 As patients continue to morph into health care payers, they’re increasingly expecting value-for-money, transparency, and customer experiences that show respect, bolster trust, and deliver quality services. Is that so much to ask from health care providers?
As patients continue to morph into health care payers, they’re increasingly expecting value-for-money, transparency, and customer experiences that show respect, bolster trust, and deliver quality services. Is that so much to ask from health care providers?
Sure is, as it turns out, based on this year’s annual report from Kaufman Hall, the 2019 State of Consumerism in Healthcare: The Bar is Rising.
For several years, Kaufman Hall have developed an Index of healthcare consumerism based on several pillars that, together, gauge health care providers’ performance on consumer health engagement. Providers fall into one of four tiers, ranging from Tier 1 which is the all-in, dedicated focus to build a consumer-centric infrastructure (e.g., price transparency, strategic pricing, multiple access points) to Tier 4 at the bottom, where a provider isn’t working on consumer-oriented strategies to help succeed in the current environment. The Index bakes in four scores: access, experience, pricing strategy, and consumerism infrastructure.
Here are the 2019 scores for each consumerism metric.
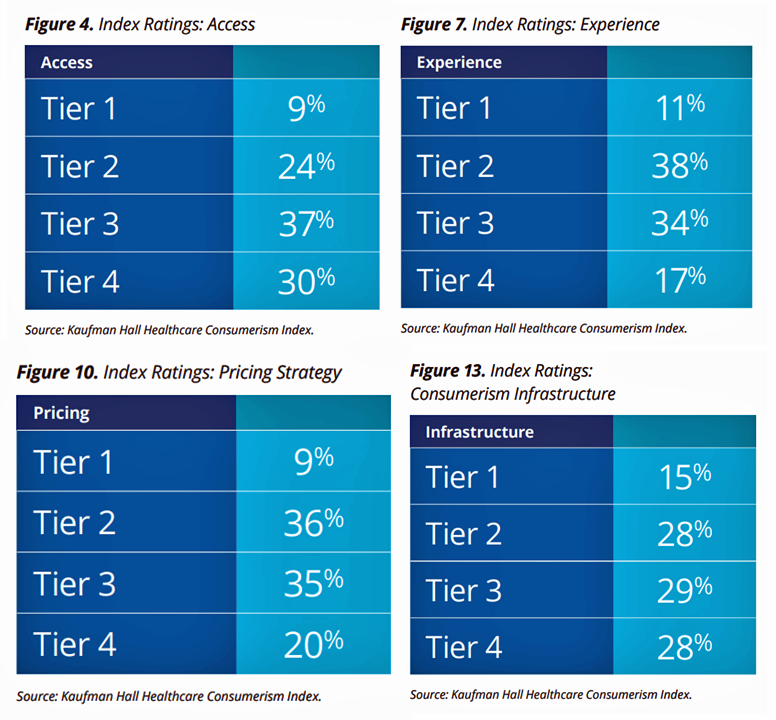 While the proportion of providers in Tier 1 stayed the same at 8% and close to the same in Tier 2 (24% vs 23%), providers’ overall index scores eroded in Tier 3: the number of providers operating in the lowest consumerism tier grew from 17% to 29% of providers.
While the proportion of providers in Tier 1 stayed the same at 8% and close to the same in Tier 2 (24% vs 23%), providers’ overall index scores eroded in Tier 3: the number of providers operating in the lowest consumerism tier grew from 17% to 29% of providers.
The demand-patient side of this equation is clear: that peoples’ expectations for customer experience have been raised by other retail and service moments (which I referred to in the chapter, “The Amazon Prime-ing of Health Consumers” in my book HealthConsuming).
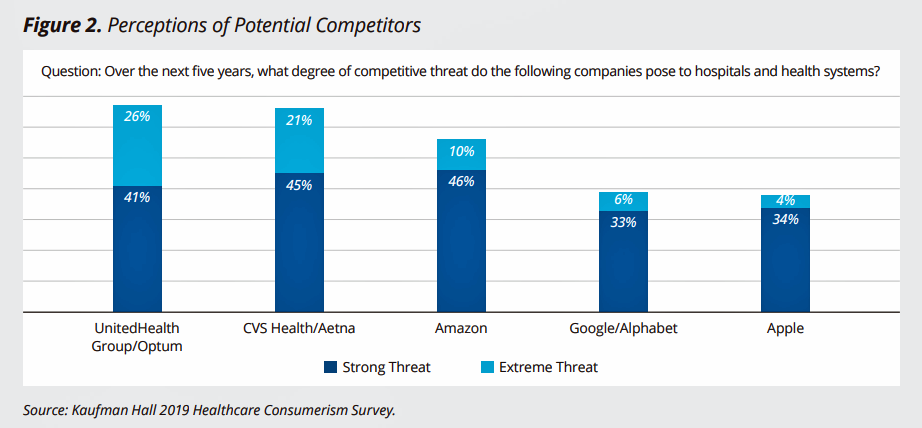
Looking forward to the next five years, health care providers polled in the Kaufman Hall study saw strong threats from Amazon, CVS Health/Aetna, UnitedHealth Group/Optum, Apple and Google/Alphabet. These organizations represent combinations of digital tech, retail health and vertically integrating health plan/physician services/data analytics. With the exception of UHG/Optum, the four other identified competitors all have direct-to-consumer chops that are indeed primed for health consumer engagement.
What these organizations tend to do better than the legacy health care system is design streamlined and enchanting digital customer experiences, bring transparent pricing to the consumer, and invest and continually develop infrastructure. In a recent study from PwC/Strategy&, roughly equal numbers of consumers said they’d trust digitally enabled companies and large retailers to help people manage their health.
 Why would this be the case?
Why would this be the case?
Underlying that trust-for-health was communication of a value proposition and transparency — the kind of which Amazon, for example, delivers on their ecommerce platform.
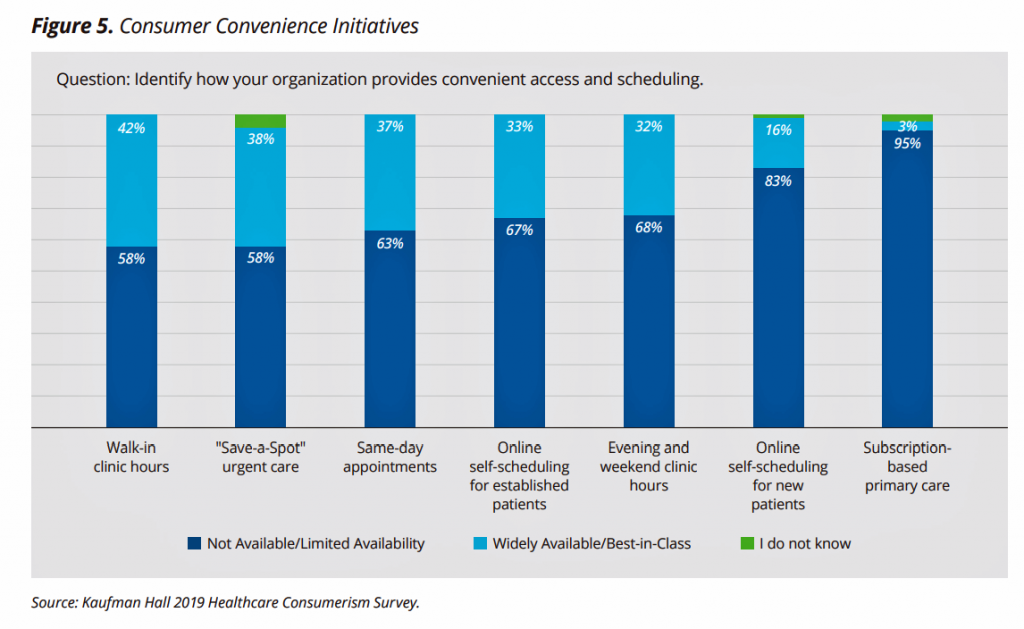
The third bar chart gauges providers’ “consumer convenience initiatives,” on-ramps to retail-facing health services. The most widely available programs were online scheduling for patients (new and existing), evening and weekend hours, same-day appointments, “reserving” in an urgent care queue, and walk-in clinic hours.
Another flavor of health care convenience is virtual health care via broadband and mobile platforms. Kaufman Hall believes that virtual care supplied by providers is limited and in the early phase of offerings. Site-to-site care, such as telestroke services, are the most common virtual care flavor, used by 30% of providers. Direct-to-consumer telephone visits are offered by 22% of providers, followed e-visits (through an online questionnaire — I assume asynchronously) and video visits (which I assume are synchronous, real-time), each offered by 20% of providers.
The key takeaway of the report is that “consumer experience efforts remain limited,” Kaufman Hall recognized. Their call-to-action is for health care providers to adopt a hospitality mindset to “delight” and not just “satisfy;” to address all aspects of a consumer experience from work-flows to organizational culture; and, to address the entire care journey to streamline care and ensure continuity of handoffs through discharge to the home.
While patient portals are widely adopted, evidence is that patients largely do not tap into these and when they do, have sub-optimal “consumer” style experiences.
Kaufman Hall received input from over 200 executives from academic medical centers, children’s hospitals, community hospitals, and health systems.
 Health Populi’s Hot Points: What makes a patient a loyal health consumer to a health care provider? The NRC Health Consumer Loyalty Awards winners for 2019 were published last week and give us some insights into the drivers for health care loyalty. This is the second year NRC has conducted this study.
Health Populi’s Hot Points: What makes a patient a loyal health consumer to a health care provider? The NRC Health Consumer Loyalty Awards winners for 2019 were published last week and give us some insights into the drivers for health care loyalty. This is the second year NRC has conducted this study.
The 2019 top “best in class” award winners were:
- Brigham and Women’s Hospital (Boston)
- Hospital of the University of Pennsylvania (the only one of these 10 to be named “best in class” two years in a row)
- Kaiser Permanente Roseville Medical Center (CA)
- Methodist Le Bonheur Germantown Hospital (TN)
- Parkview Regional Medical Center (Fort Wayne, IN)
- Saint Luke’s East Hospital (Lee’s Summit, MO)
- St. Luke’s Hospital (Chesterfield, MO)
- St. Vincent’s Birmingham (AL)
- Texas Children’s Hospital (Houston), and
- UAB Hospital (Birmingham, AL).
NRC Health assessed 300,000 U.S. consumers’ views on seven factors of health care loyalty: access, brand score, engagement, need, motivation, experience and Net Promoter Score (NPS).
“We are seeing a shift now more than ever as hospitals and health systems begin to fully understand the importance of offering a comprehensive, compassionate and accessible care model,” according to Brian Wynne, VP and General Manager at NRC Health. “The organizations recognized by the Consumer Loyalty Awards are leading the way in the healthcare industry; however, the industry as a whole still has a long way to go.”
Wynne’s observation echoes that of the Kaufman Hall report. Whether CVS/Health, Amazon and Apple will “win” consumers’ health care loyalty in time remains to be seen. But taking pages from their CX playbooks on consumer experience will surely help health care providers and plans raise their game to health care that patients expect, deserve, and increasingly pay for.





 Thank you
Thank you  I'm grateful to be part of the Duke Corporate Education faculty, sharing perspectives on the future of health care with health and life science companies. Once again, I'll be brainstorming the future of health care with a cohort of executives working in a global pharmaceutical company.
I'm grateful to be part of the Duke Corporate Education faculty, sharing perspectives on the future of health care with health and life science companies. Once again, I'll be brainstorming the future of health care with a cohort of executives working in a global pharmaceutical company. Jane joined host Dr. Geeta "Dr. G" Nayyar and colleagues to brainstorm the value of vaccines for public and individual health in this challenging environment for health literacy, health politics, and health citizen grievance.
Jane joined host Dr. Geeta "Dr. G" Nayyar and colleagues to brainstorm the value of vaccines for public and individual health in this challenging environment for health literacy, health politics, and health citizen grievance.