Most doctors see the advantages of digital health tools like telehealth, consumers’ access to their health information, and point-of-care workflow solutions, the American Medical Association found in a survey of 1300 physicians, published in September 2022.

The AMA first conducted research with physicians and their views on digital health in July 2016. This year’s study was designed to compare current clinicians’ perspectives with those garnered in the 2016 and 2019 studies.
There is a clear and positive shift of doctors’ adoption of and appreciation for digital tools, with “growth in enthusiasm” concentrated in tele-visits, the AMA learned.
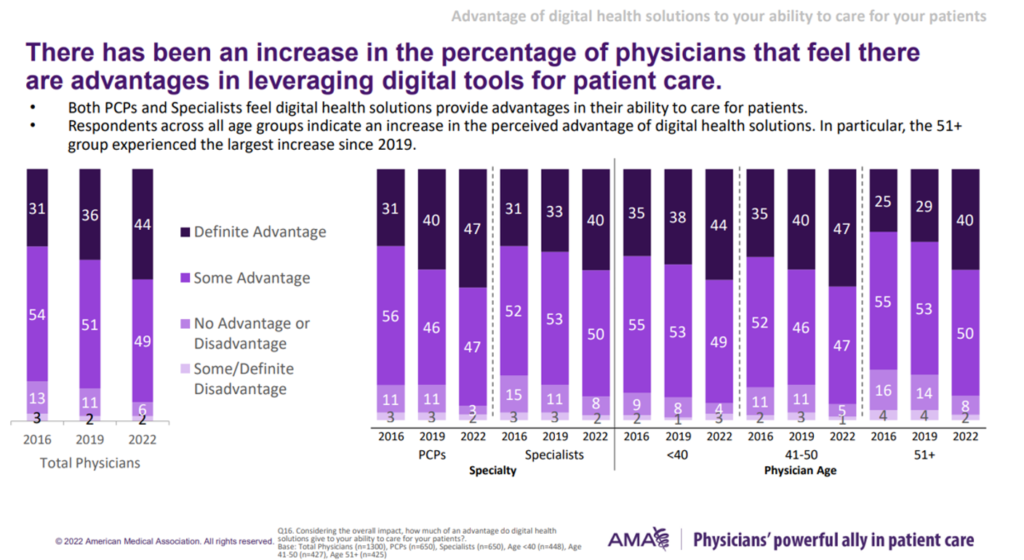
93% of physicians see advantages in digital health tools for patient care, split by 44% seeing “definite advantages” and 49% seeing “some advantage.” There was an 8-point growth in those seeing “definite advantages” since 2019.
The second bar chart illustrates that both PCPs’ and specialists’ appreciation for digital tools for patient care has grown, especially among physicians over 51 years of age.
While the adoption of digital tools has grown since 2019, tele-visits increased the most in adoption compared with other technologies in the study such as remote monitoring, patient engagement, and clinician decision support.
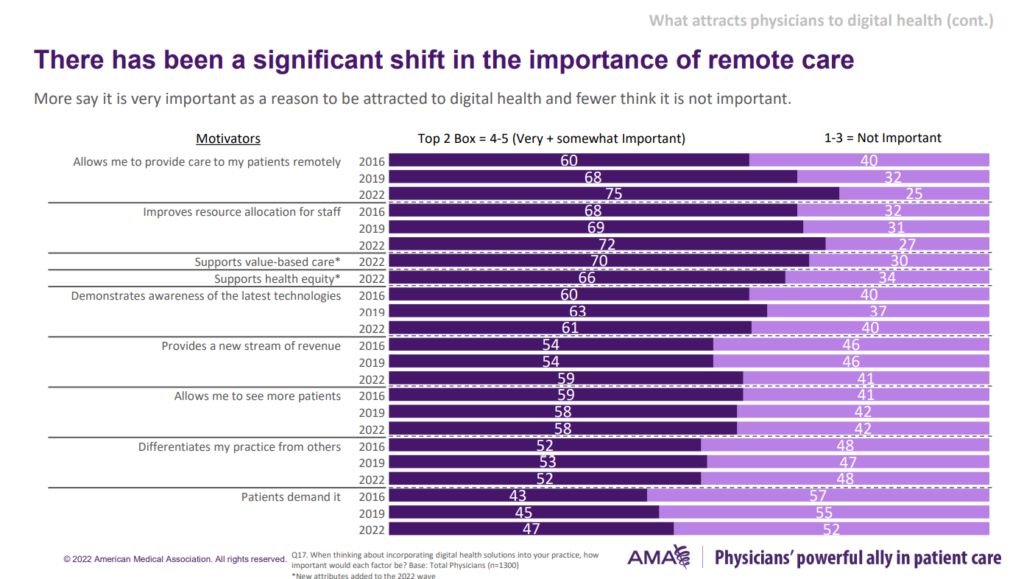
Thus, there has been a significant shift in the importance of remote care. Aside from the COVID-19’s exogenous shock on physicians’ face-to-face encounters with patients, there are other motivators inspiring doctors to use digital health tools, and especially remote care platforms.
Three key motivators stand out here:
- Improves resource allocation for staff
- Supports value-based care
- Supports heath equity.
[Note that #2 and #3 were new questions added to the 2022 study wave].
“Improves resource allocation for staff” speaks to the crisis issue of clinician burnout. Burnout (translated through anxiety, stress, depression, and suicidality) was already a challenge for U.S. physicians and nurses as the pandemic emerged in early 2020.
The poorly-conceived rollout of EHRs following the HITECH Act legislation and incentives, from design to implementation, led to a lot more insights about how technology can be well-intended and an epic fail for those who were meant to benefit from a shiny new thing.

In this year’s AMA look at digital health, we see that more physicians benefited from the use of some specific digital tools over the past several years: notably, telehealth and remote monitoring.
And most physicians better understand what technologies can help address the key needs of patients with chronic conditions — regular monitoring, supporting prevention, and augmenting physician capacity to free up time for the most acute patients.
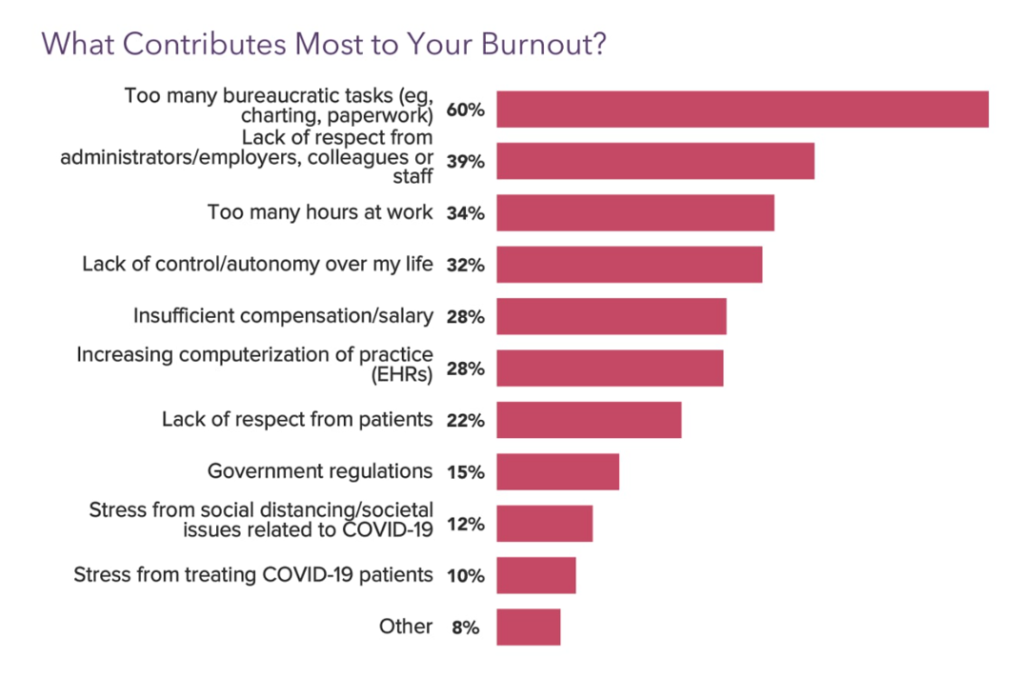
Health Populi’s Hot Points: This year’s annual Medscape look into burnout and depression found across-the-profession, from the ER to the surgical suite and therapy chaise, that most doctors (and nurses) were facing burnout for several reasons; key contributors to burnout are shown in this last bar chart from the Medscape study report.
At the top stressors are bureaucratic tasks like paperwork and charting, too many hours at work, and increasing computerization of the practice (via EHRs).
We are learning that digital health tools and IT can play a role in helping to reduce burnout, enhance clinician and patient experience alike, and support both health outcomes and health equity — when imagined, designed, and implemented with the passionate, authentic focus on user-centered design. That requires our empathy, deep study, patience, and investment of time and resources in the ready, aim, then fire mode. “Getting ready and aiming” here is the measure twice (or three times) mode. And don’t overlook the importance of sufficient investment in the implementation mode, where peers of users can be very helpful evangelists and teachers for effective, engaging on-ramping.
The 2022 AMA research gives us an especially useful roadmap for understanding where physicians are in their digital health journeys and how to better design, build, and roll out helpful tools that address the Quintuple Aim – to bolster health outcomes for patients and publics, to improve the experience of both patient and clinician, to lower per patient cost, to support health equity and reduce disparities, and to bolster our clinicians’ wellness.

Keep in mind that next week is Telehealth Awareness Week, the ATA’s (American Telemedicine Association) reminder that Telehealth Is Health. Stay tuned for more here on Health Populi to support the effort and bolster care across the continuum, from our homes and own hands to the hospital and post-acute sites….





 Thank you
Thank you  I'm grateful to be part of the Duke Corporate Education faculty, sharing perspectives on the future of health care with health and life science companies. Once again, I'll be brainstorming the future of health care with a cohort of executives working in a global pharmaceutical company.
I'm grateful to be part of the Duke Corporate Education faculty, sharing perspectives on the future of health care with health and life science companies. Once again, I'll be brainstorming the future of health care with a cohort of executives working in a global pharmaceutical company. Jane joined host Dr. Geeta "Dr. G" Nayyar and colleagues to brainstorm the value of vaccines for public and individual health in this challenging environment for health literacy, health politics, and health citizen grievance.
Jane joined host Dr. Geeta "Dr. G" Nayyar and colleagues to brainstorm the value of vaccines for public and individual health in this challenging environment for health literacy, health politics, and health citizen grievance.