“Trust is the #1 Public Health Issue” and Health Citizens Live in an “Information Abundant” World That, Counterintuitively, Underpins Divisiveness – the 2026 Edelman Trust Barometer
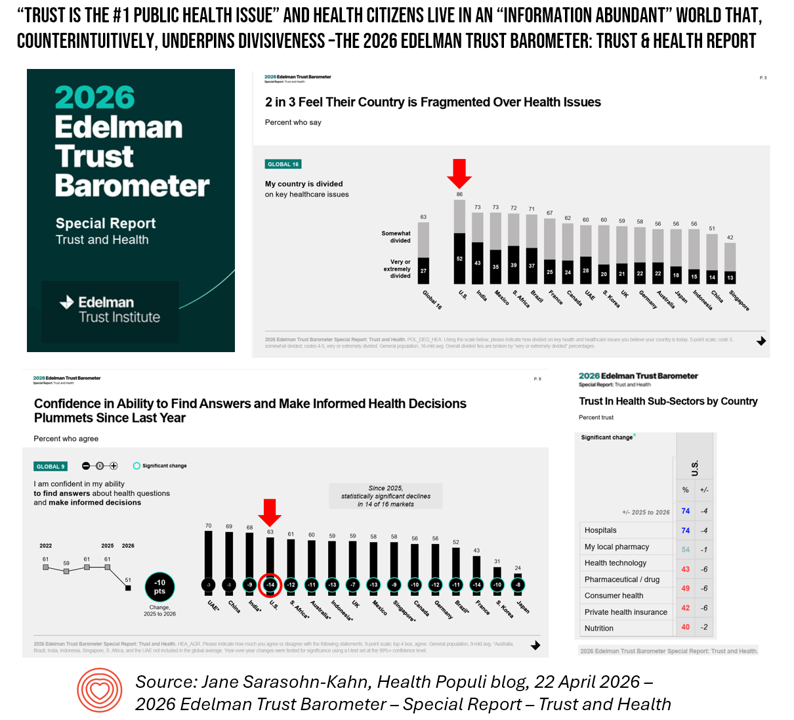
It would sound like good news that more health citizens, globally, are engaged with more information about health – a health information “abundance,” by the look at the data. But it’s not such great news when we learn that said information abundance also underpins health citizens’ confidence in finding answers and making informed health decisions, we learn in the 2026 Edelman Trust Barometer’s Trust and Health edition. In the U.S., the percent of people who felt confidence in their ability to find answers and make informed health decisions “plummeted,” in the words of the
Past is Prologue as CVS Returns to Its “CVS Pharmacy” Roots – What it Means for Health Consumers and Retail Health (with a nod to Colruyt Group in Belgium)

Going back to its roots, CVS Health announced plans to open 20 “apothecary-style” pharmacies around the U.S., the first of which was sited in Chicago’s West End. The new brick-and-mortar stores will average 3,000 square feet, providing full-service pharmacies staffed by licensed pharmacists. “Pharmacists are among the most accessible and most trusted health care providers,” Len Shankman, EVP and President of Pharmacy and Consumer Wellness for CVS Health is quoted in the press release for the plans. This new footprint is meant to enable “pharmacy teams to continue to build relationships with patients
The “Five-Month” Cognitive Penalty of Financial Decline: A Significant Loss of Financial Well-Being Correlates with About Five Months of Cognitive Decline A Year

Lower financial well-being and worsening financial conditions have been linked to declining brain function, according to new research from a team at the Columbia Mailman School of Public Health. The research, Changes in financial well-being and memory function and decline in middle-aged and older adults, was published this month in the American Journal of Epidemiology. “Worse financial well-being in midlife and older age — and especially declines over time — are associated with lower memory scores and faster cognitive decline,” the study notes — among the first to scrutinize the relationship between brain
Self-Rationing Health Care in America – 1 in 2 Americans Earning As Much as $180,000 Have Postponed a Life Event Due to Healthcare Costs
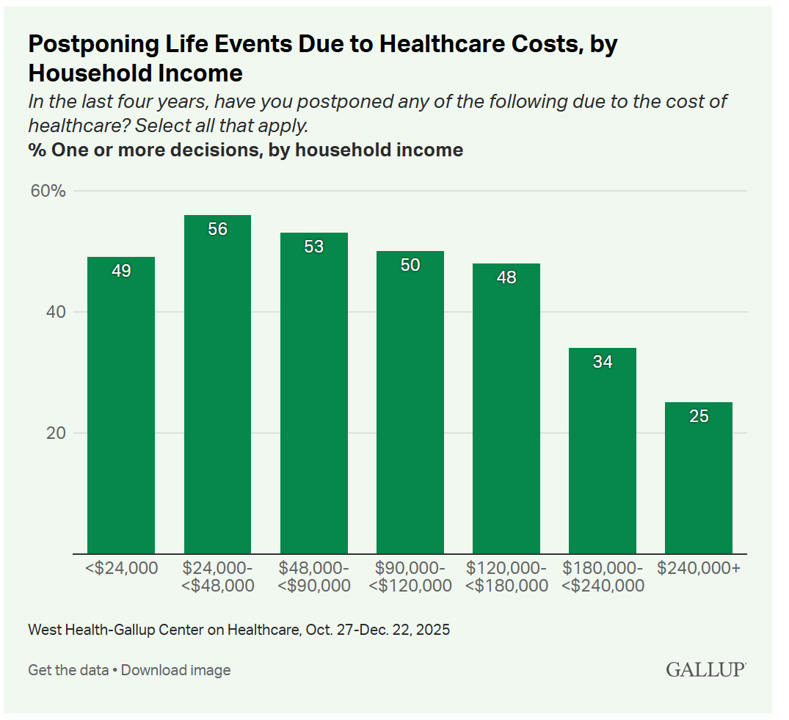
Americans’ ability to pay for health care has eroded in the past several years, with 1 in 3 people trading off life experiences, eating a meal, or driving less to cover healthcare expenses. These are some of the findings revealed by The West Health-Gallup Affordability Index published 12 March. What struck me was the rate of life event-postponement done by consumers earning relatively high incomes. One-half of Americans earning between $120,000 and $180,000 postponed a life event in the past four years due to healthcare costs. One in four Americans earning over
“Will Work For Health Care:” Americans Trading Off Wages For Healthcare (Again)
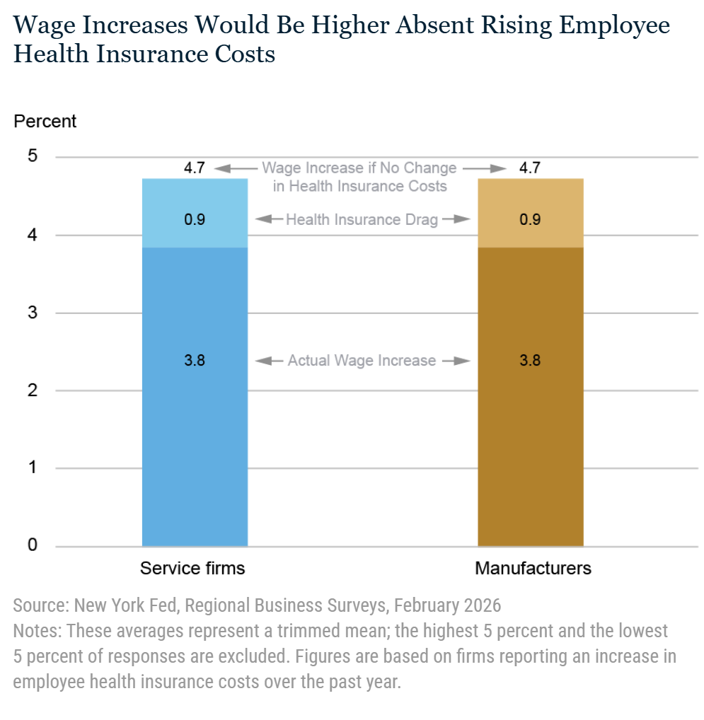
Many people living in America who receive health benefits at the workplace traded off wage growth for health insurance coverage, a report from the Federal Reserve Bank of New York published this week. For those of us working in the health economics and policy space since the 1990s, the Fed team gave me a strong sense of déjà vu. The bar graph cited in the report explains the math behind the wage/health plan trade-off. “Among those businesses experiencing an increase in employee health insurance costs, the average wage increase over
The Healthcare Affordability Elections, 2026 and 2028 – Listening to the KFF Tracking Poll, January 2026

The title of KFF’s press release launching the Foundation’s January 2026 Health Tracking Poll clearly observes, “Health Care Costs Tops the Public’s Economic Worries as the Runup to the Midterms Begins.” I’ve pulled out the key details to share my lens on the 2026 midterm and 2028 Presidential election forecast, which I believe will turn out to be (in part) The Patients’ Elections. Here’s the top-line title finding — where most people in the U.S. — 2 in 3 people (66%) — are worried more about health care costs compared with other major household expenses.
As Adult Vaccination Levels Fall, We Must Assert the Value of Vaccines

The rate of vaccinations among people 65 years of age and older has declined since 2019 — a personal health challenge for aging Americans and their caregivers and families, and a public health problem for the U.S. The Centers for Disease Control’s National Center for Health Statistics published Data Brief 547 on the situation on January 21, 2026. In the meantime, serendipity and timing are uncanny in the moment as The Value of Vaccines conversation series from Pfizer was launched this week. I am grateful to have participated in this project with several sisters-in-expertise: Elif Alyanak from Avalere, Venesa Day
Distrust is the default, insularity is our mindset: The Edelman Trust Barometer in 2026

ss Last year’s “shared reality” was a culture of trust and a crisis of grievance: this year, it’s trust and insularity, we learn from the Edelman Trust Barometer for 2026, launched this week during the World Economic Forum in Davos, Switzerland. Here are the Top 10 findings from the annual study, which Edelman conducted among nearly 34,000 citizens in 28 countries in October and November 2025: Insularity undermines trust The mass class divide deepens Nationalism is widespread Optimism for the future wanes Personal networks fill a void left by
Navigating a Constellation of Uncertainties: Health/Care in 2026 (My Un-Forecast)

Almost from the first year of launching Health Populi in 2007, I’ve written a “TrendCast” for the coming year of health care. Over many years, there weren’t so many blogs devoted to health care which featured such prognostications, and so readers could divine signal from noise and move forward into new years with manageable lists of What To Expect Next Year in Healthcare. Here’s one from ten years ago that brings a sense of déjà vu: most of the findings are consistent with what we know for sure about 2026 and it’s useful to look back with today’s eyes to
Men’s Fertility Feelings – The Influence of Trust and Social Media (My Progyny Post #3)

Trust is a key enabler for people’s health engagement. As the American Medical Colleges’ Center for Health Justice defines it, trustworthiness is “rooted in honesty and honors lived experience….. key to a successful patient-provider partnership.” In his book, Notes On Being A Man, Scott Galloway calls out that men’s fertility issues are formed as part of a larger societal context and crisis point, exacerbated by economic pressures and lack of opportunities for male bonding and in-person social touchpoints. In the second post in this series of three, we discussed those economic pressures Galloway notes, and the financial stressors that shape
Trust and AI in Healthcare: At a Crossroads, Edelman Finds

Enthusiasm for innovation is not a guaranteed thing; furthermore, trust in AI lags trust in the overall technology sector, we find in the 2025 Edelman Trust Barometer research through a Flash Poll: Trust and Artificial Intelligence at a Crossroads, discussed in a webcast on 3 December. People in the U.S. are more than twice as likely to reject the growing use of AI than embrace it, with the embrace of AI much lower than peoples’ enthusiasm for it. Edelman conducted the poll in five countries — Brazil, China, Germany, the UK and the US — with sample sizes at least 1,000+
The Home Economics of Family and Fertility: Men’s Financial Views on Their Fertility Journeys (My Progyny Post #2)

Cost is a leading reason why people say they could not obtain the fertility care they need. But the costs of IVF and other forms of fertility care lie within a larger home economics framework of family-building and -raising. The context and costs of raising a child in America. Consider the layers of a household budget starting with the home’s “macro”-economics of income. Then within that circle, especially in the U.S., the factor of whether that household is covered by employer-sponsored health insurance. The next layer of more health micro-economics in the family is the
Most MAGA Supporters Support Extending the Expiring ACA Tax Credits – Will That Move Negotiations to Re-Open the Government?

A couple of days into the U.S. Federal government shutdown, there’s one message the Congressional Democrats are tending to voice: that is that health care is on the line, and that’s the issue on which they’re betting will bring negotiators back to Capitol Hill — expecting a few Republicans to join in that dialogue. Most U.S. adults across political parties would want to see Congress extend the enhanced Affordable Care Act tax credits that are set to expire next year we see in a poll from the Kaiser Family Foundation published October 3. And that includes most Republicans and MAGA
The Emotional Drivers of Healthcare Discontent – Press Ganey Points to Access and Affordability Worries Driving Anxiety and Anger

In the current era of U.S. health citizen grievance with the health care system, people feel anxious, confused, and angry — especially when it comes to access and affordability of health care. We learn more about these emotional drivers of health/care grievance in Understanding Health Plan Member Discontent, an assessment of health consumers’ views of satisfaction across health insurance plan types (commercial, Medicaid, Medicare, and marketplace plans) and age of member, from the health consumer experience team at Press Ganey. Those three underlying factors driving discontent translate to different generations differently. Overall, anxiety relates to
How Consumers’ Access to Telehealth Impacts Medical Real Estate and Design Decisions

The idea of “hospitality” in health care is not new, but the nature of how patients-as-consumers are dealing with health care choices based on what looks and feels good is changing the nature of what hospitality means in technology-enabled health care delivery, we learn from the 2025 Patient Consumer Survey conducted by JLL. Jones Lang LaSalle Inc. (JLL) is one of the largest global commercial real estate firms with a strong portfolio of medical buildings. So it is worthwhile to track what the company is learning about health care delivery distributed both inside and outside of brick-and-mortar medical buildings.
Trust Is Eroding for Vaccines Among U.S. Parents — New Insights from KFF and the Washington Post
By the summer of 2025, 1 in 6 U.S. parents had skipped or delayed childhood vaccinations, discovered in the 37th annual edition of the KFF/The Washington Survey of Parents. The study was conducted among 2,716 parents or legal guardians of children, via interviews online in English and Spanish between July 18 and August 4, 2025. In detail by demographic, 83% of all U.S. parents had kept children up-to-date with recommended childhood vaccines (16% not doing so) 74% of self-described MAGA Republicans kept kids up to date with the recommended vaccines (25% not doing so),
Dr. Osterholm Explains “The Big One” – A Deja Vu Moment with a True North Public Health Expert

“The truism that no one is completely safe until everyone is safe is a truism because it happens to be true.” So caution Michael Osterholm, epidemiologist, professor at the University of Minnesota School of Public Health, and director of CIDRAP (the Center for Infectious Disease Research and Policy at the U-MN) and collaborating writer Mark Olshaker in their new book, The Big One. (In this post, for the sake of brevity, I’ll refer to the two authors as “O&O”). Simply put, the tagline tells us what we are about to read: a
U.S. Physicians Have to Deal with the Growing Info-Demic of Disinformation Meant to Mislead Patients

Close to 100% of U.S. doctors agree that misinformation and/or disinformation undermines patient care, according to a new survey from the Physicians Foundation. The Foundation polled over 1,000 U.S. physicians in late May 2025 to gauge doctors’ perspectives on information and patients’ health literacy. Furthermore, over one-half of physicians believe that misinformation – and/or disinformation — significantly impacts the ability to deliver quality patient care. The first graphic differentiates between “misinformation” and “disinformation,” where the latter is false or inaccurate information deliberately intended to mislead people. Misinformation is somewhat more benign in
Prescription Drug Pricing in America – a 3-Part Update, From the Over- the-Counter OPill and “Half-Price” Ozempic to Most-Favored-Nation Rx (Part 3)

Welcome to Part 2 of 3 in my consideration of Prescription Drug Pricing in America. You can catch up with yesterday’s Part 1 post here, and Part 2 here. The macro-context for these 3 posts are the forecasts for health care spending for the coming year. Health care cost increases forecasted for 2026 will, in significant part, be driven by prescription drug trend. This graphic from this week’s release of the Business Group on Health’s employer survey on healthcare cost growth to 2026 illustrates a key finding that’s echoed in other similar studies recently released and covered here in Health Populi.
Prescription Drug Pricing in America – a 3-Part Update, From the Over- the-Counter OPill and “Half-Price” Ozempic to Most-Favored-Nation Rx (Part 1)

Health care costs will increase, overall, as much as 10% in 2026, the consensus of several health benefit analysts inform us. And, “workers to bear brunt of health cost increases in 2026,” reads today’s Axios headline on the topic, weaving together several studies from the Business Group on Health, Mercer, and the International Foundation of Employee Benefit Plans. A kay cost-contributor cited in all of these health cost forecasts is the prescription drug line item: specialty drug prices, and specifically the costs of GLP-1 medicines and cancer therapies. One strategy gaining fast-traction on both the
How Taking Care of Our Pets Could Inspire Us to Care Better for Ourselves (and Each Other)

In a recent study which was part of the American Heart Association’s Healthy Bond for Life initiative, two-thirds of Americans told the AHA that they took better care of their pets than themselves. So with a lens on how to help inspire peoples’ self-care, I was keen to dive into research from Pet Partners Insurance (PPI), a pet health insurance provider, collaborating with the Human Animal Bond Research Institute (HABRI), to learn more about The Power of Pet Perks: How Pet-Inclusive Benefits Drive Employee Engagement, Retention, and Positive Workplace Culture. My interest
U.S. Workers Who Get Health Insurance From Work Can Expect Greater Cost-Sharing and New Networks in 2026

At least one-half of employers will likely raise employee cost-sharing amounts in 2026, according to the Survey on health & benefit strategies for 2026 from Mercer. Mercer surveyed 711 organizations for this study, fielded in April 2025, to assess employers’ views on and strategies for health benefits in 2026. There are three challenging pillars underlying employers’ 2026 approaches to workers’ benefits: How to disrupt cost growth with what Mercer coins as “bolder” strategies How to consider and address all dimensions of affordability, and, How to design and implement inclusive benefits that build workforce
Medical Cost Trend at 8.5% in 2026? PwC Sees “No End in Sight” for Increased Healthcare Spending
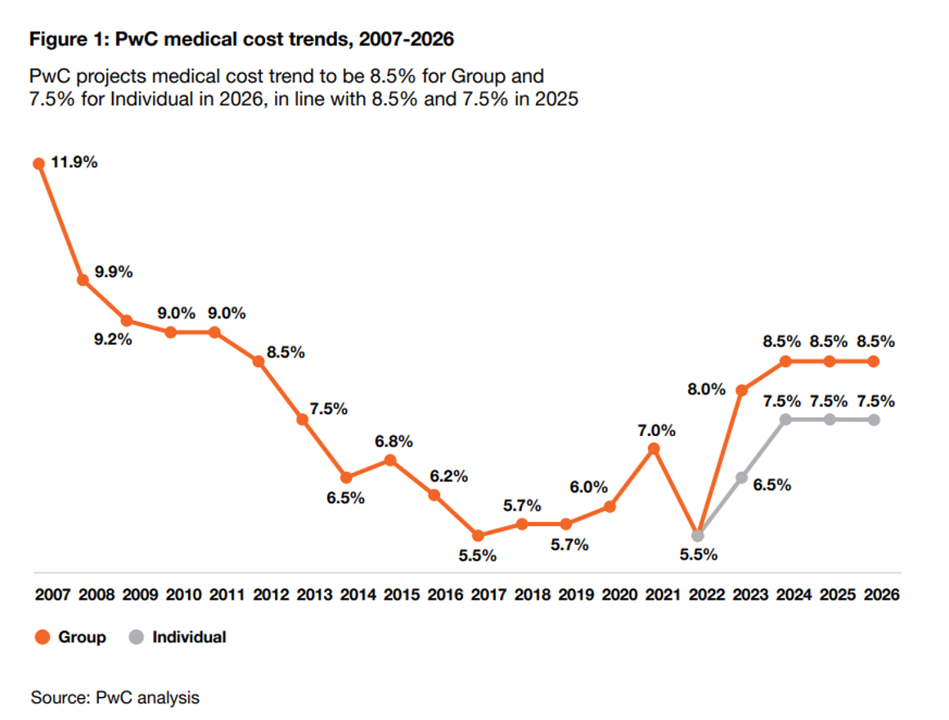
For the third year in a row, medical cost trend — the expected increase of health care costs by health plans — will be 8.5% for group health insurance. This contrasts with a low of 5.5% in 2022 when cost trend dipped coming out of the COVID-19 pandemic….then shot up to 8.0% the following year in patients’ healthcare catch-up mode. Welcome to Behind the Numbers 2026, the annual medical trend report from PwC. What’s continuing to drive up health care costs? PwC identifies 4 medical cost inflators, and 2 “deflators” (these being
National Health Spending in the U.S. in 2033: What 20.3% of the GDP Will Be Spent On

By 2033, national health spending will comprise 20.3% of the U.S. GDP, based on the latest national health expenditure projections developed by researchers from the Centers for Medicare and Medicaid Services (CMS). This growth will be happening as CMS projects coverage of insured people to decline over the period. Earlier today, I attended a media briefing hosted by Health Affairs to receive the CMS team’s top-line forecast of NHE from 2024 to 2033 discussing these findings. Fuller details on the projections will be released in the July issue of Health Affairs on 7
We Go Further Together: Calling for Collaborations, An Actionable Context for AHIP 2025

There are many ways to measure the dysfunction of health care in the U.S.: we can point to relatively poor incomes relative to the rest of the developed world, given how much money is allocated to health care in America. The maternal mortality rate in the U.S. is unconscionably high, akin to some middle- and lower-income nations in the world. And medical debt is a uniquely American form of financial toxicity compared with other OECD nations where the concept is, well, foreign. Even with these many failures, though, it’s important to put U.S. health care in a larger context: the
A Toyota RAV4 Hybrid, a Playground Set, or Healthcare for a Family of 4: What $35,119 Can Buy in 2025 According to Milliman
If you went shopping for something that cost $35,119 in 2025, which would you most value? A new 2025 Toyota RAV4 Hybrid with some extras on board? A Canyon BYO playground set for your yard, school, or social-athletic club? Or, Healthcare coverage for a family of 4 in the form of a PPO? Welcome to this year’s 20th anniversary edition of the Milliman Medical Index (MMI), which I’ve looked forward to reviewing for most of its two-decade history. [You can read my annual takes on the MMI here in Health Populi by searching “MMI” and the year of publication in
Health, Wealth, and How Business Can Support Consumers in an Era of “Uncertainty on Steroids”

Facing uncertainties across everyday life flows, U.S. consumers look to economic and health security — and welcome businesses to support these, we learn in an analysis from The Conference Board. The Conference Board (TCB) polled 3,000 U.S. consumers gauging their perspectives on uncertainties emerging out of the new Trump administration’s policy changes introduced in the first quarter of 2025. The chart details people’s financial/fiscal responses in blue, and the health (mental, social, and physical aspects) in yellow: Consumers’ fiscal strategies for coping with uncertainty are to seek out more affordable brands and retailers, adjusting
A Profile of Health Consumer-Generations’ Use of Digital Health – Rock Health Takes Us Through the Ages

In the past year, most consumers in the U.S. have used virtual care, tracked at least one health metric digitally, and own a wearable or connected health device. Digital health has certainly gone mainstream across U.S. consumers, with varying utilization and motivation by generation, we learn in the report, Screenagers to Silver Surfers: How each generation clicks with care from Rock Health. To segment health consumers by age/generation, the RH team mined the firm’s 10th Consumer Adoption of Digital Health Survey which polled over 8,000 U.S. adults in 2024 on peoples’ perspectives
Health Insurance Coverage Among Smaller U.S. Businesses Is Eroding: A Signal From JPMorganChase

Working-age people in the U.S. depend on their employers to provide health insurance; just over one-half of people in America receive employer-sponsored health insurance. But a concerning signal has emerged that calls into question how sustainable the uniquely American employer-sponsored health plan model is: that is that one in 3 small businesses in the U.S. stopped covering health insurance after the worst of the pandemic health effects in 2023 as the companies payroll expenses continued to increase, a statistic raised in The consistency of health insurance coverage in small business: industry challenges and insights, a report from the JPMorganChase Institute
U.S. Health Care in 2025 Requires Scenario Planning: The Uncertainties (AI!?) That Inspire DIY Healthcare

As Weight Watchers prepares to initiate bankruptcy proceedings, I file the news event under “thinking the unthinkable.” “Thinking about the unthinkable” is what Herman Kahn, a father of scenario planning, asked us to do when he pioneered the process. In this book, for Kahn, “the unthinkable” was thermonuclear war, and the year was 1962. The book was tag-lined as “must reading for an informed public” and in it, Kahn I’ve been drawn back to this book lately because of a more intense workflow using
Are We Liberated Yet? Tariffs Can Impact Financial Health (Riffing on MoneyLion’s Health Is Wealth Report)

Americans’ financial health was already stressing consumers out leading up to Liberation Day, April 2nd, when President Trump announced tariffs on dozens of countries with whom the U.S. buys and sells goods. A new report from MoneyLion and Mastercard called Health is Wealth is well-timed for today’s Health Populi blog. The study was fielded by The Harris Poll online among 2,092 U.S. adults 18 and older between February 28 and March 4, 2025, so it was completed a month before the tariffs came to hit peoples’ 401(k) savings and employers’ company stock market caps.
From Bowling Alone to Eating Alone – What the Shift to Take-Out Food Means for Our Social Well-Being and Mental Health

New data from the American Time Use Survey, research conducted by the U.S. Census Bureau and the Bureau of Labor Statistics, shows that Americans now favor eating in-home compared with eating out at restaurants. Corroborating this shift is other data from the National Restaurant Association sharing that 74% of all restaurant traffic in 2023 came from “off premises” customers — that is, from takeout and delivery — up from 61% in the pre-COVID era. What does this mean for our health, well-being, and sense of community and connectivity? I’m preparing a new talk to
The Growth of DIY Digital Health – What’s Behind the Zeitgeist of Self-Reliance?
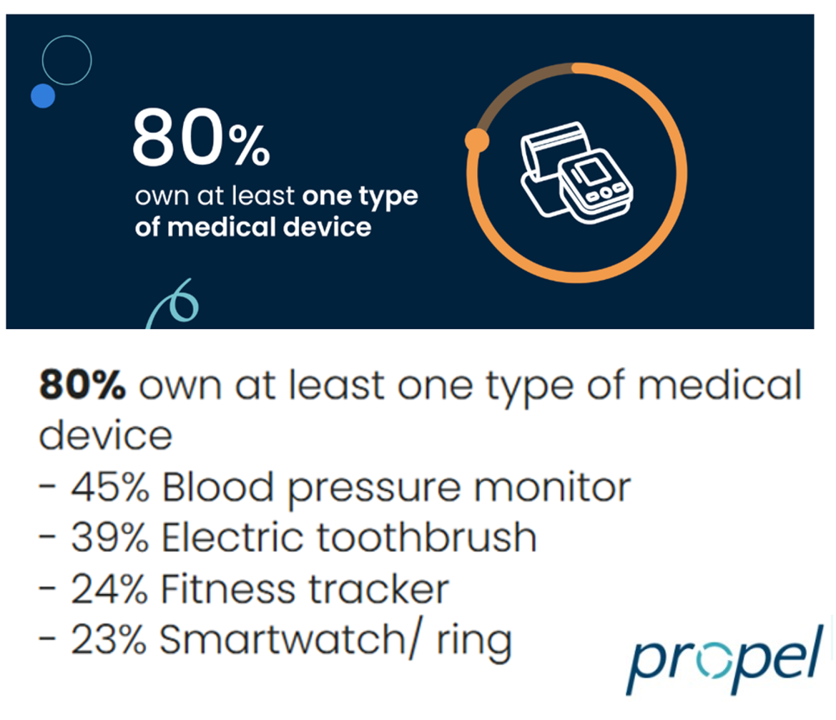
Most people in the U.S. use at least one medical device at home — likely a blood pressure monitor. used by nearly one-half of people based on a survey of 2,000 consumers conducted for Propel Software. The Propel study’s insights build on what we know is a growing ethos among health consumers seeking to take more control over their health care and the rising costs of medical bills and out-of-pocket expenses. That includes oral health and dental bills: 2 in 5 U.S. consumers use electric toothbrushes (a growing smart-device category at the
A Mis-Trust Hangover for Health Care 5 Years After COVID Began – an Edelman Trust Barometer Update

On March 11, 2020, The World Health Organization announced that the coronavirus was deemed a pandemic. WHO Director-General Dr. Tedros Adhanom Ghebreyesus asserted, “We have called every day for countries to take urgent and aggressive action. We have rung the alarm bell loud and clear.” Five years later, Edelman has fielded a survey to determine what some 4,000 health citizens living in 4 countries (Brazil, India, the UK, and the U.S.) are thinking and feeling about life after COVID-19 — and especially where their trust lies in institutions, fellow citizens, and future public health emergencies. I listened in on a discussion
Consumers Are Financially Stressed – What This Means for Health/Care in 2025

People define health across many life-flows: physical health, mental health, social health, appearance (“how I look impacts how I feel”) and, to be sure, financial well-being. In tracking this last health factor for U.S. consumers, several pollsters are painting a picture of financially-stressed Americans as President Trump tallies his first six weeks into the job. The top-line of the studies is that the percent of people in America feeling financially wobbly has increased since the fourth quarter of 2024. I’ll review these studies in this post, and discuss several potential impacts we should keep in mind for peoples’ health and
Improve Sleep, Improve the World and Health: ResMed’s Look at Global Sleep Trends

The world would be a better place if we had more, and better quality sleep. That’s the hopeful conclusion from the fifth annual Global Sleep Survey from ResMed. ResMed’s global reach with the sleeping public enabled the company to access the perspectives of over 30,000 respondents in 13 markets, finding that one in 3 people have trouble falling or staying asleep 3 or more times a week. We now live in “a world struggling with poor sleep” — “a world without rest,” ResMed coins our sleepless situation. The irony is that most people believe
Health Consumer Check-In: From Digital Detox to Analog Wellness, Social Re-Wilding, and a Return to the Bookstore

As humans have undergone personal digital transformations, living omni-channel and appreciating the conveniences that being switched-on can bring, there’s a growing demand for “analog wellness.” That’s one of ten trends covered in the Global Wellness Institute’s (GWI) report on 2025 Wellness Trends, and one I want to dig into early this year as consumers are facing growing challenges to our privacy, social bullying, and workforce stressors compelling many employees to spend too many hours in digital isolation and loneliness. To paint the larger landscape of and drivers underpinning analog wellness, I will weave several important reports and studies together, all
The Rough Guide to Health/Care Consumers in 2025: The 2025 Health Populi TrendCast

At this year-end time each year, my gift to Health Populi readers is an annual “TrendCast,” weaving together key data and stories at the convergence of people, health care, and technology with a look into the next 1-3 years. If you don’t know my work and “me,” my lens is through health economics broadly defined: I use a slash mark between “health” and “care” because of this orientation, which goes well beyond traditional measurement of how health care spending is included in a nation’s gross domestic product (GDP); I consider health across the many dimensions important to people, addressing physical,
National Healthcare Spending in the U.S. Was Nearly $5 Trillion (with a “T”) in 2023 – New Data from CMS
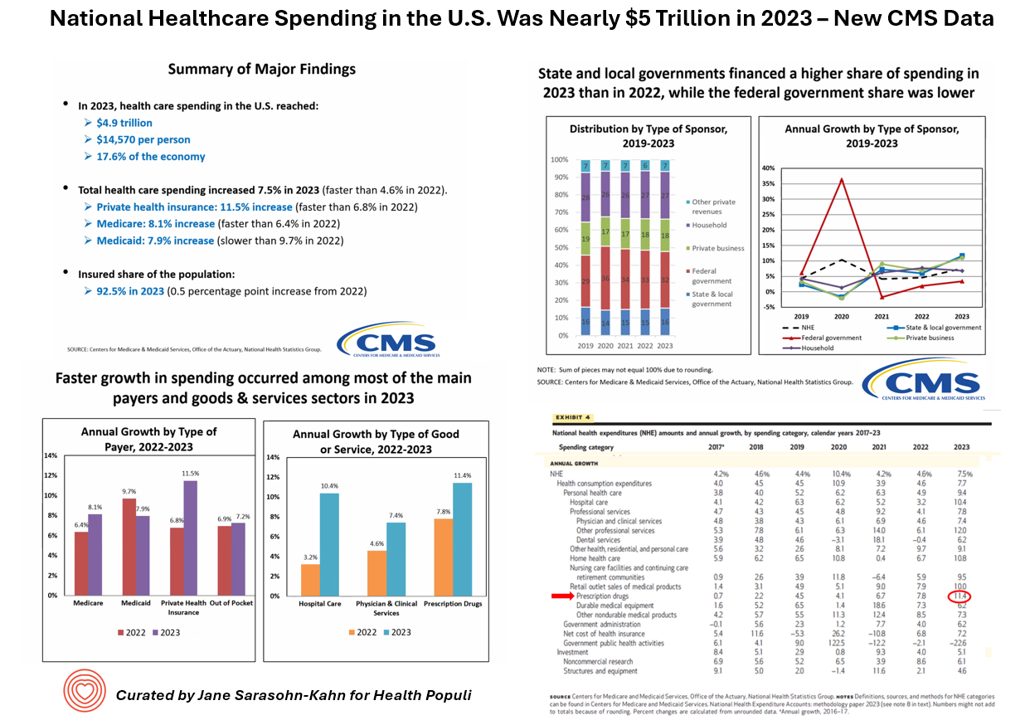
What would $5 trillion be valued around the world or on the stock market? The economy of Germany was gauged around $5 trillion in 2024. India could be the world’s 3rd largest economy by 2026 valued at $5 trillion. Nvidia could be a $5 trillion company in 2025, as could Amazon. But today we report out the latest data from the Centers for Medicare and Medicaid Services (CMS) that national health spending in America reached $4.9 trillion in 2023. The full report on national health expenditures (NHE) in the U.S. was published today in Health Affairs, which came off embargo
Workers Feel “Stuck,” Under-Insured, Financially Stressed, and Neglecting Mental Health
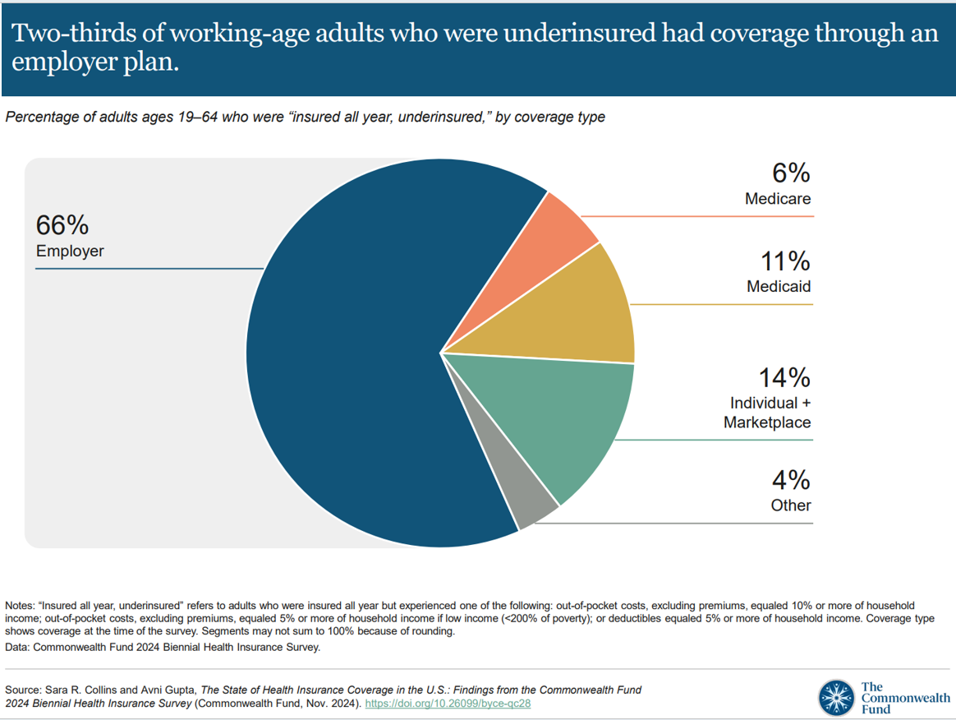
“It’s the economy stupid,” Jennifer Tescher, CEO of the Financial Health Network, titles her latest column in Forbes. Published two weeks after the 2024 U.S. elections, Jennifer’s assertion sums up what, ex post facto, we know about what most inspired American voters at the polls in November 2024: the economy, economics, inflation, the costs of daily living….pick your noun, but it’s all about those Benjamins right now for mainstream American consumers across many demographic cuts. With that realization, we must remind ourselves as we enter a new year under a second-term President Trump that health care spending for everyday people
What Stays True for U.S. Health Care Post #Election2024 (1) – Consumers’ Dissatisfaction with Drug Prices
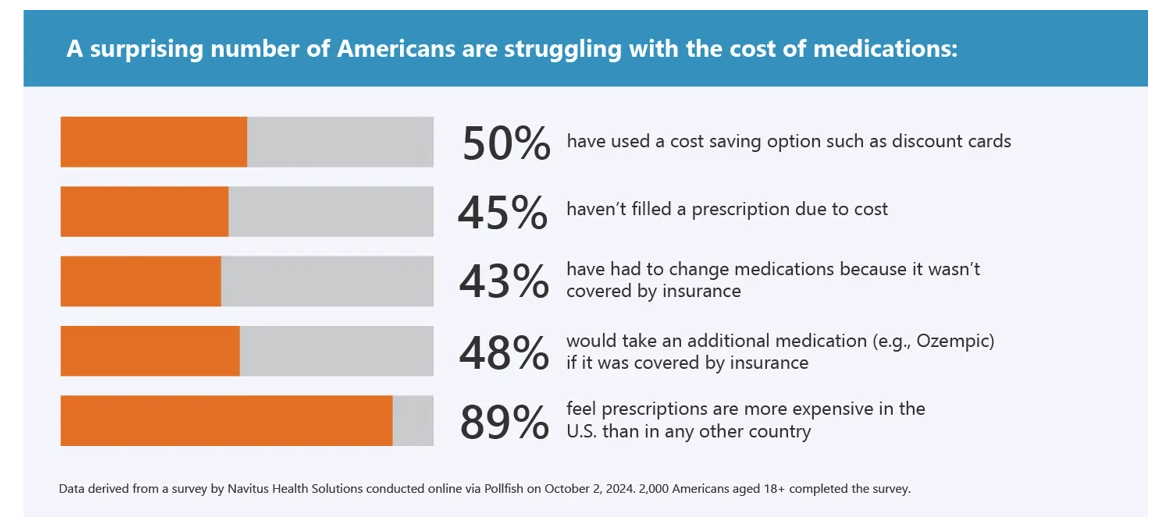
For health care, there are many uncertainties as we reflect, one week after the 2024 U.S. elections, on probably policy and market impacts that we can expect in 2025 and beyond. In today’s Health Populi post, I’ll reflect on the first of several certainties we-know-we-know about U.S. health citizens and key factors shaping the American health ecosystem. In this first of several posts on “What Stays True for U.S. Health Care Post #Election2024,” I’ll focus on U.S. consumer dissatisfaction with drug prices — across political party identification. Let’s set the context with data from a recently-published
How’s Life? Around the World – In the U.S., It’s the Sadness That Stands Out
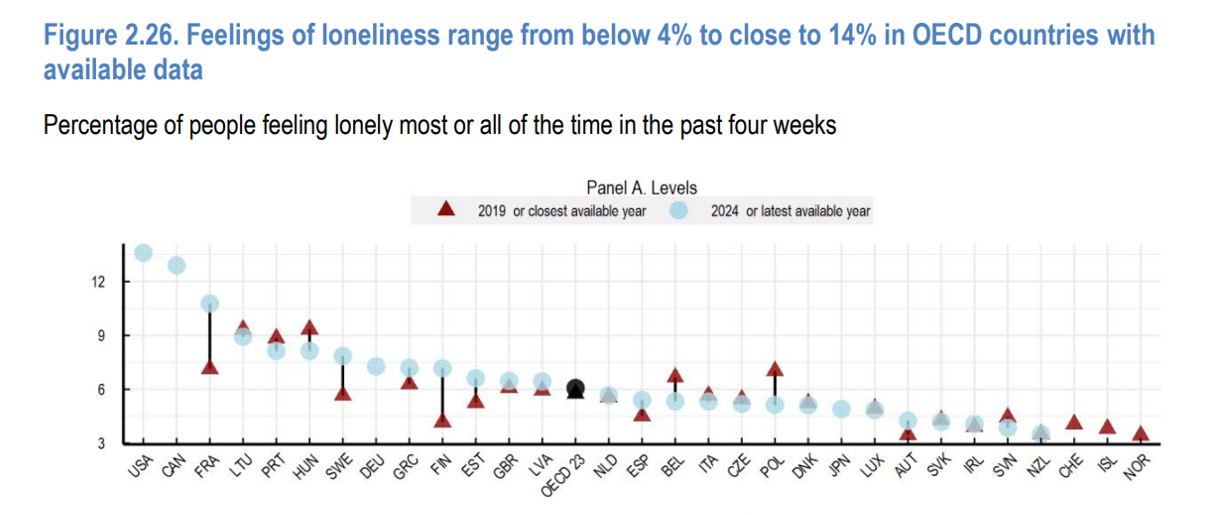
A new report from the OECD asks the question, “How’s Life?” with the tagline letting us know the plotline focuses on “well-being and resilience in times of crisis.” The Organization of Economic Cooperation and Development (OECD) has tracked the well-being of member nations for the past six years, taking a broad view on the definition of holistic health — including physical, mental, financial, and social aspects of people living in OECD countries. The first “How’s Life?” report was published at the height of the global financial crisis; the authors of this report introduce it saying that, “the
The Health Insurance Premium for a Family Averages $25,572 in 2024 – KFF’s Annual Update on Employer-Sponsored Benefits
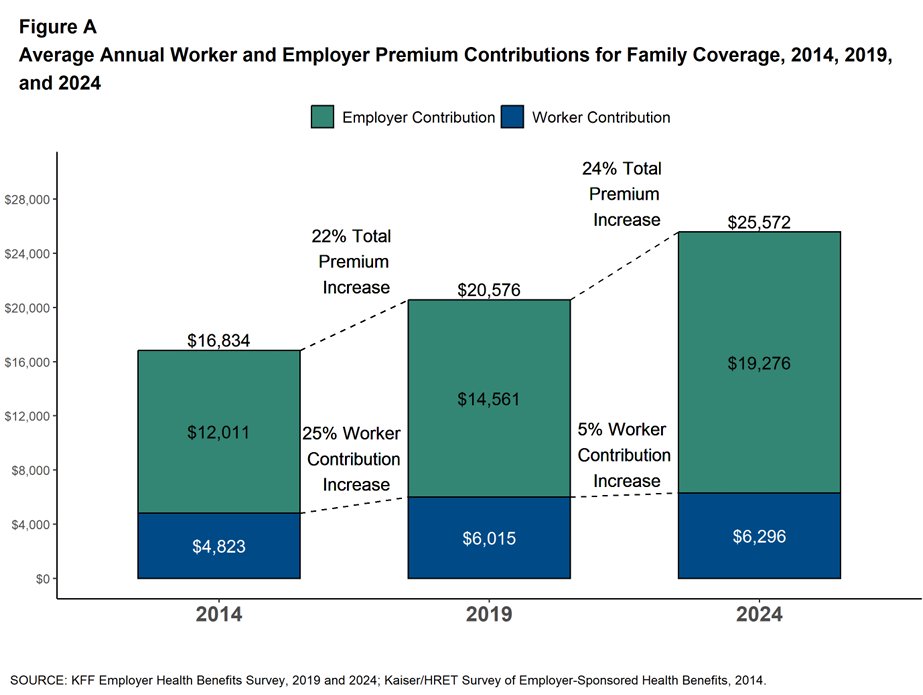
The premium for employer-sponsored health plans grew by 6-7% between 2023 and 2024, according to the report on Employer Health Benefits 2024 Annual Survey from the Kaiser Family Foundation, KFF’s 26th annual study into U.S. companies’ spending on workers’ health care. In 2024 the average annual health insurance premium for family coverage is $25,572, split by 75% covered by the employer (just over $19,000) and 25% borne by the employee ($6,296), shown in the first chart from the report. The nearly $26K family premium is the average across all plan types in the
Growing Investments in Digital Health Are Driven by Consumer Demand, Clinical Outcomes, and Cost-Savings
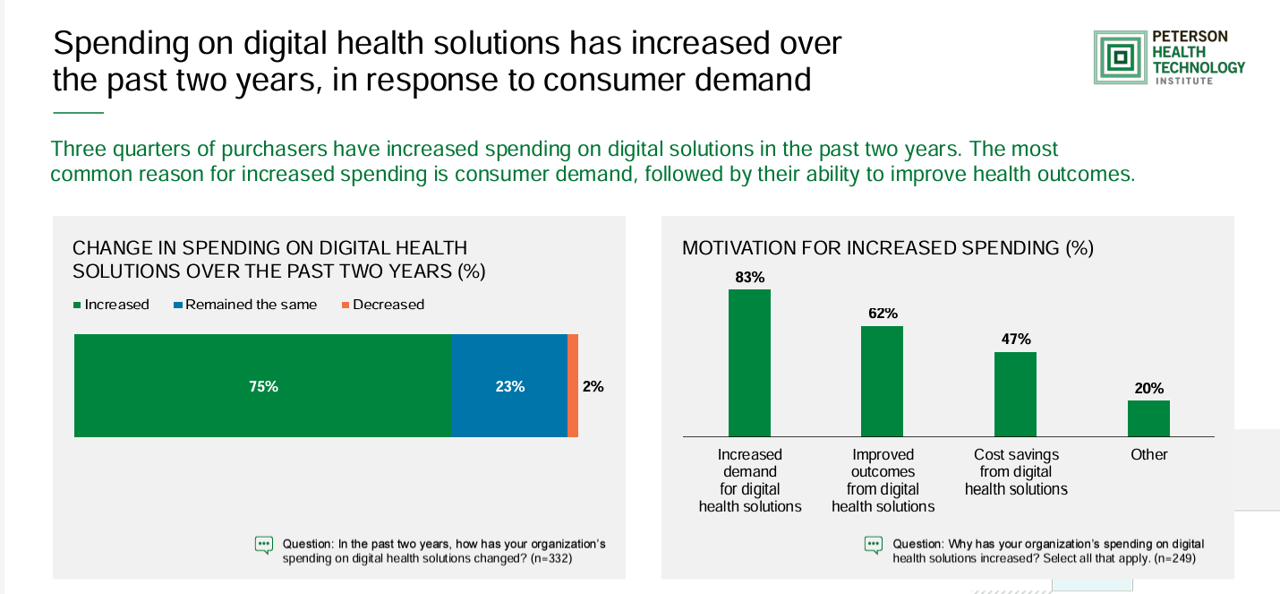
The marketing for purchasing digital health technologies is expecting to grow, driven by increased consumer demands for tech-based solutions, improved outcomes enabled through the innovations, and cost savings derived from deploying the technologies. That’s the top-line finding in the 2024 State of Digital Health Purchasing from the Peterson Health Technology Institute (PHTI). PHTI surveyed 322 digital health decision makers working in employers, health plans, and health systems, fielding the study in July and August 2024. 3 in 4 purchasers grew spending on digital health technologies in the past two years,
Obesity is a Public Health Epidemic in the U.S. — The Case for GLP-1 Coverage, Affordability and Equity

“If the U.S. were sensible, weight management would be treated as a public health issue,” David Cutler writes in the JAMA Health Forum dated August 15, 2024. Dr. Cutler, distinguished economics professor at Harvard, talks about “the pathology of U.S. health care” citing the example of weight loss medications — in short, the uptake of GLP-1 drugs to address Type 2 diabetes first, and subsequently obesity. Dr. Cutler notes that the price of these drugs in the U.S. “far exceeds” that of other countries: specifically, 9 times that of the prices in Germany and the Netherlands
The Cost of GLP-1 Drugs on Payers’ Minds as Nearly 1/3rd of U.S. Consumers Could Become Users
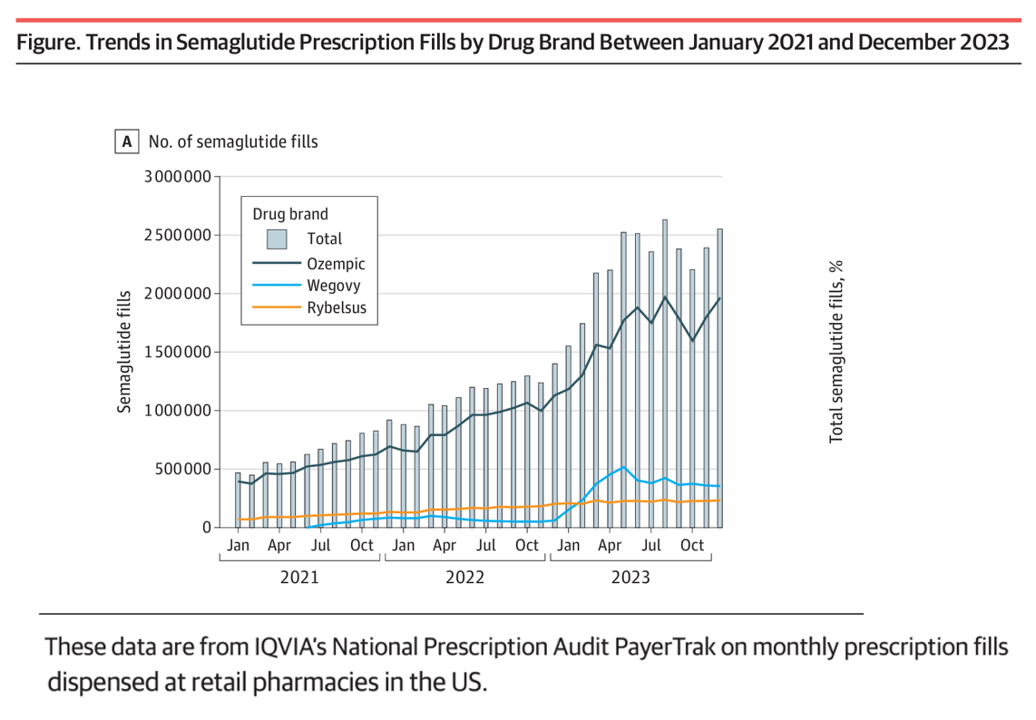
With 70 different clinical trials for GLP-1 drugs in process with the FDA, payers — and other stakeholders in the health care ecosystem — have the semaglutide-SENSE top of mind, based on my ongoing updating of this fast-moving market space. For overall market context on pace-of-growth in adoption, check out this chart from a JAMA Health Forum research letter on Prescription Fills for Semaglutide Products by Payment Method, published August 2nd. The study was based on the IQVIA National Prescription Audit PayerTrak data which captures 92% of Rx’s filled at retail pharmacies in
Medical Debt, Aflac on Eroding Health Benefits, the CBO’s Uninsured Forecast & Who Pays for Rising Health Care Prices: A Health Consumer Financial Update
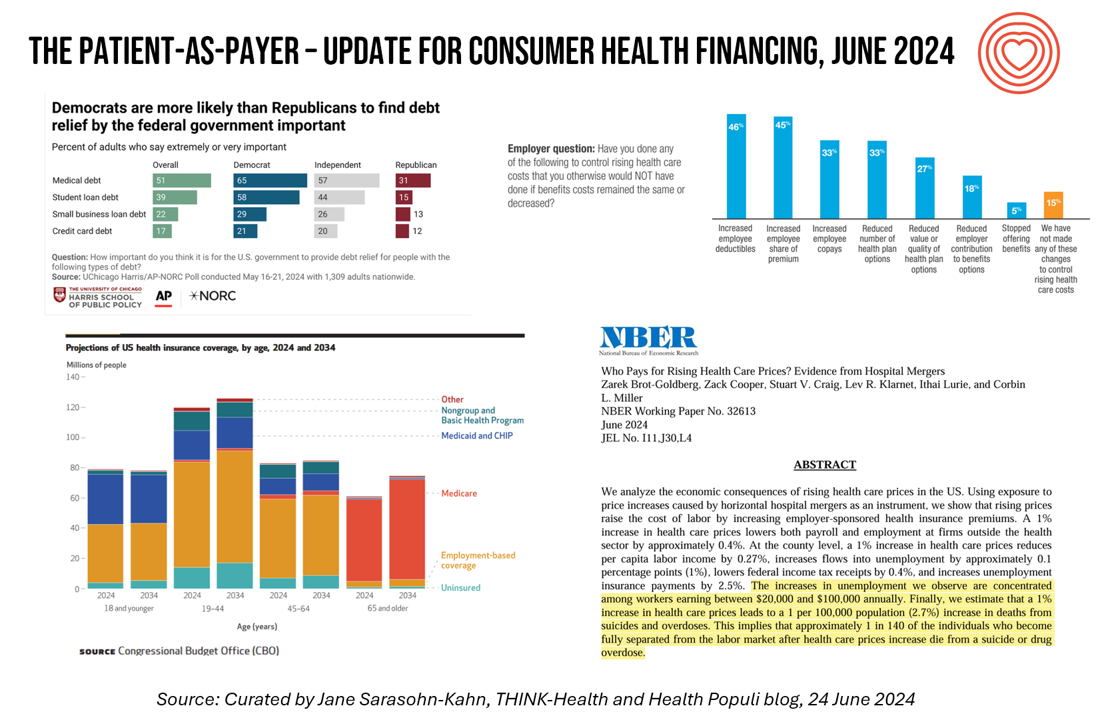
On June 11, Rohit Chopra, the Director of the Consumer Financial Protection Bureau (CFPB) announced the agency’s vision to ban Americans’ medical debt from credit reports. He called out that, “In recent years, however, medical bills became the most common collection item on credit reports. Research from the Consumer Financial Protection Bureau in 2022 showed that medical collections tradelines appeared on 43 million credit reports, and that 58 percent of bills that were in collections and on people’s credit records were medical bills.” Chopra further explained that medical debt on a consumer credit report was quite different than other kinds
A 2025 Subaru Forester, a Year at U-New Mexico, or a Health Plan for a Family of Four: the 2024 Milliman Medical Index
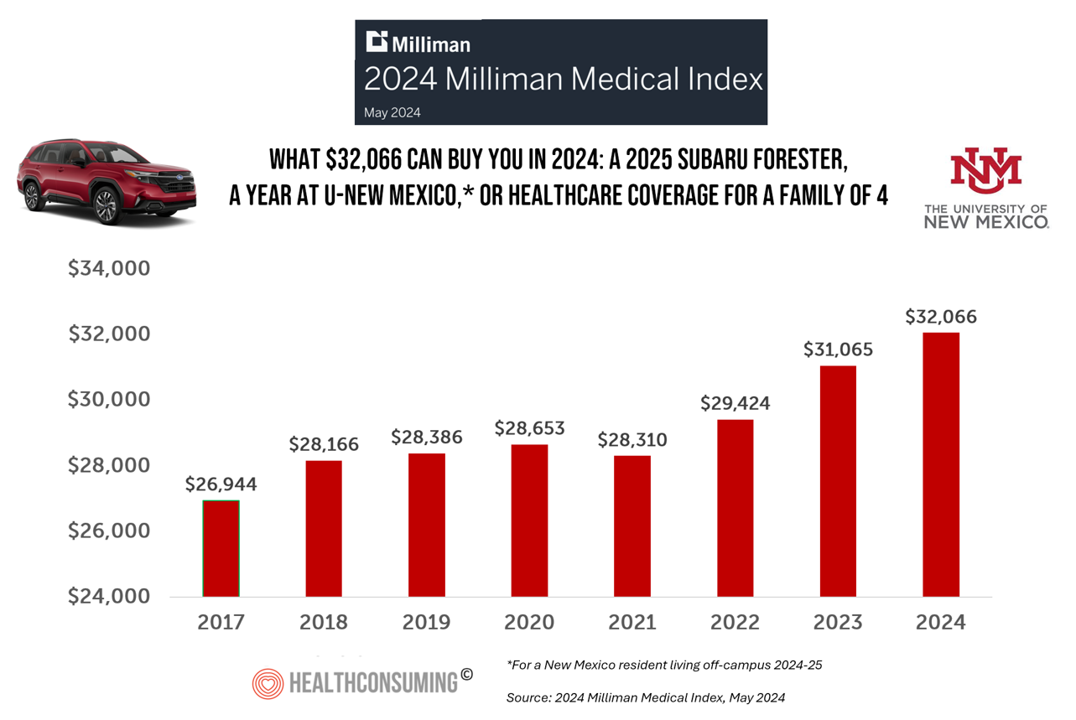
Health care costs for an “average” person covered by an employer-sponsored PPO in the U.S. rose 6.7% between 2023 and 2024, according to the 2024 Milliman Medical Index. Milliman also calculated that the largest driver of cost increase in health care, accounting for nearly one-half of medical cost increases, was pharmacy, the cost of prescription drugs, which grew 13% in the year. The big number this year is $32,066, which is the cost of that employer-sponsored PPO for a family of 4 in 2024. I’ve curated the chart of the MMI statistic for many
The Thematic Roadmap for AHIP 2024: What the Health Insurance Conference Will Cover

Health insurance plans make mainstream media news every week, whether coverage deals with the cost of a plan, the cost of out-of-network care, prior authorizations, or cybersecurity and ransomware attacks, among other front-page issues. This week, AHIP (the acronym for the industry association of America’s Health Insurance Plans) is convening in Las Vegas for its largest annual 2024 meeting. We expect at least 2,400 attendees registered for the meeting, and they’ll not just be representing the health insurance industry itself; folks will attend #AHIP2024 from other industry segments including pharmaceuticals, technology, hospitals and health systems, and the investment and financial services
Inflation, Health, and the American Consumer – “The Devil Wears Kirkland”
The Wall Street Journal reported yesterday that surging hospital prices are helping to keep inflation high. Hospital costs rose 7.7% last month, the highest increase in 13 years. This chart from WSJ’s reporting illustrates the >2x change in the CPI for hospitals vs the overall rate of price increases. Hospitals are not alone in price cliffs, with health insurance premiums spiking last year at the fastest rate in a decade, the Labor Statistics data showed. “For patients and their employers, the increases have meant higher health-insurance premiums, as well as limiting wage
Healthcare 2030: Are We Consumers, CEOs, Health Citizens, or Castaways? 4 Scenarios On the Future of Health Care and Who We Are – Part 2
This post follows up Part 1 of a two-part series I’ve prepared in advance of the AHIP 2024 conference where I’ll be brainstorming these scenarios with a panel of folks who know their stuff in technology, health care and hospital systems, retail health, and pharmacy, among other key issues. Now, let’s dive into the four alternative futures built off of our two driving forces we discussed in Part 1. The stories: 4 future health care worlds for 2030 My goal for this post and for the AHIP panel is to brainstorm what the person’s
Considering Equity and Consumer Impacts of GLP-1 Drugs – A UBS Economist Weighs In
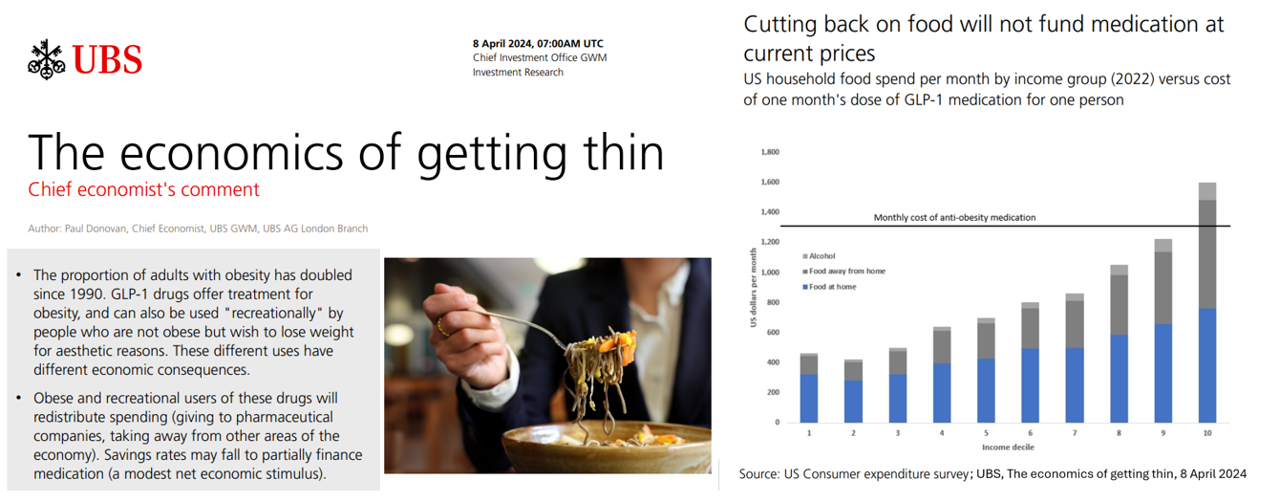
Since the introduction of GLP-1 drugs on the market, their use has split into two categories: for obesity and “recreationally,” according to the Chief Economist with UBS (formerly known as Union Bank of Switzerland). Paul Donovan, said economist, discusses The economics of getting thin in his regularly published comment blog. “These different uses have different economic consequences,” Donovan explains: Obese patients who use GLP-1s should become more productive employees, Donovan expects — less subject to prejudice, and less likely to be absent from work. While so-called recreational GLP-1 consumers may experience these
Peering Into the Hidden Lives of Patients: a Manifesto from Paytient and Nonfiction

Having health insurance in America is no guarantee of actually receiving health care. It’s a case of having health insurance as “necessary but not sufficient,” as the cost of deductibles, out-of-pocket coinsurance sharing, and delaying care paint the picture of The Hidden Lives of Workplace-Insured Americans. That’s the title of a new report that captures the results of a survey conducted in January 2024 among 1,516 employed Americans who received employer-sponsored health insurance. The study was commissioned by Paytient, a health care financial services company, engaging the research firm Nonfiction to conduct the study
The Women’s Health Gap Is Especially Wide During Her Working Years – Learning from McKinsey, the World Economic Forum, and AARP in Women’s History Month
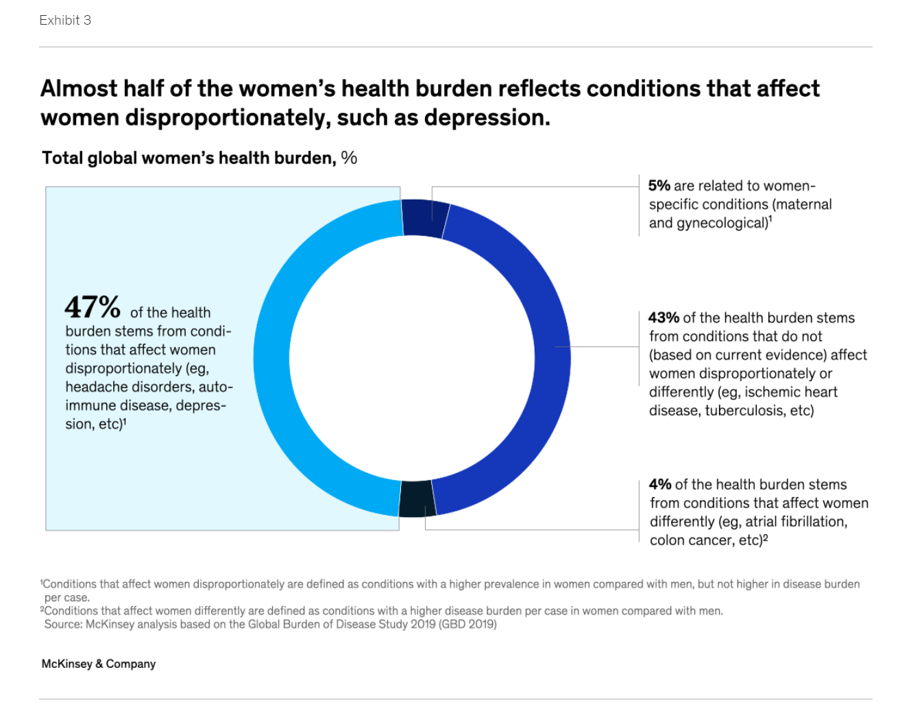
There’s a gender-health gap that hits women particularly hard when she is of working age — negatively impacting her own physical and financial health, along with that of the community and nation in which she lives. March being Women’s History Month, we’ve got a treasure-trove of reports to review — including several focusing on health. I’ll dive into two for this post, to focus in on the women’s health gap that’s especially wide during her working years. The reports cover research from the McKinsey Health Institute collaborating with the World Economic Forum on
A Health Consumer Bill of Rights: Assuring Affordability, Access, Autonomy, and Equity

Let’s put “health” back into the U.S. health care system. That’s the mantra coming out of this week’s annual Capitol Conference convened by the National Association of Benefits and Insurance Professionals (NABIP). (FYI you might know of NABIP by its former acronym, NAHU, the National Association of Health Underwriters). NABIP, whose members represent professionals in the health insurance benefits industry, drafted and adopted a new American Healthcare Consumer Bill of Rights launched at the meeting. While the digital health stakeholder community is convening this week at VIVE in Los Angeles to share innovations in health tech, NABIP
The Trust-Innovation Gap – Welcome to the 2024 Edelman Trust Barometer

If it’s January, it’s Davos-time — that is the annual meeting of the World Economic Forum convening global experts and passionistas focused on big ideas and challenges facing us mere humans living on Planet Earth. Parallel with the WEF is the annual publication of the 2024 Edelman Trust Barometer, now in its 24th year, focusing on global citizens’ concerns that unite people around the world. For the 2024 study, Edelman’s team fielded the survey in November 2023, collecting input from over 32,000 people living in 28 countries. About 1,150 interviews (plus or minus) were done in each nation which included
In 2024 U.S. Consumers Will Mash Financial Resolutions With Those For Physical Health and Mental Health, Fidelity Finds

One-third of U.S. consumers feel in worse financial shape now than in 2022, with inflation a top concern, discovered in the 2024 New Year’s Financial Resolutions Study from Fidelity Investments. In this 15th annual update of Fidelity’s research into Americans’ New Year’s resolutions for financial health, we learn the mantra that 2024 will be the year of living practically, opening new chapters for saving and paying down debt. Fidelity conducted an online poll among 3,002 U.S. adults 18 and over in October 2023 to gauge peoples’ perspectives on personal finances, and well-being currently and into 2024. This
Money and Mental Health in the U.S. – How Difficulty Paying Medical Bills Can Hurt Healing and Well-Being

There is growing evidence on the connection between people’s financial health and their mental health, explored and explained in Understanding the Mental-Financial Health Connection, a study published by the Financial Health Network. Keep that relationship in mind in the context of a new forecast from Kaiser Family Foundation estimate the 2023 cost for employer-sponsored insurance for a family to reach nearly $24,000 in 2023. That cost is a 7% increase over last year, and is expected to be split with companies covering $17K (about 70%) and employees about $6600 (roughly 30%). KFF heard that
Working in America: AI Is the Next Major Job Stressor
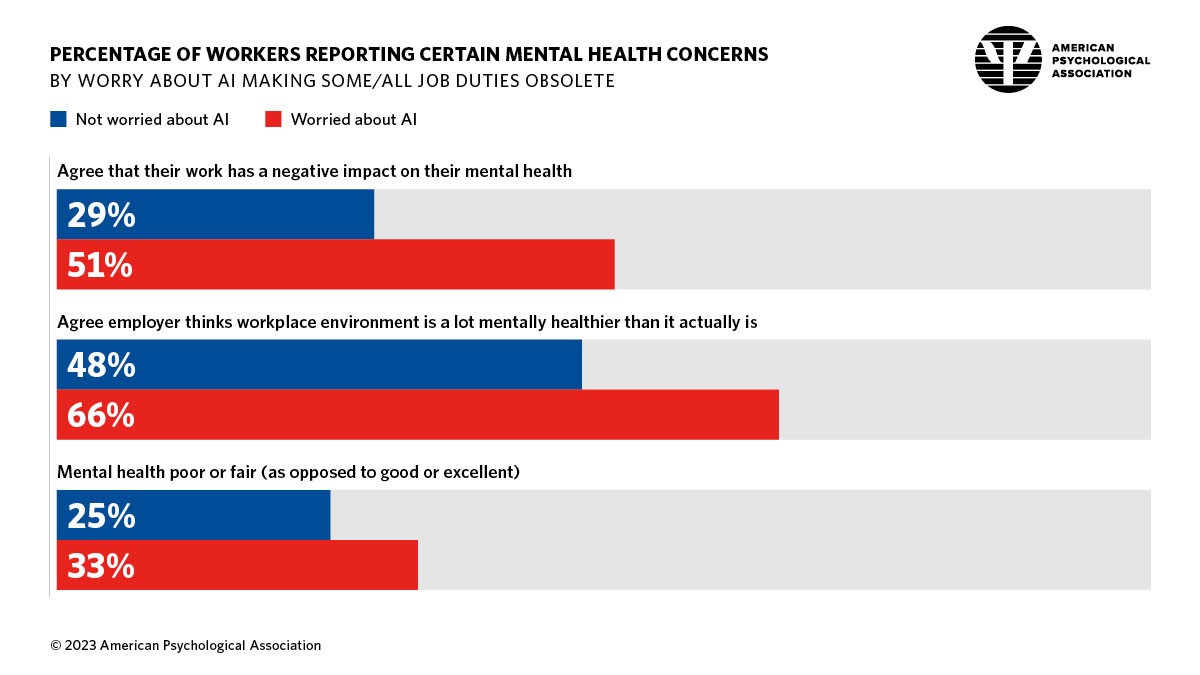
Workers in America are worried about the potential impacts that artificial intelligence (AI) could have on the workplace and jobs, according to Work in America: Artificial Intelligence, Monitoring Technology and Psychological Well-Being, a study from the American Psychological Association (APA). For many years, we’ve been tracking APA’s Stress in America studies gauging Americans’ mental health before the pandemic and during the pandemic. To social and political stress, we must now add in another stressor to peoples’ daily lives: concerns about AI and the potential for it to make one’s job obsolete, with the subsequent
Large Employers Expect More Employees Will Experience Prolonged Health Impacts Due to COVID-19. and a Note About Telehealth Engagement
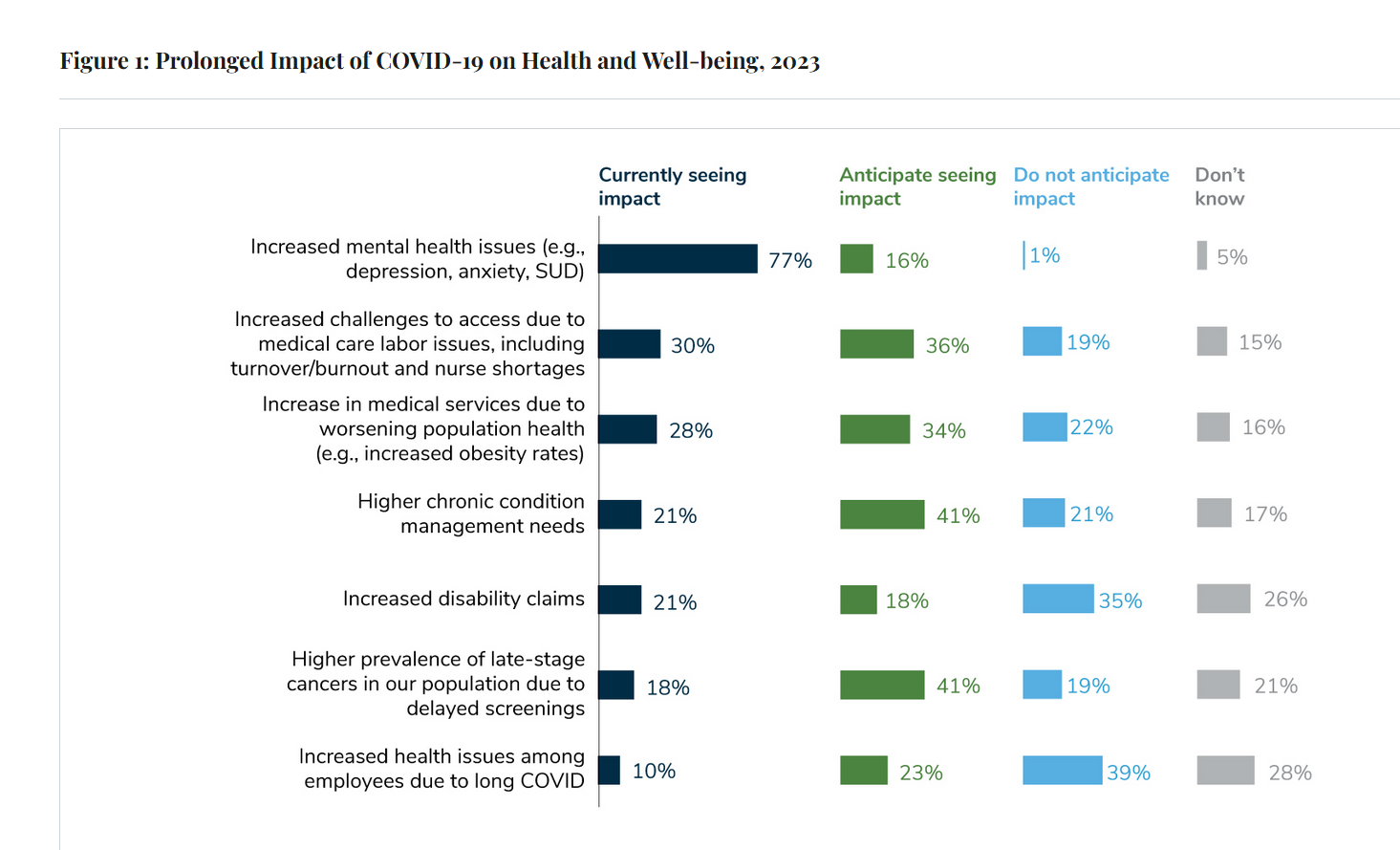
Due to their delayed return to medical services and diagnostic testing in the COVID-19 pandemic era, U.S. employees are expected to sustain serious health impacts that will drive employers’ health care costs, envisioned in the 2024 Large Employer Health Care Strategy Survey from the Business Group on Health (BGH). Dealing with mental health issues is the top health and well-being impact workers in large companies are addressing in 2023. Looking forward, large employers foresee their workers will be seeking care for chronic conditions and later-stage cancers that are diagnosed due to delayed screenings.
Hims and Hers and Hearts – Cardiology Blurs Into DTC Retail Health

Statin therapy has been used for decades to lower cholesterol with the goal of reducing mortality and preventing cardiovascular problems such as heart attacks and strokes. Hims & Hers announced a new service offering for health consumers and clinicians concerned about heart health called Heart Health by Hims. This is Hims & Hers’ first foray into cardiovascular health, working in collaboration with the American College of Cardiology (ACC). ACC clinical guidelines will inform the Hims’ provider platform for the program. “Prevention is the ideal mechanism to decrease cardiovascular events and ensure optimal heart
What $31,065 Can Buy You: a Toyota Corolla Cross Hybrid, a Year at Gnomon School, or Healthcare for a Family of 4 in America
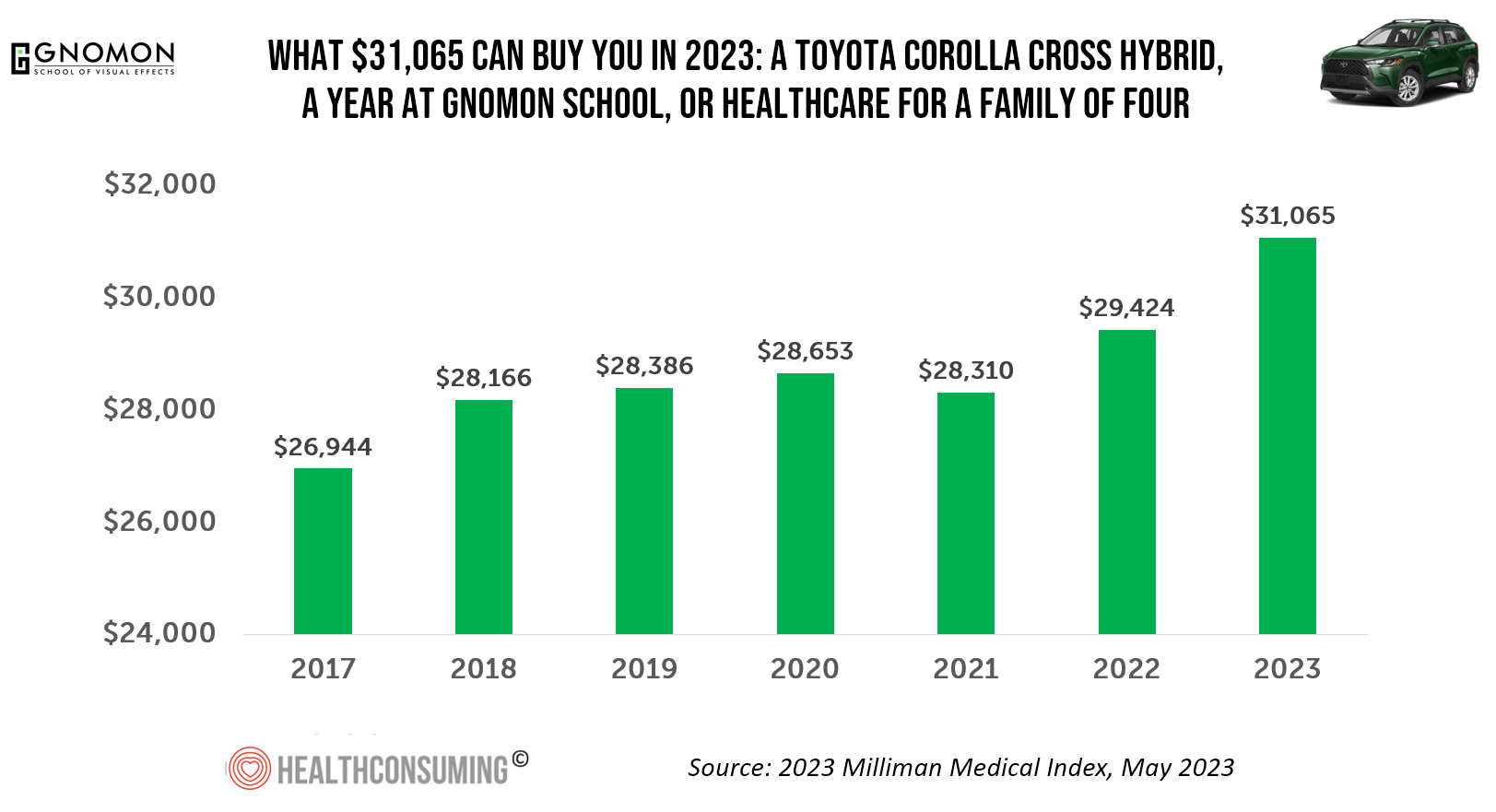
“Healthcare costs came roaring back in 2021” after falling in 2020. In 2023, that roaring growth in health care costs continues with expected growth of 5.6%. For 2023, you could take your $31K+ and buy a Toyota Corolla Cross Hybrid auto, fund a year at the Gnomon School in Hollywood toward a degree in animation or game design, or buy healthcare for your family of 4. Welcome to this year’s annual look at health care costs for a “typical” U.S. family explained in the 2023 Milliman Medical Index (MMI).
Getting Health Care at a Retail Pharmacy vs a Retail Store: Consumers May Be Favoring the Pharmacist Versus the Retailer
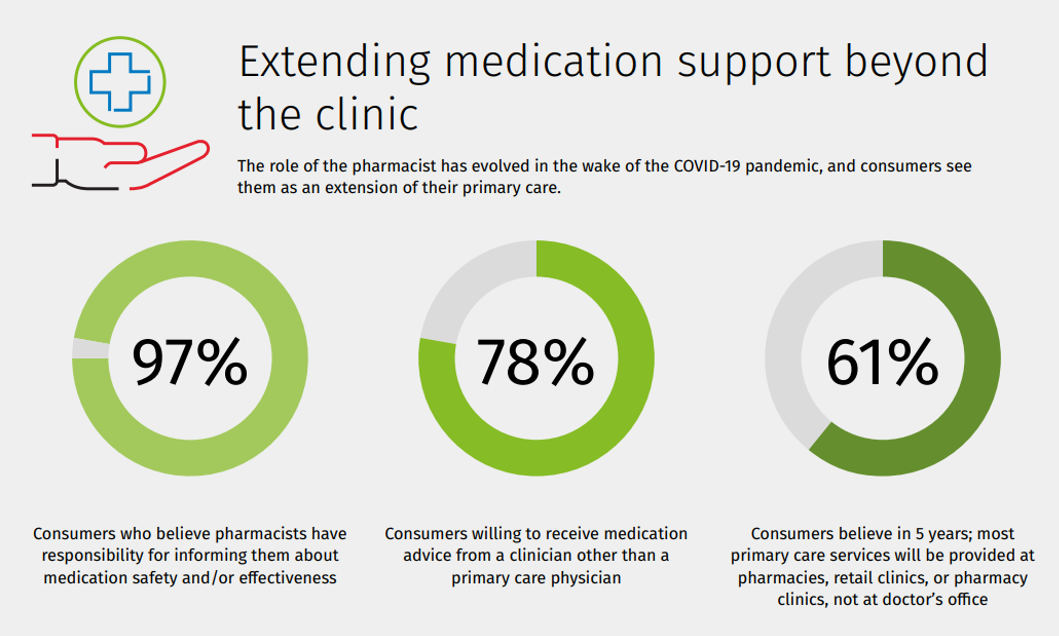
Not all “retail health” sites are created equal, U.S. consumers seem to be saying in a new study from Wolters Kluwer Health, the company’s second Pharmacy Next: Consumer Care and Cost Trends survey. Specifically, consumers have begun to differentiate between health care delivered at a retail pharmacy versus care offered at a retail store — such as Target or Walmart (both named as sites that offer “health clinics in department stores” in the study press release). While 58% of Americans were likely to visit a local pharmacy as a “first step” when faced with a non-emergency medical situation and 79%
The ROI on Feeling Cared-For At Work – Employer Trust, Love, and Building the Joyconomy
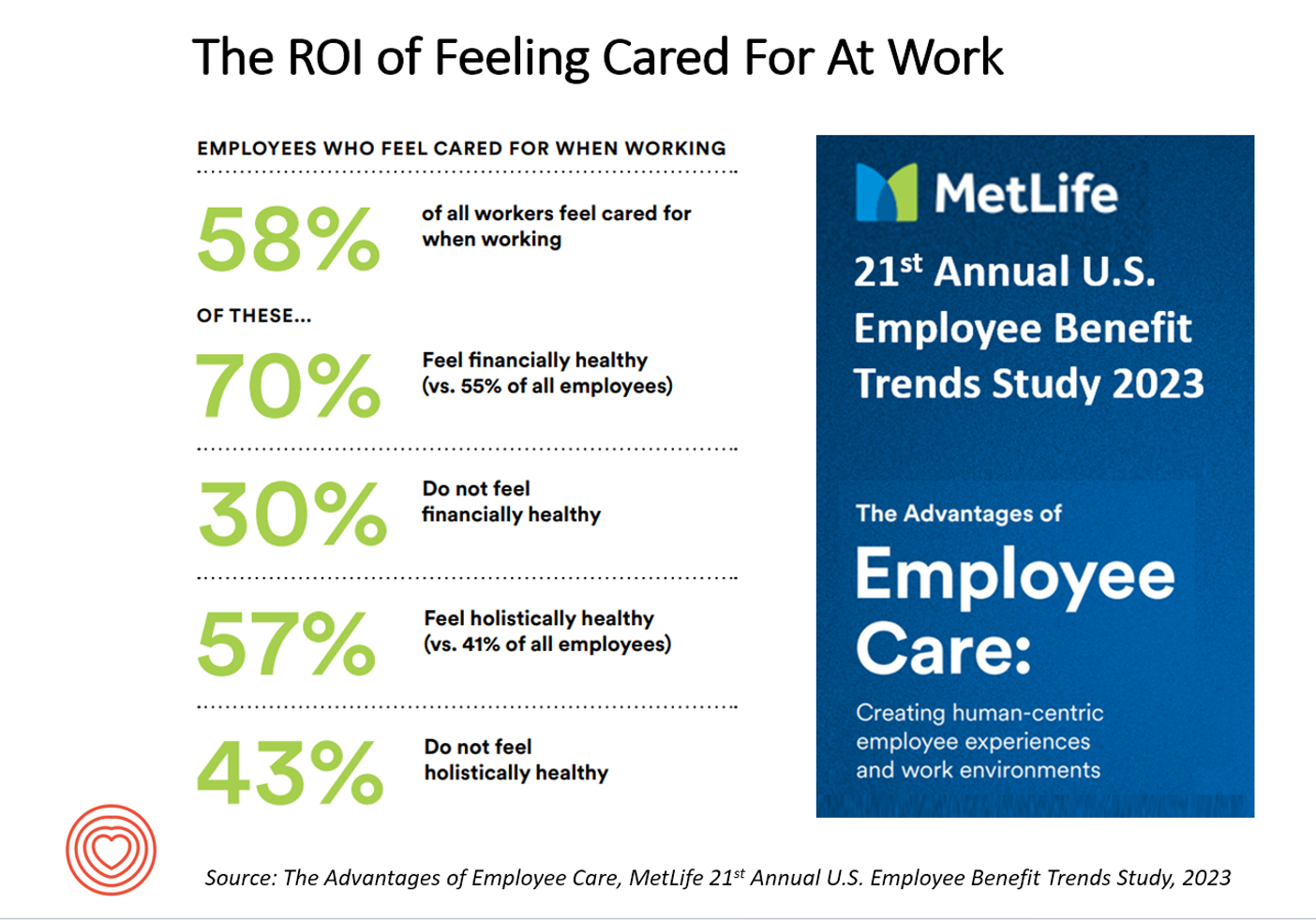
“Can employers afford not to care?” MetLife’s 21st annual U.S. Employee Benefit Trends Study asks and answers that question, with a resounding and evidence-based “NO.” I’m in Salt Lake City today discussing the drivers of health, “yesterday, today, and tomorrow” at the Virgin Pulse Thrive Summit, celebrating the ten-year anniversary of the company. As you would expect from an organization that is part of Richard Branson’s business ecosystem, the meeting will be energetically produced, delivering insights wrapped in info-taining ways. One of those features will be my being invited to create a
People Using Health Apps and Wearable Tech Most Likely Track Exercise and Heart Rate, Sleep and Weight – But Cost Is Still A Barrier
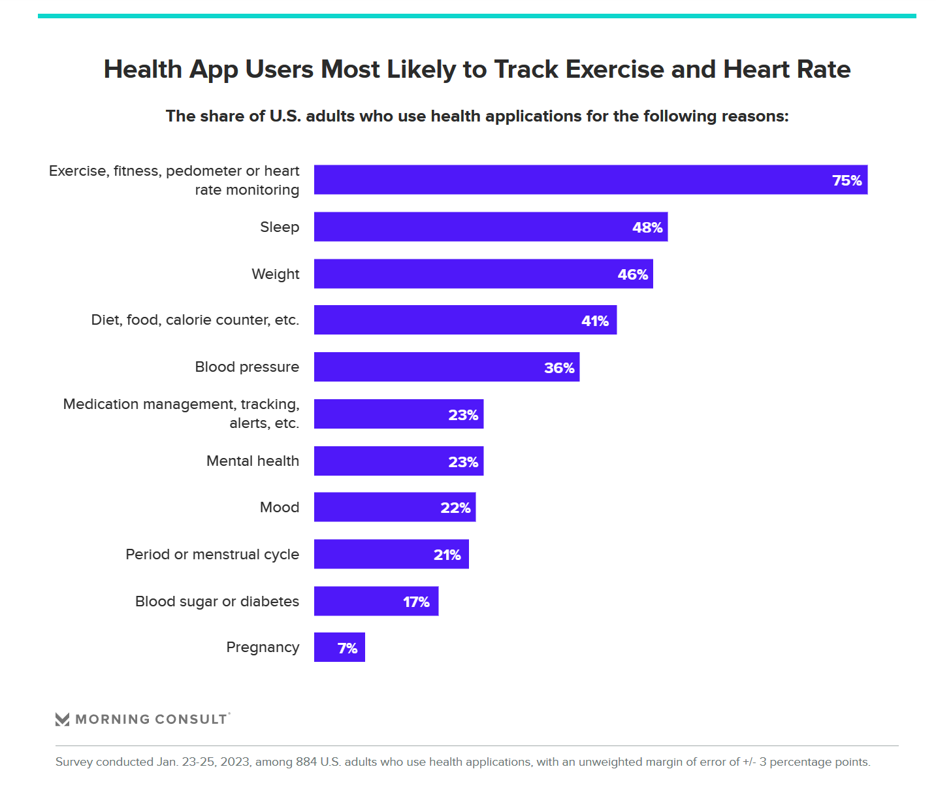
Over one in three U.S. consumers use a health app or wearable technology device to track some aspect of their health. “The public’s use of health apps and wearables has increased in recent years but digital health still has room to grow,” a new poll from Morning Consult asserts, published today. Among digital health tech users, most check into them at least once every day in the past month. One in four use these tech’s multiple times a day, the first pie chart illustrates. Eighteen percent of people use their digital
Wellness in 2023 Is About Connections, Mental Health and Science – Global Wellness Summit’s 2023 Trends

Consumers’ wellness life-flows and demands in 2023 will go well beyond exercise resolutions, eating more greens, and intermittent fasting as a foodstyle. It’s time for us to get the annual update on health consumers from the multi-faceted team who curated the Global Wellness Summit’s annual report on The Future of Wellness 2023 Trends. In this year’s look into wellness for the next few years, we see that health-oriented consumers are seeking solutions for dealing with loneliness and mental health, weight and hydration, travel-as-medicine as health destinations, and — not surprisingly —
When Household Economics Blur with Health, Technology and Trust – Health Populi’s 2023 TrendCast

People are sick of being sick, the New York Times tells us. “Which virus is it?” the title of the article updating the winter 2022-23 sick-season asked. Entering 2023, U.S. health citizens face physical, financial, and mental health challenges of a syndemic, inflation, and stress – all of which will shape peoples’ demand side for health care and digital technology, and a supply side of providers challenged by tech-enabled organizations with design and data chops. Start with pandemic ennui The universal state of well-being among us mere humans is pandemic ennui: call it languishing (as opposed to flourishing), burnout, or
Thinking Value-Based Health Care at HLTH 2022 – A Call-to-Action

The cost of health insurance for a worker who buys into a health plan at work in 2022 reached $22,463 for their family. The average monthly mortgage payment was $1,759 in mid-2022. “When housing and health both rank as basic needs in Maslow’s hierarchy, what’s a health system to do?” I ask in an essay published today on Crossover Health’s website titled Value-Based Care: Driving a Social Contract of Trust and Health. The answer: embrace value-based care. Warren Buffett wrote Berkshire Hathaway shareholders in 2008, asserting that, “Price is what you pay. Value
$22,463 Can Get You a Year of College in Connecticut, a Round of Ref Work in the Stanley Cup Playoffs, or Health Benefits for a Worker’s Family
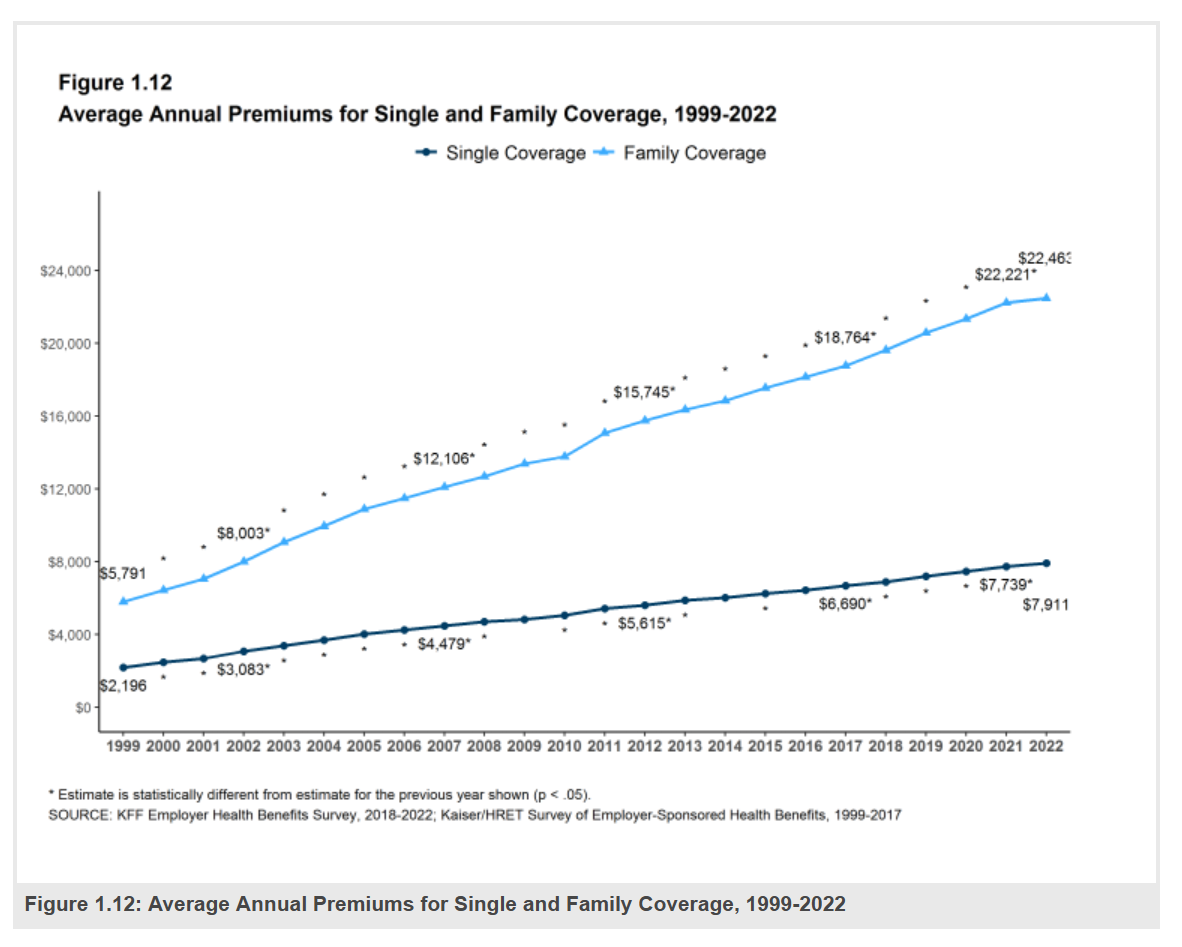
Employers covering health insurance for workers’ families will face insurance premiums reaching, on average, $22,463. That is roughly what a year at an independent college in Connecticut would cost, or a round of pay for a ref in the Stanley Cup playoffs. With that sticker-shock level of health plan costs, welcome to the 2022 Employer Health Benefits Survey from Kaiser Family Foundation, KFF’s annual study of employer-sponsored health care. Each year, KFF assembles data we use all year long for strategic and tactical planning in U.S. health care. This mega-study looks at
Virtual Care and Mental Health Top of Mind for Employers’ Workplaces in 2023
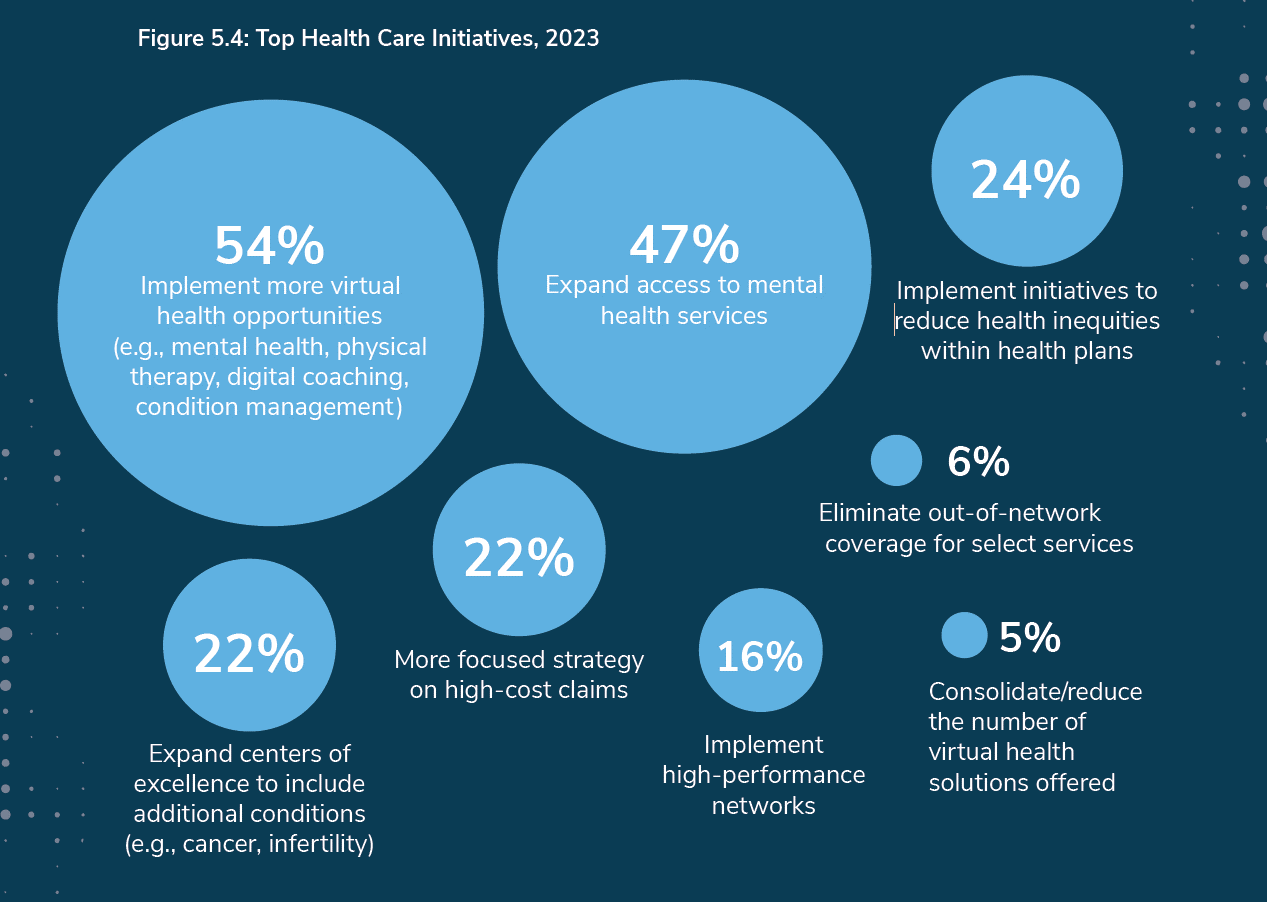
The concept that all companies are “health care companies” takes on greater import in the wake of the pandemic. The 2023 Large Employers’ Health Care Strategy and Plan Design Survey from the Business Group on Health (BGH) found that two in three large employers see their health and well-being strategy as an integral part of their overall workforce strategy. This is our annual go-to study guiding us on the private sector’s big thinking about health care plans and investments on workers’ behalf. The first line chart illustrates how this phenomenon shot up in importance for
The More Chronic Conditions, the More Likely a Patient Will Have Medical Debt
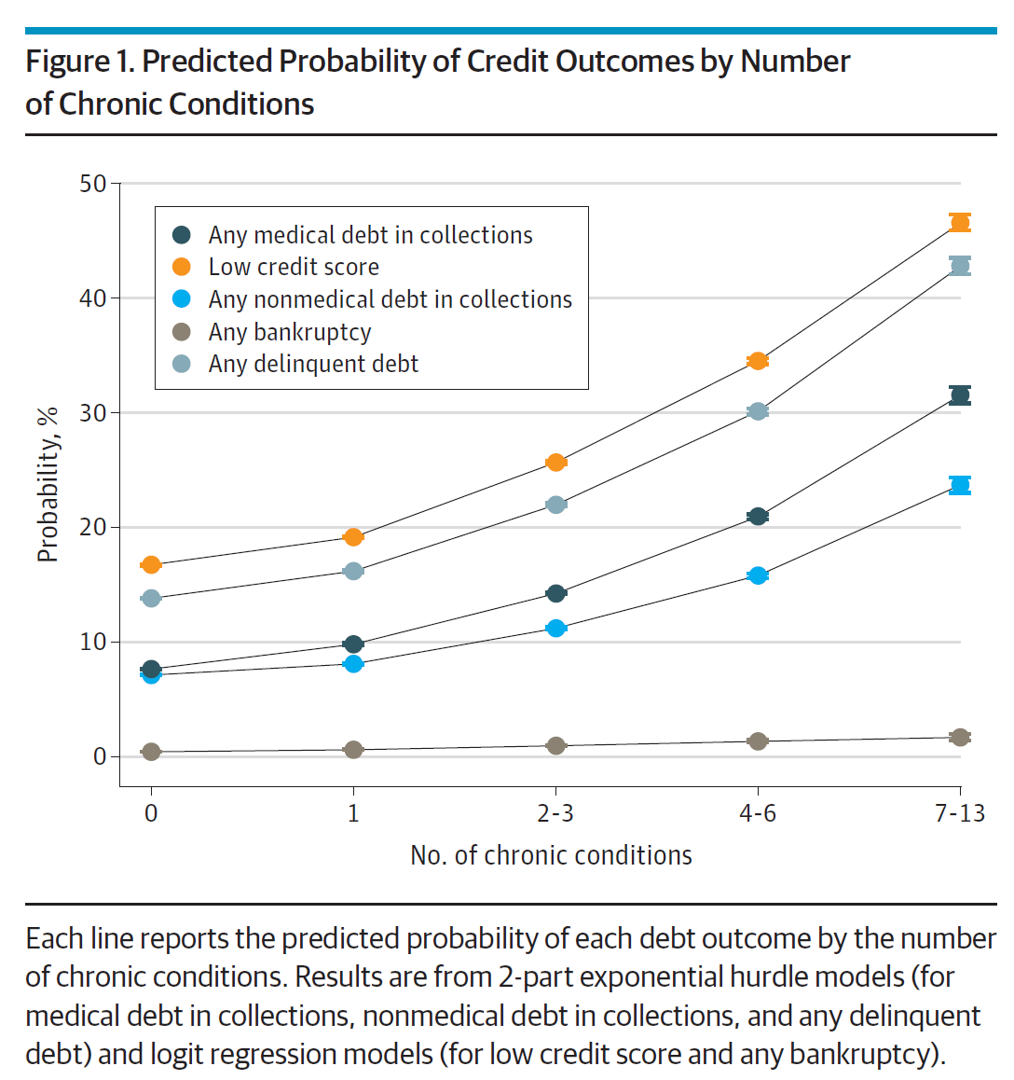
There is a direct association between a person’s health status and patient outcomes and their financial health, quantified in original research published this week in JAMA Internal Medicine. Researchers from the University of Michigan (my alma mater) Medical School and Institute for Healthcare Policy and Innovation analyzed two years of commercial insurance claims data generated between January 2019 and January 2021, linking to commercial credit data from January 2021 for patients enrolled in a preferred providers organization in Michigan. The first chart illustrates the predicted probability of credit outcomes based on the
The Retail Health Battle Royale in the U.S. – A Week-Long Brainstorm, Day 2 of 5 – Amazon and One Medical

Today we review the various viewpoints on Amazon’s announced acquisition of One Medical (ONEM, aka 1life Healthcare) which has been a huge story in both health care trade publications, business news, and mainstream media outlets. Welcome to Day 2 of The Retail Health Battle Royale in the U.S., my week-long update of the American retail health/care ecosystem weaving the latest updates from the market and implications and import for health care consumers. The deal was announced on 21 July, with Amazon striking the price at about $3.9 billion. Goldman Sachs and Morgan Stanley put the deal together,
In A Declining Consumer Tech Spending Forecast, Consumer Health Tech Will Grow in 2022: Reading the CTA Tea Leaves
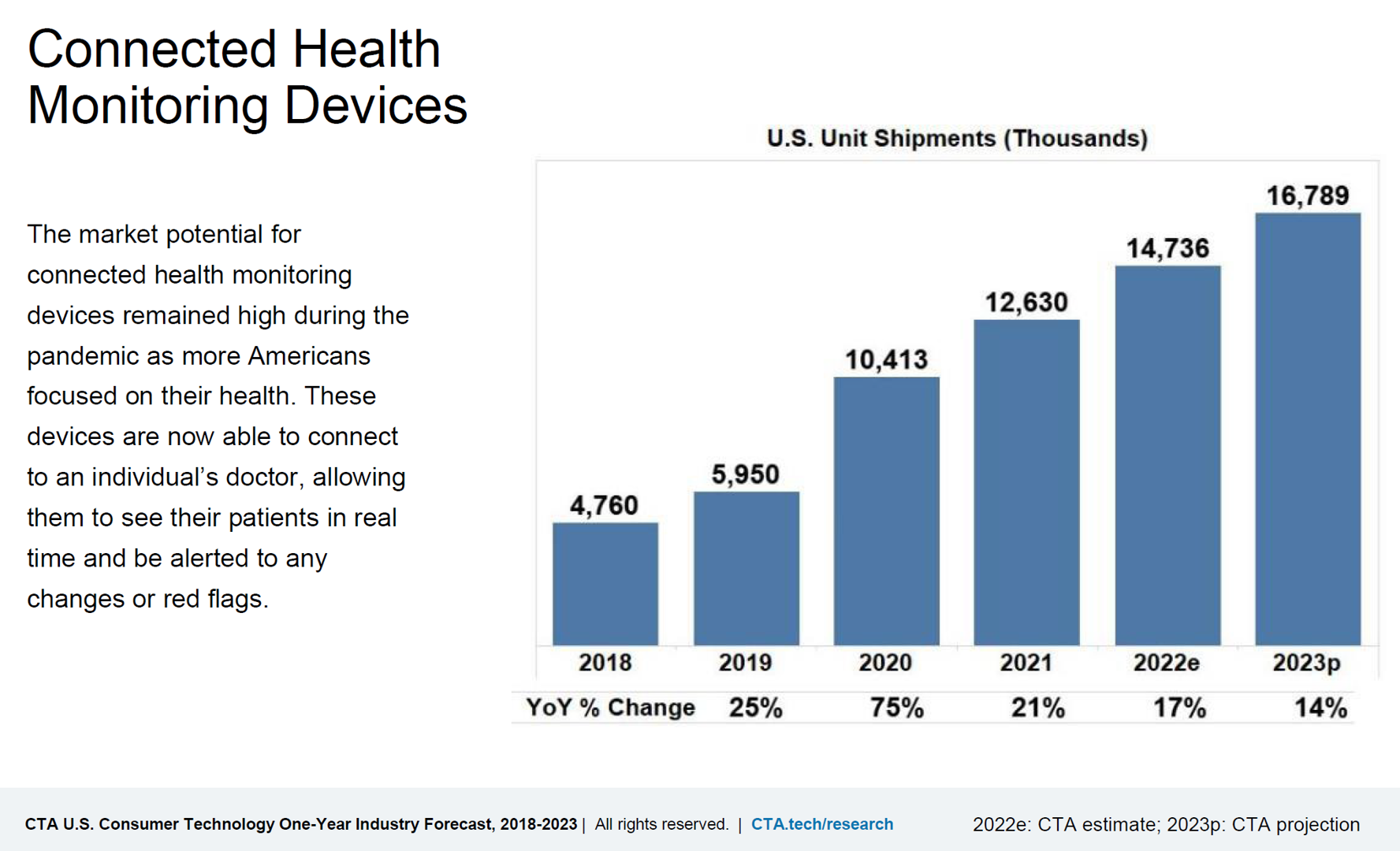
Supply chain challenges, inflation, and plummeting consumer economic sentiment are setting the stage for a decline in consumer electronics revenues for 2022. However, there will be some bright spots of growth for consumer tech spending, for 5G smartphones, smart home applications, gaming, and health technologies, noted in the Consumer Technology Association’s CTA U.S. Consumer Technology One-Year Industry Forecast, 2018-2023. Underneath the overall industry spend of $503 billion, a 0.2% drop from 2021, CTA expects software, gaming, video and audio streaming spending will grow by 3.5% and hardware to fall by 1.4% this year. With
Consumers’ Dilemma: Health and Wealth, Smartwatches and Transparency

Even as spending on healthcare per person in the United States is twice as much as other wealthy countries in the world, Americans’ health status ranks rock bottom versus those other rich nations. The U.S. health system continues to be marred by health inequalities and access challenges for man health citizens. Furthermore, American workers’ rank top in the world for feeling burnout from and overworked on the job. Welcome to The Consumer Dilemma: Health and Wellness,, a report from GWI based on the firm’s ongoing consumer research on peoples’ perspectives in the wake of
Changing Views of Retirement and Health Post-COVID: Transamerica’s Look At Workers’ Disrupted Futures

As more than 1 in 3 U.S. workers were unemployed during the pandemic and another 38% had reductions in hours and pay, Americans’ personal forecasts and expectations for retirement have been disrupted and dislocated. In its look at The Road Ahead: Addressing Pandemic-Related Setbacks and Strengthening the U.S. Retirement System from the Tramsamerica Center for Retirement Studies (TCRS), we learn about the changing views of U.S. workers on their future work, income, savings, dreams and fears. Since 1988, TCRS has assessed workers’ perspectives on their futures, this year segmented the 10,003 adults
Use of Preventive Health Services Declined Among Commercially Insured People – With Big Differences in Telehealth for Non-White People, Castlight Finds
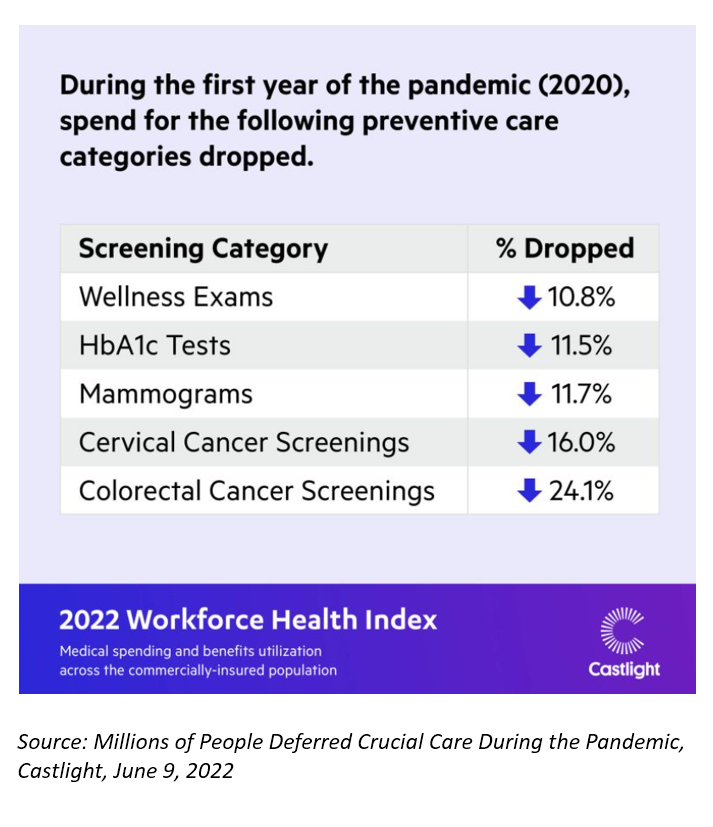
Declines in preventive care services like cancer screenings and blood glucose testing concern employers, whose continued to cover health insurance for employees during the pandemic. “As we enter the third year of the COVID-19 pandemic, employers continue to battle escalating clinical issues, including delayed care for chronic conditions, postponed preventive screenings, and the exponential increase in demand for behavioral health services,” the Chief Medical Officer for Castlight Health notes in an analysis of medical claims titled Millions of People Deferred Crucial Care During the Pandemic, published in June. The
A New Chevy Equinox SUV, a Year in Grad School, or Health Care for Four – The 2022 Milliman Medical Index
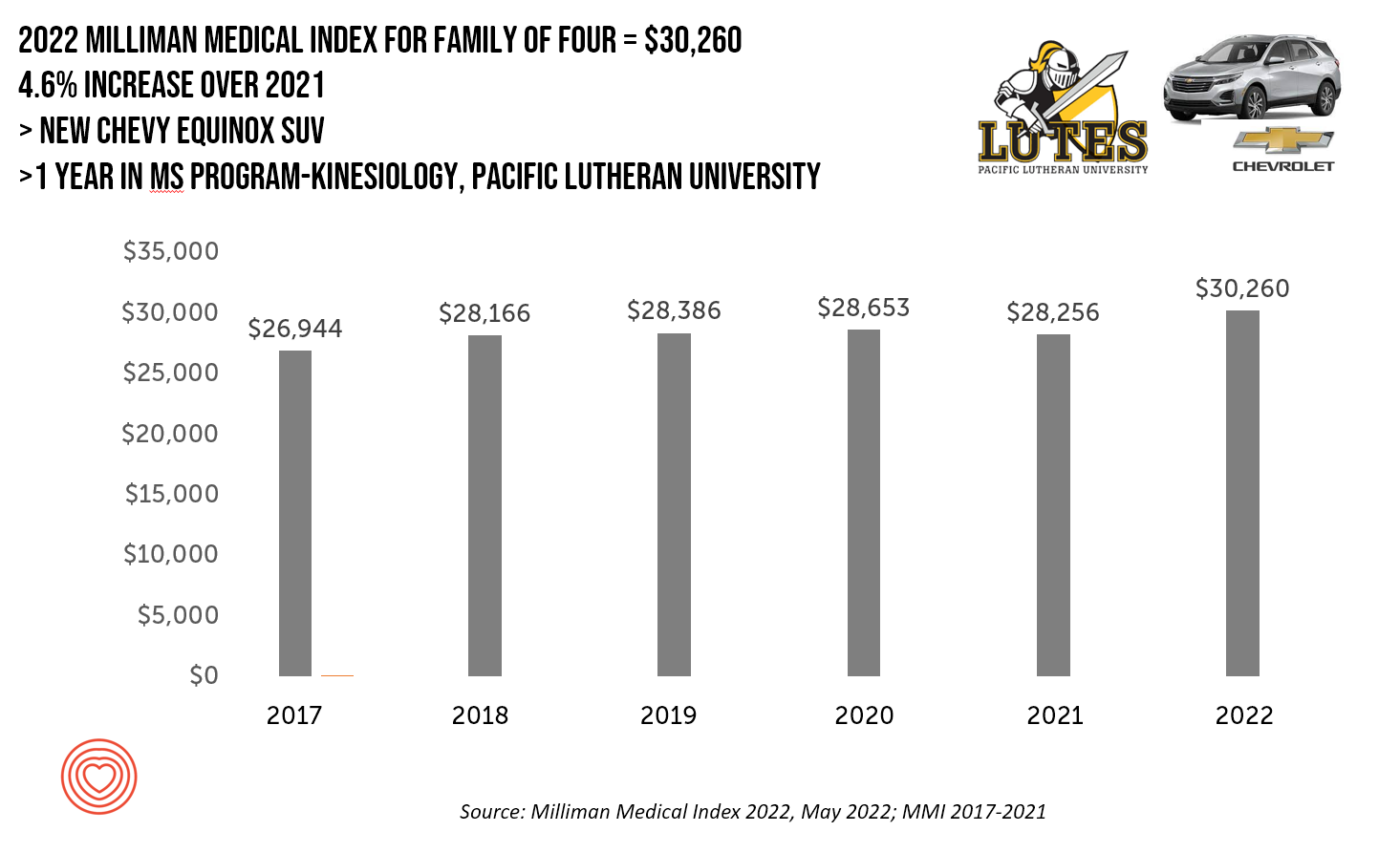
A new Chevy Equinox SUV, a year in an MS program in kinesiology at Pacific Lutheran U., or health care for a family of four. At $30,260, you could pick one of these three options. Welcome to this year’s 2022 Milliman Medical Index, which annually calculates the health care costs for a median family of 4 in the U.S. I perennially select two alternative purchases for you to consider aligning with the MMI medical index. I have often picked a new car at list price and a year’s tuition at a U.S. institution of
How Business Can Bolster Determinants of Health: The Marmot Review for Industry

“Until now, focus on….the social determinants of health has been for government and civil society. The private sector has not been involved in the discussion or, worse, has been seen as part of the problem. It is time this changed,” asserts the report, The Business of Health Equity: The Marmot Review for Industry, sponsored by Legal & General in collaboration with University College London (UCL) Institute of Health Equity, led by Sir Michael Marmot. Sir Michael has been researching and writing about social determinants of health and health equity for decades, culminating publications
McKinsey’s Six Shifts To Add Life to Years — and One More to Consider
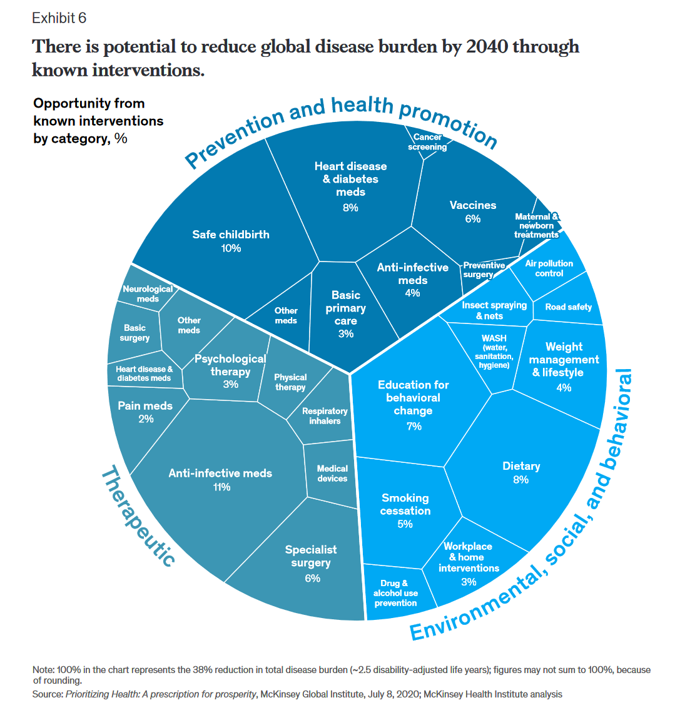
People spend one-half of their lives in “less-than-good health,” we learn early in the paper, Adding years to life and life to years from the McKinsey Health Institute. In this data-rich essay, the McKinsey team at MHI sets out an agenda that could help us add 45 billion extra years of higher-quality life equal to an average of six years per person (depending on your country and population demographics). The first graphic from the report illustrates four dimensions of health and the factors underneath each of them that can bolster or diminish our well-being: personal behaviors (such as sleep and diet),
Go Local and Go Beyond Medical Care: What Hospitals, Health Plans, and Pharma Can Do to Rebuild Trust

Without trust, people do not engage with health care providers, health plans, or life science companies….nor do many people accept “science fact.” I explore the sad state of Trust and Health Care. published in the Medecision Liberate Health blog, with a positive and constructive call-to-action for health care industry stakeholders to consider in re-building this basic driver of well-being. That is, trust as a determinant of health. Edelman’s 2022 Trust Barometer came out in January 2022, coinciding as it annually does with the World Economic Forum’s meeting in Davos, Switzerland. Every year, WEF convenes the world’s biggest thinkers to wrestle with the
The Trust Deficit Is Bad for Health: A Health/Care Lens on the 2022 Edelman Trust Barometer

“Health is the cornerstone to our core needs, thereby the cornerstone to trust.” So wrote Kirsty Graham, Global Leader of Sectors and Global Chair of Health at Edelman, in an essay explaining the 2022 Edelman Trust Barometer. If it’s January, it must be time for the World Economic Forum in Davos, the annual setting for Edelman’s launch of the company’s Trust Barometer. While WEF is mostly virtual this year due to the pandemic, Edelman has released the survey of global citizens’ views on trust in institutions right on-time and in full and sobering detail. I welcome and dig into the
Mental Health at CES 2022 – The Consumer’s Context for Wellbeing in the New Year

As we enter COVID-19’s “junior year,” one unifying experience shared by most humans are feelings of pandemic fatigue: anxiety, grief, burnout, which together diminish our mental health. There are many signposts pointing to the various flavors of mental and behavioral health challenges, from younger peoples’ greater risk of depression and suicide ideation to increased deaths of despair due to overdose among middle-aged people. And about one-in-three Americans has made a 2022 New Year’s resolution involving some aspect of mental health, the American Psychiatric Association noted approaching the 2021 winter holiday season. Underneath this overall statistic are important differences across various
The 2022 Health Populi TrendCast for Consumers and Health Citizens

I cannot recall a season when so many health consumer studies have been launched into my email inbox. While I have believed consumers’ health engagement has been The New Black for the bulk of my career span, the current Zeitgeist for health care consumerism reflects that futurist mantra: “”We tend to overestimate the effect of a technology in the short run and underestimate the effect in the long run,” coined by Roy Amara, past president of Institute for the Future. That well-used and timely observation is known as Amara’s Law. This feels especially apt right “now” as we enter 2022,
3 in 4 Insured Americans Worried About Medical Bills — Especially Women
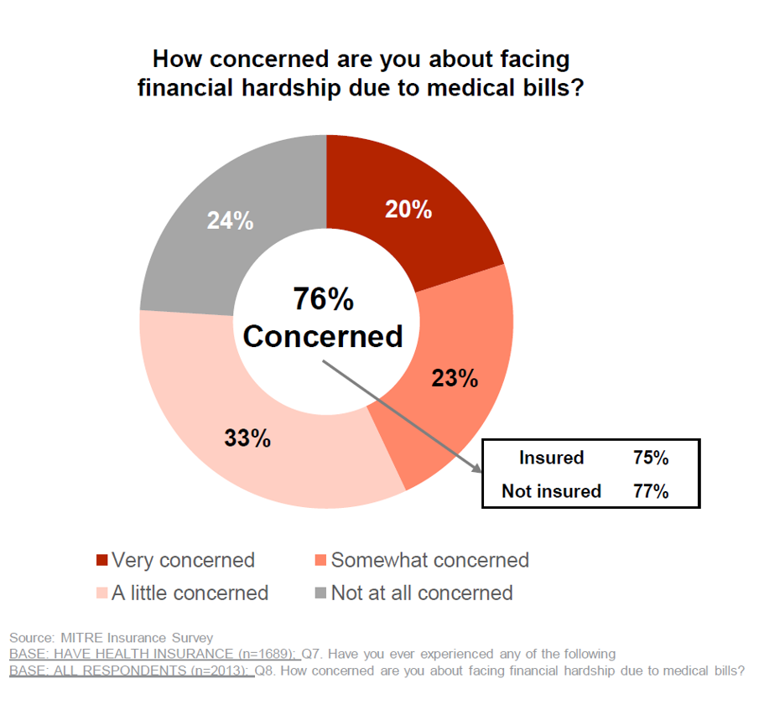
In the U.S., being covered by health insurance is one of the social determinants of health. Without a health plan, an uninsured person in America is far more likely to file for bankruptcy due to medical costs, and lack access to needed health care (and especially primary care). But even with health insurance coverage, most health-insured people are concerned about medical costs in America, found in a MITRE-Harris Poll on U.S. consumers’ health insurance perspectives published today. “Even those fortunate to have insurance struggle with bills that result from misunderstanding or underestimating costs of treatments and procedures,” Juliette Espinosa of
The Cost to Cover Health Insurance for a Family in America Is $22,221
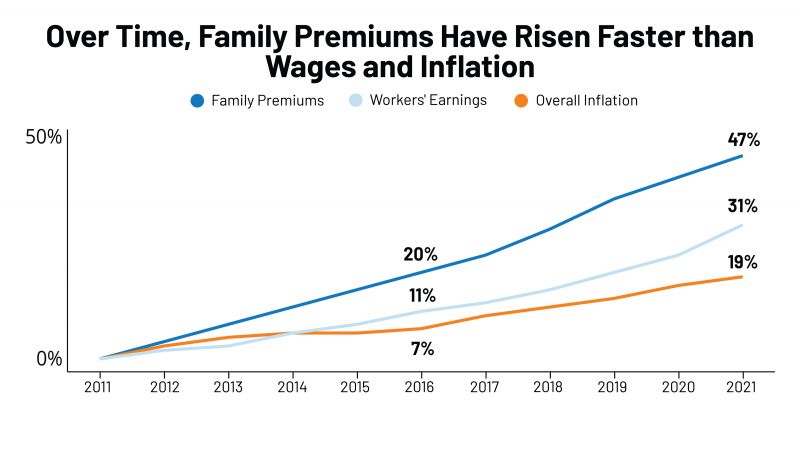
Even with growing inflation in the U.S. and post-pandemic job growth in 2021, the cost of health insurance premiums rose faster than either the price of goods or wages. That family health plan premium reached $22,221, an increase of 22% since 2016, we learn in the annual report from Kaiser Family Foundation, 2021 Employer Health Benefits Survey. This report is our go-to encyclopedia of statistics on health insurance year-after-year, surveying companies’ annual health insurance strategies for coverage and tactics for managing spending and workers’ health outcomes. This 2021 update takes into account the impacts and influence of COVID-19 on workers’
Be Mindful About What Makes Health at HLTH

“More than a year and a half into the COVID-19 outbreak, the recent spread of the highly transmissible delta variant in the United States has extended severe financial and health problems in the lives of many households across the country — disproportionately impacting people of color and people with low income,” reports Household Experiences in America During the Delta Variant Outbreak, a new analysis from the Robert Wood Johnson Foundation, NPR, and the Harvard Chan School of Public Health. As the HLTH conference convenes over 6,000 digital health innovators live, in person, in Boston in the wake of the delta
Genentech’s Look Into the Mirror of Health Inequities

In 2020, Genentech launched its first study into health inequities. The company spelled out their rationale to undertake this research very clearly: “Through our work pursuing groundbreaking science and developing medicines for people with life-threatening diseases, we consistently witness an underrepresentation of non-white patients in clinical research. We have understood inequities and disproportionate enrollment in clinical trials existed, but nowhere could we find if patients of color had been directly asked: ‘why?’ So, we undertook a landmark study to elevate the perspectives of these medically disenfranchised individuals and reveal how this long-standing inequity impacts their relationships with the healthcare system
Chronic Medical Conditions, Mental Health, and Equity On Employers’ Minds for 2022 – Employee Health in the Wake of COVID-19
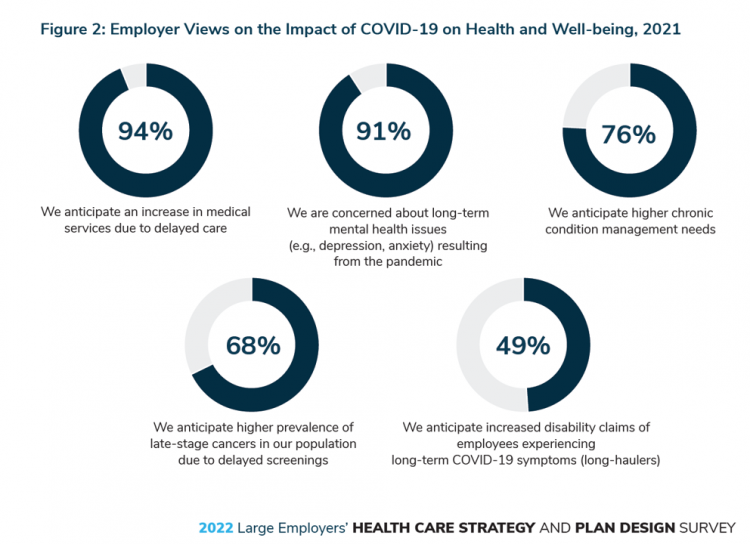
One in two people in the U.S. receive health insurance through employers. As large employers tend to be on the vanguard of benefit plan design, it’s useful to understand how these companies are thinking ahead on behalf of their employees. With that objective, it’s always instructive to explore the annual study from the Business Group on Health, the 2022 Large Employers’ Health Care Strategy and Plan Design Survey. As a result of the COVID-19 pandemic, large employees have many concerns about worker and dependents’ health. The biggest firms in America providing health insurance for workers are expecting an increase in
Why Is So Much “Patient Experience” Effort Focused on Financial Experience?
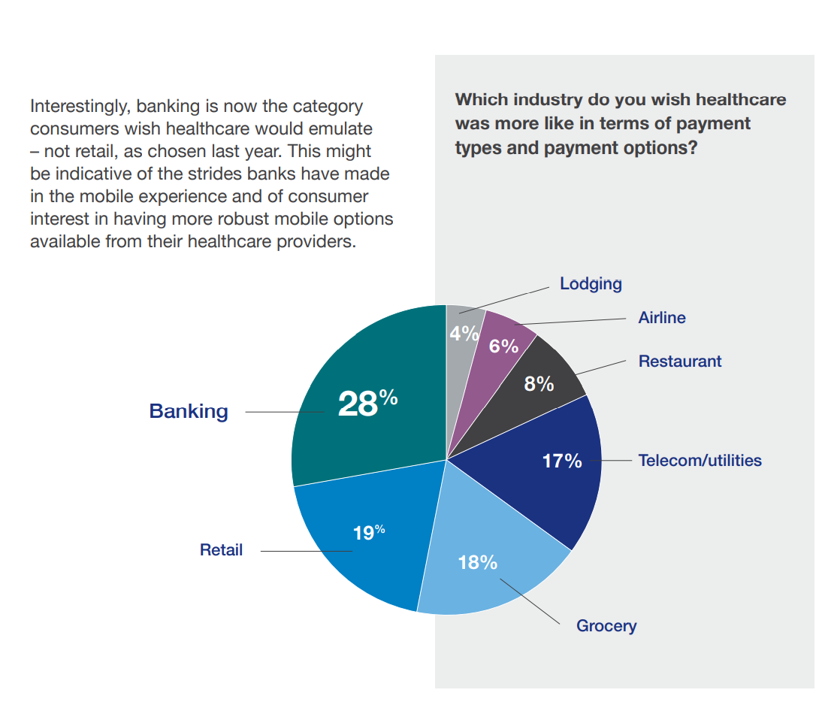
Financial Experience (let’s call it FX) is the next big thing in the world of patient experience and health care. Patients, as health consumers, have taken on more of the financial risk for health care payments. The growth of high-deductible health plans as well as people paying more out-of-pocket exposes patients’ wallets in ways that implore the health care industry to serve up a better retail experience for patients. But that just isn’t happening. One of the challenges has been price transparency, which is the central premise of this weekend’s New York Times research-rich article by reporters Sarah Kliff and
Nurses and Aides Are Beloved and Deserve Higher Pay; and a Spotlight on the Filipinx Frontline

A majority of Democrats, Independents, and Republicans agree that nurses are underpaid. Most Americans across political parties also believe that hospital executives are overpaid, according to a poll from The Associated Press-NORC Center for Public Affairs Research. The survey analysis is aptly titled, Most Americans Agree That Nurses and Aides Are Underpaid, While Few Support Using Federal Dollars to Increase Pay for Doctors, . Insurance executives are also overpaid, according to 73% of Americans — an even higher percent of people than the 68% saying hospital execs make too much money. In addition to nurses being underpaid, 6 in 10
Our Pandemic Lessons: Listening to Michael Dowling – a #HIMSS21 Wrap-Up

“We don’t un-learn,” Dr. Amy Abernethy asserted as she shared her pandemic perspectives on a panel with 2 other former U.S. health policy and regulatory leaders. The three spoke about navigating compliance (think: regulations and reimbursement) in an uncertain world. An uncertain world is our workplace in the health/care ecosystem, globally, in this moment. So to give us some comfort in our collective foxhole, my last post for this week of immersion in #HIMSS21 is based on the keynote speech of Michael Dowling, CEO of Northwell Health. Dowling keynoted on the theme of “Leading for the Future,” sharing his lessons
Reimagining Life After the Pandemic – Seeking Health, Safety, Sustainability, and Trust

COVID-19 reshaped people around the world, one-half of whom are re-defining their personal purpose and life-goals. This sense of purpose extends to peoples’ willingness to buy or patronize companies who do not meet their needs for health, safety, sustainability and trust. For example, two in three of these people would switch travel brands if they felt health and safety weren’t up to par, discovered in Life Reimagined – Mapping the motivations that matter for today’s consumers, from Accenture’s Voices of Change series. In May 2021, Accenture polled over 25,000 consumers globally, in 22 countries, and found that one-half of people
One in Two Americans with Work-Based Insurance Worries That Healthcare Costs Could Lead to Bankruptcy
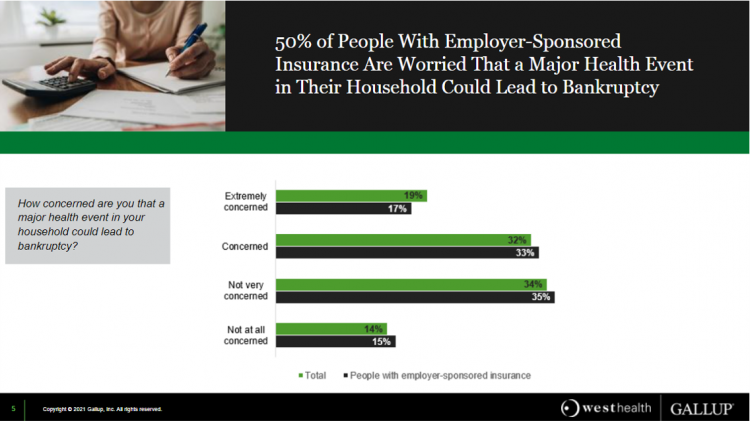
One in two people in the U.S. with employer-sponsored health insurance worry that a major health event in their household could lead to bankruptcy, according to research gathered by West Health and Gallup in Business Speaks: The Future of Employer-Sponsored Insurance. Gallup and West Health presented their study in a webinar earlier this week; in today’s post, I feature a few key data points that particularly resonate as I celebrate/appreciate yesterday’s U.S. Supreme Court’s ruling on the Affordable Care Act (i.e., California v. Texas) combined with a new study published in JAMA Network Open, discussed below the digital fold in
Post-Pandemic, U.S. Healthcare is Entering a “Provide More Care For Less” Era – Pondering PwC’s 2022 Forecast

In the COVID-19 pandemic, health care spending in the U.S. increased by a relatively low 6.0% in 2020. This year, medical cost trend will rise by 7.0%, expected to decline a bit in 2022 according to the annual study from PwC Health Research Institute, Medical Cost Trend: Behind the Numbers 2022. What’s “behind these numbers” are factors that will increase medical spending (the “inflators” in PwC speak) and the “deflators” that lower costs. Looking around the future corner, the inflators are expected to be: A COVID-19 “hangover,” leading to increased health care services utilization Preparations for the next pandemic, and
The Cost of Health Care for a Family of 4 in America Will Reach $28,256 in 2021
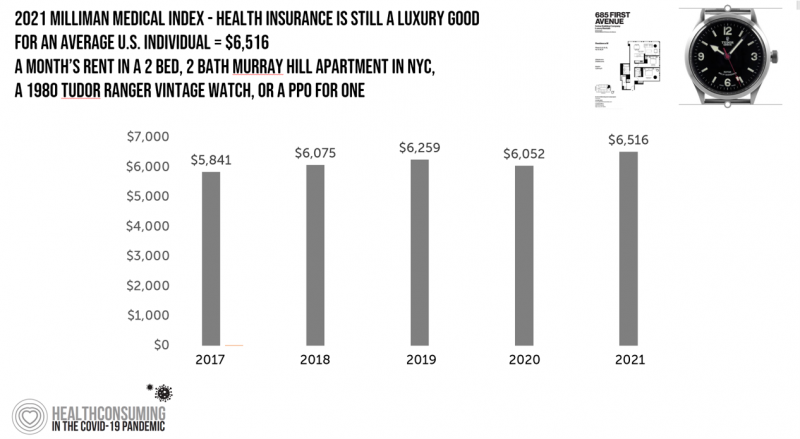
The good news for health care costs for a family of four in America is that they fell, for the first time in like, ever, in 2020. But like a déjà vu all over again, annual health care costs for a family of four enrolled in a PPO will climb to over $28,000 in 2021, based on the latest 2021 Milliman Medical Index (MMI). The first chart shows how health care costs declined in our Year of COVID, 2020, by over $1,000 for that hypothetical U.S. family. But costs rise with a statistical vengeance this year, by nearly $2,200 per family–about
Virtual Health Tech Enables the Continuum of Health from Hospital to Home
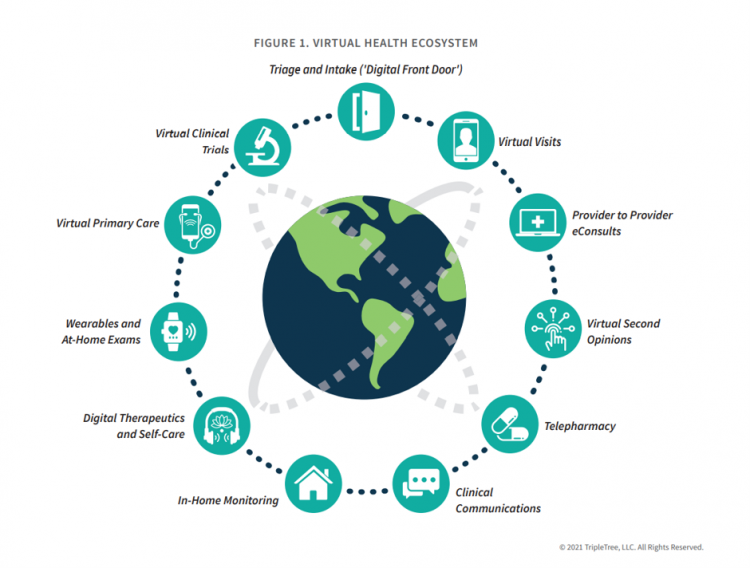
In the COVID-19 pandemic, as peoples’ daily lives shifted closer and closer to home, and for some weeks and months home-all-the-time, health care, too, moved beyond brick-and-mortar hospitals and doctors’ offices. The public health crisis accelerated “what’s next” for health care delivery, detailed in A New Era of Virtual Health, a report published by TripleTree. TripleTree is an investment bank that has advised health care transactions since 1997. As such, the team has been involved in digital health financing and innovation for 24 years, well before the kind of platforms, APIs, and cloud computing now enabling telehealth and care, everywhere. The
The Pandemic’s Death Rate in the U.S.: High Per Capita Income, High Mortality
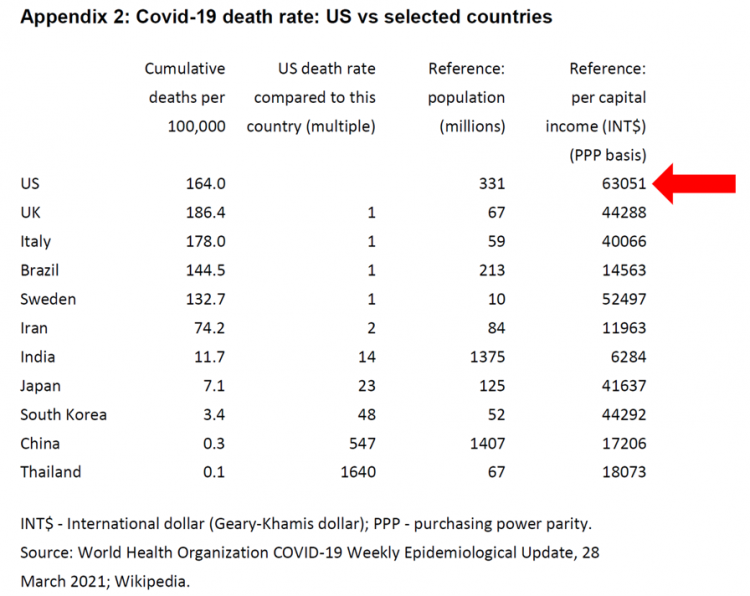
The United States has among the highest per capita incomes in the world. The U.S. also has sustained among the highest death rates per 100,000 people due to COVID-19, based on epidemiological data from the World Health Organization’s March 28, 2021, update. Higher incomes won’t prevent a person from death-by-coronavirus, but risks for the social determinants of health — exacerbated by income inequality — will and do. I have the good fortune of access to a study group paper shared by Paul Sheard, Research Fellow at the Mossaver-Rahmani Center for Business and Government at the Harvard Kennedy School. In reviewing
The Continued Erosion of Trust in the Age of COVID
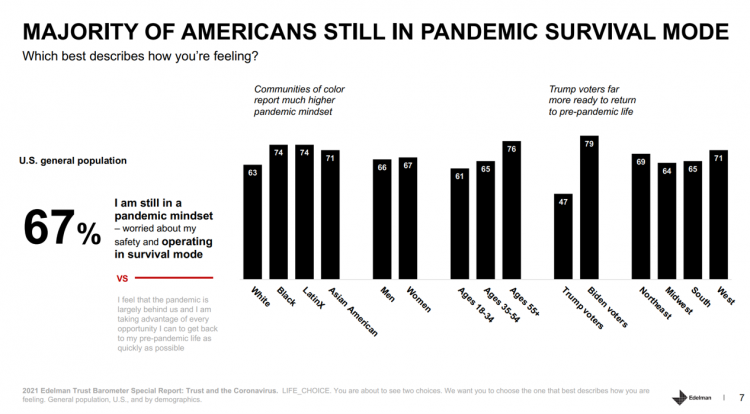
A year into the COVID-19 pandemic, most Americans are still in “survival mode,” according to an update of the 2021 Edelman Trust Barometer, Trust and the Coronavirus in the U.S. Updating the company’s annual Trust Barometer, Edelman conducted a new round of interviews in the U.S. among 2,500 people in early March. [For context, you can read my take on the 2021 Edelman Trust Barometer published during the World Economic Forum in January 2021 here in Health Populi]. The first chart shows that two in three people in the U.S. are still in a pandemic mindset, worried about safety and
Primary Care 2.0 – How Crossover Health is “Re-Bundling” Health Care
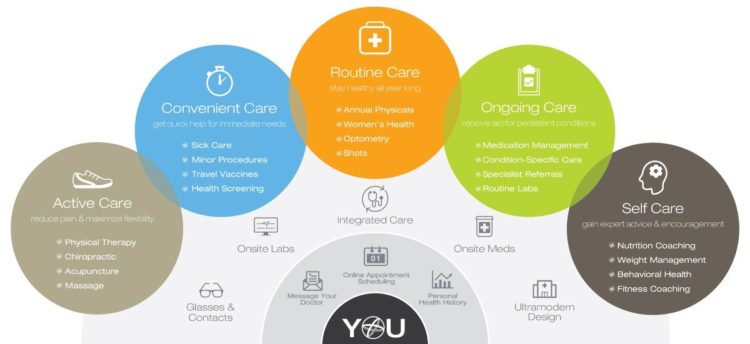
In 2020, investments in digital health reached $14.1 bn, much of which went into niche applications like lab testing, medication adherence, and on-demand triage for urgent care. These companies targeting primary care components represent the “unbundling of the family doctor,” as CB Insights recently coined the market trend. Fragmentation is a hallmark of the U.S. health care system, or more aptly “non-system” as my old friend J.D. Kleinke noted in his book titled Oxymorons….published in 2001. Twenty years later, we confront primary care as a dichotomy: as unbundled pieces of (we hope) innovation, and in organizations re-imagining a new continuity
Nurses, doctors, pharmacists join with teachers in Gallup’s 2021 honest and ethics poll
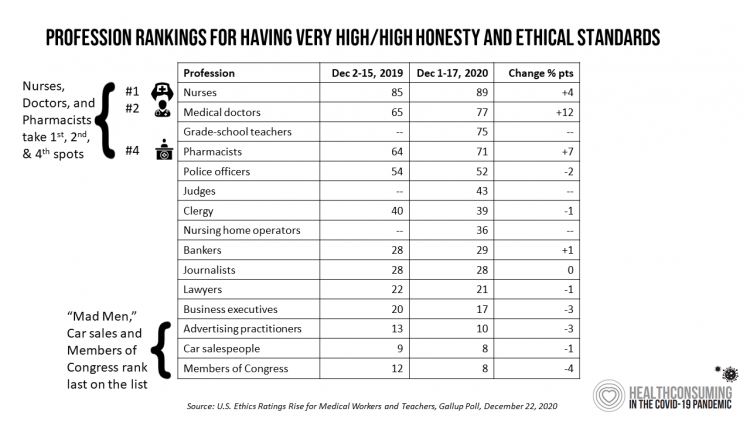
Each year, Americans rank nurses as the most honest and ethical professionals along, generally followed by doctors and pharmacists. In the middle of the coronavirus pandemic in the U.S., grade school teachers join the three medical professions in the annual Gallup Poll on the top-ranked professions for honest and ethical behavior in America as we enter 2021 with many U.S. hospitals’ intensive care units at full capacity….and schools largely emptied of students. The three health care professions scored their highest marks ever achieved in this Gallup Poll, which has been assessing honesty and ethics in America since 1999. Nurses are





 Thank you
Thank you  I'm grateful to be part of the Duke Corporate Education faculty, sharing perspectives on the future of health care with health and life science companies. Once again, I'll be brainstorming the future of health care with a cohort of executives working in a global pharmaceutical company.
I'm grateful to be part of the Duke Corporate Education faculty, sharing perspectives on the future of health care with health and life science companies. Once again, I'll be brainstorming the future of health care with a cohort of executives working in a global pharmaceutical company. Jane joined host Dr. Geeta "Dr. G" Nayyar and colleagues to brainstorm the value of vaccines for public and individual health in this challenging environment for health literacy, health politics, and health citizen grievance.
Jane joined host Dr. Geeta "Dr. G" Nayyar and colleagues to brainstorm the value of vaccines for public and individual health in this challenging environment for health literacy, health politics, and health citizen grievance.