Declines in preventive care services like cancer screenings and blood glucose testing concern employers, whose continued to cover health insurance for employees during the pandemic.
“As we enter the third year of the COVID-19 pandemic, employers continue to battle escalating clinical issues, including delayed care for chronic conditions, postponed preventive screenings, and the exponential increase in demand for behavioral health services,” the Chief Medical Officer for Castlight Health notes in an analysis of medical claims titled Millions of People Deferred Crucial Care During the Pandemic, published in June.
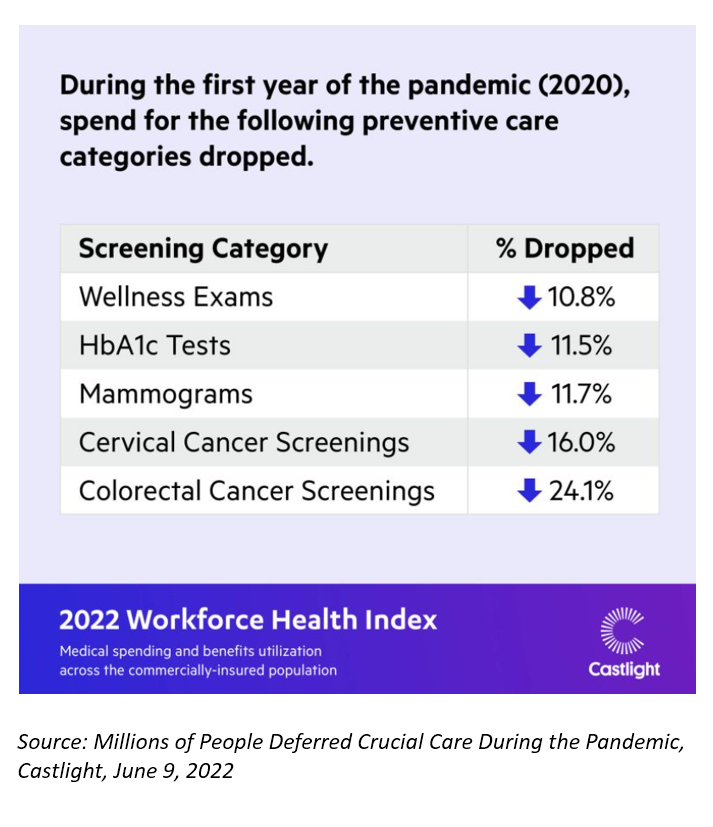
The first chart illustrates the deferred care identified in Castlight’s assessment of 160 million medical claims in its commercially-insured population data. Castlight published the full research findings in April in the company’s 2022 Workforce Health Index.
The full report speaks to medical spending and utilization trends for preventive care, telehealth, and behavioral health. [You can access state-by-state specifics on the Castlight Health supplemental dataset portal].
Take preventive services across the entire national commercial population in the study. Spending for cancer screenings dropped as much as over 24% for colorectal cancer (think: colonoscopy), 16% for cervical cancer (think: pap smear), and nearly 12% fall in the volume of mammograms.
11.5% fewer commercially insured employees were tested for HbA1C (hemoglobin blood glucose test), and wellness exams dropped by nearly 11%.
The impacts of people delaying preventive screenings can expect to lead to additional excess deaths that were directly attributable to the pandemic, this JAMA Oncology study noted.
As a result, commercial healthcare spending fell in 2020, rebounding in 2021. But flat growth is expected for 2022, Castlight forecasts.
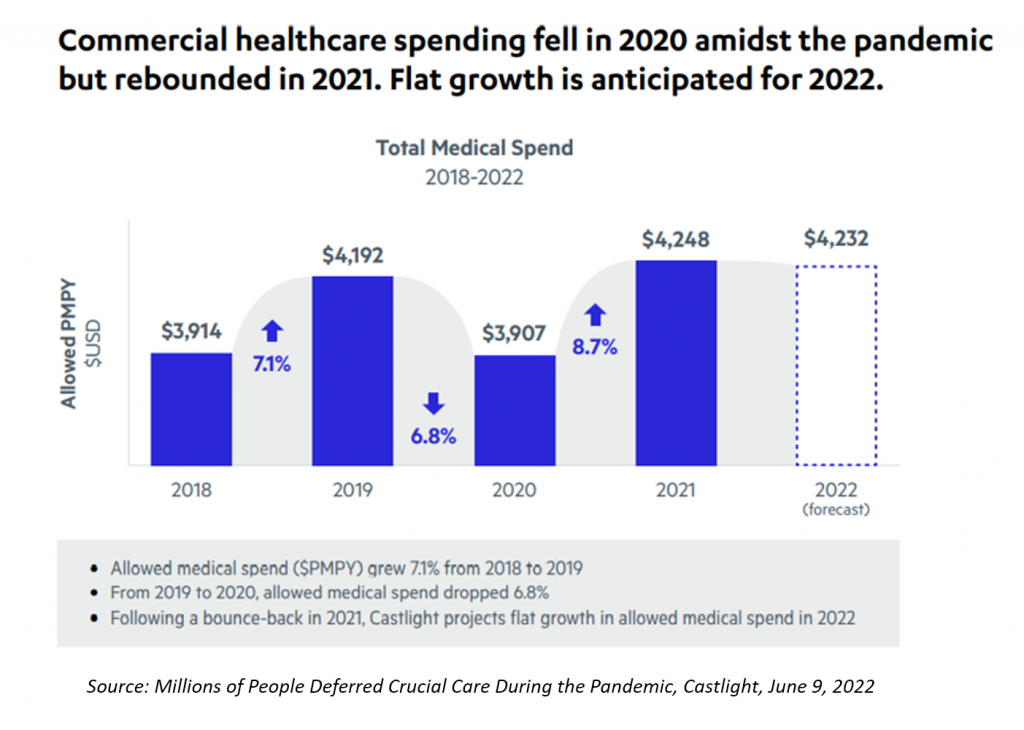
The second bar chart illustrates the per member/per month (PMPM) spend for commercially insured workers, showing growth of over 7% from 2018 to 2019, and nearly 7% drop from 2019 to 2020 in the first year of the pandemic.
2020-2021 was a sort of “catching-up-with-healthcare” year, seeing the PMPM spend grow by 8.7%.
But Castlight expects a flat-line in PMPM spending for 2022, leveling out at $4,232 per member/per month for commercially-insured employees.
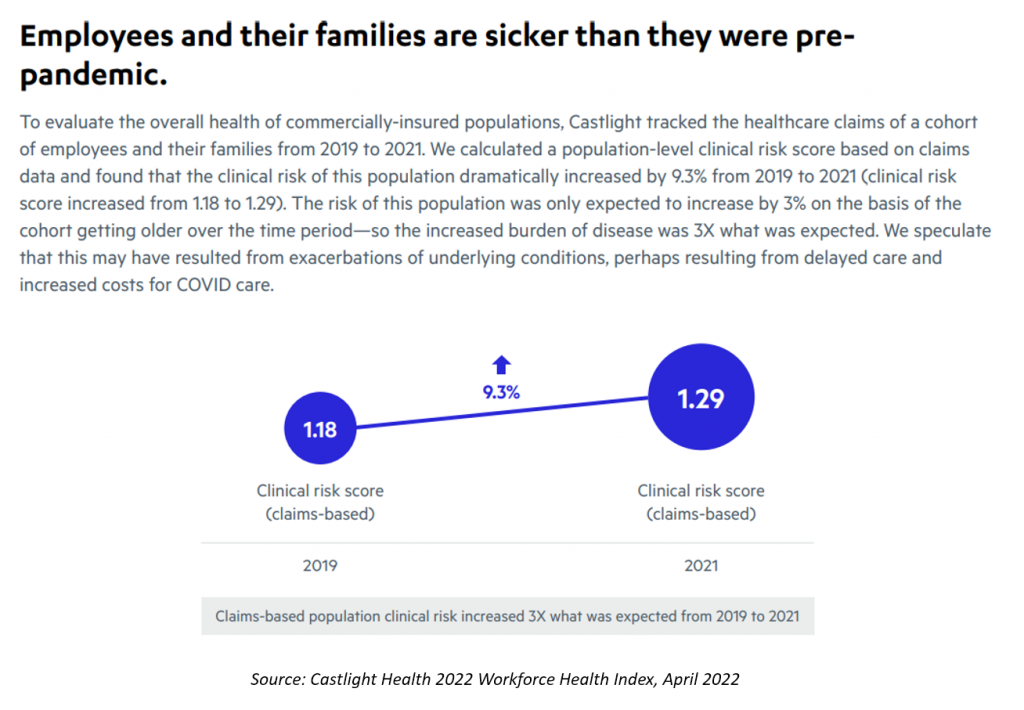
Employers covering workers with health insurance are now dealing with employees and families who are “sicker than they were pre-pandemic,” Castlight asserts in its report.
Based on their analysis of medical claims, insured workers’ clinical risk scores increased by 9.3%, from 1.18 from the start of the COVID-19 pandemic in 2019 to 1.29 in 2021.
The 9.3% is 3 times the expected increase in clinical risk scores based on what was anticipated due to the aging of the insured population in the time horizon. “We speculate that this may have resulted from exacerbations of underlying conditions, perhaps resulting from delayed care and increased costs for COVID care,” Castlight reasons.
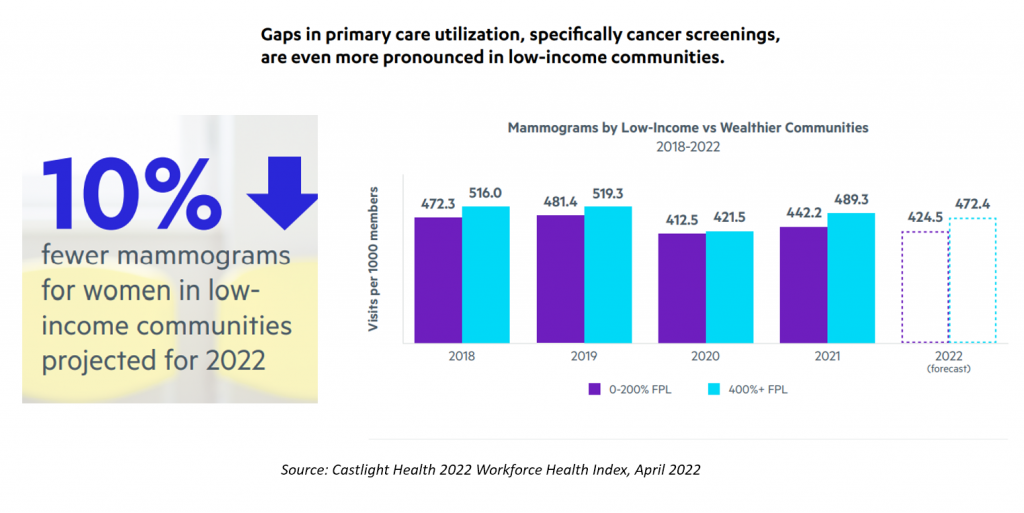
Health Populi’s Hot Points: Castlight examined the commercial medical claims even more granularly, looking into differences between higher-income workers compared with lower-income communities.
For example, women in low-income areas are projected to undergo 10% fewer mammograms in 2022, based on trend rates found in mammography since 2018.
The chart on gaps in primary care utilization, specifically cancer screenings, illustrate the general trend that women in households earning up to 200% of the Federal Poverty Level (FPL) have a lower visit rate for mammograms per 1000 health plan members (represented by the purple vertical bars) than women at the 400%+ FPL (the blue bars).
Commercially insured workers in low-income communities also had fewer visits per 1000 members for telehealth in 2020 and 2021. In 2020, the difference between those at the lower income level was 490.4 compared with 916,7 visits per 1000 members in 2020.
That delta/difference was over 100% in 2021, with lower income insured employees having a visit rate for telehealth at 452.8 compared with 941.9 for higher-income insured workers — more than double the rate of lower-income peers.
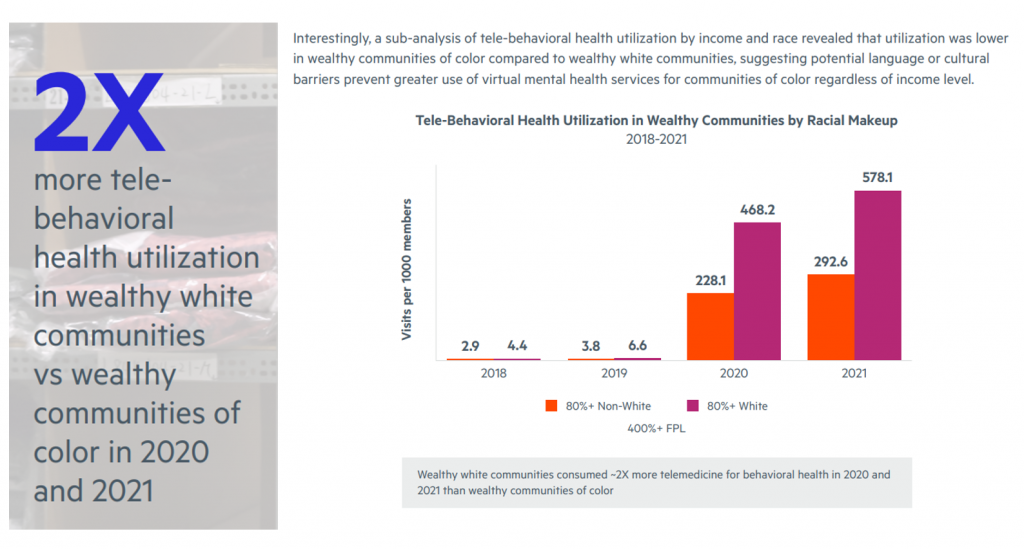
Finally, note a gap found in tele-behavioral visit utilization between wealthy white communities vs wealthy communities of color in 2020 and 2021.
This rate differential was also nearly two-times different, prompting Castlight to write that the lower use of tele-behavioral health in wealthy communities of color may be, “suggesting potential language or cultural barriers [that] prevent greater use of virtual mental health services for communities of color regardless of income level.”
Let’s restate this last finding: that, “language or cultural barriers [can] prevent greater use of virtual mental health services for communities of color regardless of income level,” even for higher-income commercially-insured employees.
And let’s reiterate that this population Castlight studied were all covered by commercial insurance: these were not people lacking health insurance or those enrolled in public programs like Medicaid or Medicare.

The National Institutes of Health convened a panel to study preventive medical services and health disparities, resulting in a workshop report from AHRQ, Achieving Health Equity in Preventive Services.
“Ongoing disparities in the use of evidence-based preventive services, despite the wide availability of guidelines and improvements in insurance coverage, are a call to action for researchers and health care providers,” the report concluded. The report offered 26 recommendations to address health equity and prevention, one of which integrated new models and systems of care delivery.
Enter the American College of Physicians, who published an approach to reforming physician payments to achieve value in health care — with a focus on patients’ socioeconomic factors — last week.
“We must continue to find ways to broaden access to care in order to achieve more equitable health benefits use,” according to Dr. Bruce Sherman, advisor to the National Alliance of Healthcare Purchaser Coalitions, a co-author of the Castlight report.
“Employers are in a unique position to address socioeconomic and workplace barriers to care among their employees and family members…Identifying and addressing inequities in workforce health benefits is not only the right thing to do, it’s a compelling business opportunity.”




 Thank you
Thank you  I'm grateful to be part of the Duke Corporate Education faculty, sharing perspectives on the future of health care with health and life science companies. Once again, I'll be brainstorming the future of health care with a cohort of executives working in a global pharmaceutical company.
I'm grateful to be part of the Duke Corporate Education faculty, sharing perspectives on the future of health care with health and life science companies. Once again, I'll be brainstorming the future of health care with a cohort of executives working in a global pharmaceutical company. Jane joined host Dr. Geeta "Dr. G" Nayyar and colleagues to brainstorm the value of vaccines for public and individual health in this challenging environment for health literacy, health politics, and health citizen grievance.
Jane joined host Dr. Geeta "Dr. G" Nayyar and colleagues to brainstorm the value of vaccines for public and individual health in this challenging environment for health literacy, health politics, and health citizen grievance.