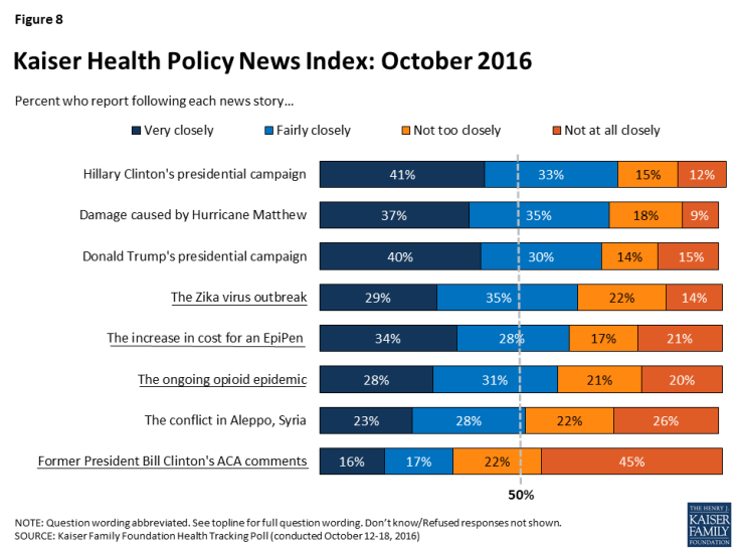
“When thinking about health care priorities for the next president and Congress to address, dealing with the high price of prescription drugs tops the public’s list while issues specific to the Affordable Care Act (ACA), such as repealing provisions of the law or repealing the law entirely, are viewed as top priorities by fewer Americans,” according to the Kaiser Health Tracking Poll for October 2016 – the last such survey to be taken before the 2016 Presidential election.
The poster child snapshot image representing the high cost of prescription drugs is the increase in cost for an EpiPen, which among current health news stories, is placed by more consumers as a closely-followed item than the ongoing opioid epidemic.
74% of American voters say that making sure high-cost drugs for chronic conditions are affordable to those who need them should be the top health care priority for the next President and Congress, shown in the table. Note that 84% of Democrats, 73% of Independents, and 68% of Republicans believe this, making Rx prices the top issue for health consumers on both sides of the political aisle. The second most important issue would be “government action to lower prescription drug prices,” an opinion also shared by a majority of consumers in all three parties.
Repealing the ACA garners 60% of Republican voters — still fewer than Republicans who want to ensure that high-cost drugs for chronic conditions are affordable to people who need them.
![]() Health Populi’s Hot Points: Note the importance of price transparency and costs ranking higher on the priorities for legislators versus more finite points about the ACA. Relatively high on the list are protecting people from being charged high prices that are received by out-of-network providers; making information about quality of health care available to patients; and, making price information for doctors’ visits, tests and procedures more available.
Health Populi’s Hot Points: Note the importance of price transparency and costs ranking higher on the priorities for legislators versus more finite points about the ACA. Relatively high on the list are protecting people from being charged high prices that are received by out-of-network providers; making information about quality of health care available to patients; and, making price information for doctors’ visits, tests and procedures more available.
These responses demonstrate that patients are stretching their health consumer muscles in response to understanding and managing high-deductibles and growing first-dollar payments to health care providers.




 Interviewed live on BNN Bloomberg (Canada) on the market for GLP-1 drugs for weight loss and their impact on both the health care system and consumer goods and services -- notably, food, nutrition, retail health, gyms, and other sectors.
Interviewed live on BNN Bloomberg (Canada) on the market for GLP-1 drugs for weight loss and their impact on both the health care system and consumer goods and services -- notably, food, nutrition, retail health, gyms, and other sectors. Thank you, Feedspot, for
Thank you, Feedspot, for  As you may know, I have been splitting work- and living-time between the U.S. and the E.U., most recently living in and working from Brussels. In the month of September 2024, I'll be splitting time between London and other parts of the U.K., and Italy where I'll be working with clients on consumer health, self-care and home care focused on food-as-medicine, digital health, business and scenario planning for the future...
As you may know, I have been splitting work- and living-time between the U.S. and the E.U., most recently living in and working from Brussels. In the month of September 2024, I'll be splitting time between London and other parts of the U.K., and Italy where I'll be working with clients on consumer health, self-care and home care focused on food-as-medicine, digital health, business and scenario planning for the future...