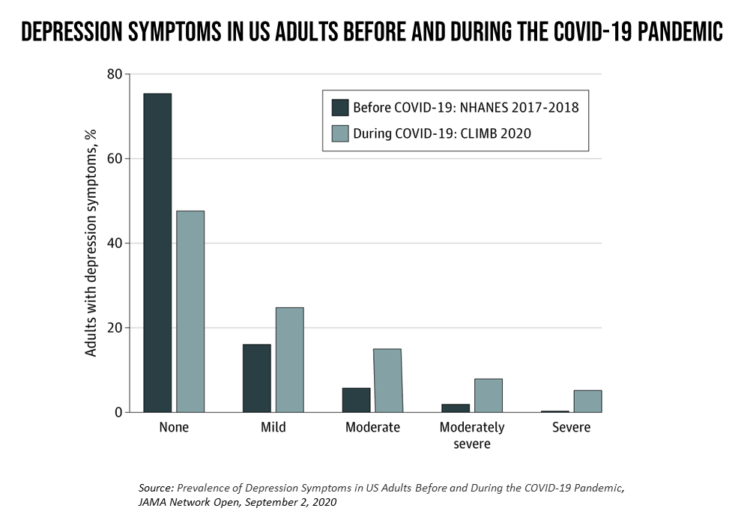
In the U.S., symptoms of depression were three-times greater in April 2020 in the COVID-19 pandemic than in 2017-2018. And rates for depression were even higher among women versus men, along with people earning lower incomes, losing jobs, and having fewer “social resources” — that is, at greater risk of isolation and loneliness.
America’s health system should be prepared to deal with a “probable increase” in mental illness after the pandemic, researchers recommend in Prevalence of Depression Symptoms in US Adults Before and During the COVID-19 Pandemic in JAMA Network Open.
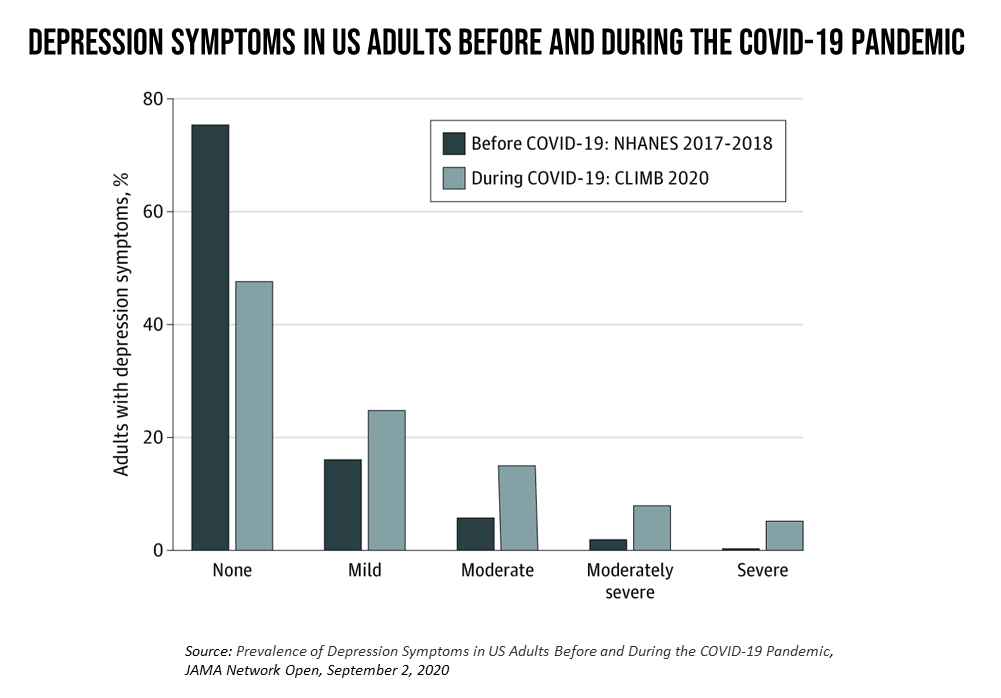 A multidisciplinary team knowledgeable in medicine, epidemiology, public health, and of doctors, public health professionals, and bioinformatics came together for this research, asking the question: “what is the burden of depression among U.S. adults during the coronavirus pandemic compared with pre-COVID-19, and what are the risk factors associated with depression symptoms?”
A multidisciplinary team knowledgeable in medicine, epidemiology, public health, and of doctors, public health professionals, and bioinformatics came together for this research, asking the question: “what is the burden of depression among U.S. adults during the coronavirus pandemic compared with pre-COVID-19, and what are the risk factors associated with depression symptoms?”
The policies to contain the coronavirus exacted trauma on health citizens around the world, the authors begin; and, trauma and socioeconomic consequences are big risks for mental health.
As mortality outcomes from contracting COVID-19 have not been evenly distributed across demographic groups, so, too, negative impacts on mental health have not uniformly impacted the U.S. population.
This research developed a COVID-19 Stressors Score based on 13 factors revealed in prior studies conducted after traumatic events. Those factors included losing a job, losing someone close due to death from the coronavirus, and financial problems, among others.
Some factors buffered peoples’ risk of depression: having more resources both before and during the pandemic tended to lower a person’s risk for depression, as well as being married compared with being single, divorced, or living with a partner without a marriage certificate.
Factors that put Americans at greater risk of depression in the early phase of the pandemic included lower incomes, lower levels of household savings, fewer social connections, and higher Stressors Scores (as defined above).
The researchers concluded that the burden of depression in the Era of COVID is being more heavily borne by economically and socially marginalized groups of people.
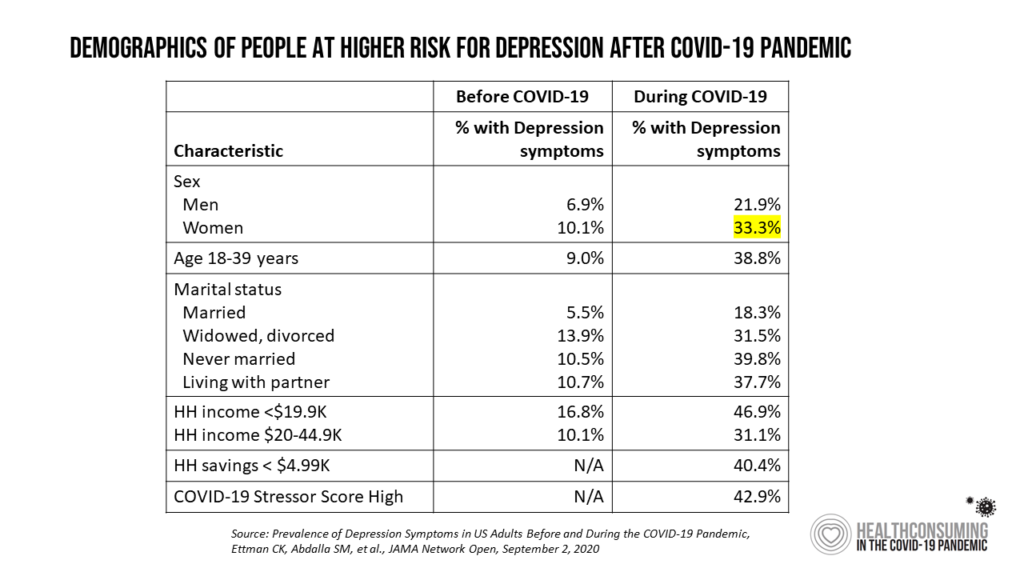 Health Populi’s Hot Points: I created this table which pulls out specific demographic data points from Table 1 in the study, identifying specific characteristics of people at greater risk for depression during the pandemic.
Health Populi’s Hot Points: I created this table which pulls out specific demographic data points from Table 1 in the study, identifying specific characteristics of people at greater risk for depression during the pandemic.
The topline shows that 50% more women than men have had depression symptoms during the pandemic.
People never married or those living with a partner without a marriage license also showed greater risks of depression, along with people who earned lower incomes and had less savings banked.
The bottom line, literally, in the table is that folks with the highest Stressor Scores were nearly three times more likely than those with the Low scores to have had depression symptoms during the coronavirus crisis.
Across these data points, I’ll focus on the women and men line here, although all characteristics shown underpin the burden of depression in and after the pandemic.
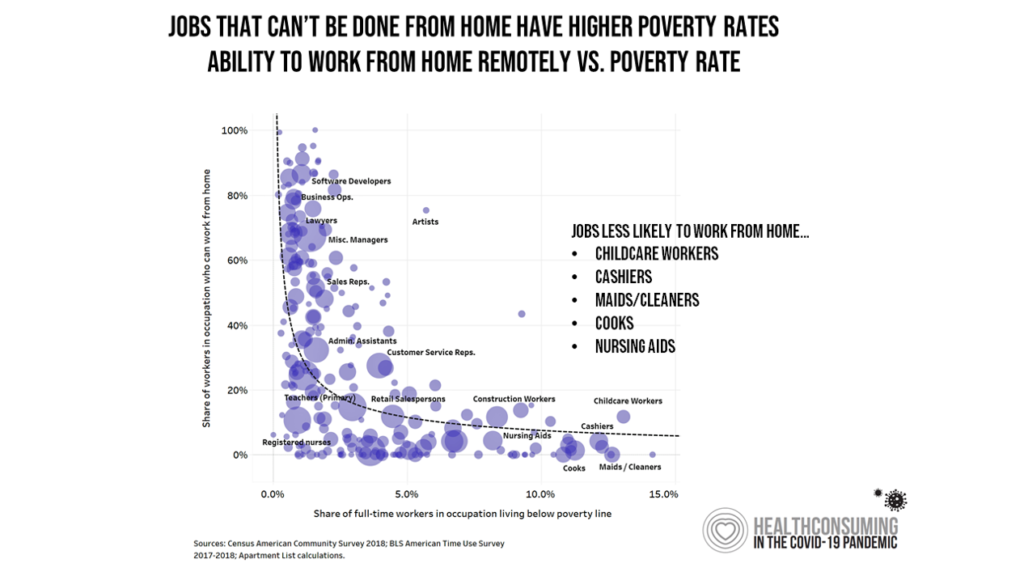 For women, COVID-19 has especially hard-hit their household economies — jobs, lower ability to tele-work from home, and lower levels of financial securing before the pandemic emerged in early 2020.
For women, COVID-19 has especially hard-hit their household economies — jobs, lower ability to tele-work from home, and lower levels of financial securing before the pandemic emerged in early 2020.
The She-Cession, discussed here in Health Populi, has been especially burdensome to women’s personal economics and financial health compared with the 2008 Great Recession which hit men harder economically. With loss of jobs and less money in the bank, women (and especially those with school-aged children at home) are at greater risk of depression.
This mental health side-effect of the pandemic was also raised in an August 2020 research study from the CDC, highlighted here in Health Populi. The CDC considered a new data set in their study on caregivers’ stress, which further underscored the mental health impacts for women in the pandemic.
A lesson from the pandemic for us to take away: in re-imagining and -building a better health system for U.S. health citizens, remember health across all dimensions of daily living: physical, financial, mental and behavioral, bolstered by financial wellness — which in America right now, means a job bundled with health insurance and affordable care.




 Interviewed live on BNN Bloomberg (Canada) on the market for GLP-1 drugs for weight loss and their impact on both the health care system and consumer goods and services -- notably, food, nutrition, retail health, gyms, and other sectors.
Interviewed live on BNN Bloomberg (Canada) on the market for GLP-1 drugs for weight loss and their impact on both the health care system and consumer goods and services -- notably, food, nutrition, retail health, gyms, and other sectors. Thank you, Feedspot, for
Thank you, Feedspot, for  As you may know, I have been splitting work- and living-time between the U.S. and the E.U., most recently living in and working from Brussels. In the month of September 2024, I'll be splitting time between London and other parts of the U.K., and Italy where I'll be working with clients on consumer health, self-care and home care focused on food-as-medicine, digital health, business and scenario planning for the future...
As you may know, I have been splitting work- and living-time between the U.S. and the E.U., most recently living in and working from Brussels. In the month of September 2024, I'll be splitting time between London and other parts of the U.K., and Italy where I'll be working with clients on consumer health, self-care and home care focused on food-as-medicine, digital health, business and scenario planning for the future...