In May 2020, the Oxford English Dictionary (OED) re-visited the acronym, “PPE.”
 As OED evolves the definition of PPE, the wordsmiths could borrow from OSHA’s website, noting that PPE,
As OED evolves the definition of PPE, the wordsmiths could borrow from OSHA’s website, noting that PPE,
“is equipment worn to minimize exposure to hazards that cause serious workplace injuries and illnesses. These injuries and illnesses may result from contact with chemical, radiological, physical, electrical, mechanical, or other workplace hazards. Personal protective equipment may include items such as gloves, safety glasses and shoes, earplugs or muffs, hard hats, respirators, or coveralls, vests and full body suits.”
Perhaps Definition 3 in the OED could be updated by a blog published online in the September 25, 2020, issue of Health Affairs, A New “PPE” For A Thriving Community: Public Health, Primary Care, Health Equity.
This essay bakes in several voices from across the health/care ecosystem, representing the Robert Graham Center for Primary Care, IBM Watson Health, and the Colorado School of Public Health. Together, they make a compelling argument for re-imagining PPE beyond the physical armament of gloves, gowns, and other protective physical gear with which frontline healthcare staff and other essential workers in the pandemic suited up.
Why redefine, really re-imagine, PPE?
Globally. in the first near-year of the pandemic, we’ve learned a lot about the science and clinical aspects of the very tricky COVID-19 virus.
In the U.S., we’ve learned a lot about the weaknesses in American health care: peoples’ lack of access to health care, a weak and patchwork quilted primary care infrastructure, fragmented and siloed health data, and a body politic often dis- or mis-engaged in evidence-based medical facts.
Given what we-know-we-know now, what’s really protective at the root of the coronavirus public health crisis are prevention and resilience-bolstering factors like building and nurturing a strong primary care backbone, re-constructing a public health infrastructure and ethos, and addressing health equity.
In the U.S., the risks of COVID-19 exposure, illness severity, and community impact have not been evenly distributed, the authors recognize: the ongoing prevalence of mental health conditions won’t be evenly distributed, either, they project, exacerbating pre-existing disparities of health care. [For more on this issue, see Health Populi here].
Primary care in the U.S. has largely focused on individuals, and not so much community and population-level health and well-being. In re-thinking the two “Ps” of PPE in America, enabling public health to collaborate with primary care would bolster health at the individual, family, community, and national levels.
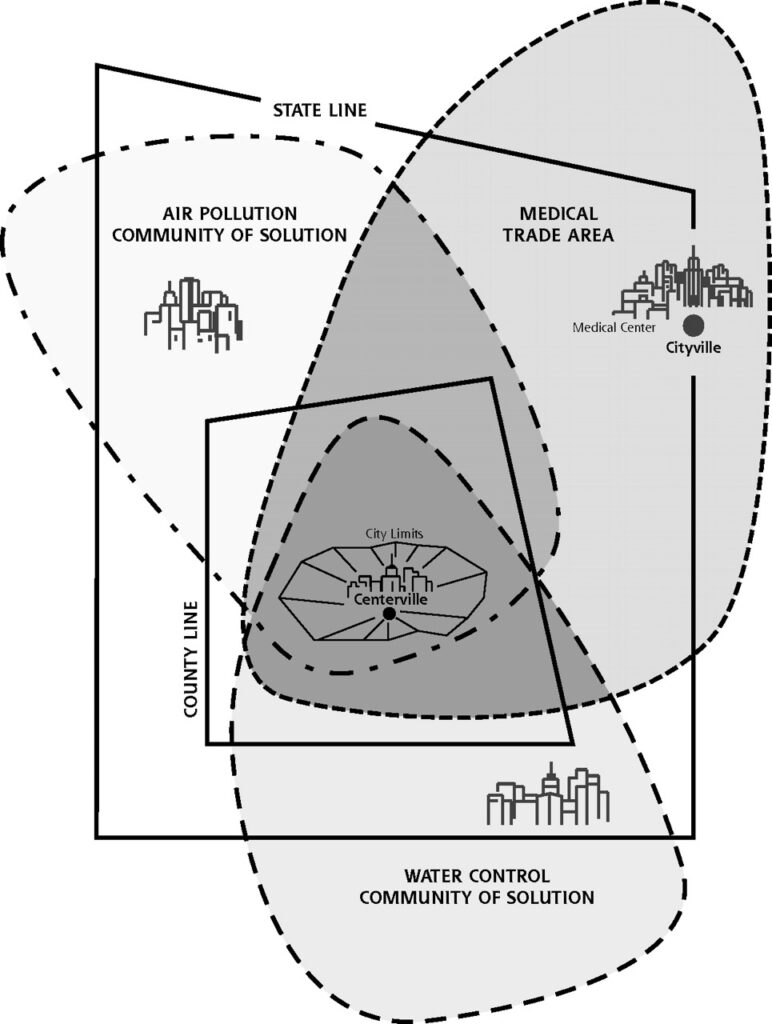 The vision is to build “local communities of solution,” as the authors coin, linking public health and primary care with community organizations that bolster social determinants of health: education, jobs and skill building, food security, environmental health, financial wellness, and other factors that are unique to neighborhoods and “ZIP codes” — more health-determining than genetic codes. The framework for the new PPE takes a page out of the report, Health is a Community Affair — written in in 1966 by the National Commission on Community Health Services.
The vision is to build “local communities of solution,” as the authors coin, linking public health and primary care with community organizations that bolster social determinants of health: education, jobs and skill building, food security, environmental health, financial wellness, and other factors that are unique to neighborhoods and “ZIP codes” — more health-determining than genetic codes. The framework for the new PPE takes a page out of the report, Health is a Community Affair — written in in 1966 by the National Commission on Community Health Services.
This was a playbook focused on re-building health at the local level based on the unique social determinants that diminished well-being in a community. This graphic comes out of the report: this illustrates a “Community of Solution” which recognizes that different factors that impact peoples’ health come out of three perspectives: territory or space, group membership, or a set of social structures and organization.
“Communities are organically derived, highly variable, and matched to a particular need or needs,” research in the Annals of Family Medicine revisiting the original NCCHS asserted.
To get to those particular needs in a region, the authors of the Health Affairs PPE essay are developing a Community PPE Index based on the three “PPE” components – primary care, public health, and health equity, giving each area equal weight in the index. The authors recognize there are other issues that could be considered in the index, but in the case of the coronavirus pandemic, research demonstrated to them that these three factors were most impactful.
The three metrics the Index will use to quantify the “new PPE,”
- Primary care workforce goals of one primary care provider per 1,500 population;
- The National Health Security Preparedness Index (NHSPI), identifying public health resources especially targeted to disasters, national security, and pandemics; and,
- The Social Deprivation Index (SDI, a county-wide measure of SDoH that predicts health outcomes beyond poverty data.
 Ultimately, the Community PPE Index could be considered, “the COVID-19 Response and Recovery Index,” the authors believe. To crush the coronavirus in the U.S., we’ll need more than physical barriers, they conclude.
Ultimately, the Community PPE Index could be considered, “the COVID-19 Response and Recovery Index,” the authors believe. To crush the coronavirus in the U.S., we’ll need more than physical barriers, they conclude.
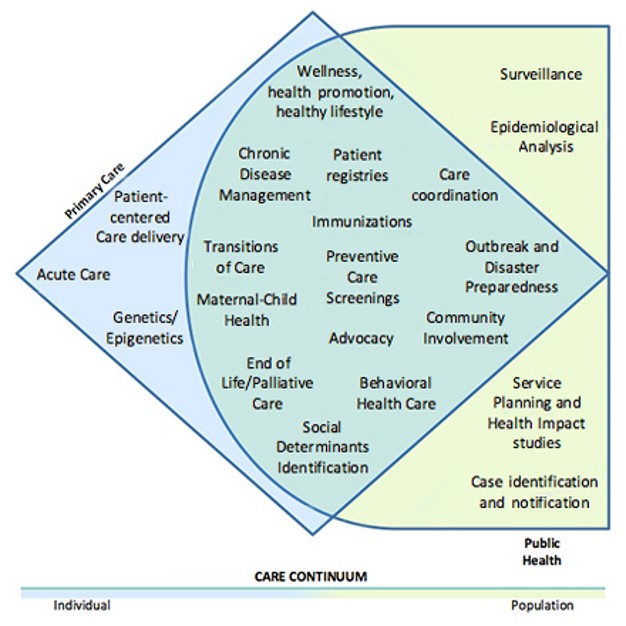
Health Populi’s Hot Points: This third graphic comes from the American Academy of Family Physicians (AAFP), which recently published a position paper on integrated primary care and public health.
This illustration gives us great detail on what that integration across siloes could look like. Making this mental model actionable would move social determinants into the continuum of care from the front-end “on-ramp” of primary care, into community organizations that address factors from food security to mental health and community engagement, through to surveillance and epidemiological analysis — the analytics that support “crushing” the pandemic.
The x-axis simply explains the “why” the U.S. hasn’t crushed the virus compared with other countries that have done a better job containing the spread of COVID-19: the care continuum is indeed a “continuum” connecting the individual to the population.
In the U.S., we haven’t come to terms with embracing our Health Citizenship — that is, our rights and responsibilities for claiming our health and health care in America. In my latest book, Health Citizenship: How a virus opened up hearts and minds, I lay out the four pillars of health care access, data citizenship, trust, and a new social contract for health in America.
That social contract is love: in the case of COVID-19, to stop the spread, love means that I wear the mask for you, and you do so for me.
Kudos to the authors: John Westfall, Stephen Patterson, Irene Dankwa-Mullan, William Kassler, Amol Rajmane, Glen Mays–and my friend, Dr. Kyu Rhee. The redefinition of “New PPE” may well be one very useful prescription to help save us in the American pandemic, and beyond — to build a more equitable and effective health care system.





 Thank you
Thank you  I'm grateful to be part of the Duke Corporate Education faculty, sharing perspectives on the future of health care with health and life science companies. Once again, I'll be brainstorming the future of health care with a cohort of executives working in a global pharmaceutical company.
I'm grateful to be part of the Duke Corporate Education faculty, sharing perspectives on the future of health care with health and life science companies. Once again, I'll be brainstorming the future of health care with a cohort of executives working in a global pharmaceutical company. Jane joined host Dr. Geeta "Dr. G" Nayyar and colleagues to brainstorm the value of vaccines for public and individual health in this challenging environment for health literacy, health politics, and health citizen grievance.
Jane joined host Dr. Geeta "Dr. G" Nayyar and colleagues to brainstorm the value of vaccines for public and individual health in this challenging environment for health literacy, health politics, and health citizen grievance.