John Hancock flips the life insurance policy with wellness and data
When you think about life insurance, images of actuaries churning numbers to construct mortality tables may come to mind. Mortality tables show peoples’ life expectancy based on various demographic characteristics. John Hancock is flipping the idea life insurance to shift it a bit in favor of “life” itself. The company is teaming with Vitality, a long-time provider of wellness tools programs, to create insurance products that incorporate discounts for healthy living. The programs also require people to share their data with the companies to quality for the discounts, which the project’s press release says could amount to $25,000 over the
Consumers trust retailers to manage health as much as health providers
40% of U.S. consumers trust Big Retail to manage their health; 39% of U.S. consumers trust healthcare providers to manage their health. What’s wrong with this picture? The first chart shows the neck-and-neck tie in the horse race for consumer trust in personal health management. The Walmart primary care clinic vs. your doctor. The grocery pharmacy vis-a-vis the hospital or chain pharmacy. Costco compared to the chiropractor. Or Apple, Google, Microsoft, Samsung or UnderArmour, because “digitally-enabled companies” are virtually tied with health providers and large retailers as responsible health care managers. Welcome to The Birth of the Healthcare Consumer according
Transparency in health care: not all consumers want to look
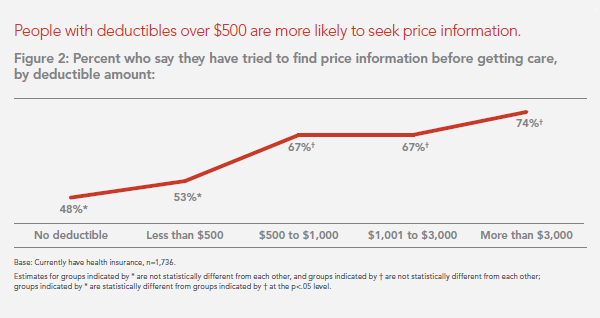
Financial wellness is integral to overall health. And the proliferation of high-deductible health plans for people covered by both public insurance exchanges as well as employer-sponsored commercial (private sector) plans, personal financial angst is a growing fact-of-life, -health, and -healthcare. Ask any hospital Chief Financial Officer or physician practice manager, and s/he will tell you that “revenue cycle management” and patient financial medical literacy are top challenges to the business. For pharma and biotech companies launching new-new specialty drugs (read: “high-cost”), communicating the value of those products to users — clinician prescribers and patients — is Job #1 (or #2,
Americans are spending $1 in $5 on health care
People in the U.S. are spending over 20.6% of their income on health care, according to data published by the U.S. Department of Commerce on March 2, 2015. This is up from 15% of personal income in 1990. Note the slope of this curve, moving up the X-Y axes from southwest to northwest. Now note the slope of the curves in the second chart, which illustrates consumer spending on other household goods and services: cars, housing, clothing, education, groceries, and eating outside of the home. Spending on these home budget line items remained relatively flat over the 25 year period 1990-2015,
Telehealth is in demand, driven by consumer convenience and cost – American Well speaks
Evidence of the rise of retail health grows, with the data point that on-demand health care is in-demand by 2 in 3 U.S. adults. American Well released the Telehealth Index: 2015 Consumer Survey, revealing an American health public keen on video visits with doctors as a viable alternative to visiting the emergency room. Virtual visits are especially attractive to people who have children living at home. [For context, this survey defines “telehealth” as a remote consultation between doctor and patient]. Convenience drives most peoples’ interest in telehealth: saving time and money, not leaving home if feeling unwell, and “avoiding germs
People in consumer-directed health plans are — surprise! — getting more consumer-directed
People with more financial skin in the health care game are more likely to act more cost-consciously, according to the latest Employee Benefits Research Institute (EBRI) poll on health engagement, Findings from the 2014 EBRI/Greenwald & Associates Consumer Engagement in Health Care Survey published in December 2014. Health benefit consultants introduced consumer-directed health plans, assuming that health plan members would instantly morph in to health care consumers, seeking out information about health services and self-advocating for right-priced and right-sized health services. However, this wasn’t the case in the early era of CDHPs. Information about the cost and quality of health care services was scant,
Building the health ecosystem: new bedfellows coming together
2015 is already becoming a year where bedfellows of different stripes are joining together to build a health care ecosystem well beyond hospitals, doctors and health plans. Announcements launched last week at the 2015 Consumer Electronics Show in Las Vegas, and coming out this week at the J.P. Morgan Conference in San Francisco, the first two weeks of 2015 reveal that new entrants and legacy health stakeholders are crossing corporate and cultural chasms to (try and) solve challenges that prevent us from getting to that Holy Grail of The Triple Aim: improving health care outcomes, driving down per capita costs,
Health and wellness at CES 2015 – trend-weaving the big ideas
Health is where we live, work, play and pray — my and others’ mantra if we want to truly bend (down) the cost curve and improve medical outcomes. If we’re serious about achieving the Triple Aim — improving public health, lowering spending, and enhancing the patient/health consumer experience (which can drive activation and ongoing engagement) — then you see health everywhere at the 2015 Consumer Electronics Show in Las Vegas this week. With this post, I’ll share with you the major themes I’m seeing at #CES2015 related to health, wellness, and DIYing medical care at home. The meta: from health care to self-care.
Health IT Forecast for 2015 – Consumers Pushing for Healthcare Transformation
Doctors and hospitals live and work in a parallel universe than the consumers, patients and caregivers they serve, a prominent Chief Medical Information Officer told me last week. In one world, clinicians and health care providers continue to implement the electronic health records systems they’ve adopted over the past several years, respond to financial incentives for Meaningful Use, and re-engineering workflows to manage the business of healthcare under constrained reimbursement (read: lower payments from payors). In the other world, illustrated here by the graphic artist Sean Kane for the American Academy of Family Practice, people — patients, healthy consumers, newly insured folks,
Power to the health care consumer – but how much and when?
Oliver Wyman’s Health & Life Sciences group names its latest treatise on the new-new health care The Patient-to-Consumer Revolution, subtitled: “how high tech, transparent marketplaces, and consumer power are transforming U.S. healthcare.” The report kicks off with the technology supply side of “Health Market 2.0,” noting that “the user experience of health care is falling behind” other industry segments — pointing to Uber for transport, Amazon for shopping, and Open Table for reserving a table. The authors estimate that investments in digital health and healthcare rose “easily ten times faster” than the industry has seen in the past. Companies like
Live from the 11th annual Connected Health Symposium – Keeping Telehealth Real
Dr. Joseph Kvedar has led the Center for Connected Health for as long as I’ve used the word “telehealth” in my work – over 20 years. After two decades, the Center and other pioneers in connected health have evidence proving the benefits, ROI (“hard” in terms of dollars, and “soft” in terms of patient and physician satisfaction), and technology efficacy for connecting health. The 11th Annual Connected Health Symposium is taking place as I write this post at the Seaport Hotel in Boston, bringing health providers, payers, plans and researchers together to share best practices, learnings and evidence supporting the
Rationing health care, driven by high deductibles
Concerns about Death Panels and government restricting health services for people that have been key arguments used against the Affordable Care Act’s (ACA) detractors and, even before the advent of the ACA, proposed health reforms under President Clinton. But it’s peoples’ self-rationing in the U.S. health system that’s causing true rationing — driven by high deductible health plans (HDHPs) that are fast-growing in the health insurance market, and by the high cost of specialty drugs and prescriptions. There are plenty of data demonstrating the consumer health rationing trend being collected and reviewed by think tanks like RAND here, and by The
Health and financial well-being are strongly linked, CIGNA asks and answers
The modern view on wellness is “having it all” in terms of driving physical, emotional, mental and financial health across one’s life, according to CIGNA’s survey report, Health & Financial Well-Being: How Strong Is the Link? The key elements of whole health, as people define them are: – Absence of sickness, 37% – Feeling of happiness, 32% – Stable mental health, 32% – Management of chronic disease, 15% – Financial health, 14% – Living my dreams, 9%. 1 in 2 people (49%) agree that health and wellness comprise “all of these” elements, listed above. This holistic view of health is
Specialty pharmaceuticals’ costs in the health economic bulls-eye
This past weekend, 60 Minutes’ Leslie Stahl asked John Castellani, the president of PhRMA, the pharmaceutical industry’s advocacy (lobby) organization, why the cost of Gleevec, from Novartis, dramatically increased over the 13 years it’s been in the market, while other more expensive competitors have been launched in the period. (Here is the FDA’s announcement of the Gleevec approval from 2001). Mr. Castellani said he couldn’t respond to specific drug company’s pricing strategies, but in general, these products are “worth it.” Here is the entire transcript of the 60 Minutes’ piece. Today, Health Affairs, the policy journal, is hosting a discussion
Health on the 2014 Gartner Hype Cycle
Remote health monitoring is in the Trough of Disillusionment. Wearables are at the Peak of Inflated Expectations, with Big Data leapfrogging wearables from the 2013 forecast — both descending toward the Disillusionment Trough. Mobile (remote) health monitoring, however, has fallen into that Trough of Disillusionment as RHM has been undergoing reality checks in the health care system especially for monitoring and patient self-management of heart disease (most notably heart failure) and diabetes. Welcome to the 2014 edition of the Gartner Hype Cycle, one of my most-trusted data sources for doing health industry forecasts in my advisory work. Compared with last year’s
Employers engaging in health engagement
Expecting health care cost increases of 5% in 2015, employers in the U.S. will focus on several tactics to control costs: greater offerings of consumer-directed health plans, increasing employee cost-sharing, narrowing provider networks, and serving up wellness and disease management programs. The National Business Group on Health’s Large Employers’ 2015 Health Plan Design Survey finds employers committed to health engagement in 2015 as a key strategy for health benefits. More granularly, addressing weight management, smoking cessation, physical activity, and stress reduction, will be top priorities, shown in the first chart. An underpinning of engagement is health care consumerism — which
Over-the-counter drugs – an asset in the collaborative, DIY health economy
Nations throughout the world are challenged by the cost of health care: from Brazil to China, India to the Philippines, and especially in the U.S., people are morphing into health care consumers. Three categories of health spending in the bulls-eye of countries’ Departments of Health are prescription drugs, and the costs of care in hospitals and doctors’ offices. In the U.S., one tactic for cost containment in health is “switching” certain prescription drugs to over-the-counter products – those deemed to be efficacious and safe for patients to take without seeking treatment from a doctor. Over-the-counter drugs (OTCs) are available every
Novel concept: people + health pricing information = market competition
In the post-Recession American economy, people shop for value in all things. And that includes health care services like MRIs — when patients are informed of pricing differences among imaging facilities and given free rein to pick-and-choose among them. In addition to lowering imaging costs in a community, price transparency also generated competition between providers. Health Affairs published this research detailed in Price Transparency for MRIs Increased Use of Less Costly Providers And Triggered Provider Competition in August 2014. An Economics 101 course teaches us that a well-oiled (perfect) market depends on lots of sellers of a product and lots of
Dialing Dr. Verizon – the telecomms company launches virtual house calls
Expanding its wireless footprint in health care, Verizon, the telecommunications company, announced the start of Verizon Virtual Visits today. The program will be marketed to employers and health plans to enable patients to see doctors at home or when traveling, via Verizon’s wireless network. I spoke with Christine Izui, Verizon’s quality officer, mobile health solution, earlier this week about Virtual Visits. We discussed the market forces that support the growth of telehealth and, in particular, physician visits “anywhere:” There is an under-supply and poor distribution of primary care doctors and certain specialties around the U.S. Employers and health plan sponsors are
Go, You Chicken Fat, Go! Kennedy Met the Music Man for Health (and Apple Takes a Bite)
What do you get when you pair Meredith Wilson, the writer-composer of The Music Man, with Robert Preston (who acted the starring role of Harold Hill, the traveling music-band instrument salesman) with a President committed to reversing the “softness” he saw in American health citizens? You get “Go, You Chicken Fat, Go,” a rousing band-and-choir backed anthem to promote people to engage in more exercise and shed their “chicken fat.” President Kennedy was the public health Prez who, in 1960, asked Meredith Wilson to pen a national anthem to motivate Americans who he considered were growing “soft.” Back in the
The business case for getting more social in health
While the U.S. spends more per person on health care than any other country in the world, we get a very low return on that investment. Other countries whose health citizens enjoy significantly better health outcomes spend less on health “care” (beds, technology, doctors’ salaries) and more per capita on social services and supports. There’s growing evidence that social factors impact health, and a business case to be made for spending more on social. The evidence and argument for providers spending more on social needs is explained in the research paper, Addressing Patients’ Social Needs: An Emerging Business Case for
The Milliman Medical Index at $23,215: A Toyota Prius, a tonne of tin, or health insurance for a family?
It costs $23,215 to cover a family of four for health care, according to the 2014 Milliman Medical Index (MMI), the annual gauge of healthcare costs from the actuarial firm. The growth rate of 5.4% from 2013 is the lowest annual change since Milliman launched the Index in 2002. This is equivalent to a new Toyota Prius or a tonne of tin. While employers cover most of these costs, the portion employees bear continues to increase. This year, insured workers will take on 42% of the total, or on average, $9,695. This is up by $552 over 2013, or 6%
We are all self-insured until we get sick – especially if we are women
During my conversation with a prominent pharma industry analyst yesterday, he observed, “As a consumer, you are self-insured until you get sick.” My brain then flashed back to a graph from the 2013 Employer Health Benefits Survey conducted annually by the Kaiser Family Foundation (KFF). The chart is shown here. It illustrates the upward line indicating that in 2013, 4 in 5 workers were enrolled in a health plan that included an annual deductible. That’s the “self-insurance” part of the observation my astute conversationalist noted. Simply put, when you are enrolled in a high-deductible health plan, You, The Consumer, are responsible for
The Season of Healthcare Transparency – Chaos, then Creation, Part 5
The consumer demand side for healthcare transparency is hungry for the light to shine on health care costs, quality and information that’s relevant and meaningful to the individual. The supply side is fast-growing, with websites and portals, government-sponsored projects, commercial-driven start-ups, and numerous mobile apps. These tools endeavor to: Help people find and access services Schedule appointments Compare peer consumers’ reviews for those providers Calculate and prepare for out-of-pocket co-payments deriving from their health plan Negotiate prices with providers Pay for the services, and Reconcile the payment with a high-deductible health plan or health savings account. On the demand side, consumers
The Season of Healthcare Transparency – Consumer Payments and Tools, Part 4
“The surge in HDHP enrollment is causing patients to become consumers of healthcare,” begins a report documenting the rise of patients making more payments to health providers. Patients’ payments to providers have increased 72% since 2011. And, 78% of providers mail paper statements to patients to collect what they’re owed. “HDHPs” are high-deductible health plans, the growing thing in health insurance for consumers now faced with paying for health care first out-of-pocket before their health plan coverage kicks in. And those health consumers’ expectations for convenience in payment methods is causing dissatisfaction, negatively affecting these individuals and their health providers’
The Season of Healthcare Transparency – Will Your Health Plan Be Your Transparency Partner? – Part 3
Three U.S. health plans cover about 100 million people. Today, those three market-dominant health plans — Aetna, Humana and UnitedHealthcare — announced that they will post health care prices on a website in early 2015. Could this be the tipping point for health care transparency so long overdue? These 3 plans are ranked #1, #4 and #5 in terms of market shares in U.S. health insurance. Together, they will share price data with the Health Care Cost Institute (HCCI), a not-for-profit organization dedicated to research on U.S. health spending. An important part of the backstory is that the HCCI was
The Season of Healthcare Transparency – HFMA’s Price Transparency Manifesto – Part 1
As Big Payors continue to shift more costs onto health consumers in the U.S., the importance of and need for transparency grows. 39% of large employers offered consumer-directed health plans (CDHPs) in 2013, and by 2016, 64% of large employers plan to offer CDHPs. These plans require members to pay first-dollar, out-of-pocket, to reach the agreed deductible, and at the same time manage a health savings account (HSA). In the past several weeks, many reports have published on the subject and several tools to promote consumer engagement in health finance have made announcements. This week of posts provides an update on
The retailization of digital health: Consumer Electronics Association mainstreams health
The Consumer Electronics Association (CEA) has formed a new Health and Fitness Technology Division, signalling the growing-up and mainstreaming of digital health in everyday life. The CEA represents companies that design, manufacture and market goods for people who pay for stuff that plugs into electric sockets and operate on batteries — like TVs, phones, music playing and listening, kitchen appliances, electronic games, and quite prominent at the 2014 Consumer Electronics Show, e-cigarettes (rebranding “safe smoking” as “vaping” technology). In its press release announcing this news, CEA President and CEO Gary Shapiro says, “Technology innovations now offer unprecedented opportunities for consumers to
The new health economy, starring the consumer
“In the New Health Economy, ‘patients’ will be ‘consumers’ first, with both the freedom and responsibility that come with making more decisions and spending their own money.” This vision of the near-future is brought to you by the New Health Economy, a report from PwC’s Health Research Institute (HRI). The chart attests the fact that U.S. “consumers” are already spending nearly $3 trillion (with a capital “T”) on products and services that bolster personal health. This spending includes $94 billion on nutrition, $62 billion on weight loss, $59 billion on sporting goods and apparel, $45 billion on (so-called) organic and
The New Chief Patient Officer
There’s a new member in the C-suite in health care, and her name is the Chief Patient Officer (CPO). That new role in health-town is filled by Dr. Anne Beal, appointed by Sanofi, the global biopharma company, to fill this new job description. Here she is, shaking hands with Colin Powell in one of the many awards ceremonies where Dr. Beal’s work in public health has been lauded. But what is a CPO? Because it’s a new job, Dr. Beal can create the role, at least within the environment and mission of Sanofi and the larger life sciences world. Some
The new math for Rx: HSAs up, adherence down
A consumer who is faced with greater financial skin-in-the-healthcare game, cost-sharing, is expected to become a smart shopper for lower-priced health products and services. When it comes to patients given prescriptions for medicines, the theory is that patients will choose less expensive generic drugs over brand names it people think the cheaper meds are good substitutes. This is referred to as the generic-drug dispensing rate (GDR). But the theory doesn’t consistently hold true in real life, a study from the Employee Benefit Research Institute (EBRI), Brand-Name and Generic Prescription Drug Use After Adoption of a Full-Replacement, Consumer-Directed Health Plan With a
Doctors and mHealth apps: chaos, evidence, creation
Over one year ago, an eClinicalWorks survey found that 9 in 10 physicians would be interested in prescribing a mobile health app to a patient. That’s a big number. That’s “interest,” but that demand hasn’t yet been expressed in the current go-go app-happy environment. An opinion piece in this week’s Online First edition of the Journal of the American Medical Association (JAMA) demonstrates the fork-in-the-road facing clinicians and the disruption/opportunity that is mobile health. In “In Search of a Few Good Apps,” a Boston-based trio of writers (two physicians and one PhD) talk about “the bewildering diversity of apps available
People want to DIY with pharma
In our increasingly-DIY society, most consumers expect high levels of access and customer service from the organizations with whom we engage. With more consumers reaching into their pockets to pay for health services and products, the health industry is increasingly a retail-facing environment. So expect quality service levels from their healthcare touch points. The pharmaceutical and prescription drug touch point is not exempt from this expectation, as learned by an Accenture survey analyzed in Great Expectations: Why Pharma Companies Can’t Ignore Patient Services. As the first picture shows, 70% of patients think pharma companies are responsible for bundling information and services
Health care in a multiscreen world
In 2014, we are digital omnivores. Most people “consume” information and entertainment on more than one screen: 7 hours’ worth over a 5-hour period. You read that right: most people who watch TV, use a laptop or PC, smartphone or tablet are multitasking use of these devices in parallel. And above all, people are using smartphones as their primary screen. The AdReaction: Marketing in a multiscreen world report from Millward Brown paints a picture of global consumers who are cobbling together multiscreen experiences. The smartphone has become the “do it all” device if you don’t carry a laptop or tablet around, especially favored
Why a grocery chain supports health data liquidity
The CEO of a family-owned grocery store chain wrote a letter to New York State lawmakers to support $65 million worth of spending on a computer system for health information in the state. That grocer is Danny Wegman, and that project is the Statewide Health Information Network, aka SHIN-NY. In his letter beginning, “Dear New York Legislator,” Wegman identifies several benefits he expects would flow out of the health IT project: 1. Improve health care for all New Yorkers 2. Lower health care costs, through reducing hospital readmission rates and reducing duplicate testing. 3. Lead to health data “liquidity” (my
Pharma warming up to the cloud to drive efficiencies and support analytics
Over the next few years, large global pharma companies will need to wring out an additional $35 billion worth of efficiencies in order to drive profitability. While the industry has most of the patent cliff challenge behind it, companies face price constraints with respect to health reform, static national economies, and access demands. As the pharmaceutical industry enters the value-based health care era, the industry must catch up with other vertical markets in adopting information technology. In particular, pharma has been slower to migrate to the cloud than other businesses, with concerns about security and health care particular needs. Today, the
Health data data everywhere – let’s human-scale it / Report from #SXSW #SXSH
Health data is everywhere, but not much useful to drink. Is #bigdata in health care at the top of the Hype Cycle? And how do we humanize it, make it relevant and useful for our everyday life? In other words, can this data help us hack our lives and health for the better? That question has been on my mind for the past couple of years since the convergence of big data and data analytics and health has emerged. Yesterday at the 2014 South-by-Southwest happening, I attended a panel discussion called Hacking Your Life For Better Health (#hacklife on Twitter).
Risk-shift: employers continue to push more risk to employees and families for health costs
With health costs increase increasing at 4.4% in 2014, a slightly higher rate of growth than the 4.1% seen in 2013. While this is lower than the double-digit increases U.S. employers faced in 2001-2004, it’s still twice the rate of general consumer price inflation. That’s what the first graph shows, based on the The 19th Annual Towers Watson/National Business Group on Health Employer Survey on Purchasing Value in Health Care. Employers generally want to continue to provide health insurance…for the time being. 92% of companies expect to make changes in health plan provisions in 2014, with 1 in 2 anticipating “significant
Employers spending more on wellness in 2014, with growing focus on food
Employers continue to invest in wellness programs aimed at improving employees’ health. In 2014, 3 in 4 employers plan to offer incentives to employees who participate in health improvement programs compared = and the financial value of these incentives has grown to $500, up from $338 in 2010. In its fifth year, the National Business Group on Health (NBGH)/Fidelity Investments have conducted their benefit consulting survey, culminating in the report, Employer Investments in Improving Employee Health. In the past 5 years, employers have increased their investments in wellness: the chart illustrates the growth of programs addressing physical activity/weight management and health eating,
HIMSS14 Monday Morning Quarterback – The Key Takeaways
Returning to terra firma following last week’s convening of the 2014 annual HIMSS conference…taking some time off for family, a funeral, the Oscars, and dealing with yet another snowstorm…I now take a fresh look back at #HIMSS14 at key messages. In random order, the syntheses are: Healthcare in America has entered an era of doing more, with less...and health information technology is a strategic investment for doing so. The operational beacon going forward is moving toward The Triple Aim: building population health, enhancing the patient’s experience, and lowering costs per patient. The CEO of Aetna, Mark Bertolini, spoke of the
The new retail health: Bertolini of Aetna connects dots between the economy and health consumers
3 in 4 people in America will buy health care at retail with a subsidy within just a few years, according to Mark Bertolini, CEO of Aetna. Bertolini was the first keynote speaker this week at the 2014 HIMSS conference convened in Orlando. Bertolini’s message was grounded in health economics 101 (about which frequent readers of Health Populi are accustomed to hearing). A healthy community drives a healthy local economy, and healthier people are more economically satisfied, Bertolini explained. The message: health care can move from being a cost driver to being an economic engine. But getting to a healthy
Where’s TripAdvisor for health care? JAMA on physician ratings sites
As more U.S. health citizens enroll in high-deductible health plans – now representing about 30% of health-insured people in America – health plan members are being called on to play the role of consumer. Among the most important choices the health consumer makes is for a physician. Ratings sites and health care report cards ranking doctors by various characteristics have been in the market for over a decade. However, little has been known on the public’s knowledge about the availability of these information sources, nor of peoples’ use of physician rating sites. This question is addressed in Public Awareness, Perception, and
Why Health IT (Should) Matter to Consumers
This is the first of four posts that are written for the HIMSS 2014 Blog Carnival. The theme, provided by HIMSS (the Healthcare Information and Management Systems Society): “Why Health IT Matters to Consumers.” You’ll note the title here has been purposefully changed. Health IT “should” matter to consumers. Since George Bush declared in 2004 that within 10 years’ time, U.S. health citizens would each have an electronic medical record, there’s been as more bipartisan support inside the Beltway for EHRs than possibly for any other issue in Congress. The American Recovery & Reinvestment Act of 2009 (ARRA), aka the
Managing cost and utilization are top goals for specialty pharmacy buyers
While the prescription drug bill makes up about 10% of U.S. national health spending, the fastest-growing component of pharmacy spending is specialty medications. These are categorized as “specialty” drugs because they rarely have generic equivalents, and treat serious or life-threatening diseases (such as cancer, MS, and rheumatoid arthritis). They are also “special” because specialty pharmaceuticals average $3,000 per patient per month and can surpass $100,000 a year for certain products. As a result, the top two goals for managing specialty medications among employers are #1, to reduce inappropriate utilization, and #2, to reduce drug acquisition costs, based on a survey
Health Care Everywhere at the 2014 Consumer Electronics Show
When the head of the Consumer Electronics Association gives a shout-out to the growth of health products in his annual mega-show, attention must be paid. The #2014CES featured over 300 companies devoted to “digital health” as the CEA defines the term. But if you believe that health is where we live, work, play, and pray, then you can see health is almost everywhere at the CES, from connected home tech and smart refrigerators to autos that sense ‘sick’ air and headphones that amplify phone messages for people with hearing aids, along with pet activity tracking devices like the Petbit. If
mHealth will join the health ecosystem – prelude to the 2014 Consumer Electronics Show
The rise of digital health at the 2014 Consumer Electronics Show signals the hockey-stick growth of consumer-facing health devices for fitness and, increasingly, more medical applications in the hands of people, patients, and caregivers. This year at #CES2014, while the 40% growth of the CES digital health footprint will get the headlines, the underlying story will go beyond wristbands and step-tracking generating data from an N of 1 to tools that generate data to bolster shared-decision making between people and the health system, and eventually support population health. For example: – Aetna is partnering with J&J to deploy their Care4Today
3 Things I Know About Health Care in 2014
We who are charged with forecasting the future of health and health care live in a world of scenario planning, placing bets on certainties (what we know we know), uncertainties (what we know we don’t know), and wild cards — those phenomena that, if they happen in the real world, blow our forecasts to smithereens, forcing a tabula rasa for a new-and-improved forecast. There are many more uncertainties than certainties challenging the tea leaves for the new year, including the changing role of health insurance companies and how they will respond to the Affordable Care Act implementation and changing mandates
Don’t over-forecast mobile health in the short-run
The 2013 Mobile Health Summit was hosted by HIMSS at The Gaylord Resort in suburban Washington DC, taking place over 4 days during the mid-atlantic region’s iciest conditions in years. But inside the cocoon of this convention space, 5,000 conveners took in demonstrations of innovations using mobile platforms and standards that extend health services, knowledge and self-help tools to people and providers. Several themes emerged out of the meeting… Lots of apps, too few business models. There are too many apps and not enough companies, Esther Dyson noted in a keynote session during which she dialogued with two Steve’s: Steven
A certain forecast: health consumers will be more cost-squeezed in 2014 for Rx and insurance
Gird your wallets, U.S. consumers: watch the dollars flow out-of-pocket for prescription drugs in 2014, as predicted by the 2013-2014 Prescription Drug Benefit Cost and Plan Design Report published by the Pharmacy Benefit Management Institute (PBMI) this week. Constraints covering most plan members are: Step therapy Prior authorization (to get approvals to fill high-cost drugs, notably growth hormones, injectables, controlled substances, Retin-A, and medications for sleep disorders, and Compulsory 90 day refills at retail (90-day dispensing for chronic meds). This Report, sponsored by Takeda, is the gold standard of drug benefit trends, having been published since 1995. Average 30-day copayments
More chronically ill people use online health resources – but they’re not so social, Pew finds
People who are diagnosed with at least one chronic medical condition are more likely to seek information online, use social media to understand peer patients’ reviews on drugs and treatments, and learn from other patients about their personal health experiences. While that’s encouraging news for a health empowerment headline, the underlying challenge that should prevent congratulatory fist-bumps among patient-engagement proponents is that people living with chronic disease are less likely to have internet access. Why? Because chronically ill people tend to be older and less educated, and they’re also less likely to be working. Simply put, “People living with chronic
Make health care “feel” more like retail via transparency
Consumers who are well-covered by health insurance are in favor of talking about costs with their doctors. This research finding illustrates the fact that price transparency in health care isn’t just the concern of un- and under-insured people, but that shining the light on the price of health care is everybody’s business. But it’s also the case that most physicians aren’t yet involved in these health-financial conversations with their patients. Two studies presented at the recent 2013 annual meeting of the American Society of Clinical Oncology (ASCO) learned that patients are keen to know more about health care costs from
Getting to health engagement will require more than a patient portal
Patient and health engagement is the flavor du jour in health circles these days, from the corridors of hospitals to the caffeinated marketing meetings in Big Pharma’s east coast meet-ups. But there’s no standard agreement on what we mean by peoples’ health engagement, whether by patient or well consumer. In Market Insights: The Evolution of Consumer Engagement in Health Care, Porter Research endeavors to deepen our understanding of this important concept. In the introductory section of the paper, “Understanding Engagement,” Porter proffers that industry – providers, payers and employers – consider engagement as “changing consumer behavior through increased participation in consumers’ own health
Innovating and thriving in value-based health – collaboration required
In health care, when money is tight, labor inputs like nurses and doctors stretched, and patients wanting to be treated like beloved Amazon consumers, what do you do? Why, innovate and thrive. This audacious Holy Grail was the topic for a panel II moderated today at the Connected Health Symposium, sponsored by Partners Heathcare, the Boston health system that includes Harvard’s hospitals and other blue chip health providers around the region. My panelists were 3 health ecosystem players who were not your typical discussants at this sort of meeting: none wore bow ties, and all were very entrepreneurial: Jeremy Delinsky
The new era of consumer health risk management: employers “migrate” risk
The current role of health insurance at work is that it’s the “benefits” part of “compensation and benefits.” Soon, benefits will simply be integrated into “compensation and compensation.” That is, employers will be transferring risk to employees for health care. This will translate into growing defined contribution and cost-shifting to employees. Health care sponsorship by employers is changing quite quickly, according to the 2013 Aon Hewitt Health Care Survey published in October 2013. Aon found that companies are shifting to individualized consumer-focused approaches that emphasize wellness and “health ownership” by workers to bolster behavior change and, ultimately, outcomes. The most
A new medical side-effect: out-of-pocket health care costs
When we say the phrase “side effects,” what do we think of? The FDA says that “all medicines have benefits and risks. The risks of medicines are the chances that something unwanted or unexpected could happen to you when you use them. Risks could be less serious things, such as an upset stomach, or more serious things, such as liver damage.” There’s a new risk in town in health care, and it’s the equivalent of an upset stomach when it comes to a co-pay for a branded on-formulary drug, or liver damage if it involves a coinsurance percent of “retail”
For Medtech, Design is the New Plastics (advice to The Graduate)
Return on innovation in medical technology is on the decline. Med tech needed a GPS for its role in the health ecosystem, and lost its way as it focused on a few wrong priorities. In a $349 billion market, there has been much to lose…and will be to gain. The new world for medical technology and how the industry can turn around is the subject of P2C’s report, Medtech companies prepare for an innovation makeover, published in October 2013 by the PwC Health Research Institute (HRI). The problem has been an addiction to incremental improvements on existing products: think about the analog in
7 Women and 1 Man Talking About Life, Health and Sex – Health 2.0 keeping it real
Women and binge drinking…job and financial stress…sleeplessness…caregiving challenges…sex…these were the topics covered in Health 2.0 Conference’s session aptly called “The Unmentionables.” The panel on October 1, 2013, was a rich, sobering and authentic conversation among 7 women and 1 man who kept it very real on the main stage of this mega-meeting that convenes health technology developers, marketers, health providers, insurers, investors, patient advocates, and public sector representatives (who, sadly, had to depart for Washington, DC, much earlier than intended due to the government shutdown). The Unmentionables is the brainchild of Alexandra Drane and her brilliant team at the Eliza
The slow economy is driving slower health spending; but what will employers do?
By 2022, $1 in every $5 worth of spending in the U.S. will go to health care in some way, amounting to nearly $15,000 for each and every person in America. From biggest line item on down, health spending will go to payments to: Hospitals, representing about 32% of all spending Physicians and clinical costs, 20% of spending Prescription drugs, 9% of spending Nursing, continuing care, and home health care, together accounting for over 8% of health spending (added together for purposes of this analysis) Among other categories like personal care, durable medical equipment, and the cost of health insurance.
Healing the Patient-Doctor Relationship with Health IT
A cadre of pioneering Americans has been meaningfully using personal health information technology (PHIT), largely outside of the U.S. health care system. These applications include self-tracking and wearable health technologies, mobile health apps, and digital medical tracking devices like glucometers that streamline tracking and recording blood glucose levels. In the meantime, only 21% of doctors surveyed by Accenture currently allow patients to have online access to their medical summary or patient chart – very basic components of the electronic health record. We know what’s primarily driving health providers’ adoption of health IT: namely, the HITECH Act’s provisions for incentives. But
Defining Mobile Health – the blur between health and health care
Mobilising Healthcare, a new report from Juniper Research, segments the mobile health sector into “healthcare” and “health & fitness” segments. The research summary notes that fitness is a relatively new market compared with health “care,” which has been around for eons. Fitness, the analysts say, “is exempt from government intervention.” Mobile healthcare (“mHealth”) applications explored include SMS health messaging, remote health provision such as cardiac monitoring, electronic health records and personal health records. In mFitness, Juniper looks into mobile tech for athletes and fitness conscious people, and activity tracking including heart function, distance, respiration, and perspiration, among other parameters. mHealth
Consumers don’t get as much satisfaction with high-deductible health plans
Since the advent of the so-called consumer-directed health care era in the mid-2000s, there’s been a love-gap between health plan members of traditional plans, living in Health Plan World 1.0, and people enrolled in newer consumer-driven plans – high-deductible health plans (HDHPs) and consumer-directed health plans (CDHPs). That gap in plan satisfaction continues, according to the Employee Benefits Research Institute (EBRI)’s poll of Americans’ consumer engagement in health care. The survey was conducted with the Commonwealth Fund. As the bar chart illustrates, some 62% of members in traditional plans were satisfied (very or extremely) with their health insurance in 2012.
People with doctors interested in EMRs, but where’s the easy button?
1 in two people who are insured and have a regular doctor are interested in trying out an electronic medical record. But they need a doctor or nurse to suggest this, and they need it to be easy to use. The EMR Impact survey was conducted by Aeffect and 88 Brand Partners to assess 1,000 U.S. online consumers’ views on electronic medical records (EMRs): specifically, how do insured American adults (age 25 to 55 who have seen their regular physician in the past 3 years) view accessing their personal health information via EMRs? Among this population segment, 1 in 4 people (24%)
Working for health care in 2013: workers’ health insurance cost burden still grows faster than wages
Insurance premium costs grew 4% for families between 2012 and 2013, with workers now bearing 39% of health premiums in 2013 compared with only 26% ten years ago, in 2003. That’s a 50% increase in health plan premium “burden” for working families, by my calculation. This snapshot of health insurance in 2013 comes to us from the 2013 Employer Health Benefits Survey, provided by the Kaiser Family Foundation (KFF) and the Health Research & Educational Trust (HRET). This research is one of the most important annual reports to hit the health care industry every year, and this year’s analysis provides strategic context
10 Reasons Why ObamaCare is Good for US
When Secretary Sebelius calls, I listen. It’s a sort of “Help Wanted” ad from the Secretary of Health and Human Services Kathleen Sebelius that prompted me to write this post. The Secretary called for female bloggers to talk about the benefits of The Affordable Care Act last week when she spoke in Chicago at the BlogHer conference. Secretary Sebelius’s request was discussed in this story from the Associated Press published July 25, 2013. “I bet you more people could tell you the name of the new prince of England than could tell you that the health market opens October 1st,” the
In the US health care cost game, doctors have seen the enemy – and it’s not them
When it comes to who’s most responsible for reducing the cost of health care in America, most doctors put the onus on trial lawyers, health insurance companies, pharma and medical device manufacturers, hospitals, and even patients. But physicians themselves ? Not so much responsibility – only 36% of doctors polled said doctors should assume major responsibility in reducing health care costs. And, in particular, most U.S. physicians have no enthusiasm for reducing health care costs by changing payment models, like penalizing providers for hospital re-admissions or paying a group of doctors a fixed, bundled price for managing population health. Limiting
Urgent care centers: if we build them, will all patients come?
Urgent care centers are growing across the United States in response to emergency rooms that are standing-room-only for many patients trying to access them. But can urgent care centers play a cost-effective, high quality part in stemming health care costs and inappropriate use of ERs for primary care. That’s a question asked and answered by The Surge in Urgent Care Centers: Emergency Department Alternative or Costly Convenience? from the Center for Studying Health System Change by Tracy Yee et. al. The Research Brief defines urgent care centers (UCCs) as sites that provide care on a walk-in basis, typically during regular
What to expect from health care between now and 2018
Employers who provide health insurance are getting much more aggressive in 2013 and beyond in terms of increasing employees’ responsibilities for staying well and taking our meds, shopping for services based on cost and value, and paying doctors based on their success with patients’ health outcomes and quality of care. Furthermore, nearly one-half expect that technologies like telemedicine, mobile health apps, and health kiosks in the back of grocery stores and pharmacies are expected to change the way people regularly receive health care. What’s behind this? Increasing health care costs, to be sure, explains the 18th annual survey from the National
They call it “primary” care because it comes first — and it should
It’s called “primary” care for a reason: it’s first and foremost important in the health care services a person can use. In its report, Primary care: our first line of defense, The Commonwealth Fund explains why primary care is crucial to one’s individual health, and how primary care is morphing into medical teams and patient-centered medical homes. And that’s a good thing for you and me, the Fund says. That’s because people in the U.S. who have a primary care doctor have 33% lower health costs and 19% lower risk of dying than people who see only a specialist (Source:
Health consumers, meet the medical bank
Health consumers, meet a new player in your health care world: the bank. Financial services companies will play a growing role in U.S. health care as patients morph into health care consumers responsible for making more money-based decisions about their health care. This shift could make paying for health care just like paying other bills in the consumer retail market. And that’s a new role for health providers – doctors and hospitals – to fill. The Impact of Growing Patient Financial Responsibility on Healthcare Providers, prepared for Citi Enterprise Payments by Boundary Information Group, discusses what the impact of consumers’ payments in
As health cost increases moderate, consumers will pay more: will they seek less expensive care?
While there is big uncertainty about how health reform will roll out in 2014, and who will opt into the new (and improved?) system, health cost growth will slow to 6.5% signalling a trend of moderating medical costs in America. Even though more newly-insured people may seek care in 2014, the costs per “unit” (visit, pill, therapy encounter) should stay fairly level – at some of the lowest levels since the U.S. started to gauge national health spending in 1960. That’s due to “the imperative to do more with less has paved the way for a true transformation of the
The emerging economy for consumer health and wellness
The notion of consumers’ greater skin in the game of U.S. health care — and the underlying theory of rational economic men and women that would drive people to greater self-care — permeated the agenda of the 2nd annual Consumer Health & Wellness Innovation Summit, chaired by Lisa Suennen of Psilos Ventures. Lisa kicked off the meeting providing a wellness market landscape, describing the opportunity that is the ‘real’ consumer-driven health care: people getting and staying well, and increasing participation in self-management of chronic conditions. The U.S. health system is transforming, she explained, with payors beginning to look like computer
Consumer-directed health isn’t always so healthy
Giving health consumers more skin in the game doesn’t always lead to them making sound health decisions. Over four years in consumer-directed health plans, enrollees used one-quarter fewer visits to doctors every year and filled one fewer prescription drugs. CDHP members also received fewer recommended cancer screenings, and visited the emergency room more often. These rational health consumer theory-busting findings were published in the June 2013 issue of the Health Affairs article, Consumer-Directed Health Plans Reduce The Long-Term Use of Outpatient Physician Visits And Prescription Drugs by Paul Fronstin of the Employee Benefit Research Institute and colleagues from IBM and RxEconomics,
Health care costs for a family of 4 in 2013: a college education, a diamond or a 4-door sedan
If you have $22,030 in your wallet, you can buy: A princess-cut diamond A Ford Focus 4-door A year’s tuition at James Madison University (in-state, 2013-14) A health plan for a family of four. The 2013 Milliman Medical Index gauges the annual health care costs for a typical American family at $22,030, up $1,302 from 2012 — a 6.3% increase, nearly 6x the all-items increase of 1.1% for the U.S. Consumer Price Index from April 2012-April 2013. That 1.1% includes the costs of food and energy, along with cars, tobacco, shelter, and other consumer goods. In 2013, the average family will
Most employers will provide health insurance benefits in 2014…with more costs for employees
Nearly 100% of employers are likely to continue to provide health insurance benefits to workers in 2014, moving beyond a “wait and see” approach to the Affordable Care Act (ACA). As firms strategize tactics for a post-ACA world, nearly 40% will increase emphasis on high-deductible health plans with a health savings account, 43% will increase participants’ share of premium costs, and 33% will increase in-network deductibles for plan members. Two-thirds of U.S. companies have analyzed the ACA’s cost impact on their businesses but need to know more, according to the 2013 survey from the International Foundation of Employee Benefit Plans (IFEBP).
The Slow Economy Has Slowed Health Spending
Why has health cost growth in the U.S. slowed in the past few years? It’s mostly due to the economy, argues the Kaiser Family Foundation in Assessing the Effects of the Economy on the Recent Slowdown of Health Spending. The answer to this question is important because, as the American economy recovers, it begs the next question: will costs increase faster once again as they did in previous go-go U.S. economies, further exacerbating the budget deficit problems in the long-term? KFF worked with Altarum to develop an economic model to answer these questions. The chart illustrates the predicted vs. actual
Bending the cost-curve: a proposal from some Old School bipartisans
Strange political bedfellows have come together to draft a formula for dealing with spiraling health care costs in the U.S. iin A Bipartisan Rx for Patient-Centered Care and System-Wide Cost Containment from the Bipartisan Policy Center (BPC). The BPC was founded by Senate Majority Leaders Howard Baker, Tom Daschle, Bob Dole, and George Mitchell. This report also involved Bill Frist, Pete Domenici, and former White House and Congressional Budget Office Director Dr. Alice Rivlin who together work with the Health Care Cost Containment Initiative at the BPC. The essence of the 132-page report is that the U.S. health system is
The value of big data in health care = $450 billion
Exploiting Big Data in industry is Big News these days, and nowhere is the potential for leveraging the concept greater than in health care. McKinsey & Company estimates that harnessing big data across five dimensions of health care could yield nearly one-half trillion dollars’ worth of value in The ‘big data’ revolution in healthcare. The chart summarizes McKinsey’s calculations on the value of Big Data in health care at its maximum. Before digging into the value potential, just what is Big Data in health care? Statistics and information are generated in the health care system about patients: say, during visits
U.S. Health Costs vs. The World: Is It Still The Prices, and Are We Still Stupid?
Comparing health care prices in the U.S. with those in other developed countries is an exercise in sticker shock. The cost of a hospital day in the U.S. was, on average, $4,287 in 2012. It was $853 in France, a nation often lauded for its excellent health system and patient outcomes but with a health system that’s financially strapped. A routine office visit to a doctor cost an average of $95 in the U.S. in 2012. The same visit was priced at $30 in Canada and $30 in France, as well. A hip replacement cost $40,364 on average in the
The Not-So-Affordable Care Act? Cost-squeezed Americans still confused and need to know more
While health care cost growth has slowed nationally, most Americans feel they’re going up faster than usual. 1 in 3 people believe their own health costs have gone up faster than usual, and 1 in 4 feel they’re going out about “the same amount” as usual. For only one-third, health costs feel like they’re staying even. As the second quarter of 2013 begins and the implementation of the Affordable Care Act (ACA, aka “health reform” and “Obamacare”) looms nearer, most Americans still don’t understand how the ACA will impact them. Most Americans (57%) believe the law will create a government-run health plan,
Arianna and Lupe and Deepak and Sanjay – will the cool factor drive mobile health adoption?
Digital health is attracting the likes of Bill Clinton, Lupe Fiasco, Deepak Chopra, Dr. Sanjay Gupta, Arianna Huffington, and numerous famous athletes who rep a growing array of activity trackers, wearable sensors, and mobile health apps. Will this diverse cadre of popular celebs drive consumer adoption of mobile health? Can a “cool factor” motivate people to try out mobile health tools that, over time, help people sustain healthy behaviors? Mobile and digital health is a fast-growing, good-news segment in the U.S. macroeconomy. The industry attracted more venture capital in 2012 than other health sectors, based on Rock Health’s analysis of the year-in-review. Digital health
The lights are still out on health prices for Americans – #healthcost transparency limits consumerism in health
Only two U.S. states have comprehensive health care price transparency regulations that ensure citizens’ access to clear and open health price information. While those two states, Massachusetts and New Hampshire, earn an “A” in the Report Card on State Price Transparency Laws, an addition five state earn a “B,” with the remainder of the United States garnering a “C” or less. The map illustrates that most states are red states, earning the lowest score of “F.” With the growth of high-deductible health plans (under the umbrella of so-called “consumer-directed” plans) where health consumers pay thousands of dollars to meet a spending
A health economics lesson from Jonathan Bush, at the helm of athenahealth
At HIMSS13 there are the equivalent of rock stars. Some of these are health system CIOs and health IT gurus who are driving significant and positive changes in their organizations, like Blackford Middleton, Keith Boone, Brian Ahier, and John Halamka. Others are C-level execs at health IT companies. In this latter group, many avoid the paparazzi (read: health trade reporters) and stay cocooned behind closed doors in two-story pieces of posh real estate on the exhibition floor. A few walk the floor, shake hands with folks, and take in the vibe of the event. We’ll call them open-source personalities. The
The future of sensors in health care – passive, designed, integrated
Here’s Ann R., who is a patient in the not-too-distance-future, when passive sensors will be embedded in her everyday life. The infographic illustrates a disruption in health care for people, where data are collected on us (with our permission) that can help us improve our own self-care, and help our clinicians know more about us outside of their offices, exam rooms and institutions. In Making Sense of Sensors: How New Technologies Can Change Patient Care, my paper for the California HealthCare Foundation, I set out to organize the many types of sensors proliferating the health care landscape, and identify key
Consumer health empowerment is compromised by complex information
The U.S. economy is largely built on consumer purchasing (the big “C” in the GDP* – see note, below Hot Points). Americans have universally embraced their role as consumers in virtually every aspect of life — learning to self-rely in making travel plans, stock trades, photo development, and purchasing big-dollar hard goods (like cars and washing machines). Consumers transact these activities thanks to usable tools and information that empower them to learn, compare, and execute smarter decisions. That is, in every aspect of life but in health care. While the banner of “consumerism” in health care has been flown
The Accountable Care Community opportunity
“ACOs most assuredly will not…deliver the disruptive innovation that the U.S. health-care system urgently needs,” wrote Clay Christensen, godfather of disruptive innovation, et. al., in an op-ed in the Wall Street Journal of February18, 2013. In the opinion piece, Christensen and colleagues make the argument that Accountable Care Organizations (ACOs) as initially conceived won’t address several key underlying forces that keep the U.S. health care industry in stasis: Physicians’ behavior will have to change to drive cost-reduction. Clinicians will need “re-education,” the authors say, adopting evidence-based medicine and operating in lower-cost milieus. Patients’ behavior will have to change. This requires
Lower calories are good business
The restaurant chain business employs 10% of U.S. workers and accounts for $660 bn worth of the national economy. Where restaurant chains are growing fastest is in serving up lower-calorie meals, and it’s been a boon to the bottom-line. The case for lower calories leading to better business is made in Lower-Calorie Foods: It’s Just Good Business from the Hudson Institute‘s Obesity Solutions Initiative, published February 2013. In the report, researchers analyzed nitty-gritty restaurant chain data on servings and traffic from 2006-2011 to sort out whether sales of so-called lower-calorie menu items in 21 chains led to improved business. The chains
Health cost transparency on the W-2: sticker shock at the point-of-paystub
If you receive health insurance benefits from your employer, you’ll see a new line item on your W-2, courtesy of the Internal Revenue Service: the cost of employer-sponsored group health plan coverage. This new piece of data, shown in Box 12, DD information, comes as part of health reform, The Affordable Care Act, which requires employers with over 250 workers to show how much they spend on employer-sponsored health benefits in total. This is the employer’s premium cost, and does not include the covered worker’s out-of-pocket spending (e.g., copays, coinsurance and deductibles). It is being furnished on W-2’s “for informational
The more engaged a patient is, the lower their costs
There are many ways to measure and express “patient engagement.” One such metric is “patient activation,” innovated by Dr. Judith Hibbard, long affiliated with the University of Oregon. Dr. Hibbard has written extensively about the Patient Activation Measure, PAM, first described in 2004. She and a team of researchers have determined that the higher a patient’s PAM score, the lower their health costs. Hibbard et. al. published these findings in the February 2013 issue of Health Affairs, which is entirely devoted to patient engagement – a top topic in Health Populi. The team analyzed the medical records of 33,163 patients
More consumers want to make health care decisions
U.S. consumers’ desire to take an active role in their health decisions is growing, according to the Altarum Institute Survey of Consumer Health Care Opinions. 61% of people want to make health decisions either on their own (26%) or with input from their doctor (38%). The proportion of people wanting to be “completely in charge of my decisions” rose 4 percentage points in one year, from 2011. This statistic skews younger, with 33% of people 25-34 and 31% of those 35-44 wanting to be “completely in charge.” Only 17% of those 55-64 felt like being totally in charge of their
Health reform, costs and the growing role of consumers: PwC’s tea leaves for 2013
PwC has seen the future of health care for the next year, and the crystal ball expects to see the following: Affordable Care Act implementation, with states playing lead roles The role of dual eligibles Employer’s role in health care benefits Consumers’ role in coverage Consumers’ ratings impact on health care Transforming health delivery Population health management Bring your own device Pharma’s changing value proposition The medical device industry & tax impact. In their report, Top health industry issues of 2013: picking up the pace on health reform, PwC summarizes these expectations as a “future [that] includes full implementation of
Retail and work-site clinics – medical homes for younger adults?
The use of retail and work-site health clinics is up, and their consumers skew young. Overall, 27% of all U.S. adults have stepped into a walk-in clinic in the past two years. But only 15% of people 65 and over have used such a clinic. This begs the question: are retail and on-site clinics at the workplace filling the role of medical homes for younger adult Americans? The Harris Interactive/HealthDay poll published in January 2013 discovered that use of retail clinics grew from 7% in 2008 to 27% in 2012. The largest age cohort using walk-in clinics is people between
Cost-conscious health consumers are adopting personal health IT
People enrolled in consumer-directed health plans (CDHPs) and high-deductible health plans (HDHPs) are more cost-conscious than those enrolled in more traditional plans, according to Findings from the 2012 EBRI/MGA Consumer Engagement in Health Care Survey from the Employee Benefit Research Institute (EBRI), published in December 2012. The logic behind CDHPs and HDHPs is that if health plan enrollees have more “skin in the game” — that is, personal financial exposure — they’ll behave more like health “consumers.” By 2012, 36% of employers with over 500 employees offered either HRA- or HSA-eligible plans. About 15% of working age adults are enrolled
Call them hidden, direct or discretionary, health care costs are a growing burden on U.S. consumers
Estimates on health spending in the U.S. are under-valued, according to The hidden costs of U.S. health care: Consumer discretionary health care spending, an analysis by Deloitte’s Center for Health Solutions. Health spending in the U.S. is aggregated in the National Health Expenditure Accounts (NHEA), assembled by the Department of Health and Human Services (DHHS) Centers for Medicare and Medicaid Services (CMS). In 2010, the NHEA calculated that $2.6 trillion were spent on health care based on the categories they “count” for health spending. These line items include: Hospital care Professional services (doctors, ambulatory care, lab services) Dental services Residential
The physician time-squeeze and burnout: just-in-time information is part of the solution
One in two doctors is burned out. Physicians are seeing more patients in a day and spend less time with each of them. This leads to job burnout, and greater probability for medical errors and eventual liability challenges, along with feeling pushed toward early retirement. In a study published in August 2012 in the Archives of Internal Medicine, Mayo Clinic researchers learned that physicians are more burned out than workers in any other profession. And those at greatest risk of “being on a hamster wheel,” as Dr. Jeff Cain, president-elect of the American Academy of Family Physicians describes the scenario, are primary
Americans #1 health care priority for the President: reduce costs
Reducing health care costs far outranks improving quality and safety, improving the public’s health, and upping the customer experience as Americans’ top priority for President Obama’s health care agenda, according to a post-election poll conducted by PwC’s Health Research Institute. In Warning signs for health industry, PwC’s analysis of the survey results, found that 7 in 10 Americans point to the high costs of health care as their top concern in President Obama’s second term for addressing health care issues. Where would cost savings come from if U.S. voters wielded the accountant’s scalpel? The voters have spoken, saying, Reduce payments
Employers slow health cost increases for 2013 by growing consumer-directed plans
Health benefit costs grew a relatively low 4.1% in 2012 (5.4% for large employers), largely due to companies moving workers into lower-cost consumer-directed health plans. Last year, benefit costs grew at an annual rate of 6.1%, representing about a 30% fall in year-on-year cost growth for companies. And, coverage is up to 59% of employees having ticked down to 55% for the past couple of years. Employers expect about a 5% increase for 2013. Mercer’s National Survey of Employer-Sponsored Health Plans analysis finds that U.S. employers are looking toward 2014, when they’ll be covering more uninsured workers, and using this advance
The 3 cliffs of health care
As I prepare remarks to present a talk about health reform and the pharmaceutical market landscape for tomorrow, Election Day, it struck me that the health industry is now facing 3 Cliffs: the patent cliff, the health care cost cliff, and the Fiscal Cliff. The patent cliff represents about $290 billion worth of sales losses to the pharmaceutical industry between 2012 and 2018. The first chart illustrates that dramatic slope downward, with this year, 2012, being the height of patent losses for the industry. EvaluatePharma, a UK consultancy, says that falling revenue for a pharma is usually a precursor to
Aetna finds consumers aren’t very empowered in health
Americans find health insurance decisions the second most difficult major life decision only behind saving for retirement (36%) and slightly more difficult than purchasing a car (23%), via Aetna’s Empowered Health Index Survey. Why are health insurance choices so tough? Consumers told Aetna that the available information is confusing and complicated (88% percent), there is conflicting information (84%) and it’s difficult to know which plan is right for them (83%). Based on this survey’s findings, millions of Americans indeed feel dis-empowered by health care decision making. Who is empowered? Aetna says the empowered are likely to be more affluent, insured, married, take
A handful of health plans adopts HIT to get closer to consumers
Health payers and plans are realigning their business operations to get closer to consumers. Anticipating the impact of the Affordable Care Act (ACA), coupled with the continuing trend toward consumer-driven health plans, Chilmark Research published the 2012 Benchmark Report: Payer Adoption of Emerging Consumer Tech in August 2012. John Moore, industry analyst and founder of Chilmark, and I had an email exchange to discuss the report. JSK: Why is this topic so timely now? JM: Payers have been trying for years to engage their members with less than stellar results. The advent of new consumer technologies such as social media, mobile,
Wellness takes hold among large employers – and more sticks nudge workers toward health
Employee benefits make up one-third of employers’ investments in workers, and companies are looking for positive ROI on that spend. Health benefits are the largest component of that spending, and are a major cost-management focus. In 2012 and beyond, wellness is taking center stage as part of employers’ total benefits strategies. In the 2012 Wellness & Benefits Administration Benchmarking study, a new report from bswift, a benefits administration company, the vast majority of large employers (defined as those with over 500 workers) are sponsoring wellness programs, extending them to dependents as well as active workers. Increasingly, sticks accompany carrots for





 Thank you
Thank you  Jane joined host Dr. Geeta "Dr. G" Nayyar and colleagues to brainstorm the value of vaccines for public and individual health in this challenging environment for health literacy, health politics, and health citizen grievance.
Jane joined host Dr. Geeta "Dr. G" Nayyar and colleagues to brainstorm the value of vaccines for public and individual health in this challenging environment for health literacy, health politics, and health citizen grievance.  I'm grateful to be part of the Duke Corporate Education faculty, sharing perspectives on the future of health care with health and life science companies. Once again, I'll be brainstorming the future of health care with a cohort of executives working in a global pharmaceutical company.
I'm grateful to be part of the Duke Corporate Education faculty, sharing perspectives on the future of health care with health and life science companies. Once again, I'll be brainstorming the future of health care with a cohort of executives working in a global pharmaceutical company.