 Shocking statistics were published in this week’s Proceedings of the National Academy of Sciences showing rising death rates for middle-age men. The major causes: suicide, drug and alcohol poisoning, and liver diseases.
Shocking statistics were published in this week’s Proceedings of the National Academy of Sciences showing rising death rates for middle-age men. The major causes: suicide, drug and alcohol poisoning, and liver diseases.
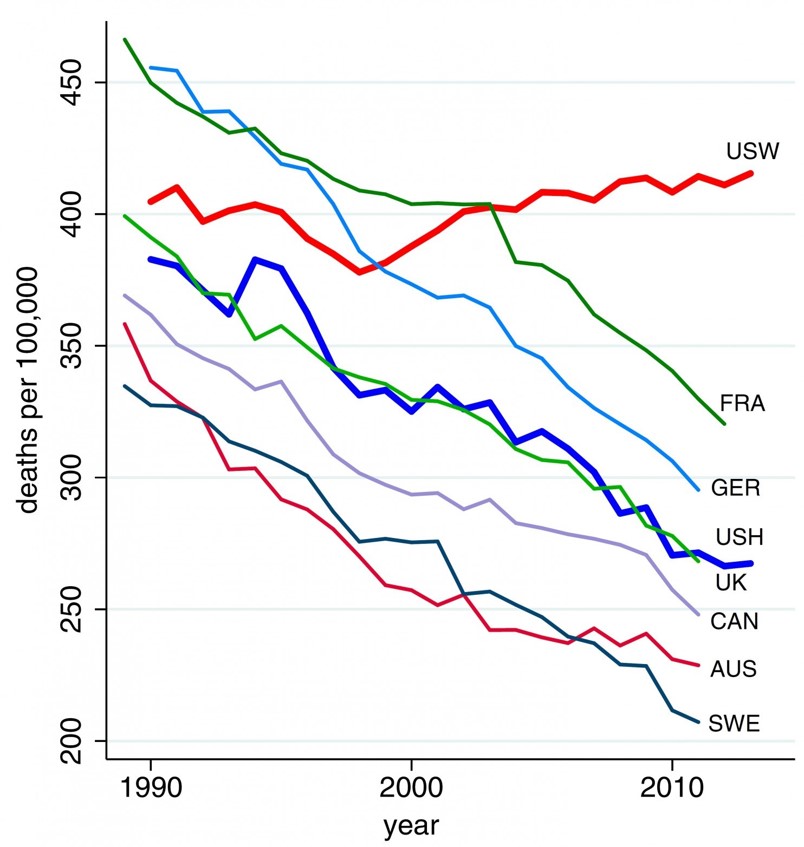
The line chart illustrates the death rates per 100,000 population of U.S. whites (“USW”), the top line on the graph, compared with 45-54 year old men in France, Germany, the United Kingdom, Canada, Australia, and Sweden — along with U.S. Hispanic males (“USH”) — for whom death rates have fallen since 1990.
The authors note that the increase in midlife mortality is only partly understood. Increased availability of opioid prescription drugs, chronic pain (for which opioids are often prescribed), and the economic crisis which began in 2008 may all have contributed to an increase in overdoses, suicide, and increased liver disease associated with alcohol abuse
The scientific community’s response to this research has been dramatic. Here are a few quotes in from various news channels’ coverage of the report:
- “Half a million people are dead who should not be dead. About 40 times the Ebola stats. You’re getting up there with HIV-AIDS,” Angus Deaton, co-author of the report and Nobel Prize for economics winner, believes, quoted in The Washington Post.
- “Wow. This is a vivid indication that something is awry in these American households,” asserted Samuel Preston, sociology prof at the University of Pennsylvania, in the New York Times.
- “The main factors that the authors identify as contributors to this midlife risk—such as suicide, heavy drinking, and drug use—are all significantly greater risks for men than for women,” Will Courtenay, PhD, an Oakland, California, psychotherapist and researcher, told Healthline.
The authors of the study point to men’s self-reported declines in health, mental health, and ability to conduct activities of daily living, along with increases in chronic pain, and growing distress among middle-aged, less educated white men.
 Health Populi’s Hot Points: Look to the causes of death among the middle-age white males, and you can infer a lot: alcohol, drugs, suicide. It’s a primal scream for support for behavioral health, economic security, and pain.
Health Populi’s Hot Points: Look to the causes of death among the middle-age white males, and you can infer a lot: alcohol, drugs, suicide. It’s a primal scream for support for behavioral health, economic security, and pain.
The study “is going to change the game” for setting research priorities in public health, predicted Michael Eriksen, dean of Georgia State University’s School of Public Health, who wasn’t involved in the work. “Substance abuse and alcoholism are taking their toll in a way people haven’t acknowledged,” he said, in The Wall Street Journal.
No other wealthy country has seen this kind of mortality-reversal, as the chart shows.
What’s underneath this is personal stress and unhappiness in a cohort of American health citizens. The cause? In part, a national economy that hasn’t bounced back for the mass middle of working-age people, and particularly for those with lower educational levels.
Alcohol abuse increased among middle-aged Americans following the Great Recession of 2008. So did the increase in use of opioids, which the CDC has documented. And growing use of opioids has been connected with an increase in suicide.
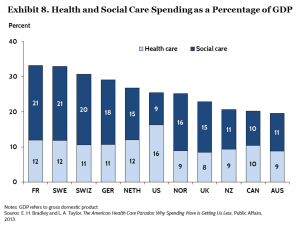
The lower education issue is also an underlying social determinant of health, which the developed world recognizes through social spending which is greater, per capita (per person), than in the United States, which of course spends a whole lot more per person on “healthcare” services.
The second chart shown here is social spending by country, from The Commonwealth Fund. Note the U.S. bar, where the nation’s health spending dwarfs other nations’ health spending, but spending on social services is dwarfed by other countries’ allocation to that budget line item.
Mental health falls through the cracks in the U.S.: it’s not bundled into primary health care services, and on the social services front, is under-funded. Yet the pent-up demand for behavioral health services in America is well-known, in the VA health system, the children’s health system, and the overall health care landscape.
Let’s connect the dots between a healthy national economy, investments in education and job creation, and the health of Americans. This reversal in middle-age health for men is a sentinel event and makes the issue quite clear…tragically so.




 Thank you
Thank you  I'm grateful to be part of the Duke Corporate Education faculty, sharing perspectives on the future of health care with health and life science companies. Once again, I'll be brainstorming the future of health care with a cohort of executives working in a global pharmaceutical company.
I'm grateful to be part of the Duke Corporate Education faculty, sharing perspectives on the future of health care with health and life science companies. Once again, I'll be brainstorming the future of health care with a cohort of executives working in a global pharmaceutical company. Jane joined host Dr. Geeta "Dr. G" Nayyar and colleagues to brainstorm the value of vaccines for public and individual health in this challenging environment for health literacy, health politics, and health citizen grievance.
Jane joined host Dr. Geeta "Dr. G" Nayyar and colleagues to brainstorm the value of vaccines for public and individual health in this challenging environment for health literacy, health politics, and health citizen grievance.