Ten years ago, ECRI named the top 10 health technology hazards for 2013: they were alarm hazards, medication administrative errors using infusion pumps, unnecessary exposure and radiation burns from diagnostic radiology procedures, patient/data mismatches in EHRs and other HIT systems, interoperability failures with medical devices and health IT systems, and five other tech-related hazards.
In 2014, ECRI pivoted the title of this annual report to “patient safety concerns,” a nuance away from health technology.
Fast forward to 2023 and ECRI’s latest take on the Top 10 Patient Safety Concerns 2023. While technology is embedded in this list, the headlines have more to do with social, mental, and behavioral health than pure-play technology and devices.

Topping the 2023 list of patient safety concerns is the pediatric mental health crisis. This, in ECRI’s words, “recognizes that children and youth are facing a true crisis. The proportion of youth experiencing mental health challenges is high and growing yet resources and access are limited. The healthcare sector must act now to protect our youngest and most vulnerable population,” ECRI asserts from the start of the report.
For each concern, ECRI provides a data snapshot and explanation of the challenge providing context and evidence on the issue. Following the statement, ECRI provides Acton Recommendations that hospitals and providers can consider to address the challenge.
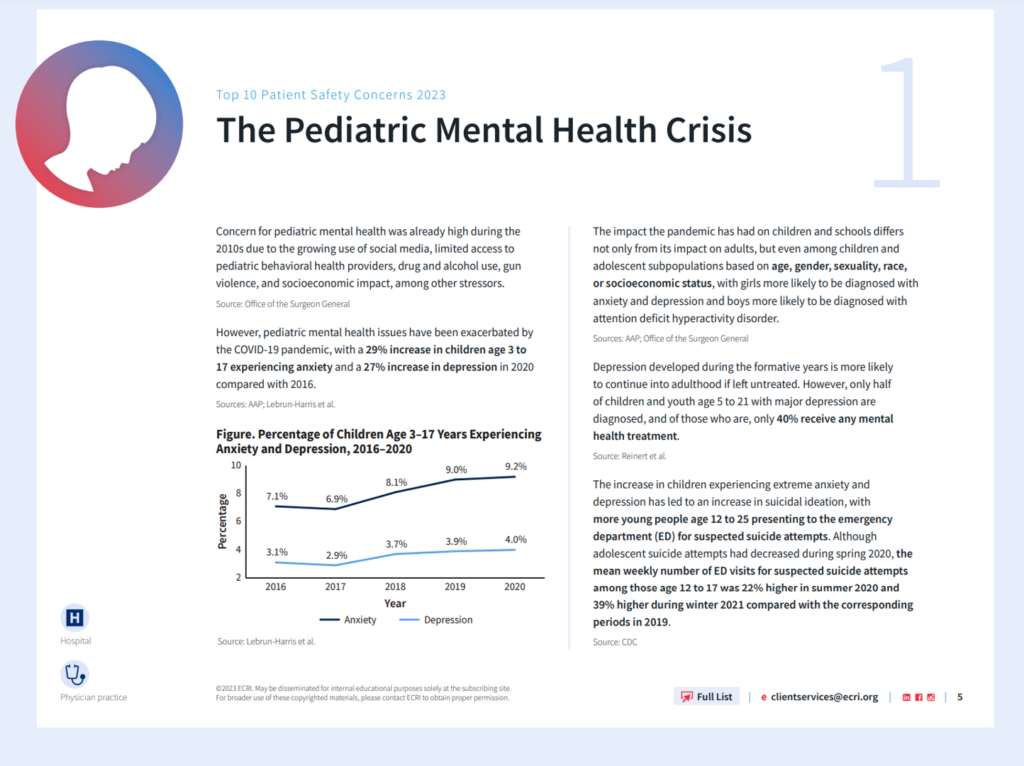
Here is ECRI’s top issue statement for the pediatric mental health crisis. The key safety implications here are lack of access to pediatric behavioral health providers, drug and alcohol use, gun violence, and other stressors. The risk to suicide among young people has been especially acute, with ECRI citing CDC data finding that more young people in the U.S. ages 12 to 17 presented to the emergency department for suspected suicide attempts in the winter of 2021 — 39% greater than in the same period in 2019.
In its recommendations for action, ECRI notes that health care providers cannot solve this crisis themselves, but can take specific actions to address the pediatric mental health crisis. These actions include leadership support and resources to shift the organization’s culture toward behavioral health needs, patient and family engagement tactics, and warm handoffs to pediatric mental health services in the community, among many other constructive recommendations.

I’ll explore one more challenge on this sobering list of safety concerns, which is #3 on the list: uncertainty surrounding maternal-fetal medicine.
I support ECRI’s call-out of this challenge as a patient as well as provider safety issue, given the politicization of women’s health care access which has emerged a national as well as State-level crisis for women and the people who love us.
Here is ECRI’s discussion of clinician needs in times of uncertainty surrounding maternal-fetal medicine.
The issue statement begins with ECRI’s noting, “On June 24, 2022, the Supreme Court held that the Constitution does not provide a right to an abortion, overruling Roe v. Wade. In doing so, the Court returned the full power to regulate abortion to the states,” sourcing the Dobbs decision.
The problem statement includes a table on restrictiveness of State abortion laws for some data points and context for the safety challenge.
The safety issues include resource and capacity constraints leading to all-time highs of provider burnout, especially in the wake of the pandemic. In addition, patients have seen delays in getting treatment for other conditions unrelated to reproductive services. Of course, cross-border care has complicated women’s health based on the states in which they live, compromising health and potentially life (see this piece in the New York Times providing details on five Texas women suing the state, each dealing with difficult pregnancies and situations).
Specific actions ECRI recommends for stakeholders to address the uncertainties for maternal-fetal medicine including engaging in two-way communications with frontline staff to share concerns and develop guidance for caring for patients (aka “tiered safety huddles”), to create patient education materials for staff to share with patients and families on a state-by-state basis, offer emotional and mental health support for clinicians experiencing high levels of moral distress and burnout, among others.
ECRI builds this report of the Top 10 patient safety issues leveraging its long-time expertise in this field: their staff are expert across the health care landscape including people in medicine, nursing, pharmacy, risk management, and of course patient safety and quality. The team reviews the scientific literature, assesses event reports, root cause analyses, research requests they’ve received int he past year, accident investigations and a plethora of other data souuces. The Top 10 risks are based on severity, frequency, breadth, insidiousness (meaning is the problem difficult to recognize or challenging to rectify), and profile — does this safety issue place significant pressure on the organization.

Health Populi’s Hot Points: Each year, ECRI informs us on their view of the Top 10 patient safety challenges. Year after year, some challenges persist, and these are shown in the last chart here from the 2023 report.
Among the dozen+ safety issues are medication safety, health IT, workforce staffing, telehealth and digital health risks, infection prevention and control, and health equity — which ECRI noted as #1 last year in its 2021 review as “racial and ethnic disparities.”
Clearly, patient safety challenges in 2023 go well beyond technology in and of itself. Our cultures of care, caring, and social health have as much to do with patient safety as technology glitches and cleaning and disinfection.





 Interviewed live on BNN Bloomberg (Canada) on the market for GLP-1 drugs for weight loss and their impact on both the health care system and consumer goods and services -- notably, food, nutrition, retail health, gyms, and other sectors.
Interviewed live on BNN Bloomberg (Canada) on the market for GLP-1 drugs for weight loss and their impact on both the health care system and consumer goods and services -- notably, food, nutrition, retail health, gyms, and other sectors. Thank you, Feedspot, for
Thank you, Feedspot, for  As you may know, I have been splitting work- and living-time between the U.S. and the E.U., most recently living in and working from Brussels. In the month of September 2024, I'll be splitting time between London and other parts of the U.K., and Italy where I'll be working with clients on consumer health, self-care and home care focused on food-as-medicine, digital health, business and scenario planning for the future...
As you may know, I have been splitting work- and living-time between the U.S. and the E.U., most recently living in and working from Brussels. In the month of September 2024, I'll be splitting time between London and other parts of the U.K., and Italy where I'll be working with clients on consumer health, self-care and home care focused on food-as-medicine, digital health, business and scenario planning for the future...