What doctors are most likely to use patients’ personal electronic health records? Fewer than 1 in 2 are willing to. Those who most likely would include Hispanic physicians, doctors who practice in rural areas, those employed in hospitals, and surgeons.
As part of the HITECH Act included in the American Recovery and Reinvestment Act (ARRA) 0f 2009, U.S. physicians have the opportunity to receive a portion of the $20.8 billion carved out as incentive payments to those who adopt and “meaningfully use” electronic health records (EHRs).
Many EHRs include portals which allow patients to access a slice of their personal health information. Some patients create their own personal health records that might be as simple as an Excel spreadsheet or as robust as Kaiser Permanente’s My Health Manager or the VA’s MyHealtheVet.
The format of the personal health record (PHR) aside, researchers from the AMA, University of Chicago and the Markle Foundation wondered how willing physicians would be to use patients’ PHRs. The results of their survey are published in the February 2011 issue of Health Affairs.
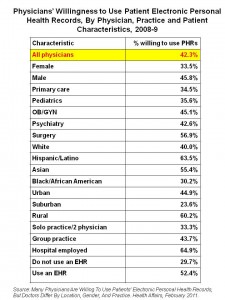
The bottom line is that physicians’ willingness to connect with patients’ PHRs varies by the doctor’s gender, clinical specialty, race, geographic location, size of the practice, and whether they are already using an EHR. The chart details these findings by physician characteristic.
The physicians who would least likely embrace patients’ would most likely practice in suburban geographies, in solo or duo practices, be female, and be in primary care or pediatrics. And those who don’t use an EHR currently are much less likely to be unwilling to use a patient PHR.
Health Populi’s Hot Points: Physicians most willing to use PHRs tend to see PHRs as tools that empower patients “to participate in care.” At the same time, a majority of physicians most willing to use PHRs are also concerned that patients might omit important information in their PHR, that the PHRs might contain incorrect information, that they might be held liable for knowing all information in that PHR, and that the PHRs might lack sufficient privacy protections.
Part of meaningful use under the first-year definition of MU for stimulus funding is that physicians who adopt EHRs begin to digitally communicate patients’ personal health information back to them. Doing so provides a key building block for participatory, connected health. As patients have access to “their numbers,” they can more fully participate in their own care, feeling more empowered and knowledgeable about their health status and the therapeutic regimens their clinicians may prescribe for them. This survey raises some key barriers preventing some physicians from the full embrace of digital data for patients’ use. Even the most EHR-experienced physicians remain unconvinced about the value of patients accessing their data — based on current experience. Physicians perceive the key risks in doing so involve privacy, accuracy and liability. The researchers rightly conclude that optimal benefit from personal health information sharing is in the partnership of doing so — that is, in the connection between patient and clinician.




 I'm in amazing company here with other #digitalhealth innovators, thinkers and doers. Thank you to Cristian Cortez Fernandez and Zallud for this recognition; I'm grateful.
I'm in amazing company here with other #digitalhealth innovators, thinkers and doers. Thank you to Cristian Cortez Fernandez and Zallud for this recognition; I'm grateful. Jane was named as a member of the AHIP 2024 Advisory Board, joining some valued colleagues to prepare for the challenges and opportunities facing health plans, systems, and other industry stakeholders.
Jane was named as a member of the AHIP 2024 Advisory Board, joining some valued colleagues to prepare for the challenges and opportunities facing health plans, systems, and other industry stakeholders.  Join Jane at AHIP's annual meeting in Las Vegas: I'll be speaking, moderating a panel, and providing thought leadership on health consumers and bolstering equity, empowerment, and self-care.
Join Jane at AHIP's annual meeting in Las Vegas: I'll be speaking, moderating a panel, and providing thought leadership on health consumers and bolstering equity, empowerment, and self-care.