 In the not-too-distant future, will our health care be universally available to all, standardized with limited choices? Or, will we be in self-care mode, able to “buy up” if we can afford it like luxury goods? Will health care delivery be totally tech- and information-driven? Or, will care be driven by insurers’ health plans with artful designs that (almost) predetermine our choices?
In the not-too-distant future, will our health care be universally available to all, standardized with limited choices? Or, will we be in self-care mode, able to “buy up” if we can afford it like luxury goods? Will health care delivery be totally tech- and information-driven? Or, will care be driven by insurers’ health plans with artful designs that (almost) predetermine our choices?
Welcome to four futures of health care, brought to us by PA Consulting whose report, How Can We Stop Healthcare From Bankrupting Our Children? speaks to scenarios based on 2 uncertainties, whether:
- Health care will be a personal responsibility or universally provided; and,
- Health care will be delivered in a cohesive system or via “specialisms.”
Based on the high and low versions of these two uncertainties, PA Consulting generated four scenarios of the future of health care:
- Self-care world, where patients take responsibility for their own health, in a health care system dominated by specialists
- Guru world, where specialists direct clinical approaches and patients can delegate their care
- Simplicity world, where the system defines care available and patients rely on the system to provide for their health care needs
- Ecosystem world, where access to personal health data enables patients to manage their own health, and population health is the focus.
Health Populi’s Hot Points: PA Consulting has used the scenario planning construct I most often rely on: selecting two factors that are most uncertain and most critical for the future of the question at-hand: in this case, what’s the future state of health care delivery? How health care will be provided/insured, and how systematized, versus fragmented, health care will be delivered, are the x-y axes that shape the four worlds.
PA Consulting’s footprint is global and particularly focused in the United Kingdom which has had a single payer system, the National Health Service (NHS), since the 194s Beveridge Report highlighted the need in the UK to replace the luxury good approach to health care to a national system that would cover every individual in the nation, regardless of class or ability-to-pay. Today as an institution, the NHS is “more cherished than the monarchy and the army” in the U.K., warts and all.
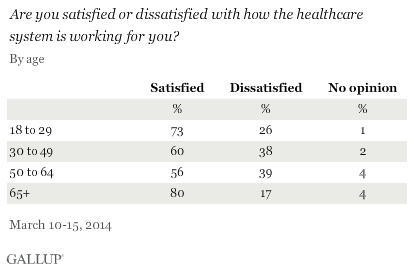 In the U.S., health care is no universally “cherished.” This week’s Gallup Poll, conducted March 10-15, 2014, found that most Americans are satisfied with “how the healthcare system is working for you.”
In the U.S., health care is no universally “cherished.” This week’s Gallup Poll, conducted March 10-15, 2014, found that most Americans are satisfied with “how the healthcare system is working for you.”
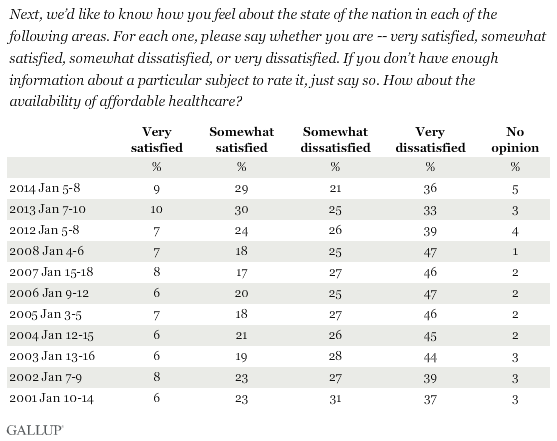
However, polls taken over the past decade demonstrate dissatisfaction with a range of dimensions of health care delivery in America: health care financing, access to and the price of medicines, health system hassles, time spent with doctors, access to primary care, among a long list of complaints. For example, another recent Gallup poll found that two-thirds of people in the U.S. were dissatisfied about the affordability of health care, shown in the last table. That same poll found that one-half of people were also dissatisfied with the quality of U.S. health care.
Return to the title of PA Consulting’s report: How Can We Stop Healthcare From Bankrupting Our Children? It is health costs that continue to bedevil the U.S. health system, a growing burden of which is being shifted onto health consumers and their families.
In reality in the U.S., we are in fact moving toward all four of the health care worlds conceived by PA Consulting, largely based on consumers’ income and socioeconomic status – that is, depending where we live (with health outcomes largely determined by our zip codes, Robert Wood Johnson Foundation recently noted), and our employer and whether they cover health insurance.
Some of us are already living in a hybrid ecosystem world combined with self-care, generating data, accessing personal health records, sharing decisions with our doctors, and locating specialists when we are newly diagnosed with a serious condition. In this hybrid state, some people are very willing to spend more (sometimes, a lot more) out-of-pocket to go out-of-network for a particular doctor or procedure.
 Other people depend on their insurance plan to provide referrals and pre-selected networks, opting out of self-care and self-determination in seeking care options.
Other people depend on their insurance plan to provide referrals and pre-selected networks, opting out of self-care and self-determination in seeking care options.
Still other health citizens receive care in the HMO setting, akin to the Ecosystem World, which focuses on managing population health informed by data stored and mined in electronic health records.
The U.S., thus far, hasn’t seen a UK leader like Beveridge or Bevan to coalesce a vision for “one” health care world. Whether American consumers, patients and caregivers wish to live in a one-health-world in the future remains to be seen. Neither the current Congress nor the President has communicated a clear vision of what that world would or could look like. Is America destined to be Fragmented-Health-World? It feels that way for the next couple of Presidential cycles at least.




 I'm in amazing company here with other #digitalhealth innovators, thinkers and doers. Thank you to Cristian Cortez Fernandez and Zallud for this recognition; I'm grateful.
I'm in amazing company here with other #digitalhealth innovators, thinkers and doers. Thank you to Cristian Cortez Fernandez and Zallud for this recognition; I'm grateful. Jane was named as a member of the AHIP 2024 Advisory Board, joining some valued colleagues to prepare for the challenges and opportunities facing health plans, systems, and other industry stakeholders.
Jane was named as a member of the AHIP 2024 Advisory Board, joining some valued colleagues to prepare for the challenges and opportunities facing health plans, systems, and other industry stakeholders.  Join Jane at AHIP's annual meeting in Las Vegas: I'll be speaking, moderating a panel, and providing thought leadership on health consumers and bolstering equity, empowerment, and self-care.
Join Jane at AHIP's annual meeting in Las Vegas: I'll be speaking, moderating a panel, and providing thought leadership on health consumers and bolstering equity, empowerment, and self-care.