprise that’s trying to message and persuade women to calls-to-action? If you are working to inspire, influence, or engage that portion of the world’s population who are women, then a new study from 8th-Day brand consultancy can inform your strategies. It’s titled Hidden Women: Unlocking brand growth by seeing the unseen, and it’s chock full of insights and lightbulb moments from which you can benefit. In full and delightful disclosure, the 8th-Day team are
“Trust is the #1 Public Health Issue” and Health Citizens Live in an “Information Abundant” World That, Counterintuitively, Underpins Divisiveness – the 2026 Edelman Trust Barometer
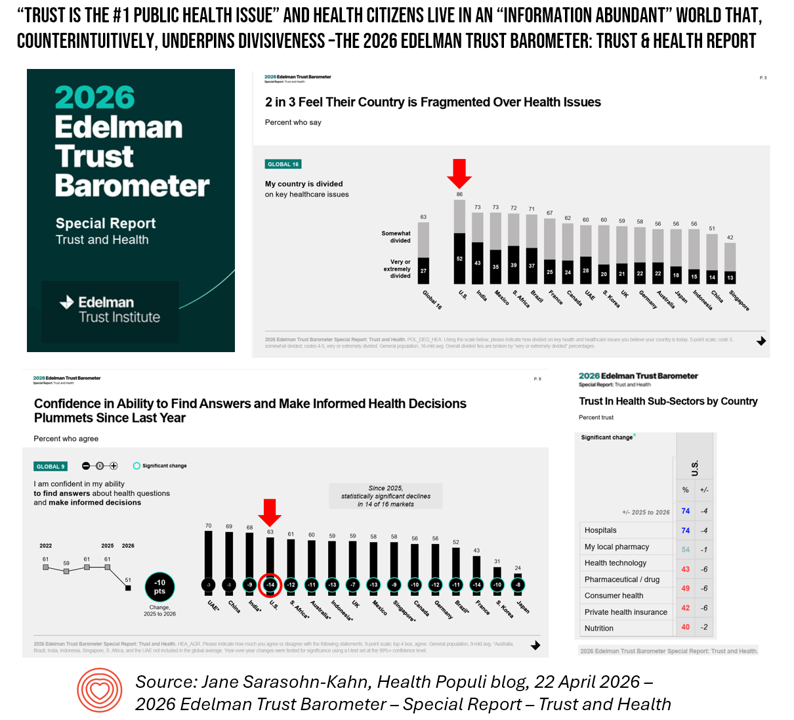
It would sound like good news that more health citizens, globally, are engaged with more information about health – a health information “abundance,” by the look at the data. But it’s not such great news when we learn that said information abundance also underpins health citizens’ confidence in finding answers and making informed health decisions, we learn in the 2026 Edelman Trust Barometer’s Trust and Health edition. In the U.S., the percent of people who felt confidence in their ability to find answers and make informed health decisions “plummeted,” in the words of the
“The #1 longevity hack is ‘don’t be poor’” — Kara Swisher is a health economist

In full transparency, I’ve been a fangirl of Kara Swisher since I first read her work with Walt Mossberg and Recode, coinciding with my own work on the early adoption of the Internet in health care. Today, Swisher is everywhere all-at-once, covering technology, politics, and now, seeking truths about the so-called longevity economy. Swisher appeared with Nicolle Wallace on her podcast, The Best People, on 13th April, so I was keen to tune in. The conversation covered a lot of ground, and it was Swisher’s take on science and health that I was most
The New Era of DIY Healthcare – The State of Consumer Healthcare is Buoyant, Empowering, and Holistic, from Head to Gut to Wallet

Consumers’ spending on healthcare, beyond a health insurance premium and hospital bills, is among the fastest-growing industries in the U.S. — with spending increasing faster than overall retail, Circana’s tracking data has quantified. In 2019, I published one of the early books on health care consumerism, HealthConsuming, my spidey-senses perceiving an expanding retail health landscape where patients-as-consumers, caregivers, Quantified Self’ers, and wellness aficionados were engaging with a variety of touchpoints based on their personal values and sense of value to co-create personal and family health: in grocery stores, Big
Americans Are Health Information Seekers — Far Above All, Valuing Info from Providers and Medically-Trained Sources (and lessons for AI in health)
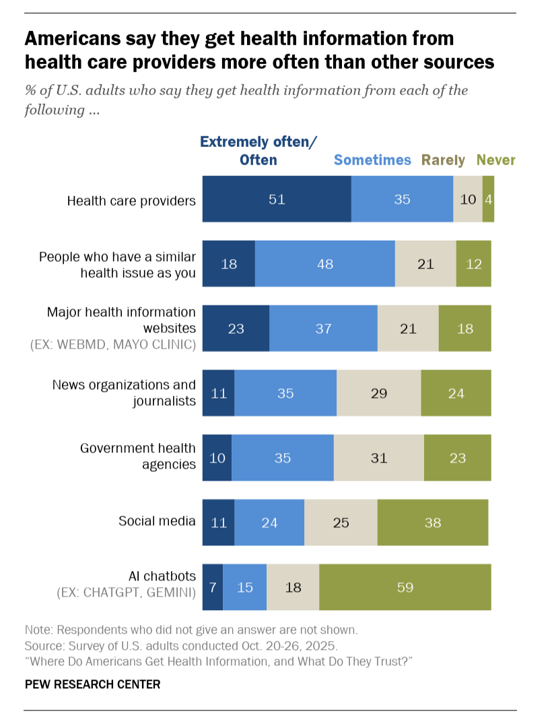
A commentary in Nature Medicine this week asserts that, “Quality health infomration for all is a fundamental determinant of health.” Lawrence Gostin, a learned health care legal expert at Georgetown, and colleagues, note that, “Society is at a turning point, faced with misleading guidance and ubiquitous, fast-spreading digital and social media…Amplified by generative AI, poor quality information corrodes trust in science and drives social and political polarization.” With the context in mind that health information is a social determinant of health, we turn to a report from the Pew Research Group which asks and answers the question, Where do Americans
Past is Prologue as CVS Returns to Its “CVS Pharmacy” Roots – What it Means for Health Consumers and Retail Health (with a nod to Colruyt Group in Belgium)

Going back to its roots, CVS Health announced plans to open 20 “apothecary-style” pharmacies around the U.S., the first of which was sited in Chicago’s West End. The new brick-and-mortar stores will average 3,000 square feet, providing full-service pharmacies staffed by licensed pharmacists. “Pharmacists are among the most accessible and most trusted health care providers,” Len Shankman, EVP and President of Pharmacy and Consumer Wellness for CVS Health is quoted in the press release for the plans. This new footprint is meant to enable “pharmacy teams to continue to build relationships with patients
Doctors and Consumers in America Agree: Health Care Access and Affordability Rank Top of Mind in March 2026 (surveys from Athenahealth and Gallup)
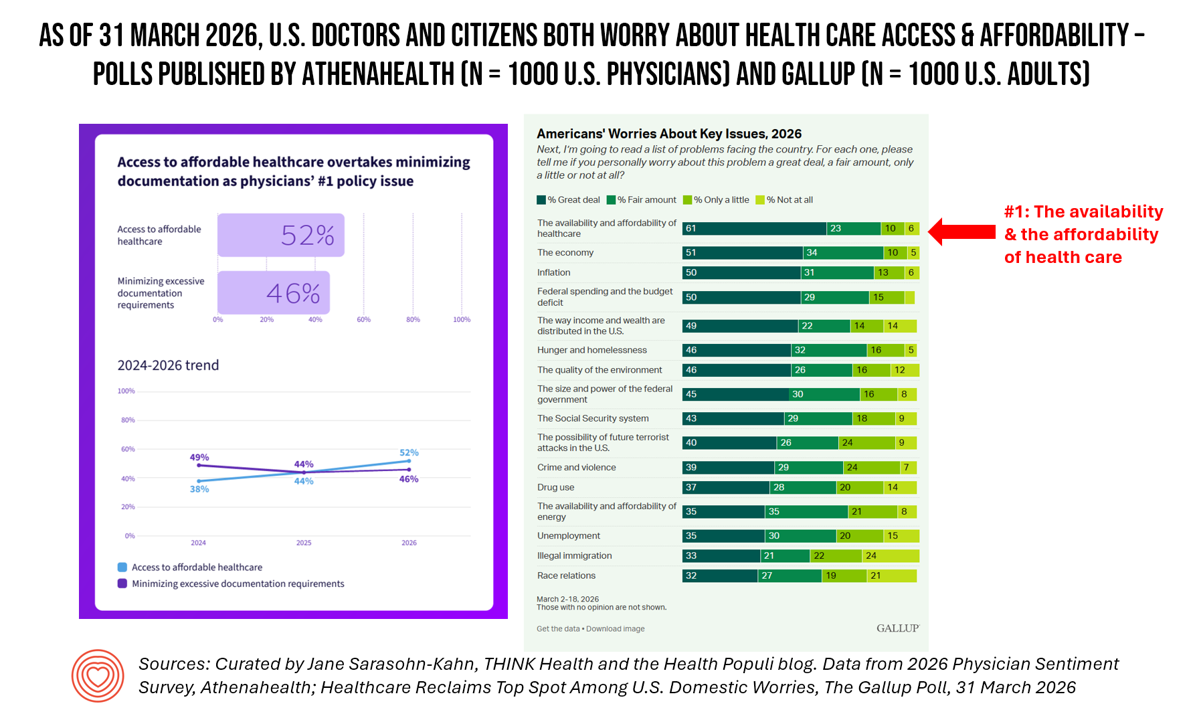
In uncannily-timed releases of two surveys in March 2026, we see that U.S. physicians and consumers both rank health care access and affordability as the top issue they face — for medical practices among doctors, and for everyday life worries among U.S. health citizens. On the physician front, The 2026 Physician Sentiment Survey was published by Athenahealth, gauging U.S. doctors’ views on the state of medical practice and healthcare in America. “Over the past three years,” Athenahealth observes, “access to affordable healthcare has risen sharply to become
Food & Wine Magazine Features Food-As-Medicine: Good for People, Good for the (Local) Economy

When the mainstream media food magazine Food & Wine devotes a long article to the concept of food-as-medicine, it calls to me….loudly. Here’s another proof-point for tying together public and individual health while boosting local economies. F&W featured Stacey Leasca’s essay, What Happens When Doctors Start Prescribing Food Instead of Pills?, online this month, and Stacey did her homework. One of Stacey’s go-to evidence-based resources for her column was the recently-released Rockefeller Foundation report, From Farm to FIM: The Economic Impact of Local Food is Medicine. The Foundation studied several local
Consumers Using AI for Health — Especially Motivated When People Lack Access to Care
Peoples’ use of AI for researching health information and supporting mental health appears to trump consumers’ trust in the technology, based on the March 2026 Kaiser Family Foundation (KFF) Tracking Poll on Health Information and Trust. Similar to the recent Rock Health consumer survey on AI adoption (discussed in Health Populi earlier this week), about 1 in 3 U.S. adults have used AI for health information in the past year for either physical or mental health queries. There are many studies gauging consumers’ use of AI in health care, but
Consumer Adoption of AI for Health and Self-Care – Doubling to 36% in a Year, Via Rock Health’s Latest Snapshot
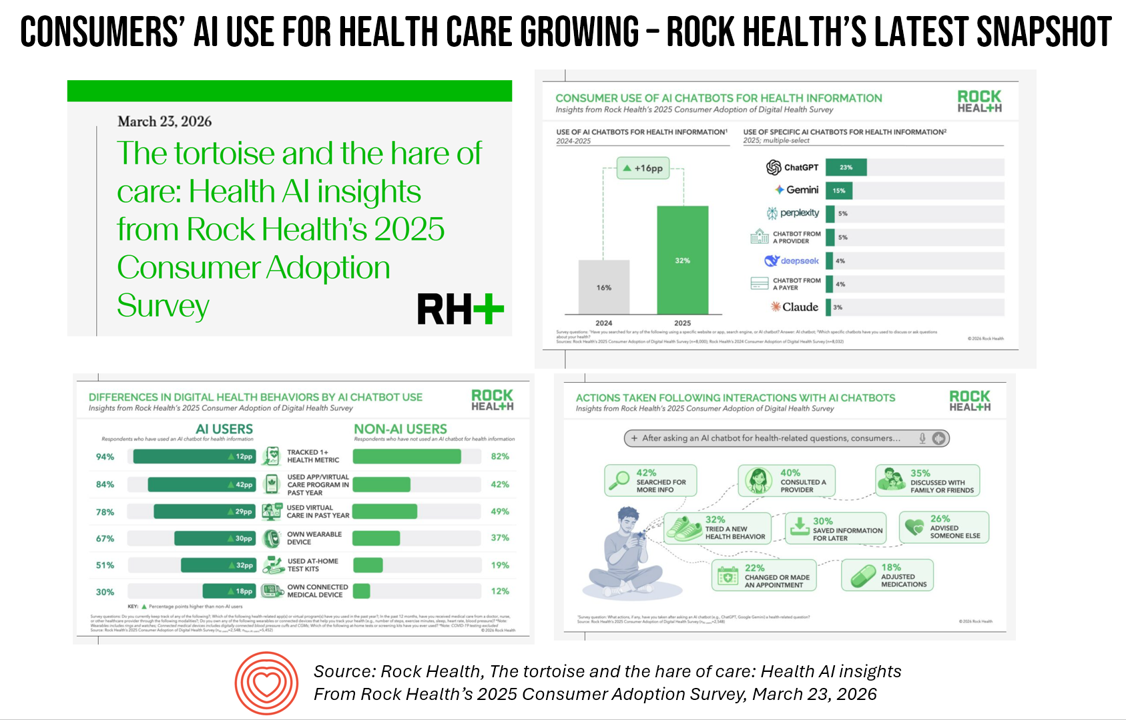
From pre- and self-diagnosis of symptoms to prescription drug treatments and ongoing care, millions of U.S. consumers have used AI chatbots for health and wellness according to the consumer health adoption survey from Rock Health. The report was published in late March 2026, with AI-focused data from the consumer survey fielded in December 2025. In just one year from 2024 to 2025, consumers’ use of AI chatbots for health information doubled from 16% of people to 32%. The most popular brand of AI for health information seeking was ChatGPT (owned by OpenAI, with whom
The “Five-Month” Cognitive Penalty of Financial Decline: A Significant Loss of Financial Well-Being Correlates with About Five Months of Cognitive Decline A Year

Lower financial well-being and worsening financial conditions have been linked to declining brain function, according to new research from a team at the Columbia Mailman School of Public Health. The research, Changes in financial well-being and memory function and decline in middle-aged and older adults, was published this month in the American Journal of Epidemiology. “Worse financial well-being in midlife and older age — and especially declines over time — are associated with lower memory scores and faster cognitive decline,” the study notes — among the first to scrutinize the relationship between brain
Healthcare AI Direct-to-Consumer: Everything, Everywhere, All At Once

The announcements of consumer-focused AI for health are coming Fast and Furious. As we are coming off of the 2026 Oscars broadcast, it inspires me to quote another movie title, Everything, Everywhere, All at Once. In the moment, it feels like consumer health-focused AI is indeed in a fast-and-furious launch phase. It’s time for me to provide an update on this fast-moving-consumer service, discussing the latest vendor announcements and the ongoing concerned embrace of AI among early adopting citizen-users of AI for health/care. For context, let’s start with long-time AI-medical expert Dr. Eric Topol’s view on the current state. Registering





 I'm grateful to be part of the Duke Corporate Education faculty, sharing perspectives on the future of health care with health and life science companies. Once again, I'll be brainstorming the future of health care with a cohort of executives working in a global pharmaceutical company.
I'm grateful to be part of the Duke Corporate Education faculty, sharing perspectives on the future of health care with health and life science companies. Once again, I'll be brainstorming the future of health care with a cohort of executives working in a global pharmaceutical company. Jane joined host Dr. Geeta "Dr. G" Nayyar and colleagues to brainstorm the value of vaccines for public and individual health in this challenging environment for health literacy, health politics, and health citizen grievance.
Jane joined host Dr. Geeta "Dr. G" Nayyar and colleagues to brainstorm the value of vaccines for public and individual health in this challenging environment for health literacy, health politics, and health citizen grievance.  I'm grateful to be part of the Duke Corporate Education faculty, sharing perspectives on the future of health care with health and life science companies. Once again, I'll be brainstorming the future of health care with a cohort of executives working in a global health care enterprise.
I'm grateful to be part of the Duke Corporate Education faculty, sharing perspectives on the future of health care with health and life science companies. Once again, I'll be brainstorming the future of health care with a cohort of executives working in a global health care enterprise.