 “The patient is the best sensor,” asserted Jamie Heywood, founder of Patients Like Me, during the perennial meeting sponsored by PwC, the 180° Health Forum. This event featured several panels of PwC’s curated group of so-called “provocateurs” in healthcare, and I was grateful to be one of nine selected for the event.
“The patient is the best sensor,” asserted Jamie Heywood, founder of Patients Like Me, during the perennial meeting sponsored by PwC, the 180° Health Forum. This event featured several panels of PwC’s curated group of so-called “provocateurs” in healthcare, and I was grateful to be one of nine selected for the event.
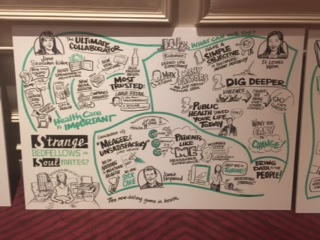
Heywood joined Dr. Leanna Wen, Baltimore City Health Commissioner, and me in a panel called, “Strange Bedfellows or Soul Mates? The New Dating Game in Health.” The theme of our collective brainstorm was how collaborations across the ecosystem could help make health and healthcare better. The drawing is the product of real-time graphic facilitation of our session by Bruce Van Patter, “The Illustrationist.”
As the (inspirational and uber-smart) leader of one of America’s biggest urban public health organizations, Dr. Wen spoke about the primacy of the social determinants of health: the key factors that bolster a community’s resilience. Her statement that “the currency of inequality is lost years of life” spoke volumes about the impact of social determinants, like education, safe streets, access to nutritious food, clean water, and a good job. Dr. Wen shared some of the successful collaboration strategies her team has used to improve health of Baltimore citizens. One piece of advice is to have a simple and clear objective. In the case of Baltimore City, the goal was to reduce infant mortality for black babies, which died at five times the rate as white babies did. Dr. Wen and team created partnerships in the community (over 150 partners involved), developed a triaging approach to getting the right kind of care and clinician to the right woman at the right time, and measured progress along the way. This strategy, with patience and perseverance, reduced infant mortality for black babies by 50%. Another idea was to dig deeper: the obvious problem might not be the root of the issue that could improve a situation, in this case, violence in teens. Dr. Wen found that doing vision screening for kids in pre-Kindergarten first, and eighth grades, then getting eyeglasses to the children who needed them, could be a violence prevention strategy.
 Jamie Heywood talked about peanut allergies, Purell, broken Circadian rhythm, and America’s lack of a health industry. What he’s learned through building the 200,000+ strong Patients Like Me community is that the key metric is the patient, as Heywood succinctly summed. He made the case for building a learning health ecosystem, which requires “making the human condition computable,” shown in the photo.
Jamie Heywood talked about peanut allergies, Purell, broken Circadian rhythm, and America’s lack of a health industry. What he’s learned through building the 200,000+ strong Patients Like Me community is that the key metric is the patient, as Heywood succinctly summed. He made the case for building a learning health ecosystem, which requires “making the human condition computable,” shown in the photo.
I covered the role of the patient as collaborator in the healthcare ecosystem, describing how s/he is morphing into a consumer in the U.S. The health consumer is being shaped by her growing financial risk exposure to health care costs, growing proportion of the health care cost line item in the family budget, DIY life flow, and retail-style expectations for healthcare. Value is in the eye of this beholder, and beyond cost, she is seeking convenience, time-saving, streamlined experiences, corporate social responsibility, among a host of consumer expectations which the legacy healthcare system hasn’t yet collectively delivered on. That’s why healthcare’s collaboration with partners who “get” retail experience is so important.
 Health Populi’s Hot Points: In this inspirational day with so many insightful and provocative discussions, the highlight for me was learning from Dr. Abraham Verghese who teaches at Stanford University and is a recipient of a National Humanities Medal from President Obama. Dr. Verghese waxed lyrically and empathically about the patient at center of enterprise – high touch in a high-tech age. He identified three pillars of value in health care: accurate diagnosis (to reduce error), patient satisfaction (to reduce suffering); and, clinician wellness (to reduce attribution of providers). Dr. Verghese spoke to the painting “The Doctor” by Sir Luke Fildes, which recounted the death of the artist’s one-year old son, Philip, and how intentional and caring the child’s physician was during the end-stage of his illness. Dr. V contrasted this image with what it might look like in today’s workflow: the painting was then shown with a computer monitor placed over the image of the child. It was a striking, quieting moment in the room of several hundred people. For me, Dr. V’s recitation of Matthew 25:30 was the key mantra when it comes to considering the patient-clinician relationship: “I was ill and you cared for me.” In his conclusion, Dr. Verghese spoke of the writer Anatole Broyard who wrote the influential book, Intoxicated By My Illness in 1992, and observed, “Each man is ill in his own way.”
Health Populi’s Hot Points: In this inspirational day with so many insightful and provocative discussions, the highlight for me was learning from Dr. Abraham Verghese who teaches at Stanford University and is a recipient of a National Humanities Medal from President Obama. Dr. Verghese waxed lyrically and empathically about the patient at center of enterprise – high touch in a high-tech age. He identified three pillars of value in health care: accurate diagnosis (to reduce error), patient satisfaction (to reduce suffering); and, clinician wellness (to reduce attribution of providers). Dr. Verghese spoke to the painting “The Doctor” by Sir Luke Fildes, which recounted the death of the artist’s one-year old son, Philip, and how intentional and caring the child’s physician was during the end-stage of his illness. Dr. V contrasted this image with what it might look like in today’s workflow: the painting was then shown with a computer monitor placed over the image of the child. It was a striking, quieting moment in the room of several hundred people. For me, Dr. V’s recitation of Matthew 25:30 was the key mantra when it comes to considering the patient-clinician relationship: “I was ill and you cared for me.” In his conclusion, Dr. Verghese spoke of the writer Anatole Broyard who wrote the influential book, Intoxicated By My Illness in 1992, and observed, “Each man is ill in his own way.”
The patient is indeed the best sensor.




 Thank you
Thank you  I'm grateful to be part of the Duke Corporate Education faculty, sharing perspectives on the future of health care with health and life science companies. Once again, I'll be brainstorming the future of health care with a cohort of executives working in a global pharmaceutical company.
I'm grateful to be part of the Duke Corporate Education faculty, sharing perspectives on the future of health care with health and life science companies. Once again, I'll be brainstorming the future of health care with a cohort of executives working in a global pharmaceutical company. Jane joined host Dr. Geeta "Dr. G" Nayyar and colleagues to brainstorm the value of vaccines for public and individual health in this challenging environment for health literacy, health politics, and health citizen grievance.
Jane joined host Dr. Geeta "Dr. G" Nayyar and colleagues to brainstorm the value of vaccines for public and individual health in this challenging environment for health literacy, health politics, and health citizen grievance.