In the first six months of the COVID-19 pandemic, telehealth was a “bright spot in the ‘new normal,’” according to a report from J.D. Power, Telehealth Patient Satisfaction Surges During Pandemic but Barriers to Access Persist.
But as the report’s title asserts, most telehealth users experienced obstacles to accessing and using virtual care platforms that drove less positive consumer experiences.
 Overall, the telehealth segment achieved a higher consumer satisfaction score (860 points out of 1,000) than other sectors J.D. Power has studied including health insurance, insurance and financial services.
Overall, the telehealth segment achieved a higher consumer satisfaction score (860 points out of 1,000) than other sectors J.D. Power has studied including health insurance, insurance and financial services.
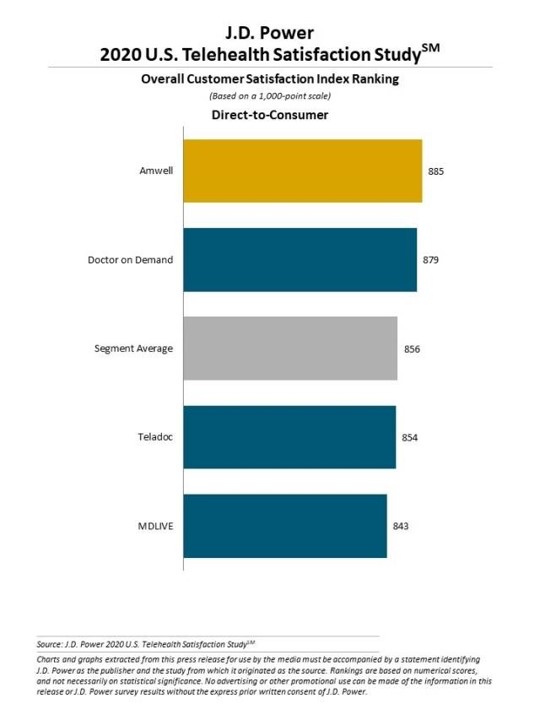
J.D. Power assessed two categories of telehealth vendors: direct-to-consumer (DTC) and payer-provided. Amwell (aka American Well before the company’s re-branding) emerged first in the DTC league, with an overall segment average of 856 points out of 1,000.
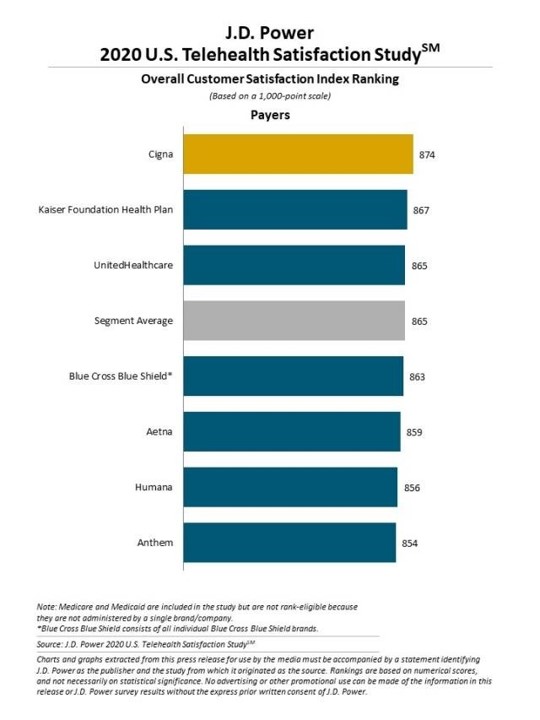
Cigna ranked highest among telehealth payer-providers, with payers scoring 865 points in 1,000—higher overall than for DTC players.
Across all providers, AmWell scored highest at 885, followed by Doctor on Demand with 879 points. Cigna, the highest-scoring payer-backed telehealth organization, racked up 874 points on the 1,000-point scale.
In the study, J.D. Power found that:
- Barriers to access persist, including limited services, confusing technology requirements, and lack of transparency for costs.
- One-third of telehealth users had a problem during a visit, in particular with tech audio issues.
- At-risk patients report lower levels of satisfaction at a level of 117 points lower for a poor experience. These folks felt less personalized visits and were less likely to understand information provided during the visit.
- Safety was the key driver for utilization at a rate of 46% of people using telehealth in 2020, and only 13% in 2019.
This is the second year that J.D. Power has measured telehealth satisfaction, based on four considerations: customer service, consultation, enrollment, and billing and payment. The study was fielded in June-July 2020 among 4,302 U.S. adults who had done a telehealth visit in the past year.
 Health Populi’s Hot Points: Since the pandemic emerged in the U.S. in February 2020, telehealth has received substantial funding for growing existing companies, as well as new innovations popping up in the growing virtual care landscape. For example, AmWell began collaborating with the Google cloud business, where the company invested $100 million to scale the alliance. Amwell also began allying with TytoCare this week, to enable home-based physical exams using med-tech designed for patients’ at-home use.
Health Populi’s Hot Points: Since the pandemic emerged in the U.S. in February 2020, telehealth has received substantial funding for growing existing companies, as well as new innovations popping up in the growing virtual care landscape. For example, AmWell began collaborating with the Google cloud business, where the company invested $100 million to scale the alliance. Amwell also began allying with TytoCare this week, to enable home-based physical exams using med-tech designed for patients’ at-home use.
WebMD announced a new service enabling consumers to schedule telehealth visits from the WebMD Care and Vitals platforms. This is building on WebMD’s strategy to grow beyond being an information provider to channeling services on a delivery platform.
And, GoodRx became a public company, launching its initial public offering on September 23, which will expand its role beyond e-prescribing morphing toward being a telehealth company.
As $billions are poured into the virtual care landscape, it will be important to pay attention to how consumer satisfaction with telehealth could down-shift when/if their health plans reduce coverage of virtual visits in terms of providing reimbursement to clinicians and reducing co-payments to patients.
This turning point for telemedicine has reached mass media mainstream status, covered this past weekend in The New York Times in a headlined articled, “Some insurers end pandemic waivers of fees and deductibles for telehealth.”
We are beginning to feel the tension between the bullish telehealth experience and what some may see as irrationally exuberant investment in the first months of the pandemic. Right now, we are moving into the next normal, a phase of crafting business models to enable telehealth to simply blur into “healthcare” workflows.
Nothing eases us like learning from smart people in market-chaotic times like this, and we have that salvo in an editorial in the journal Telehealth and Medicine Today by Lyle Berkowitz, Steve Ommen, and John Halamka – three physicians on the front lines of digital health innovation.
They discuss the lessons learned from telehealth in the pandemic and what we can expect to emerge in the coming year. Their helpful bottom line conclusion is that a combination of autonomous care and telehealth visits can ensure we can bolster access to quality, efficient and cost-effective care. This is what I’ve been calling omni-channel health care, which in my consumer research during the pandemic is what people, younger and older, expect to be offered as part of their overall health care portfolio of services once the pandemic fades.




 Thank you
Thank you  I'm grateful to be part of the Duke Corporate Education faculty, sharing perspectives on the future of health care with health and life science companies. Once again, I'll be brainstorming the future of health care with a cohort of executives working in a global pharmaceutical company.
I'm grateful to be part of the Duke Corporate Education faculty, sharing perspectives on the future of health care with health and life science companies. Once again, I'll be brainstorming the future of health care with a cohort of executives working in a global pharmaceutical company. Jane joined host Dr. Geeta "Dr. G" Nayyar and colleagues to brainstorm the value of vaccines for public and individual health in this challenging environment for health literacy, health politics, and health citizen grievance.
Jane joined host Dr. Geeta "Dr. G" Nayyar and colleagues to brainstorm the value of vaccines for public and individual health in this challenging environment for health literacy, health politics, and health citizen grievance.