Access to the Internet has been a key determinant of health — or more aptly, death — during the COVID-19 pandemic.
Americans lacked Internet access were more likely to die due to complications from the coronavirus, according to a study published in JAMA Network Open this month.
 The study’s key finding was that for every additional 1% of people living in a county who have access to the Internet, between 2.4 and 6.0 COVID-19 deaths per 100,000 were preventable.
The study’s key finding was that for every additional 1% of people living in a county who have access to the Internet, between 2.4 and 6.0 COVID-19 deaths per 100,000 were preventable.
The paper asserts that,
“More awareness is needed about the essential asset of technological access to reliable information, remote work, schooling opportunities, resource purchasing and/or social community.”
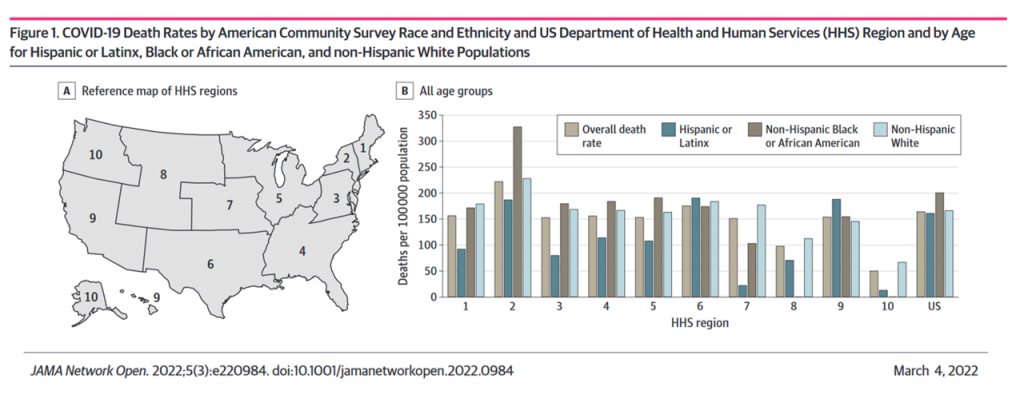
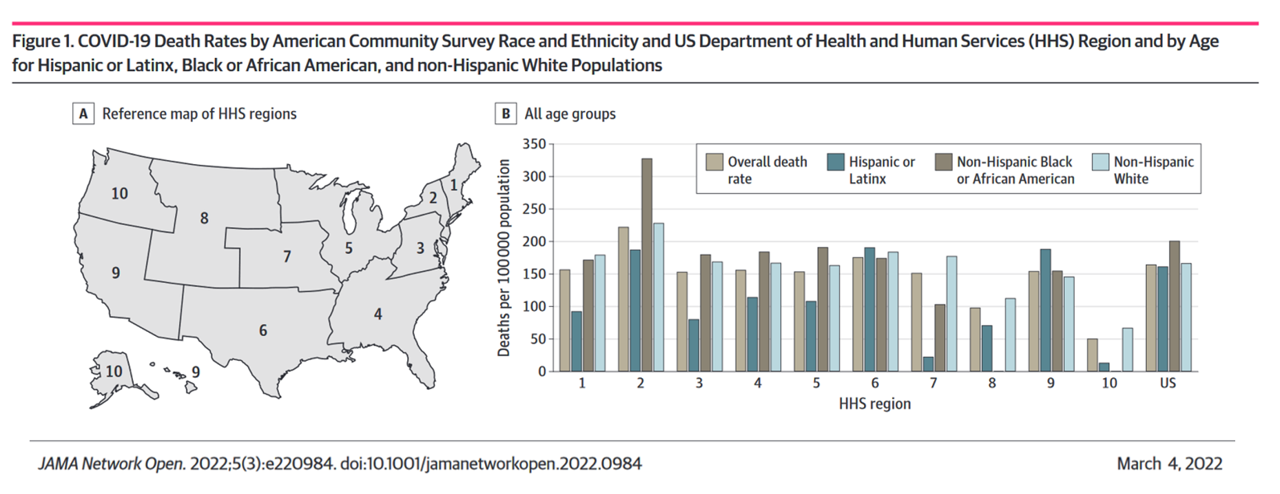
The researchers used spatial analysis to explore disproportionate mortality outcomes for COVID-19 experienced by different racial and ethnic groups: comparing overall death rates with those of Hispanic or Latinx, Non-Hispanic Black or African-American, and Non-Hispanic White populations.
Underneath the overall statistic of 2.4 to 6.0 preventable deaths, there were nuances for different social determinants of health and racial and spatial disparities found in the study especially pointing to living in rural versus urban or suburban communities.
In urban areas: Internet access and the so-called “mixed immigrant cohesion and accessibility index” contributed to mortality differences. Housing problems were associated with greater COVID-19 incidence and mortality. This more directly impacted counties with a higher proportion of Hispanic and Latinx people compared with other urban geographies. In addition, these counties also had a higher percentage of working-age people lacking health insurance.
In suburban areas: Higher COVID-19 death rates were associated with higher poverty rates and older adults and people with disabilities who had lower rates of mobility.
In rural areas: Greater COVID-19 mortality was associated with lower access to quality health care services (think: long distances and lack of transportation options to travel to health care providers).
Internet access was a significant factor in COVID-19 mortality across all three community types, which the researchers note should prompt us to consider the “essential asset of technological access to reliable information, remote work, schooling opportunities, resource purchasing, and/or social community.”
 Health Populi’s Hot Points: The American Medical Association polled physicians in late 2021 to gauge doctors’ perspectives on telehealth. The report lays out physicians’ majority support for telehealth and key issues preventing further adoption and proliferation of use across the U.S.
Health Populi’s Hot Points: The American Medical Association polled physicians in late 2021 to gauge doctors’ perspectives on telehealth. The report lays out physicians’ majority support for telehealth and key issues preventing further adoption and proliferation of use across the U.S.
Key to universal adoption of telehealth are reimbursement and regulatory policy (such as waivers and reducing licensure obstacles).
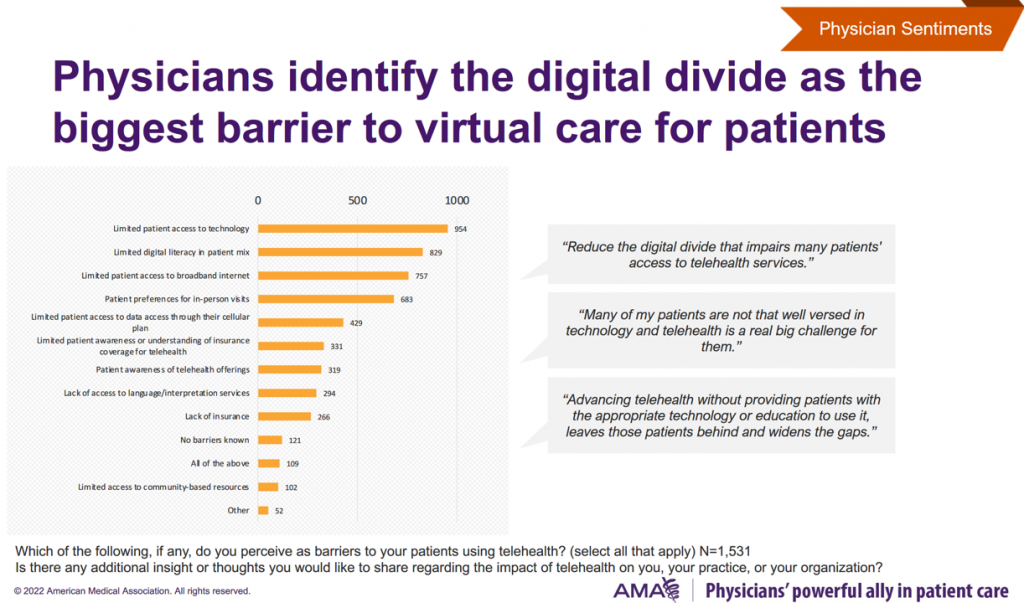
Next in line of barriers are patients’ challenges with technology, noted in the graphic shown here from the report.
The most challenging aspects for patients’ digital divide are their access to technology, limited digital literacy, and limited broadband access.
This speaks to the importance of connecting the dots between broadband availability enabling people and patients to connect to the Internet, coupled with on that demand side, health citizens understand just how to use digital technologies at the platform level of general use to how to access a telehealth “digital front door” for a clinical visit.
As one of the physicians quoted told the AMA, “Advancing telehealth without providing patients with the appropriate technology or education to use it, leave those patients behind and widens the gaps.”
Together, the JAMA Network Open research paper and AMA physician survey inform us with useful insights to close that health care digital divide which could make a major difference between some patients’ lives versus their demise.




 Interviewed live on BNN Bloomberg (Canada) on the market for GLP-1 drugs for weight loss and their impact on both the health care system and consumer goods and services -- notably, food, nutrition, retail health, gyms, and other sectors.
Interviewed live on BNN Bloomberg (Canada) on the market for GLP-1 drugs for weight loss and their impact on both the health care system and consumer goods and services -- notably, food, nutrition, retail health, gyms, and other sectors. Thank you, Feedspot, for
Thank you, Feedspot, for  As you may know, I have been splitting work- and living-time between the U.S. and the E.U., most recently living in and working from Brussels. In the month of September 2024, I'll be splitting time between London and other parts of the U.K., and Italy where I'll be working with clients on consumer health, self-care and home care focused on food-as-medicine, digital health, business and scenario planning for the future...
As you may know, I have been splitting work- and living-time between the U.S. and the E.U., most recently living in and working from Brussels. In the month of September 2024, I'll be splitting time between London and other parts of the U.K., and Italy where I'll be working with clients on consumer health, self-care and home care focused on food-as-medicine, digital health, business and scenario planning for the future...