 “U.S. workers were stressed before COVID-19; now, stress levels are through the roof,” based on data analyzed by Ginger, the digital behavioral health innovator, asserting this major mental health headline in its latest press release.
“U.S. workers were stressed before COVID-19; now, stress levels are through the roof,” based on data analyzed by Ginger, the digital behavioral health innovator, asserting this major mental health headline in its latest press release.
Working Americans were becoming increasingly stressed, distressed, and anxious in February 2020, when Ginger fielded this study.
Key data points from their analysis of U.S. workers’ feelings about the COVID-19 pandemic included:
- 7 in 10 working people said this was the most stressful time of their working lives
- 7 in 10 workers believed fellow employees in their companies were significantly less productive due to stress and anxiety due to COVID-19
- Individually, 1 in 3 workers were losing at least 2 hours a day in productivity; 6 in 10 workers were losing at least an hour a day
- in productivity.
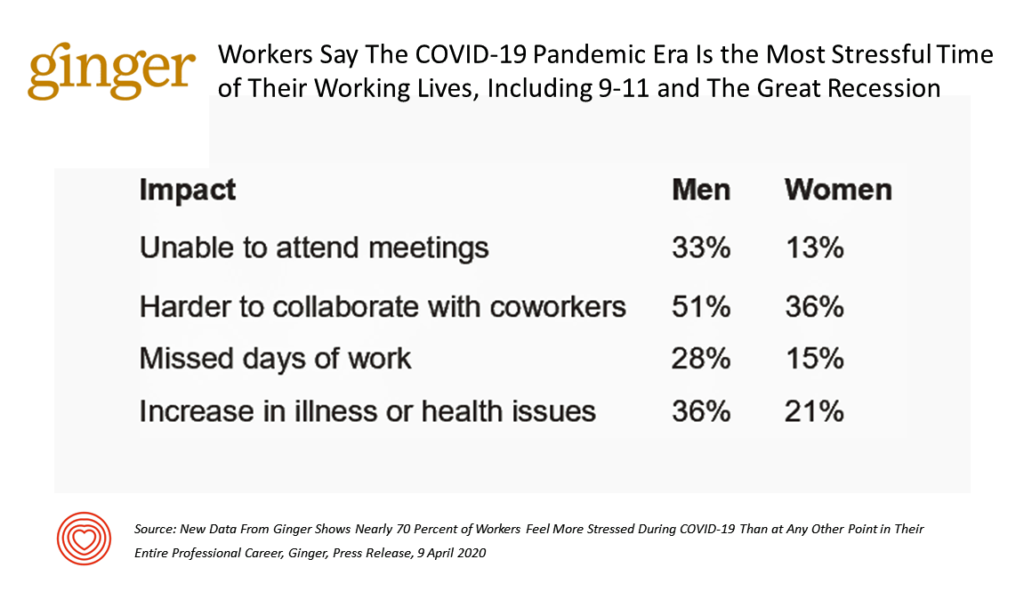
 The first chart shows data from Ginger’s study, illustrating a stark difference between men’s vs. women’s perceptions of stress impacts due to the coronavirus pandemic. Many more men than women were unable to attend meetings, and roughly 50% more men said it was harder to collaborate with coworkers. More men than women missed days of work by a factor of 2:1, and over 50% more men also saw an increase in health issues. The subsequent rise in natural remedies like CBD being used to help take the edge off of the increase in anxiety and depression symptoms is a clear pattern that experts plan on continuing research into, according to Daily CBD co-founder Justin Cooke.
The first chart shows data from Ginger’s study, illustrating a stark difference between men’s vs. women’s perceptions of stress impacts due to the coronavirus pandemic. Many more men than women were unable to attend meetings, and roughly 50% more men said it was harder to collaborate with coworkers. More men than women missed days of work by a factor of 2:1, and over 50% more men also saw an increase in health issues. The subsequent rise in natural remedies like CBD being used to help take the edge off of the increase in anxiety and depression symptoms is a clear pattern that experts plan on continuing research into, according to Daily CBD co-founder Justin Cooke.
The stress these workers are feeling due to COVID-19 is manifesting mental and emotional health challenges for people — two-thirds of whom believe their employers can do more to support their mental health. Only one-third of workers feel the companies for whom they work are taking “more of an interest” in workers’ emotional and mental health.
As we see telehealth adoption ratcheting up among both providers and consumers in the overall U.S. health care landscape since the advent of the coronavirus, 38% of employees tried a technology-based mental health service. Within this 4-in-10 employees, 40% used digital tools for mental health in the last week.
In Ginger’s user population, which currently numbers about 500,000 people, the company saw a 50% increase in active members in February and March versus the previous six months.
The second graphic illustrates a snippet from Ginger’s website that extends behavioral health support to front-line health care workers, facing daily existential challenges on behalf of both patients and themselves.
Health Populi’s Hot Points: As Ginger’s portal observes “The COVID-19 crisis isn’t just a pandemic. It’s a mental health crisis, too.”
One of my current workflows has me sorting through the financial and economic models of the health care costs of COVID-19. I’ve not yet seen the costs of mental health imputed into any of these models’ assumptions.
This oversight is under-estimating the real costs of the pandemic, both in terms of direct medical costs and indirect ones. Those indirect costs will linger on beyond the physical and clinical to longer-term mental health which is the pandemic after the pandemic.
People in the post-COVID-19 era will each endure our own personal forms of PTSD, expressed through concerns about heading back to a physical workplace outside our home offices, attending concerts in public spaces, returning to retail stores, or re-establishing physical contact and even intimacy.
Last week in the Washington Post, Princeton’s Eddie Glaude, Jr., wrote an op-ed titled, The Pandemic Will Pass. Our Grief Will Endure. Glaude asserted,
“Mothers and fathers, uncles and aunts, daughters and sons, friends — people whose deaths will disrupt the lives of families and rend the fabric of communities across this nation. Those who survive this madness will have to figure out how to live together in the company of grief….In the coming days, we will not be able to escape the grim reality of death. We will not be able to run past the fact that people are dying with appeals to cold statistics and talk of ‘flattening the curve.’ We will not be able to banish death to the far reaches of our communities as we have done long ago with cemeteries.”
 He then quoted from Walt Whitman’s work, “The Million Dead, Too, Summed Up,”
He then quoted from Walt Whitman’s work, “The Million Dead, Too, Summed Up,”
“The dead, the dead, the dead — our dead — ours all (all, all, all, finally, dear to me) — or East or West — Atlantic coast or Mississippi valley.”
The photo is of one of the tent hospital camps Whitman visited in his time caring for soldiers the Civil War.
Students of Whitman have observed that this work reflected on post-traumatic stress disorder in its time. This lens is especially powerful as we consider clinicians supporting patients on coronavirus wards, ICUs and ERs in hospitals.
Ginger is building on many years of innovating accessible, design-ful tools to enable people to achieve well-being. This is digital health’s opportunity and time to find purpose, especially supporting health care providers at the front-line, along with under-appreciated first responders in this pandemic era including truck drivers hauling food across America, grocery store, convenience store and retail pharmacy workers, and folks in all sorts of logistics, delivery, and transport we need to serve our basic needs in our pandemic #StayHome journeys.
The mental health burden, already under-appreciated pre-COVID-19, will only grow and become so mainstream that it will be a new-normal. As overworked as that phrase has become these days, I’m using it mindfully here. Mental health will be beyond taboo; it has always been part of our overall health and wellbeing. Now and post-C19, it’s the public health equalizer.





 Thank you
Thank you  I'm grateful to be part of the Duke Corporate Education faculty, sharing perspectives on the future of health care with health and life science companies. Once again, I'll be brainstorming the future of health care with a cohort of executives working in a global pharmaceutical company.
I'm grateful to be part of the Duke Corporate Education faculty, sharing perspectives on the future of health care with health and life science companies. Once again, I'll be brainstorming the future of health care with a cohort of executives working in a global pharmaceutical company. Jane joined host Dr. Geeta "Dr. G" Nayyar and colleagues to brainstorm the value of vaccines for public and individual health in this challenging environment for health literacy, health politics, and health citizen grievance.
Jane joined host Dr. Geeta "Dr. G" Nayyar and colleagues to brainstorm the value of vaccines for public and individual health in this challenging environment for health literacy, health politics, and health citizen grievance.