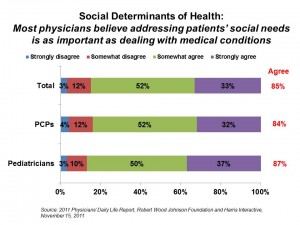
 Most U.S. primary care physicians realize the health of their patients is largely out of their hands — with their social needs ranking as important as addressing their medical conditions, according to the 2011 Physicians’ Daily Life Report, conducted on behalf of the Robert Wood Johnson Foundation by Harris Interactive in September-October 2011, results published in November 2011. In fact, unmet social needs are directly leading to worse health for Americans, say 9 in 10 doctors.
Most U.S. primary care physicians realize the health of their patients is largely out of their hands — with their social needs ranking as important as addressing their medical conditions, according to the 2011 Physicians’ Daily Life Report, conducted on behalf of the Robert Wood Johnson Foundation by Harris Interactive in September-October 2011, results published in November 2011. In fact, unmet social needs are directly leading to worse health for Americans, say 9 in 10 doctors.
With that recognition, most physicians feel they’re unable to address patients’ health concerns caused by unmet social needs. This has led to most doctors confessing they’re unable to deliver quality care due to patients’ unmet needs which are beyond their control. The result: a confidence-gap among physicians, who believe they can’t close the gap between unmet social needs and the delivery of high quality health care to patients.
The online survey polled 1,000 physicians, including 690 primary care doctors and 310 pediatricians, randomly sampling the American Medical Association Masterfile.
Health Populi’s Hot Points: The discussion of unmet social needs falls under the umbrella known as the “social determinants of health.” You can follow #sdoh on Twitter to get up to speed on this critical issue.
I worked on the Healthcare 2010 forecast for RWJF with Wendy Everett when she led the health group at Institute for the Future in 2000. 12 years ago, the LA Times interviewed Wendy, who quoted a paradigm in the report that 50% of health was determined by lifestyle, 20% by genetics, 20% by environment, and 10% by health care access.
Today, the World Health Organization, RWJF, and many other NGOs devote substantial resources to educate the world, policymakers, and health citizens on the importance of the social determinants of health. WHO lists these as, “the conditions in which people are born, grow, live, work and age.”
This sounds remarkably like the mantra of the U.S. Surgeon General Regina Benjamin who says that health is where people “live, work, play and pray.”
In nations’ search to bend their countries’ health care cost curves, policymakers and citizens alike should be mindful of Wendy’s 50% lifestyle + 20% environment: that 70% of health (at least) is determined by factors beyond the control of (1) genetics and (2) the health system.
The primary care doctors studied by RWJF are justified in feeling the gap between the care they are trying to provide versus the intractable forces of the social determinants of health, like housing, healthy food, safe work environments and schools that are directly shaping the health of the people they treat.
“Physicians wish they could write prescriptions to help patients with social needs,” observes the commentary report that complements the survey data, Health Care’s Blind Side: the overlooked connection between social needs and good health. 1 in 7 prescriptions would be for addressing social needs, such as fitness, nutritious food, transport assistance, employment assistance, adult education, and housing assistance.
The payors of health care need to embrace the concept of social needs’ impact on health. If payment reforms to address outcomes, and not transactions/encounters, providers in communities will be better aligned to prescribe remedies beyond the back of the pharmacy.




 Interviewed live on BNN Bloomberg (Canada) on the market for GLP-1 drugs for weight loss and their impact on both the health care system and consumer goods and services -- notably, food, nutrition, retail health, gyms, and other sectors.
Interviewed live on BNN Bloomberg (Canada) on the market for GLP-1 drugs for weight loss and their impact on both the health care system and consumer goods and services -- notably, food, nutrition, retail health, gyms, and other sectors. Thank you, Feedspot, for
Thank you, Feedspot, for  As you may know, I have been splitting work- and living-time between the U.S. and the E.U., most recently living in and working from Brussels. In the month of September 2024, I'll be splitting time between London and other parts of the U.K., and Italy where I'll be working with clients on consumer health, self-care and home care focused on food-as-medicine, digital health, business and scenario planning for the future...
As you may know, I have been splitting work- and living-time between the U.S. and the E.U., most recently living in and working from Brussels. In the month of September 2024, I'll be splitting time between London and other parts of the U.K., and Italy where I'll be working with clients on consumer health, self-care and home care focused on food-as-medicine, digital health, business and scenario planning for the future...