The pandemic has put health care top-of-mind for health citizens the world over. As the public health crisis continues its up-and-downticks around the globe, people are connecting health care to their national economies and politics, based on a global survey from the Pew Research Center, Citizens in Advanced Economies Want Significant Changes to Their Political Systems.
 For this analysis, the Pew research team assessed the views of some 2,600 health citizens living in 17 developed countries in February 2021. The study report was published in late October 2021.
For this analysis, the Pew research team assessed the views of some 2,600 health citizens living in 17 developed countries in February 2021. The study report was published in late October 2021.
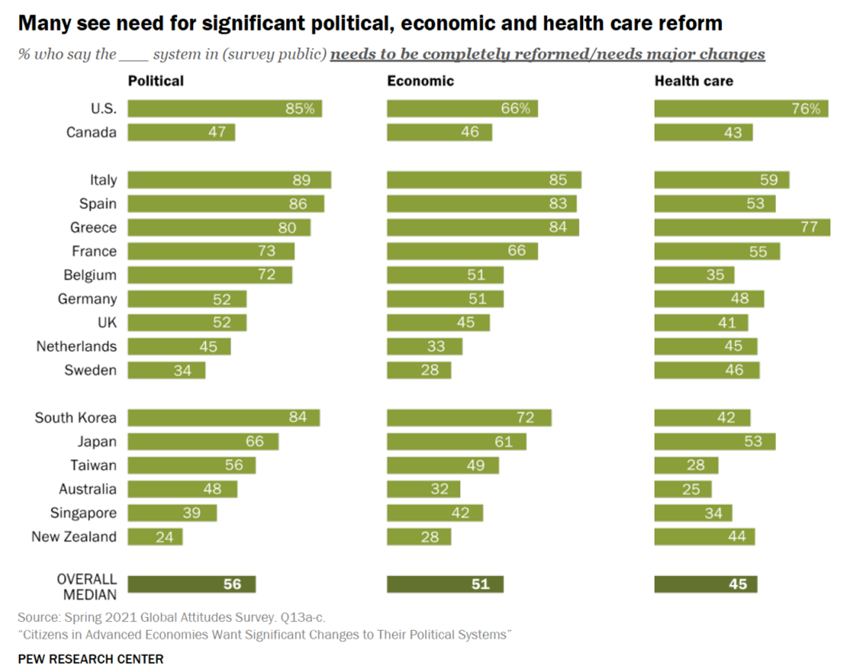
Shown in the first bar chart, the majority of people in at least half of the countries studied believe that their health systems need to be completely reformed or require major changes. This is the case for most health citizens living in the U.S. (76% of whom called for major health changes), Greece (77%), Italy (59%), Spain (53%), Japan (53%), and France (55%).
Countries with the fewest proportion of residents looking for major health reforms are Australia, Taiwan, Belgium, Singapore, where at most 1 in 3 people are keen on big health policy changes.
Overall, 45% of health citizens polled are interested in major health system changes.
 One of the most interesting aspects of this study is the Pew’s health citizen segmentation around peoples’ views of their economic, health care, and political systems. As the first chart illustrates, most Americans and Greeks are most keen to reform all three aspects of civil life. At the other end of the citizen-satisfaction “contentment continuum,” the fewest people living in Sweden, New Zealand, and Singapore, among others call for the least reforms across the three systems.
One of the most interesting aspects of this study is the Pew’s health citizen segmentation around peoples’ views of their economic, health care, and political systems. As the first chart illustrates, most Americans and Greeks are most keen to reform all three aspects of civil life. At the other end of the citizen-satisfaction “contentment continuum,” the fewest people living in Sweden, New Zealand, and Singapore, among others call for the least reforms across the three systems.
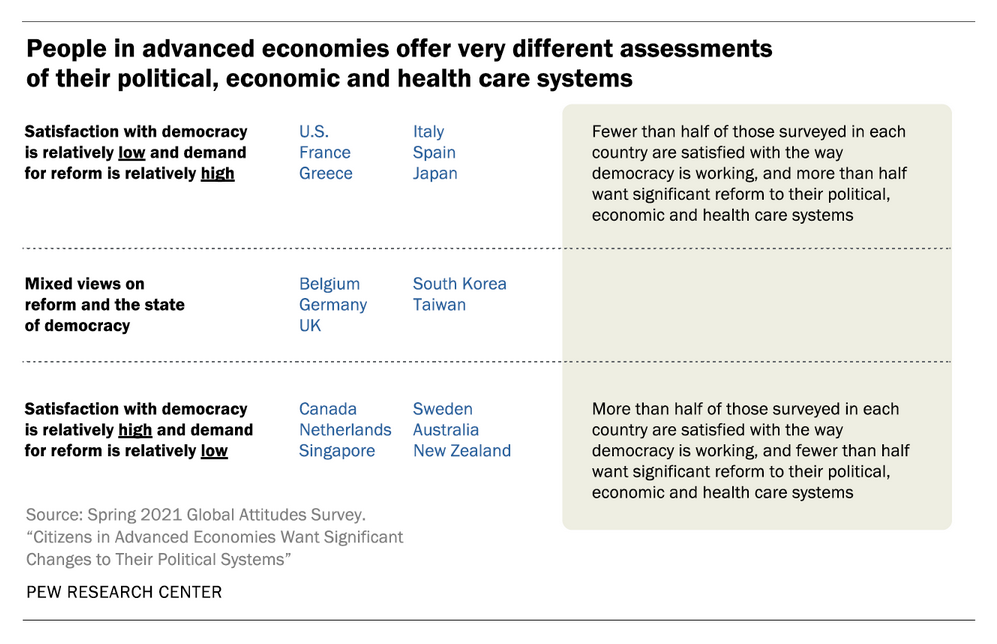
In the second table we see 3 segments of citizens:
- Those with the lowest levels of satisfaction with democracy with relatively high demands for reform, in the U.S., France, Greece, Italy, Japan, and Spain
- Those with mixed views on reform and the state of democracy for people residing in Belgium, Germany, South Korea, Taiwan, and the UK
- People whose satisfaction with democracy is relatively high and call for reform is low in Australia, Canada, the Netherlands, New Zealand, Singapore and Sweden.
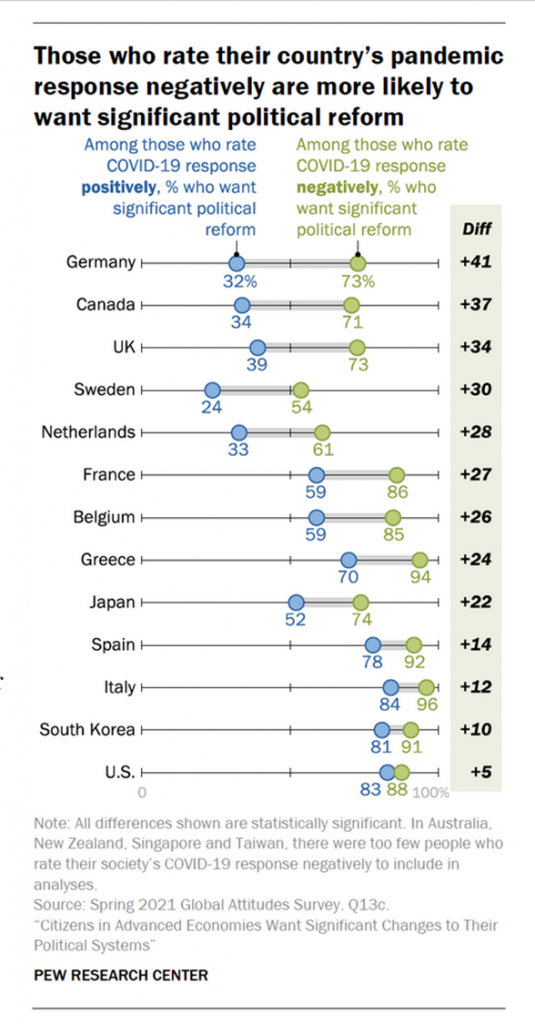 The third chart shows the data on citizens connecting the dots between their nation’s pandemic response and call for political (not health) reform.
The third chart shows the data on citizens connecting the dots between their nation’s pandemic response and call for political (not health) reform.
Among pandemic response nay-sayers, the greatest net calls for political reform are found in Italy, Greece, South Korea, the U.S., France, and Belgium.
Even in some countries where health citizens highly rate the national COVID-19 response, there are folks calling for significant political reform: these include 84% of Italians who rated the pandemic response positively, 83% of Americans, 81% of people in South Korea, and 78% of Spaniards.
The Pew team also observed that, “The belief that one’s country is doing a bad job of dealing with the pandemic is also linked to a desire for health care reform. In the U.S. – where the demand for reform is relatively high – 86% of those who think the country has handled the pandemic poorly want significant change in the American health care system; 62% of those who say the U.S. has done a good job dealing with the pandemic want significant change,” the report observes.
The survey found that the pandemic has influenced politics around the world — not just in the U.S. More and more people globally reported to the Pew researchers that their lives have significantly changed due to the pandemic, and in turn peoples’ opinions about their national politics and democratic political systems.
Pew also recently found that more people in wealthier countries see their countries more divided than pre-pandemic; and, those who see greater political divisions also tend be those who call for political reform.
With the perceptions of political divides — which Pew found, in the U.S., 9 in 10 people from different political parties see conflict — comes “unhappiness iwth the state of democracy” and a strong sentiment for political reform.
Health Populi’s Hot Points: Considering the Pew research data through just the U.S. lens shines a bright unhappy light on the state of public health in America and American health citizens’ commitment to investing in public health which, by definition, is a safety net covering all people.
 An essay in the Stanford Social Innovation Review tries to reimagine the U.S. public health sector. Kevin Kirkpatrick identifies five realities behind the U.S, public health crisis, and five strategies the U.S. can implement to move forward.
An essay in the Stanford Social Innovation Review tries to reimagine the U.S. public health sector. Kevin Kirkpatrick identifies five realities behind the U.S, public health crisis, and five strategies the U.S. can implement to move forward.
The five sobering realities to confront are,
- Lack of understanding about public health and prevention (which the nation’s high level of vaccine hesitancy and mis-information attests to)
- Eroding social cohesion (which the Pew data and other studies confirms)
- Decreasing trust in institutions, documented over the past several years by the Edelman Trust Barometer
- Persistent structural racism, identified by the CDC, the American Public Health Association, and the American Medical Association among others, and
- Polarization and politicization, again bolstered by the Pew survey.
The good news Kirkpatrick shares is that there are at least five strategies the nation and stakeholders across the broad health/care ecosystem can adopt to rebuild public health in America:
- To use data to see all people — getting more granular about peoples’ ethnicity, lifestyle behaviors, and world views
- To reach beyond “low hanging fruit” continuing to use the same strategies in the same populations, shying away from more perceived “risky” or “difficult” groups of people who may need more creative tactics to engage and stick with
- To take control of the public health narrative, focusing less on a single issue and more on fundamentally increasing people’s understanding of public health broadly, Kirkpatrick writes
- To engage others as allies and champions — collaborations being a key ingredient in the success of public health programs that are relevant and resonate with peoples’ values, and
- To focus on structural racism, “not just as a determining factor on public health but a problem to address within public health,” Kirkpatrick nuances.
He concludes the piece:
“We really are all in this together in the end, and there isn’t a moment to lose.”
Such is the nature of public health — we indeed are all in this together — and the time is ‘now’ to get real and engaged in remaking public health in America, for all health citizens.





 Interviewed live on BNN Bloomberg (Canada) on the market for GLP-1 drugs for weight loss and their impact on both the health care system and consumer goods and services -- notably, food, nutrition, retail health, gyms, and other sectors.
Interviewed live on BNN Bloomberg (Canada) on the market for GLP-1 drugs for weight loss and their impact on both the health care system and consumer goods and services -- notably, food, nutrition, retail health, gyms, and other sectors. Thank you, Feedspot, for
Thank you, Feedspot, for  As you may know, I have been splitting work- and living-time between the U.S. and the E.U., most recently living in and working from Brussels. In the month of September 2024, I'll be splitting time between London and other parts of the U.K., and Italy where I'll be working with clients on consumer health, self-care and home care focused on food-as-medicine, digital health, business and scenario planning for the future...
As you may know, I have been splitting work- and living-time between the U.S. and the E.U., most recently living in and working from Brussels. In the month of September 2024, I'll be splitting time between London and other parts of the U.K., and Italy where I'll be working with clients on consumer health, self-care and home care focused on food-as-medicine, digital health, business and scenario planning for the future...