How to Get Better Care to More People? Address Burnout, Bridge Insights with AI, Embed Sustainability – the Philips Future Health Index 2024

Health care access is a challenge in rural and urban areas, cities and suburbs, and across more demographic groups than you might realize, as we see wait times grow for appointments, primary care shortages, and delays in screening plaguing health systems around the world. In the Future Health Index 2024, Philips’ latest annual report presents a profile of the state of health care focused on how to provide better care for more people. For the report, Philips surveyed a total of 2,800 healthcare leaders consisting of 200 respondents in 14 countries: Australia, Brazil, China,
Is There an Easy-Button for AI In Healthcare Team Well-Being? Exploring a New PC with Embedded AI

“The greatest opportunity offered by AI is not reducing errors or workloads, or even curing cancer: it is the opportunity to restore the precious and time-honored connection and trust,” Dr. Eric Topol wrote in his 2019 book, Deep Medicine: How Artificial Intelligence Can Make Healthcare Human Again. In the five years since Dr. Topol looked for AI to bolster the human-touch in health care, we’ve lived, worked, and muddled our way through the COVID-19 pandemic and witnessed the growing epidemic of burnout among clinicians, the front-line of medical care. I recalled Dr. Topol’s assertion on AI’s promise for humanizing health
Physicians Feeling Burnout and Depression Continues in 2024 — The Annual View From Medscape
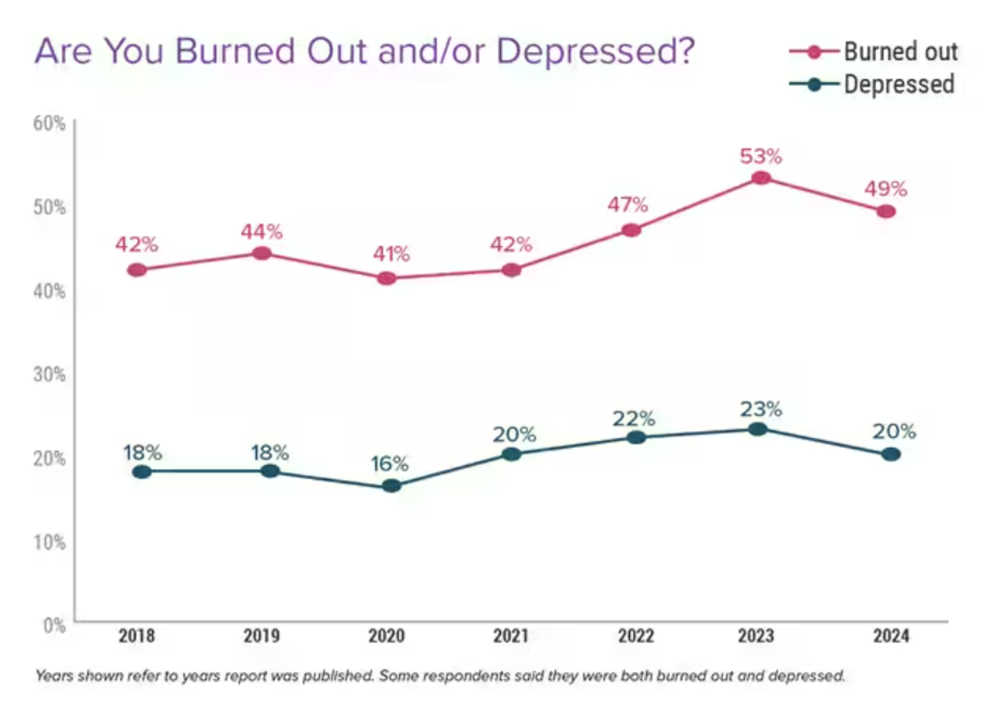
One-half of U.S. physicians report feeling burned out, and 3 in 5 of those doctors say they have felt burned out for over two years, according to the Physician Burnout & Depression Report for 2024 from Medscape. While the study’s press release asserts there may be “progress” given the percent of doctors citing burnout fell by 4 percentage points from 53% of doctors in 2022 to 49% in 2023, it is obvious the U.S. physicians need greater support and less taboo concerning their mental health which impacts both their professional and personal lives.
Ethics for AI in Health – A View From The World Health Organization

For health care, AI can benefit diagnosis and clinical care, address paperwork and bureaucratic duplication and waste, accelerate scientific research, and personalize health care direct-to-patients and -caregivers. On the downside, risks of AI in health care can involve incomplete or false diagnoses, inaccuracies and errors in cleaning up paperwork, exacerbate differential access to scientific knowledge, and exacerbate health disparities, explained in the World Health Organization’s (WHO) report, Ethics and governance of artificial intelligence for health. WHO has released guidance on the use of large multi-modal models (LMMs) in health care which detail 40+ recommendations for
Workforce Shortages and Health Care Cost Pressures Inspire RSNA 2023 (and yes, AI’s in the mix, too)

Radiology and radiologists play starring roles in our health care, with he core work flow of diagnostic imaging supporting prevention, disease detection, diagnosis, delivering and monitoring therapy, linking specialists to other providers in telehealth, and as a medium for teaching clinicians, patients and caregivers. As health care delivery continues to change and adapt to technological innovations, demographic shifts, and economic-social-political forces, so, too, are the roles of radiology and radiologists in motion. Every year when American Thanksgiving weekend comes along, you’ll find folks involved in digital imaging flocking to chilly Chicago to convene at McCormick Place for
Accenture’s Great Expectations for a Decade of Deconstruction – the 2024 Life Trends Forecast

In the company’s 17th annual look into consumers’ “life trends,” Accenture finds that, top-line, “The harmony between people, tech and business is showing tensions, and society is in flux.” And these consumer-facing trends will also shape peoples’ attitudes about their health care, how they access and pay for it, and what kinds of services and support health consumers will expect in this era of “deconstruction.” Taken together, the trends noted in Accenture’s 2024 report on Life Trends finds that one-half of consumers, globally, are changing their life goals, making their jobs and retirement stability more important than
The Clinician of the Future: A Partner for Health, Access, Collaboration, and Tech-Savviness

One-half of clinicians working in the U.S., doctors and nurses alike, are considering leaving their current role in the next two to three years. That 1 in 2 clinicians is significantly greater than the global 37% of physicians and nurses thinking about leaving their roles in the next 3 years, according to the report Clinician of the Future 2023 from Elsevier. Elsevier first conducted research among doctors and nurses for the Clinician of the Future report in 2022, following up this year’s survey research online among 2,607 clinicians working around the world: Elsevier polled
“Your care, your way:” Learning from the Philips Future Health Index 2023

Consider the key drivers of supply and demand in health care, globally, right now: On the medical delivery supply side, the shortage of staff is a limiting factor to continuing to deliver care based on the usual work-flows and payment models. On the demand side, patients are taking on more demanding roles as consumers with high expectations for service, convenience, and safe care delivered closer to home — or at home. This dynamic informs The Future Health Index 2023 report from Philips, launched this week at HIMSS 2023. This is the eighth annual global FHI report, with detailed country-specific analyses to
The Top 10 Patient Safety Concerns for 2023 Are About Social, Mental and Behavioral Health

Ten years ago, ECRI named the top 10 health technology hazards for 2013: they were alarm hazards, medication administrative errors using infusion pumps, unnecessary exposure and radiation burns from diagnostic radiology procedures, patient/data mismatches in EHRs and other HIT systems, interoperability failures with medical devices and health IT systems, and five other tech-related hazards. In 2014, ECRI pivoted the title of this annual report to “patient safety concerns,” a nuance away from health technology. Fast forward to 2023 and ECRI’s latest take on the Top 10 Patient Safety Concerns 2023. While technology is embedded in this list, the headlines have more
Medscape Diagnoses Worsening Burnout and Depression Among U.S. Physicians
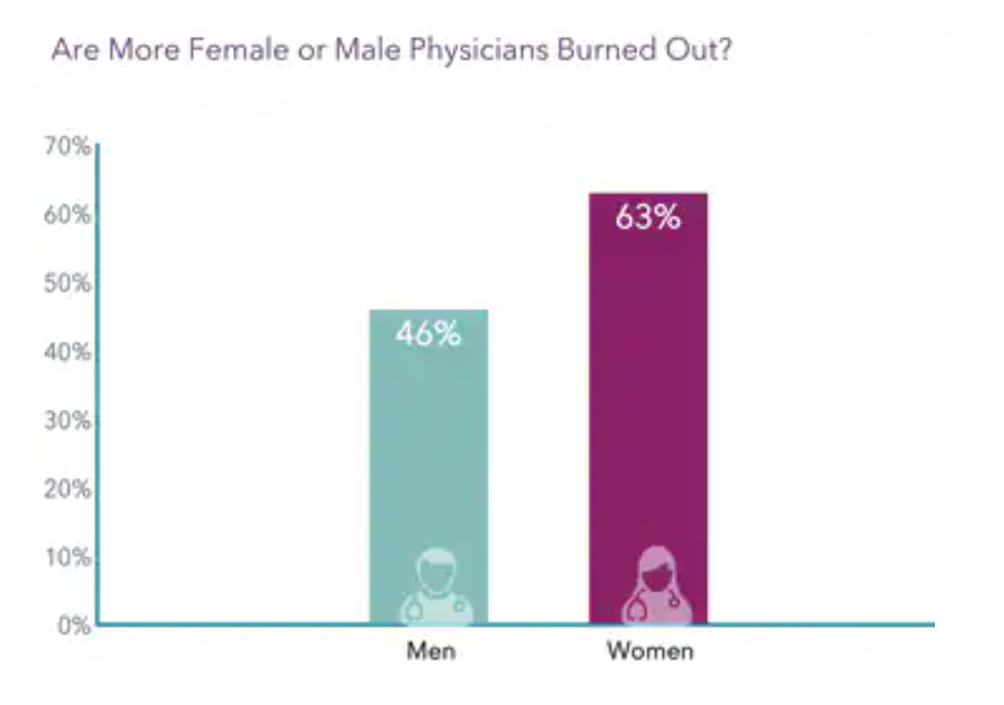
In the organization’s annual study into physicians’ wellbeing, Medscape has diagnosed worsening burnout and depression among America’s doctors. Over one-half of U.S. physicians say they are burned out or depressed, the chart from the U.S. Physician Burnout & Depression Report for 2023 calls out. “I cry but not one cares,” is one of the represented color comments provided by one of the physicians included in the survey of 9,175 physicians polled online between June and October 2022. The study covered 29 specialties, finding most burned out physicians worked in emergency medicine (65% saying
Show Me The Evidence and The ROI: Digital Health Investing in 2023 via GSR Ventures
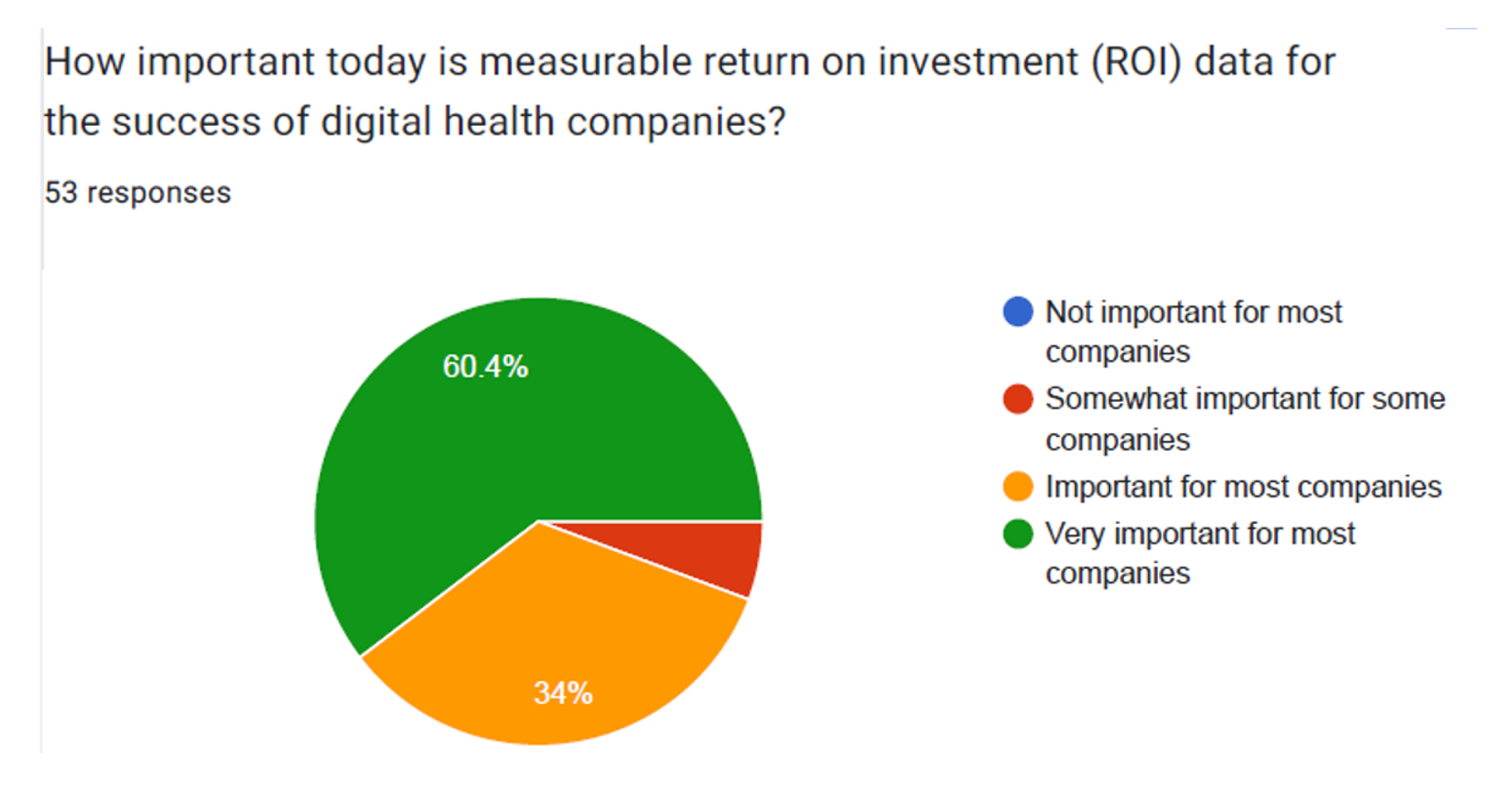
With valuations of digital health companies expected to decline in 2023, investors in the sector are Missourian in spirit in “Show Me” mode: here, it’s all about the clinical evidence and ROI, according to a survey from GSR Ventures. conducted among over 50 major digital health venture capital investors. Most of the 50+ responses to the survey expect that in 2023, valuations for digital health companies will decrease by over 20%: that’s a net of 83% including 60% expecting valuations to fall 20-40%, and 23% anticipating declines of over 40% of valuations in the next
Physicians More Bullish On the Benefits of Digital Tools for Patient Care, the AMA Tells Us

Most doctors see the advantages of digital health tools like telehealth, consumers’ access to their health information, and point-of-care workflow solutions, the American Medical Association found in a survey of 1300 physicians, published in September 2022. The AMA first conducted research with physicians and their views on digital health in July 2016. This year’s study was designed to compare current clinicians’ perspectives with those garnered in the 2016 and 2019 studies. There is a clear and positive shift of doctors’ adoption of and appreciation for digital tools, with “growth in enthusiasm” concentrated in tele-visits, the
Healthcare access, racial disparities, guns and climate – U.S. doctors are worried about some big social issues
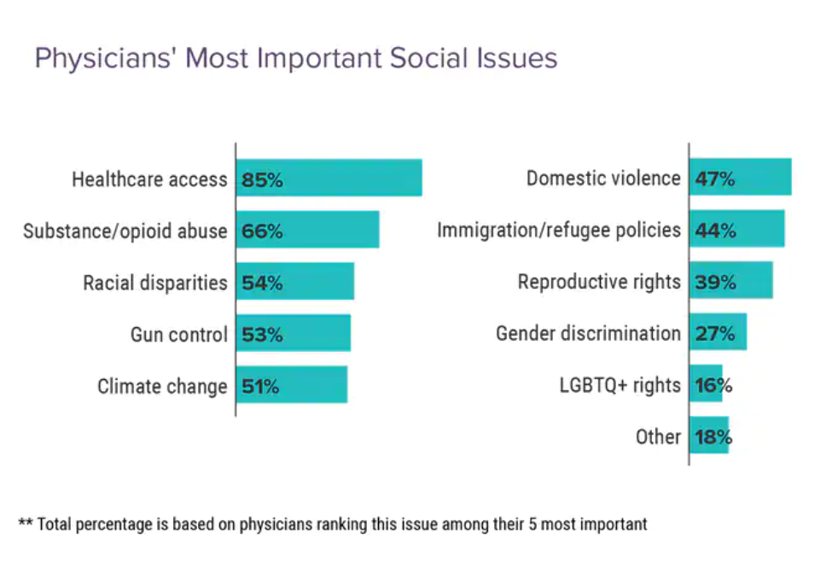
Doctors heads and hearts are jammed with concerns beyond curing patients’ medical conditions: U.S. physicians are worried about big social issues, according to a Medscape survey report, Physicians’ Views on Today’s Divisive Social Issues 2022. Topping physicians’ list of their top-five most important social issues, far above all others ranked healthcare access. Underneath that top-line statistic, it’s important to note that: 52% of doctors are “very concerned” about healthcare access, 28% are “concerned,” and 13% are “somewhat concerned.” Medscape underscores that in 2020, 31 million U.S. residents had no health insurance coverage, and
Social Determinants of Health Risks Challenge the Promise of Hospital-to-Home

In the wake of the pandemic and growing consumer preferences, the hospital-to-home movement is gaining traction among health systems. Amidst bullish forecasts for the promise of hospital-to-home discharges, the ability for many patients to make this migration would be a difficult bridge to cross. On the promising front, recent studies reviewed through a meta-analysis published in JAMA found that hospital-to-home programs can be clinically and cost-effective for inpatients discharged from hospital. Earlier this year, McKinsey addressed how “Care at Home” ecosystems can reshape the way health systems — and people — envision patient care. This
Stress in America on the Pandemic’s 2nd Anniversary: Money, Inflation, and War Add to Consumers’ Anxiety

As we mark the second anniversary of the COVID-19 pandemic, the key themes facing health citizens deal with money, inflation, and war — “piled on a nation stuck in COVID-19 survival mode,” according to the latest poll on Stress in America from the American Psychological Association. Financial health is embedded in peoples’ overall sense of well-being and whole health. Many national economies entered the coronavirus pandemic in early 2020 already marked by income inequality. The public health crisis exacerbated that, especially among women who were harder hit financially in the past two years than men were. That situation was even worse
Diagnosis: Stress, Anxiety and Anger – the 2022 Medscape Physician Burnout & Depression Report

As physicians deal on the frontlines in Year 3 of the COVID-19 pandemic, they’re stressed, anxious, and angry concludes the Medscape 2022 Physician Burnout & Depression Report. This year, the tagline focuses on stress, anxiety and anger. [Over the past couple of years, the study has used the word “suicide” in the title of the report, FYI]. Those reporting burnout are more likely women physicians than males (56% vs. 41%), work in the ER or critical care departments, and deal with too many bureaucratic tasks like charting and paperwork. For this annual look into the state of U.S. physicians mindsets





 Interviewed live on BNN Bloomberg (Canada) on the market for GLP-1 drugs for weight loss and their impact on both the health care system and consumer goods and services -- notably, food, nutrition, retail health, gyms, and other sectors.
Interviewed live on BNN Bloomberg (Canada) on the market for GLP-1 drugs for weight loss and their impact on both the health care system and consumer goods and services -- notably, food, nutrition, retail health, gyms, and other sectors. Thank you, Feedspot, for
Thank you, Feedspot, for  As you may know, I have been splitting work- and living-time between the U.S. and the E.U., most recently living in and working from Brussels. In the month of September 2024, I'll be splitting time between London and other parts of the U.K., and Italy where I'll be working with clients on consumer health, self-care and home care focused on food-as-medicine, digital health, business and scenario planning for the future...
As you may know, I have been splitting work- and living-time between the U.S. and the E.U., most recently living in and working from Brussels. In the month of September 2024, I'll be splitting time between London and other parts of the U.K., and Italy where I'll be working with clients on consumer health, self-care and home care focused on food-as-medicine, digital health, business and scenario planning for the future...