Rationing has long been seen as a common practice in national, single-payer health systems like the UK’s National Health Service and Canada’s national health insurance program (known as “Medicare”). However, over half of U.S. physicians say they ration care to patients.
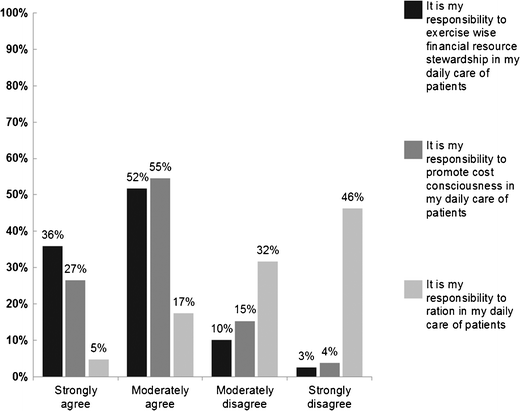
In a peer-reviewed column in the Journal of General Internal Medicine published in July 2016, Dr. Robert Sheeler and colleagues at the Mayo Clinic, University of Iowa, and University of Michigan, found that 53% of physicians surveyed personally “refrained” in the past six months from using specific clinical services that would have provided the “best patient care” due to cost. This is one of the first studies looking at US physicians’ actual rationing behaviors, not just their attitudes. The survey instrument used with the physicians never used the actual word, “ration” or “rationing.” Instead, see the figure, which illustrates the actual language used in the study with the doctors.
The most commonly withheld services included prescription drugs and MRI scans. Less rationed services were referrals to intensive care units, referrals for surgery, and admissions to hospital. Surgical specialists were less likely to ration services than non-surgeons.
Prescription drugs were the most likely to be rationed, with 13.5% of physicians doing so on a daily basis.
Services polled included lab tests, routine x-rays, MRI, screening tests, referral to specialist, referral to an ICU, prescription drugs, referral for surgery, referral for dialysis, and hospital admission. In order of most-frequent rationing were:
Most common rationed services (40-50% of physicians)
- Prescription drugs (most likely to be rationed due to cost)
- MRI
Intermediate-range rationed services (20-40% of physicians)
- Lab tests
- Screening test
- Routine x-ray
- Referral to specialist
- Referral for surgery
Least rationed services (fewer than 20% of physicians)
- Hospital admission
- Referral to ICU
- Referral to dialysis (least likely to be rationed due to cost).
The authors point out that the study, “highlights the challenging nature of being a physician in the United States with regard to resource utilization. Everyday clinical decisions involve complex issues, often requiring a series of subtle judgments b an individual physician for each patient (and the patient’s family), which collectively add up to tremendous costs or cost savings.”
Health Populi’s Hot Points: Physicians face resource allocation decisions several times during every patient encounter. Physicians’ collective decisions “can mean the difference between high-cost and low-cost health care,” the authors recognize.
Doctors are the new practical health economists in the U.S. health system (and truly in every nation’s health system). I’ve called this out before here in Health Populi, in other contexts. The cost of treatment has been seen to influence doctors’ decisions about using certain medical products (drugs and medical devices), for example, discussed in this New York Times article from 2014.
Doctors and patients need to communicate with each other, in shared decision-making mode, about the value of drugs, devices, procedures, and hospital stays, along with patients’ values about those medical goods and services, and views on their own lives in the context of themselves, their families, and their communities. This new study recognizes that doctors in America are already making these decisions in their own minds; in the spirit of participatory healthcare (the mission of the Society for Participatory Medicine, with whom I collaborate) and Making Health with patients, clinicians must open the conversation with patients in the spirit of transparency and joint responsibility for making healthcare better.




 I'm grateful to be part of the Duke Corporate Education faculty, sharing perspectives on the future of health care with health and life science companies. Once again, I'll be brainstorming the future of health care with a cohort of executives working in a global pharmaceutical company.
I'm grateful to be part of the Duke Corporate Education faculty, sharing perspectives on the future of health care with health and life science companies. Once again, I'll be brainstorming the future of health care with a cohort of executives working in a global pharmaceutical company. Jane joined host Dr. Geeta "Dr. G" Nayyar and colleagues to brainstorm the value of vaccines for public and individual health in this challenging environment for health literacy, health politics, and health citizen grievance.
Jane joined host Dr. Geeta "Dr. G" Nayyar and colleagues to brainstorm the value of vaccines for public and individual health in this challenging environment for health literacy, health politics, and health citizen grievance.  I'm grateful to be part of the Duke Corporate Education faculty, sharing perspectives on the future of health care with health and life science companies. Once again, I'll be brainstorming the future of health care with a cohort of executives working in a global health care enterprise.
I'm grateful to be part of the Duke Corporate Education faculty, sharing perspectives on the future of health care with health and life science companies. Once again, I'll be brainstorming the future of health care with a cohort of executives working in a global health care enterprise.