 People are spending more out of their own pockets on health care, and particularly for medications. There are two sides to the medicine-spending coin: there’s the low-end which are generic drugs, most of which carry a co-pay of $10 or less. Then there’s the high end of specialty pharmaceuticals, a fast-growing category of very expensive products for which many consumers dearly pay — if and when they choose to take their doctors’ recommendations.
People are spending more out of their own pockets on health care, and particularly for medications. There are two sides to the medicine-spending coin: there’s the low-end which are generic drugs, most of which carry a co-pay of $10 or less. Then there’s the high end of specialty pharmaceuticals, a fast-growing category of very expensive products for which many consumers dearly pay — if and when they choose to take their doctors’ recommendations.
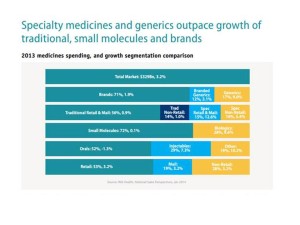
In Medicine use and shifting costs of healthcare, IMS Institute for Healthcare Informatics reports that while (inexpensive) generic drugs comprise 86% of prescriptions in the U.S., it’s high cost drugs falling into the specialty category that are driving Rx spending up — despite the fact that nearly 9 in 10 prescribed medications is a generic.
On the cost-lowering side of this equation, individual drug costs for most patients are declining, with most prescriptions costing well under $10 due to the rise of generics in the market.
On the cost-increasing side, 30% of patient prescription out-of-pocket costs came from 2.3% of prescriptions – especially high-cost specialty medications.
The first chart illustrates the high growth of specialty/generic medicines vs. brands and small molecule drugs. Generics are growing at 9% a year, specialty drugs via retail channels at 12.6%, and biologics at 9.6%. On the other hand, Rx brands are growing at a paltry 1.9%, and small molecule drugs at 0.1%.
 The slowdown of generic approvals in 2013 also contributed to a rise in medicine spending by 3.2% overall, with the growth of new approvals for oncology, hepatitis C, HIV, and autoimmune diseases which in aggregate grew by 11%.
The slowdown of generic approvals in 2013 also contributed to a rise in medicine spending by 3.2% overall, with the growth of new approvals for oncology, hepatitis C, HIV, and autoimmune diseases which in aggregate grew by 11%.
The report was published in April 2014.
Health Populi’s Hot Points: The growth of high-deductible health plans in employer groups and health insurance exchange plans is making health costs more visible to consumers who, under these plans, must reach into household budget-pockets to pay for health care until the deductible is reached. A survey on employee financial wellness from PwC published earlier this month found that one-third of U.S. companies have already increased deductibles and cost-sharing, and another 50% are considering doing so in 2015.
The retailization of health costs — where health plan enrollees are morphing into health care consumers — may already be having an impact on retail spending, according to Chris Low of FTN Financial. Low recognizes that the growth in consumer health spending “is already so substantial, we ignore it at our own peril.” For consumers managing household finances, this means that retail spending may be shifting from consumer goods purchased at Target and Walmart to health care.
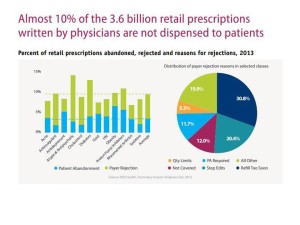
That will be the case for those consumers who heed their clinicians’ prescription recommendations. However, not every patient fills the first prescription, or re-fills the second or subsequent scripts. The second graphic illustrates this phenomenon of prescription abandonment, where about 10% of the 3.6 billion Rx’s written by physicians are not dispensed to patients. IMS Health found that the highest levels of Rx abandonment are among obesity drugs, Rx’s for proton pump inhibitors, and prescriptions for antidepressants and diabetes.
The Kaiser Family Foundation Health Tracking Poll from September 2013 also found that because of cost, 27% of U.S. adults did not fill a prescription that a doctor had written. That’s a direct health “consumer” response to a direct cost of a health care good.
CVS/pharmacy announced a new service today called Bill Pay. This spring, the pharmacy chain, working with InComm (an ecommerce/payments company), will enable consumers to pay their monthly health insurance premium bills at any CVS/pharmacy cash register at the back-of-store pharmacy or at a cash register in the front by the chewing gum.
The role of the pharmacy (and pharma) are expanding their role in the retail health ecosystem. But that retailization is also impacting costs and how consumers perceive and react to them in the context of all household retail spending.




 Interviewed live on BNN Bloomberg (Canada) on the market for GLP-1 drugs for weight loss and their impact on both the health care system and consumer goods and services -- notably, food, nutrition, retail health, gyms, and other sectors.
Interviewed live on BNN Bloomberg (Canada) on the market for GLP-1 drugs for weight loss and their impact on both the health care system and consumer goods and services -- notably, food, nutrition, retail health, gyms, and other sectors. Thank you, Feedspot, for
Thank you, Feedspot, for  As you may know, I have been splitting work- and living-time between the U.S. and the E.U., most recently living in and working from Brussels. In the month of September 2024, I'll be splitting time between London and other parts of the U.K., and Italy where I'll be working with clients on consumer health, self-care and home care focused on food-as-medicine, digital health, business and scenario planning for the future...
As you may know, I have been splitting work- and living-time between the U.S. and the E.U., most recently living in and working from Brussels. In the month of September 2024, I'll be splitting time between London and other parts of the U.K., and Italy where I'll be working with clients on consumer health, self-care and home care focused on food-as-medicine, digital health, business and scenario planning for the future...