 What will employers do with their health insurance sponsorship once health reform kicks into full-implementation in 2014? Will they drop coverage? There’s been some speculation that more employers would exit covering employees, but researchers at RAND see quite the opposite scenario.
What will employers do with their health insurance sponsorship once health reform kicks into full-implementation in 2014? Will they drop coverage? There’s been some speculation that more employers would exit covering employees, but researchers at RAND see quite the opposite scenario.
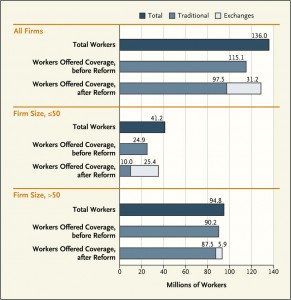
An additional 13.6 million workers will be offered health insurance coverage in a post-ACA America, based on a forecasting model the RAND team constructed. This increases the percentage of employers offering workers health insurance from 84.6% of workers to 94.6% of workers post-reform.
The increase is driven, the model predicts, by two key factors:
- More demand for coverage by workers due to the individual mandate penalties if they don’t buy into health coverage
- The availability of new, lower-cost insurance plans accessible to small business.
The reform impacts small business disproportionately, in a good way, versus large businesses who already tend to offer health insurance benefits to employees. Of the new 13.6 million workers being offered insurance, only 3.2 million are forecasted to be working in large companies.
RAND’s model includes variables for the individual mandate, penalties for firms with over 50 employees that don’t offer coverage, Medicaid expansion to include people with incomes up to 133% of the Federal Poverty Level, and the creation of state health insurance exchanges open to individuals and business with 100 or fewer employees.
Health Populi’s Hot Points: One of President Obama’s founding pillars for health reform in the U.S. was to build on the nation’s existing employer-sponsored health insurance system. That foundation, though, was known to have faults — most fundamentally, the fact that small employers couldn’t compete with larger companies for health insurance for employees. That’s why the ACA focused on this weaknesses in the system. RAND’s model takes this into account and yields a result that is largely intended by the legislation.
The researchers believe that employer-sponsored insurance will continue to be intact, and even strengthened, post-ACA. But they note that large employers could change the nature of how they cover health insurance: more employers may switch to provide insurance coverage through the new insurance exchanges, which could enable them to reduce their administrative costs, manage insurance risk by adding to a wider pool of insured workers, and expanding the number of health plan choices available to employees.
This last point is an important one: most employers who offer health insurance have reduced the number of plans they offer workers to manage administrative expense and hassle. But workers-cum-consumers want some semblance of choice: younger, single workers may prefer a high-deductible plan with lower costs, while middle-aged workers with adult children could demand a more comprehensive plan with more clinical bells-and-whistles and more open physician networks.
Thanks to the New England Journal of Medicine for publishing this important study; NEJM has gone beyond serving the clinical health community is becoming an increasingly important go-to source for insights into health reform.




 I'm in amazing company here with other #digitalhealth innovators, thinkers and doers. Thank you to Cristian Cortez Fernandez and Zallud for this recognition; I'm grateful.
I'm in amazing company here with other #digitalhealth innovators, thinkers and doers. Thank you to Cristian Cortez Fernandez and Zallud for this recognition; I'm grateful. Jane was named as a member of the AHIP 2024 Advisory Board, joining some valued colleagues to prepare for the challenges and opportunities facing health plans, systems, and other industry stakeholders.
Jane was named as a member of the AHIP 2024 Advisory Board, joining some valued colleagues to prepare for the challenges and opportunities facing health plans, systems, and other industry stakeholders.  Join Jane at AHIP's annual meeting in Las Vegas: I'll be speaking, moderating a panel, and providing thought leadership on health consumers and bolstering equity, empowerment, and self-care.
Join Jane at AHIP's annual meeting in Las Vegas: I'll be speaking, moderating a panel, and providing thought leadership on health consumers and bolstering equity, empowerment, and self-care.