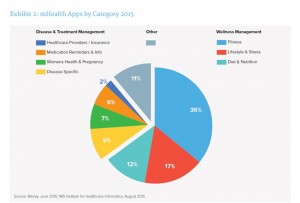
 Of the over 165,000 mobile health (mHealth) apps available in the Apple iTunes and Google Play (Android) stores, 36 are responsible for one-half of all downloads, based on IMS Institute‘s latest research into Patient Adoption of mHealth: Use, Evidence and Remaining Barriers to Mainstream Adoption published today.
Of the over 165,000 mobile health (mHealth) apps available in the Apple iTunes and Google Play (Android) stores, 36 are responsible for one-half of all downloads, based on IMS Institute‘s latest research into Patient Adoption of mHealth: Use, Evidence and Remaining Barriers to Mainstream Adoption published today.
This report updates IMS Institute’s 2013 report on mHealth, covered here in Health Populi.
For the 2015 research, IMS Institute looked at the state of mHealth apps, number and type, uptake and usage, evidence of the impact apps have on patient care, and consideration of barriers and progress made for apps becoming a more mainstream part of health care delivery.
Of the 165,000 apps in the market, IMS Institute studied over 26,000 in detail. The research learned that:
- 1 in 10 apps have some type of capability to connect to a device or sensor, opening up the ability to gather biofeedback and physiological function from patients which enhances both accuracy and convenience of data collection
- Over the past two years, the percent of mHealth apps with connectivity to social networks grew from 26% to 34% of all apps – underscoring the importance of social networks in consumer health engagement
- Less progress has been made in enabling apps to connect and communicate securely with healthcare provider systems and electronic health records
- Since 2013, clinical evidence is growing for some mobile health apps: several hundred studies have been published in peer-reviewed publications or posters, especially around the utilization of mHealth apps. While evidence is short of what’s required for universal acceptance of when app can bring meaningful impact to patient care, improving outcomes and lowering costs, direction is positive and body of evidence continues to grow, Murray Aitken, Executive Director at the IMS Institute for Healthcare Informatics, told a conference call prior to the report’s publication. We can expect the evidence base to grow over the next couple of years: there are about 300 clinical trials on ClinicalTrials.gov website which relate to mHealth.
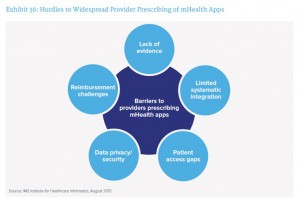 IMS Institute conducted in-depth interviews with executives in health care system organizations to assess the state of mHealth apps among providers. Overall, health care leaders see potential for mHealth to improve the wellness of their members or patients. However, there remain several barriers which persist from IMS Institute’s 2013 study, shown in the second diagram. Topping the list of obstacles to adoption is the lack of integration with electronic health records and clinical decision making IT systems. This continues to be a barrier as providers are, as Aitken put it, “preoccupied with MU and ICD-10 implementation.” Efforts to enable the integration of mobile and patient-generated health care data continues to be pushed back and thus represents a major barrier. That being said, there is concordance that the shift from volume-based payment to value would incentivize providers to adopt mobile health technology as part of health care delivery and changing workflows.
IMS Institute conducted in-depth interviews with executives in health care system organizations to assess the state of mHealth apps among providers. Overall, health care leaders see potential for mHealth to improve the wellness of their members or patients. However, there remain several barriers which persist from IMS Institute’s 2013 study, shown in the second diagram. Topping the list of obstacles to adoption is the lack of integration with electronic health records and clinical decision making IT systems. This continues to be a barrier as providers are, as Aitken put it, “preoccupied with MU and ICD-10 implementation.” Efforts to enable the integration of mobile and patient-generated health care data continues to be pushed back and thus represents a major barrier. That being said, there is concordance that the shift from volume-based payment to value would incentivize providers to adopt mobile health technology as part of health care delivery and changing workflows.
While progress is also being made in the areas of privacy and security, they still remain barriers to mainstream adoption and “prescription” of mHealth apps among providers.
Finally, the inability to reach the most vulnerable cohorts of patients — especially the elderly and non-English speaking people — remains a challenge for many health systems looking to adopt relevant and person-centered designed apps.
Health Populi’s Hot Points: Bringing health care providers into the discussion of mobile health apps is essential for mHealth app developers and those advocating their use in health care delivery. Consumers more like sustain use of a mobile health app when prescribed or recommended by a health care professional.
Furthermore, most apps are single-use functions, which can be a fragmented approach that threatens continuity-of-care as well as interoperability with other legacy health IT systems.
The Big Challenge facing patients and consumers is the overwhelming volume of mobile health apps available online. Without a level of guidance, the choice can be intimidating and un-helpful. The number of Apple IoS health apps more than doubled in 2 years since 2013.
This volume-challenge leads to two consumer behaviors: people who download the most popular apps (e.g., IMS Institute found that 90% of downloads are among 12% of healthcare apps — a heavy skewing toward relatively few apps). Second, some people download lots of apps and try them out once or twice: 40% of apps have fewer than 5,000 downloads.
From a physician’s perspective, there are emerging platforms in the market to help clinicians make informed recommendations to patients based on peer physicians’ experiences as well as some sites that certify mHealth apps. Data coming through the IMS AppScript platform show that when physicians recommend apps to a patient, the use of the app after 30 days is significantly higher than when patients download apps they select themselves — resulting in a 10% higher average utilization rate of apps after 30 days when an app recommended by physician. For fitness apps, the consumer-retention rate is as much as 30% higher level of sustained use.
Barbara Spurner of the Mayo Clinic offers her organization’s vision for where mHealth apps can take the institution: “We’ve completed many proof of concepts and pilots and now we are building out a mobile health framework and infrastructure. It’s part of our new Center for Connected Care. Rather than have all of these one-offs in the organization, we are working to integrate our offerings and leverage the power of a platform.”




 Thank you
Thank you  I'm grateful to be part of the Duke Corporate Education faculty, sharing perspectives on the future of health care with health and life science companies. Once again, I'll be brainstorming the future of health care with a cohort of executives working in a global pharmaceutical company.
I'm grateful to be part of the Duke Corporate Education faculty, sharing perspectives on the future of health care with health and life science companies. Once again, I'll be brainstorming the future of health care with a cohort of executives working in a global pharmaceutical company. Jane joined host Dr. Geeta "Dr. G" Nayyar and colleagues to brainstorm the value of vaccines for public and individual health in this challenging environment for health literacy, health politics, and health citizen grievance.
Jane joined host Dr. Geeta "Dr. G" Nayyar and colleagues to brainstorm the value of vaccines for public and individual health in this challenging environment for health literacy, health politics, and health citizen grievance.