More U.S. employers are growing activist roles as stakeholders in the healthcare system, according to the 2019 Large Employers Health Care Strategy and Plan Design Survey from the National Business Group on Health (NBGH).
Consider the Amazon-Berkshire Hathaway-JPMorgan Chase link up between Jeff Bezos, Warren Buffet, and Jamie Dimon, as the symbol of such employer-health activism.
The NBGH report is based on survey results collected from 170 large employers representing 13 million workers and 19 million covered lives (families/dependents). This annual survey is one of the most influential such reports released each year, providing a current snapshot of large employers’ views on healthcare, costs, and strategic options that will enable companies to continue providing health insurance to workers. The study was fielded in May-June 2018 and represents actions that employers will take in 2019 for health benefits, Brian Marcotte, President and CEO of NBGH, explained this morning during a press conference launching the report.
For 2019, employers look to their overall healthcare strategy, first, to bolster a productive, competitive, engaged workforce, and then second, to manage costs.
But managing to the Triple Aim — that is, enhancing healthcare experience, driving outcomes, and lowering per capita costs — is still a goal of employers, which underpins their activism. One-third of large employers will adopt new delivery and payment models like accountable care organizations and high-performing networks in 2019. More employers will also channel employees and dependents to Centers of Excellence for focused clinical areas like cancer treatment, cardiovascular care. orthopedic/musculoskeletal, and fertility.

Behavioral health is gaining traction among large employers, growing anti-stigma campaigns and manager training focusing on mental health conditions and treatments.
One of the most concerning rising cost components in medical trend come from the pharmaceutical supply chain. Large employers identified the key drivers of cost trend: high-cost claims and conditions, and specialty pharmacy costs. The second chart summarizes large employers’ views on prescription drug costs, as employers are looking for greater transparency and a new business model that simplifies and streamlines the chain to lower costs. The vast majority of employers do not believe the current rebate-based system works to reduce pharmaceutical costs, and most welcoming an alternative to rebates. Specifically, over half of employers don’t see that rebates benefit patients at the point-of-sale. As a result, 30% of employers will implement co-pay accumulator programs in 2019, and Marcotte expects this to accelerate to as much as 50% within a few years.
Health Populi’s Hot Points: One part of the NBGH survey asked employers about the impact of mergers and consolidation in the industry, along with so-called “new entrants” — such as technology companies, retailers, and organizations that typically haven’t served the legacy healthcare system. Here, consider Lyft and Uber, grocery stores, and of course, the multiple health/care strategies of Amazon, Apple, and Google.
70% of employers said these new market entrants will be necessary to disrupt the market in a positive way.
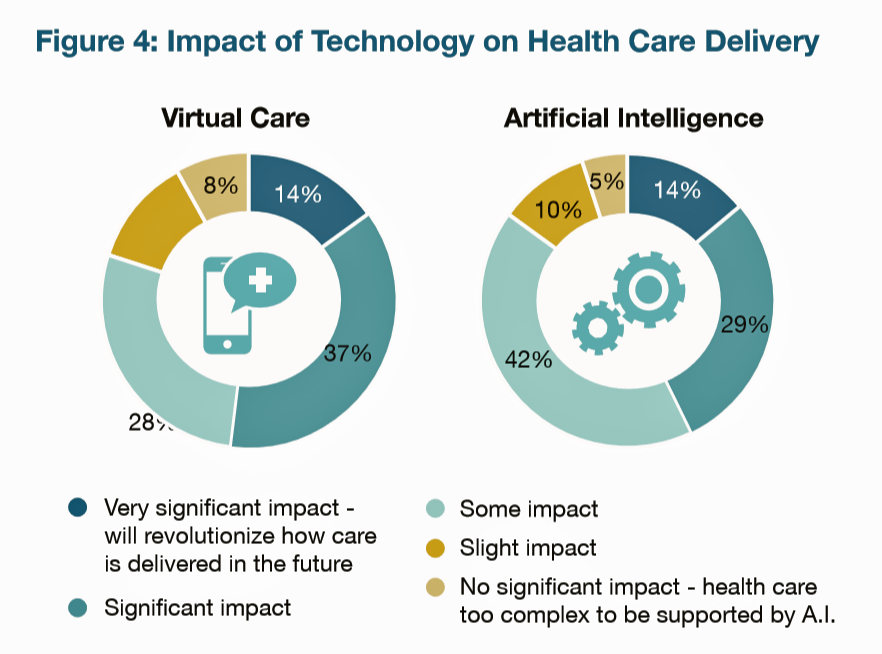
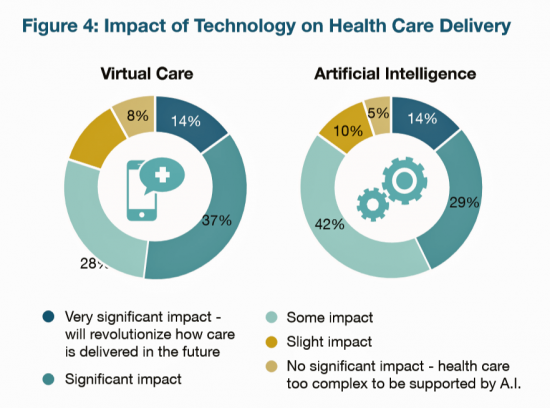
This vision is supported by large employers’ viewing positive impacts of virtual care and artificial intelligence (AI) in healthcare delivery, shown in the first chart. 65% of employers see that virtual care — telehealth, telemedicine, remote monitoring, and cognitive behavioral therapy, for example — will have a significant impact on healthcare delivery. 71% of employers see AI having a significant impact on healthcare.
These findings show a more empowered, engaged employer in America. My hypothesis is that, as I continue to evangelize about the “Amazon Prime-ing” of the health care consumer, employers are also these people, looking to the tech-based platforms and solutions and apps that enable all of us to streamline our lives for travel, for grocery shopping, for way-finding, and for financial transactions. Why not for healthcare, channeled through our workplaces?
One other finding in the survey stood out: that some employers are “dialing back” full replacement of consumer-directed health plans (CDHPs). For the first time in four years, employers have begun to offer at least one other option of a plan beyond a CDHP (high-deductible plan, coupled with a health savings account). This may be “bringing choice back in,” Marcotte observed, in companies’ battle for talent acquisition.
Employers may also be recognizing the fact that the consumer-employee is also the payor, and as such, customer experience through both virtual and convenient care options, and transparency that empowers a worker to make rational choices based on their own value and values, will help transform both health plan design and an engaged workforce. “Our health system was not was not designed with the consumer in mind,” Marcotte observed. The 2019 NBGH survey shows that large employers are becoming more design-thinking when it comes to health benefits, a welcome phenomenon.




 Interviewed live on BNN Bloomberg (Canada) on the market for GLP-1 drugs for weight loss and their impact on both the health care system and consumer goods and services -- notably, food, nutrition, retail health, gyms, and other sectors.
Interviewed live on BNN Bloomberg (Canada) on the market for GLP-1 drugs for weight loss and their impact on both the health care system and consumer goods and services -- notably, food, nutrition, retail health, gyms, and other sectors. Thank you, Feedspot, for
Thank you, Feedspot, for  As you may know, I have been splitting work- and living-time between the U.S. and the E.U., most recently living in and working from Brussels. In the month of September 2024, I'll be splitting time between London and other parts of the U.K., and Italy where I'll be working with clients on consumer health, self-care and home care focused on food-as-medicine, digital health, business and scenario planning for the future...
As you may know, I have been splitting work- and living-time between the U.S. and the E.U., most recently living in and working from Brussels. In the month of September 2024, I'll be splitting time between London and other parts of the U.K., and Italy where I'll be working with clients on consumer health, self-care and home care focused on food-as-medicine, digital health, business and scenario planning for the future...