What’s Expected to Drive Up Health Plan Costs in 2025: GLP-1s, Behavioral Health, and Inflationary Pressures for Hospitals and Doctors – PwC’s Behind the Numbers 2025
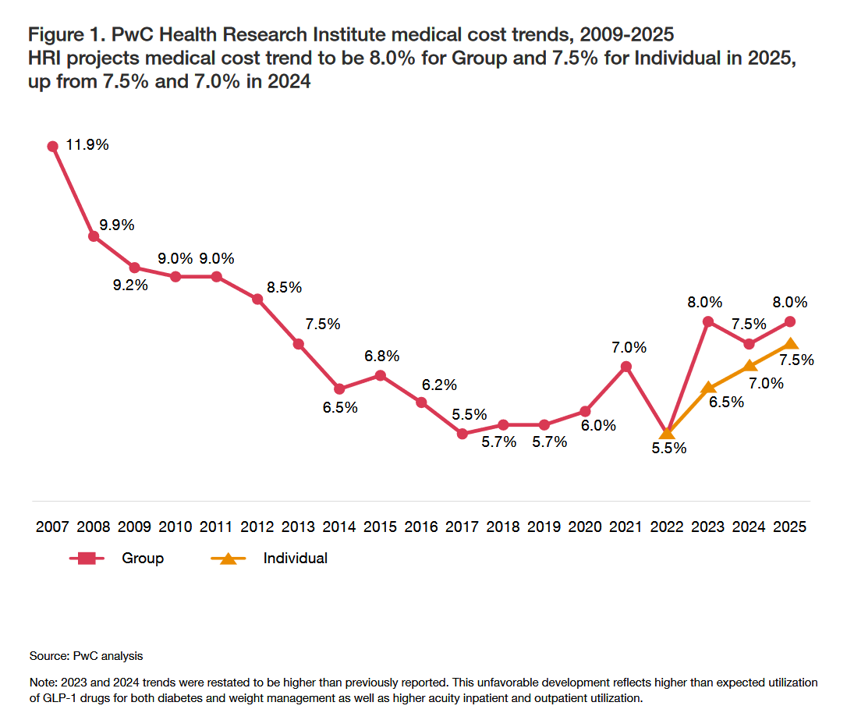
The U.S. Bureau of Labor Statistics had good news for American consumers long-facing inflation for household spending over the past couple of years, announcing on July 11, 2024, that the general consumer price index (CPI) fell, lowering real prices for people buying airline tickets, used cars and trucks, communication, and petrol to fill auto tanks. That positive economic news did not extend to medical care and personal care, the BLS reported, whose costs increased by 3.3% and 3.2%, respectively. (Motor vehicle insurance costs grew a whopping 19.5% in the report, FYI). Following the
Financial Strain Among Older People in America, and What Project 2025 Could Mean for Their Well-Being
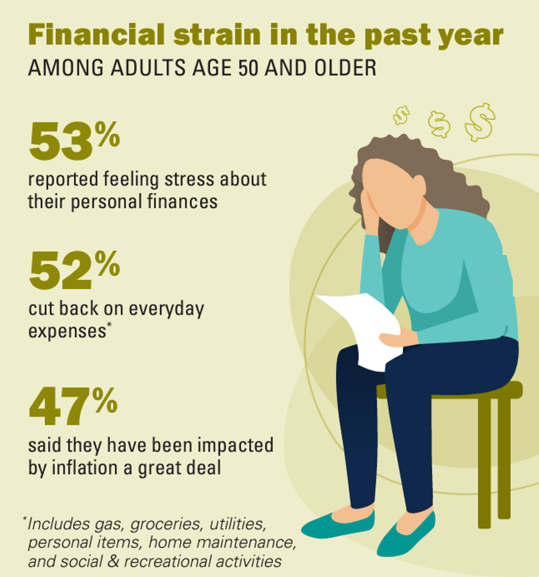
Over one-half of people 50 years of age and older in the U.S. have felt financial strain in the past year, resulting in 1 in 2 folks cutting back on everyday expenses like groceries and gas. We learn that nearly one-half of people 50 and over say they’ve been impacted by inflation “a great deal” in Making Ends Meet: Financial Strain and Well-Being Among Older Adults, the latest report from the Institute for Healthcare Policy and Innovation’s National Poll on Healthy Aging based at the University of Michigan (my alma mater). The poll was conducted by NORC at the University
“Listen to Me:” Personalization in Health Care Starts With Taking Patients’ Voices Seriously – the 15th Beryl Institute-Ipsos PX Pulse Survey
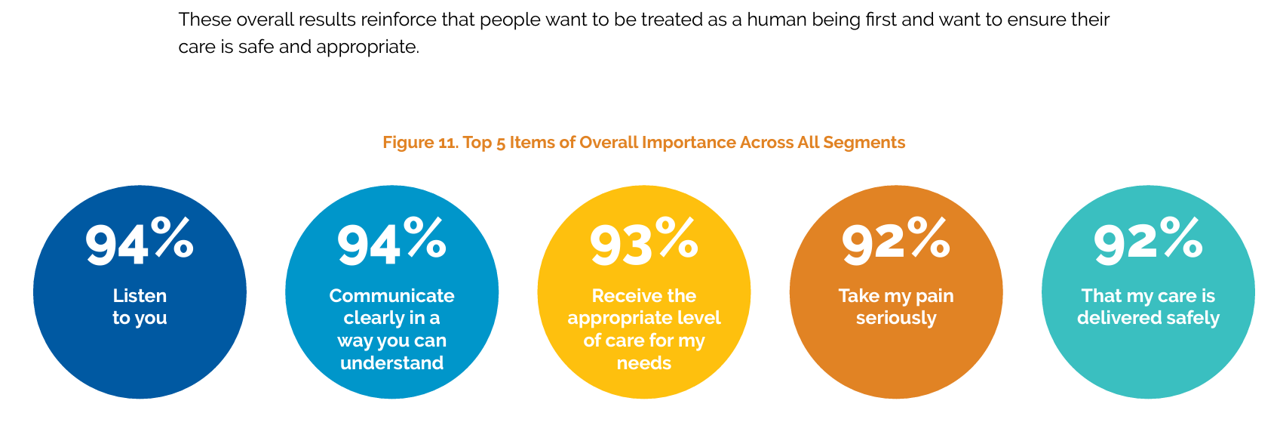
Patients’ experience with health care in the U.S. dropped to its lowest point over the past year, explained in the 15th release of The Beryl Institute – Ipsos PX Pulse survey. The study into U.S. adult consumers’ perspectives defined “patient experience” (PX) as, “The sum of all interactions, shaped by an organization’s culture, that influence patient perceptions across the continuum of care.” The survey was fielded by Ipsos among 1,018 U.S. adults in March 2024. Health care providers (and other industry stakeholders that go B2B or B2B2C (or P) are all thinking
Medical Debt, Aflac on Eroding Health Benefits, the CBO’s Uninsured Forecast & Who Pays for Rising Health Care Prices: A Health Consumer Financial Update
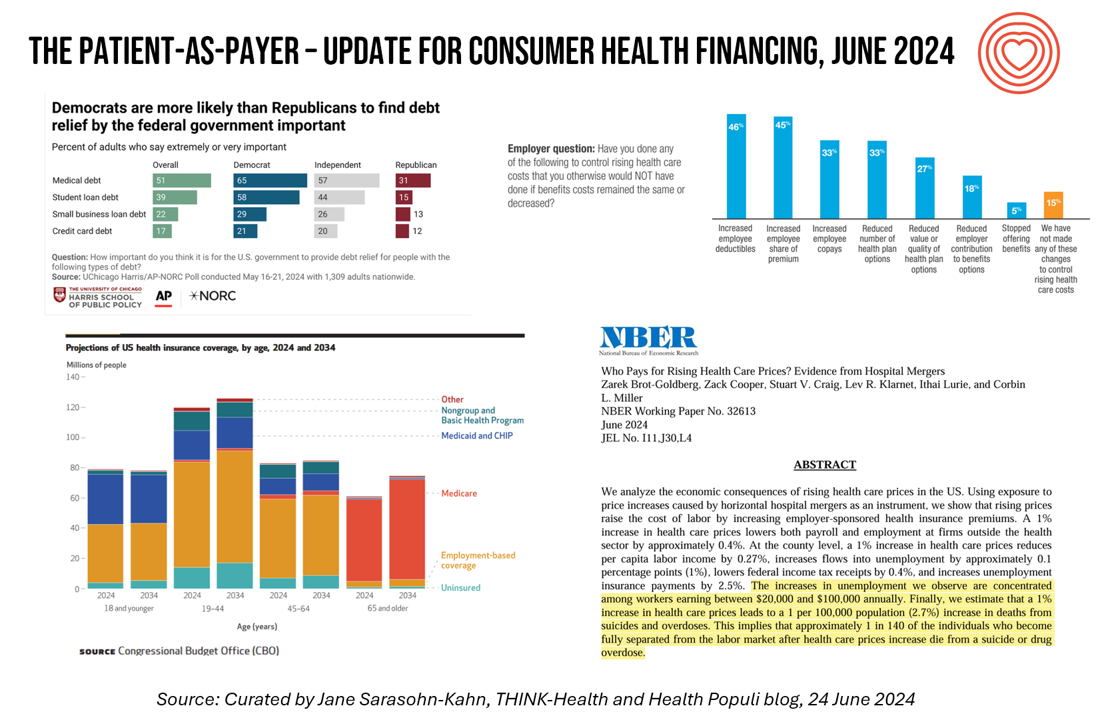
On June 11, Rohit Chopra, the Director of the Consumer Financial Protection Bureau (CFPB) announced the agency’s vision to ban Americans’ medical debt from credit reports. He called out that, “In recent years, however, medical bills became the most common collection item on credit reports. Research from the Consumer Financial Protection Bureau in 2022 showed that medical collections tradelines appeared on 43 million credit reports, and that 58 percent of bills that were in collections and on people’s credit records were medical bills.” Chopra further explained that medical debt on a consumer credit report was quite different than other kinds
Most Americans Follow an Eating Pattern in Search of Energy, Protein, and Well-Being – With Growing Financial Stress: A Food as Medicine Update
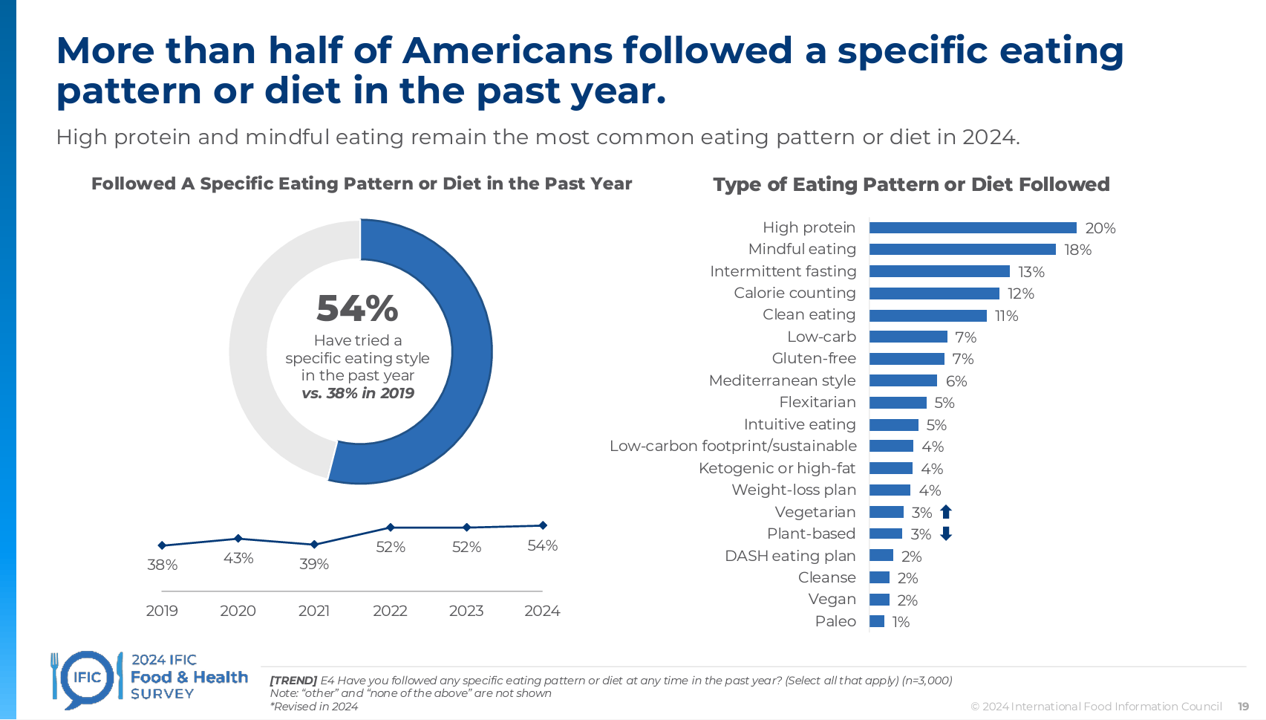
Most Americans follow some kind of eating regime, seeking energy, more protein, and healthy aging, according to the annual 2024 Food & Health Survey published this week by the International Food Information Council (IFIC). But a person’s household finances play a direct role in their ability to balance healthful food purchases and healthy eating, IFIC learned. In this 19th annual fielding of this research, IFIC explored 3,000 U.S. consumers’ perspectives on diet and nutrition, trusted sources for food information, and new insights into peoples’ views on the GLP-1 weight-loss drugs and the growing sense
Most Americans, Both Younger and Older, Worry About the Future of Medicare and Social Security

You would assume that most people over 50 would be worried about the financial future of Medicare to cover health care as those middle-aged Americans age. But a surprising two-thirds of young Americans between 18 and 29, and 7 in 10 between 30 and 39 years of age, are concerned that Medicare’s solvency will worsen leading to their not being able to receive Medicare when eligible to receive it, discovered in the 2024 Healthcare in America Report from West Health and Gallup. This year’s research focused on aging in America, exploring areas of U.S. health care system successes as well
The Most Trusted Brands of 2024 Tell Us A Lot About Health Consumers

From bandages to home hygiene, OTC pain meds and DIY home projects, Morning Consult’s look into the most-trusted brands of 2024 give us insights into health consumers. I’ve been tracking this study since before the public health crisis of the coronavirus, and it always offers us a practical snapshot of the U.S. consumer’s current ethos on trusted companies helping people risk-manage daily living — and of course, find joy and satisfaction as well. In the top 15, we find self-care for health and well-being in many brands and products: we can call out Band-Aid, Dove, Colgate, Kleenex, and Tylenol. For
A 2025 Subaru Forester, a Year at U-New Mexico, or a Health Plan for a Family of Four: the 2024 Milliman Medical Index
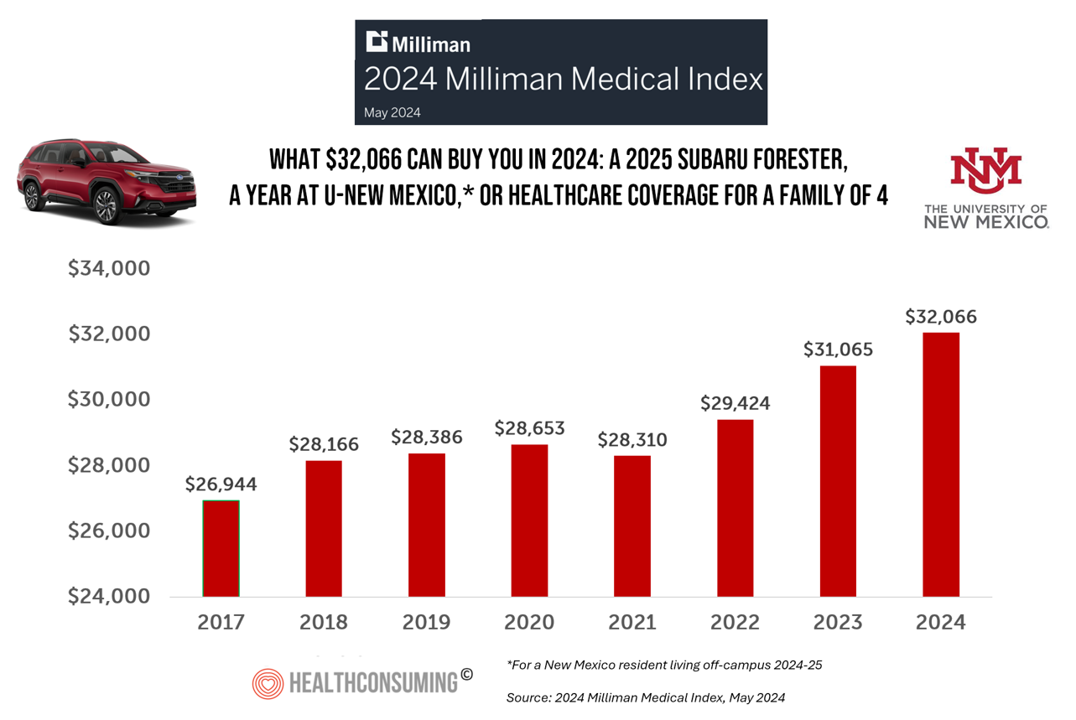
Health care costs for an “average” person covered by an employer-sponsored PPO in the U.S. rose 6.7% between 2023 and 2024, according to the 2024 Milliman Medical Index. Milliman also calculated that the largest driver of cost increase in health care, accounting for nearly one-half of medical cost increases, was pharmacy, the cost of prescription drugs, which grew 13% in the year. The big number this year is $32,066, which is the cost of that employer-sponsored PPO for a family of 4 in 2024. I’ve curated the chart of the MMI statistic for many
The Thematic Roadmap for AHIP 2024: What the Health Insurance Conference Will Cover

Health insurance plans make mainstream media news every week, whether coverage deals with the cost of a plan, the cost of out-of-network care, prior authorizations, or cybersecurity and ransomware attacks, among other front-page issues. This week, AHIP (the acronym for the industry association of America’s Health Insurance Plans) is convening in Las Vegas for its largest annual 2024 meeting. We expect at least 2,400 attendees registered for the meeting, and they’ll not just be representing the health insurance industry itself; folks will attend #AHIP2024 from other industry segments including pharmaceuticals, technology, hospitals and health systems, and the investment and financial services
GLP-1s’ direct and indirect impacts on health care and consumer goods – Jane speaks with Bloomberg BNN
Today, I spoke live with Paul Bagnell, news anchor with Bloomberg BNN, on the topic of the GLP-1 agonists and their impact on health care, industries beyond health and medicine, and consumers. In this post, I’ll share with you some of the plotline for our discussion. Gallup polled U.S. adults in March to gauge their experience with injectable weight loss drugs, the results published earlier this week. The first chart tells us that 6% of people have used these drugs, and 3% were doing so in March. Consumers using the meds were more
Prescriptions Are Up, Health Services Utilization Down, and GLP-1s Are a Major Growth Driver: IQVIA’s 2024 Update
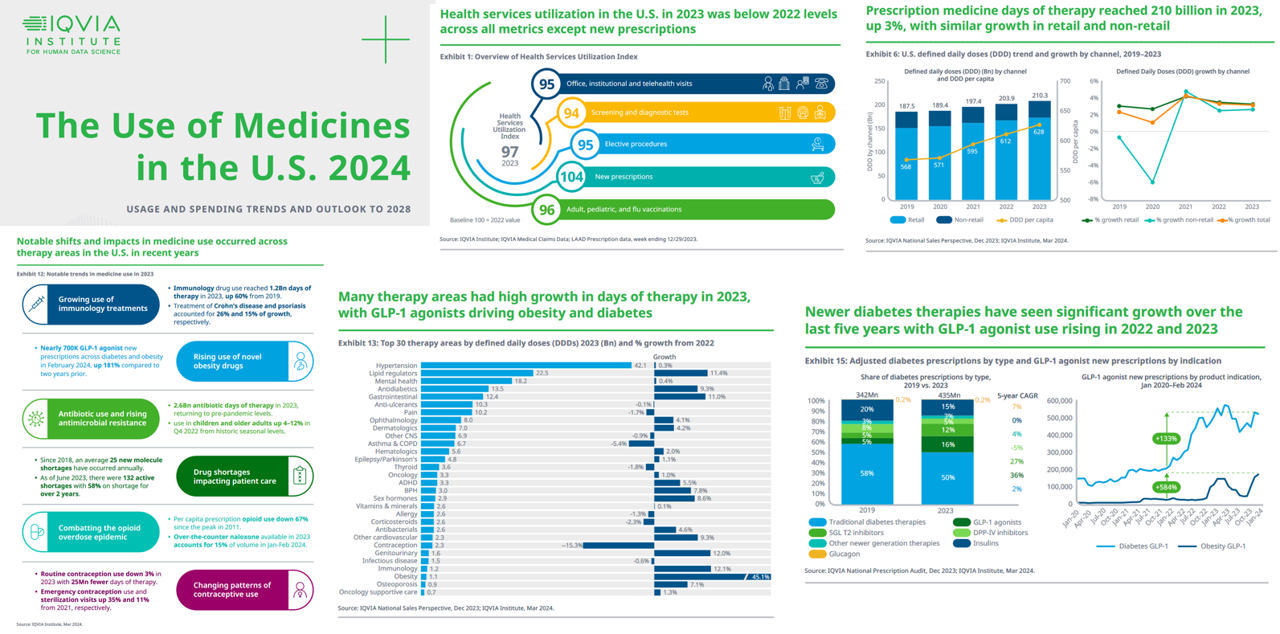
In the past year, the growth of prescription drug utilization and spending has much to do with the use of GLP-1 agonists to treat diabetes and obesity, along with immunology therapy, and lipid meds, along with specialty medicines now accounting for over half of spending — up from 49% in 2018. This update comes from The Use of Medicines in the U.S. 2024 from the IQVIA Institute for Human Data Science. The annual report details trends in health services utilization, the use of prescription drugs, patient financing of those costs, the drivers underpinning the medicines spending, and an outlook to 2028.
Inflation, Health, and the American Consumer – “The Devil Wears Kirkland”
The Wall Street Journal reported yesterday that surging hospital prices are helping to keep inflation high. Hospital costs rose 7.7% last month, the highest increase in 13 years. This chart from WSJ’s reporting illustrates the >2x change in the CPI for hospitals vs the overall rate of price increases. Hospitals are not alone in price cliffs, with health insurance premiums spiking last year at the fastest rate in a decade, the Labor Statistics data showed. “For patients and their employers, the increases have meant higher health-insurance premiums, as well as limiting wage
The Cost of Medical Care, Long-Term Care, and Prescription Drugs Top Older Americans’ Health-Related Concerns – With Social Security and Medicare Top of Mind
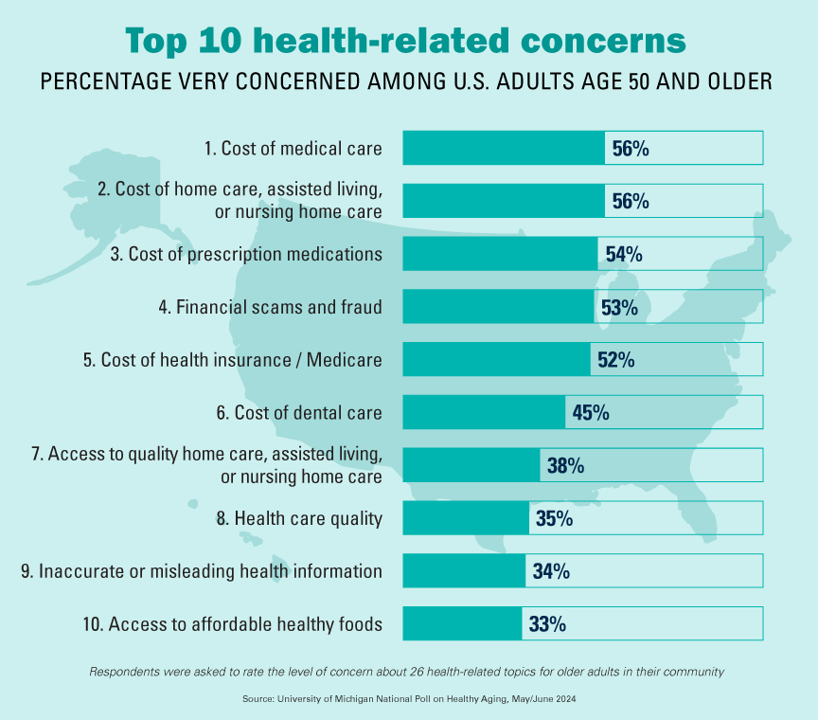
Among Americans 50 years of age and over, the top health-related concerns are Cost, Cost, and Cost — for medical services, for long-term and home care, and for prescription medications. Quality of care ranks lower as a concern versus the financial aspects of health care in America among people 50 years of age and older, as we learn what’s On Their Minds: Older Adults’ Top Health-Related Concerns from the University of Michigan Institute for Healthcare Policy and Innovation. AARP sponsors this study, which is published nearly every month of the year on the Michigan Medicine portal.
Most Americans See Rise of Mental Health Issues, Poorly Treated by the Health System (with a postscript on Walmart Health)
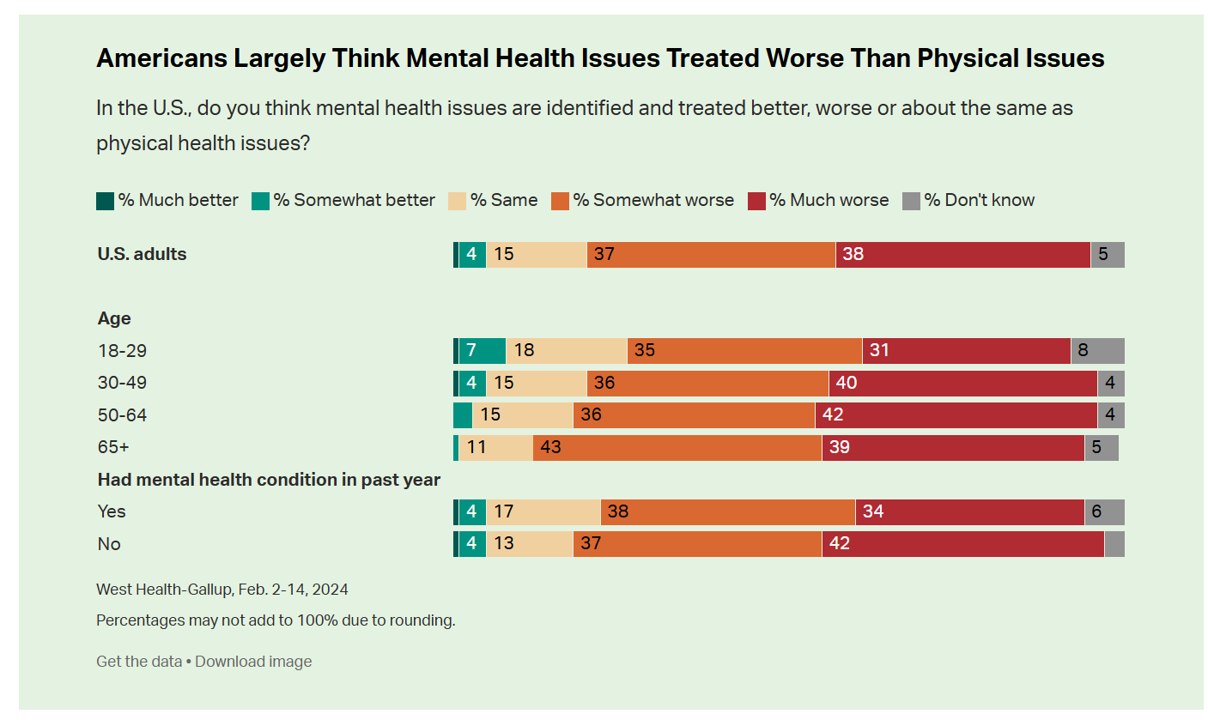
While people in the U.S. perceive a dramatic rise in mental health conditions among fellow health citizens growing over the past five years, people note barriers of cost, insufficient supply of providers, and stigma as barriers to getting care in the latest Gallup and West Health poll on the subject. In West Health’s words, three-quarters of Americans feel that, “mental health takes a back seat to physical health” in the U.S. A key theme of the research found that Americans find that mental health is not treated as well as physical health in
A Tax on Moms’ Financial and Physical Health – The 2024 Women’s Wellness Index
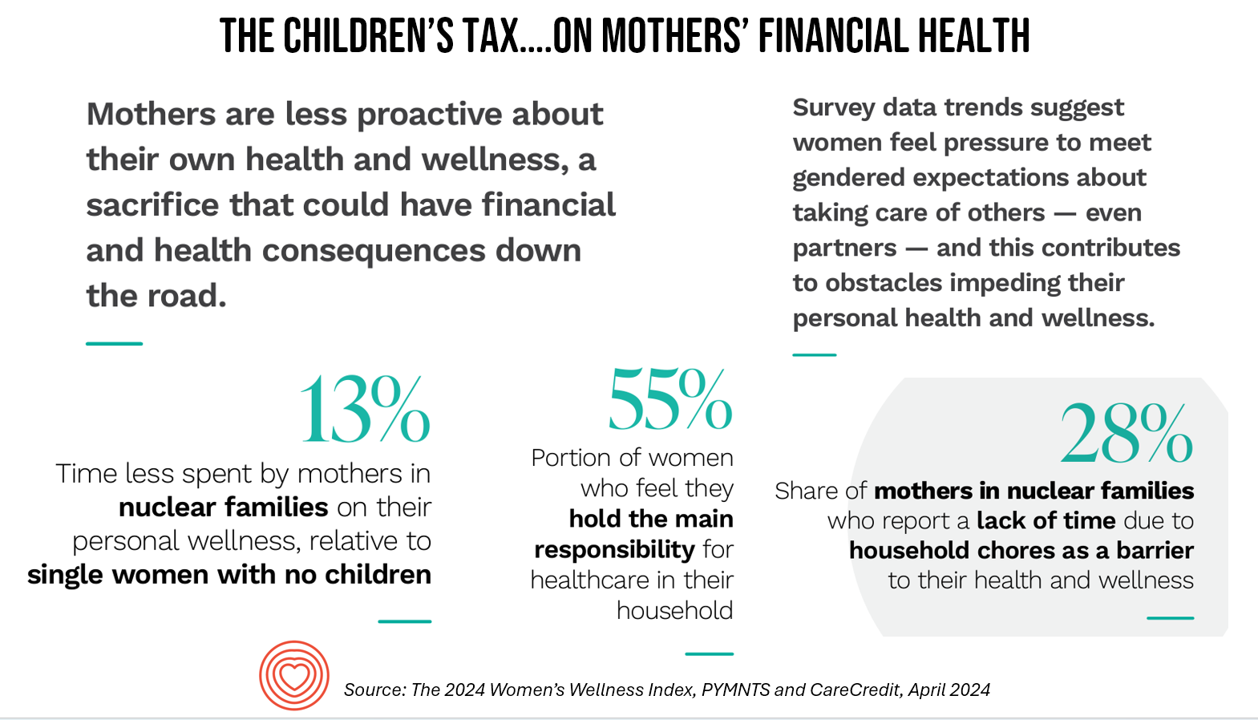
“Motherhood is the exquisite inconvenience of being another person’s everything” is a quote I turn to when I think about my own Mom and the remarkable women in my life raising children. With Mother’s Day soon approaching, the 2024 Women’s Wellness Index reminds us that the act of “being another person’s everything” has its cost. The Index, sponsored by PYMNTS in collaboration with CareCredit, was built on survey responses from 10,045 U.S. consumers fielded in November-December 2023. The study gauged women’s perspectives on finances, family, social life impacts on health and well-being. My key takeaway from
Leveraging Trust, Showing Humility: How Health Care Organizations Can Serve Consumers – A New Read from McKinsey
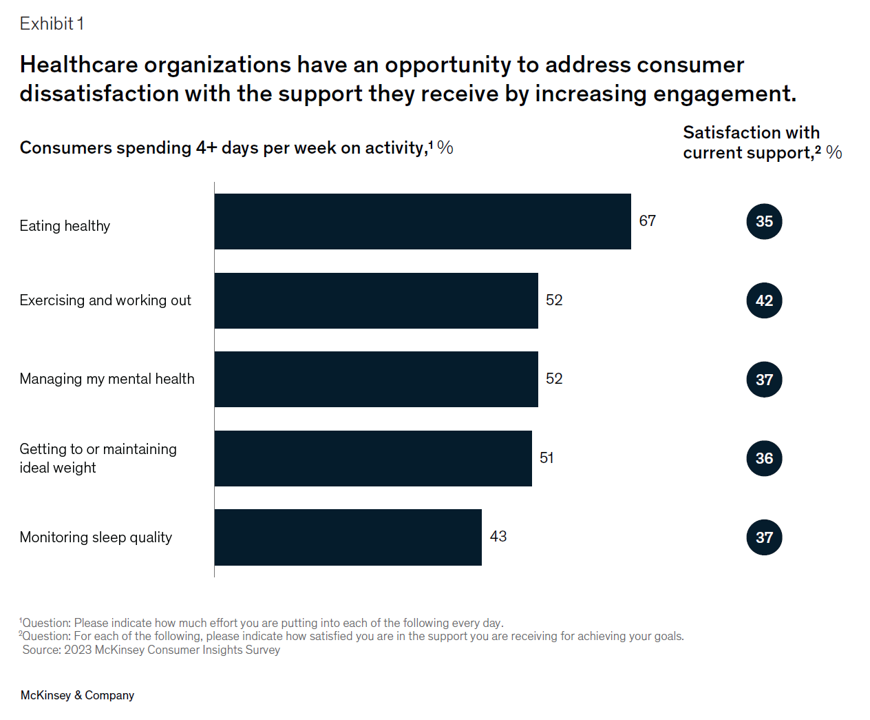
Three trends underpin health consumers’ evolving demands for service: spending more but getting less satisfaction and innovation; trusting health care with data but underwhelmed by the use of that personal information; and, growing “shopping” behavior seeking quality, availability, proximity, cost, and options across channels for health care. That’s the current read from McKinsey & Company’s team noting that Consumers rule: Driving healthcare growth with a consumer-led strategy. In this health consumer update, McKinsey spoke with three consumer marketing experts from other industries to learn best practices on how best to “be there”
Healthcare 2030: Are We Consumers, CEOs, Health Citizens, or Castaways? 4 Scenarios On the Future of Health Care and Who We Are – Part 2
This post follows up Part 1 of a two-part series I’ve prepared in advance of the AHIP 2024 conference where I’ll be brainstorming these scenarios with a panel of folks who know their stuff in technology, health care and hospital systems, retail health, and pharmacy, among other key issues. Now, let’s dive into the four alternative futures built off of our two driving forces we discussed in Part 1. The stories: 4 future health care worlds for 2030 My goal for this post and for the AHIP panel is to brainstorm what the person’s
Considering Equity and Consumer Impacts of GLP-1 Drugs – A UBS Economist Weighs In
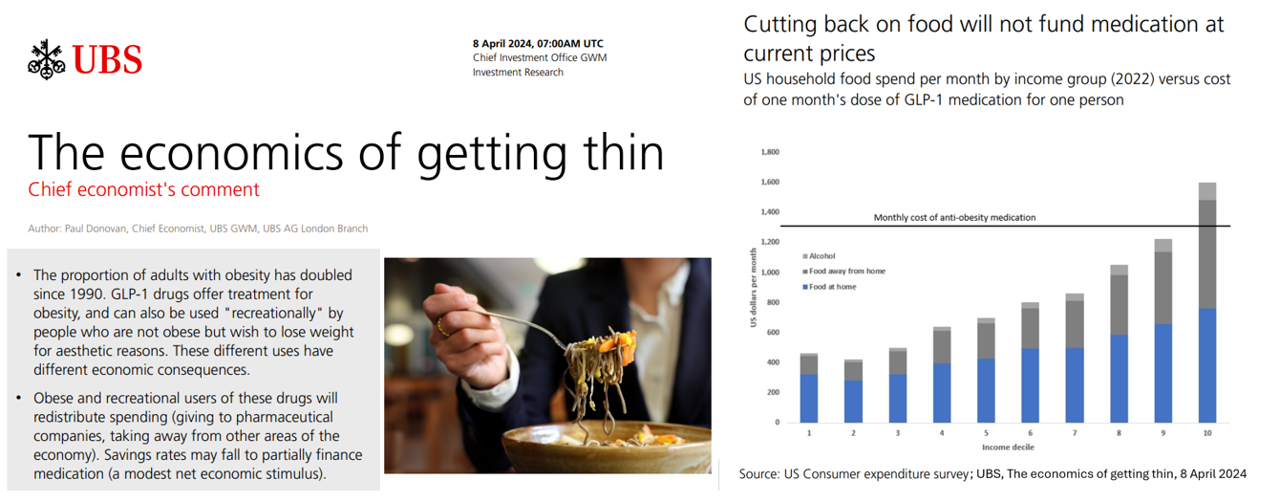
Since the introduction of GLP-1 drugs on the market, their use has split into two categories: for obesity and “recreationally,” according to the Chief Economist with UBS (formerly known as Union Bank of Switzerland). Paul Donovan, said economist, discusses The economics of getting thin in his regularly published comment blog. “These different uses have different economic consequences,” Donovan explains: Obese patients who use GLP-1s should become more productive employees, Donovan expects — less subject to prejudice, and less likely to be absent from work. While so-called recreational GLP-1 consumers may experience these
A Springtime Re-Set for Self-Care, From Fitness to Cozy Cardio: Peloton’s Latest Consumer Research

How many people do you know that don’t know their cholesterol or their BMI, their net worth or IQ, their credit score, astrological sign, or ancestry pie-chart? Chances are fewer and fewer as most people have gained access to medical records and lab test results on patient portals, calorie burns on smartwatches, credit scores via monthly credit card payments online, and completing spit tests from that popularly gifted Ancestry DNA test kits received during the holiday season. Meet “The Guy Who Didn’t Know His Cholesterol” conceived by Roz Chast,
Consumers Are So Over Their Paper Chase in Health Care Payments

As we start the month of April 2024 in the U.S., it’s tax season in America with Federal (and other) income taxes due on the 15th of the month. This is also the time my research clock alarm goes off for an important annual report that describes the latest profile of the patient-as-payer in the U.S. ‘Tis the season for J.P. Morgan’s InstaMed team to analyze health care payments data, describing the experiences of consumers, providers and payers in the Trends in Healthcare Payments Fourteenth Annual Report. The overall takeaway for
The Self-Prescribing Consumer: DIY Comes to Prescriptions via GLP-1s, the OPill, and Dexcom’s CGM

Three major milestones marked March 2024 which compel us to note the growing role of patients-as-consumers — especially for self-prescribing medicines and medical devices. This wave of self-prescribed healthcare is characterized by three innovations: the Opill, GLP-1 receptor agonists, and Dexcom’s Continuous Glucose Monitoring (CGM) system that’s now available without a prescription. Together, these products reflect a shift in health care empowerment toward patients as consumers with greater autonomy over their health care when the products and services are accessible, affordable, and designed with the end-user central to the value proposition and care flows. Let’s take a look at each
Peering Into the Hidden Lives of Patients: a Manifesto from Paytient and Nonfiction

Having health insurance in America is no guarantee of actually receiving health care. It’s a case of having health insurance as “necessary but not sufficient,” as the cost of deductibles, out-of-pocket coinsurance sharing, and delaying care paint the picture of The Hidden Lives of Workplace-Insured Americans. That’s the title of a new report that captures the results of a survey conducted in January 2024 among 1,516 employed Americans who received employer-sponsored health insurance. The study was commissioned by Paytient, a health care financial services company, engaging the research firm Nonfiction to conduct the study
The Economic Contours of the Change Healthcare Cyber Attack: Taking Stock So Far

On February 22, 2024, I went to a CVS Pharmacy-Inside-Target in my community to fill a prescription for benzonatate 200 mg capsules. I had caught a bad case of the flu the week before, and subsequently suffered a very long tail of a cough. That’s TMI for me to write about in the Health Populi blog, but this story has a current-events twist: the pharmacist could not electronically link with my insurance company to transact my payment. He tried a few work-flows, and ended up using a discount card which in the moment worked for us, and I paid the
The Women’s Health Gap Is Especially Wide During Her Working Years – Learning from McKinsey, the World Economic Forum, and AARP in Women’s History Month
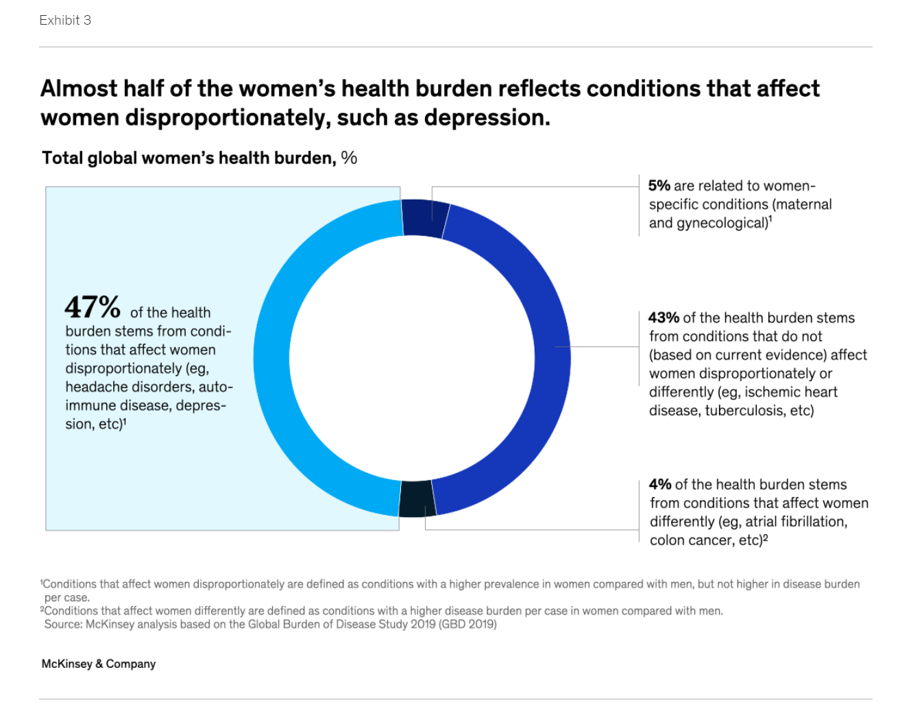
There’s a gender-health gap that hits women particularly hard when she is of working age — negatively impacting her own physical and financial health, along with that of the community and nation in which she lives. March being Women’s History Month, we’ve got a treasure-trove of reports to review — including several focusing on health. I’ll dive into two for this post, to focus in on the women’s health gap that’s especially wide during her working years. The reports cover research from the McKinsey Health Institute collaborating with the World Economic Forum on
A Health Consumer Bill of Rights: Assuring Affordability, Access, Autonomy, and Equity

Let’s put “health” back into the U.S. health care system. That’s the mantra coming out of this week’s annual Capitol Conference convened by the National Association of Benefits and Insurance Professionals (NABIP). (FYI you might know of NABIP by its former acronym, NAHU, the National Association of Health Underwriters). NABIP, whose members represent professionals in the health insurance benefits industry, drafted and adopted a new American Healthcare Consumer Bill of Rights launched at the meeting. While the digital health stakeholder community is convening this week at VIVE in Los Angeles to share innovations in health tech, NABIP
Americans Come Together in Worries About Medical Bills, the Cost of Health Care, and Prescription Drug Costs
In the U.S., national news media, Federal statistics, dozens of business leaders and the Federal Reserve Bank have been talking about an historically positive American economy on a macro level. But among individual residents of the U.S., there is still a negative feeling about the economy in a personal context, revealed in the Kaiser Family Foundation Health Tracking Poll for February 2024. I’ve selected three figures of data from the KFF’s Poll which make the point that in peoples’ negative feelings about the national economy, their personal feelings about medical costs rank high
People With Medical Debt Are Much More Likely to Be in Financial Distress in America
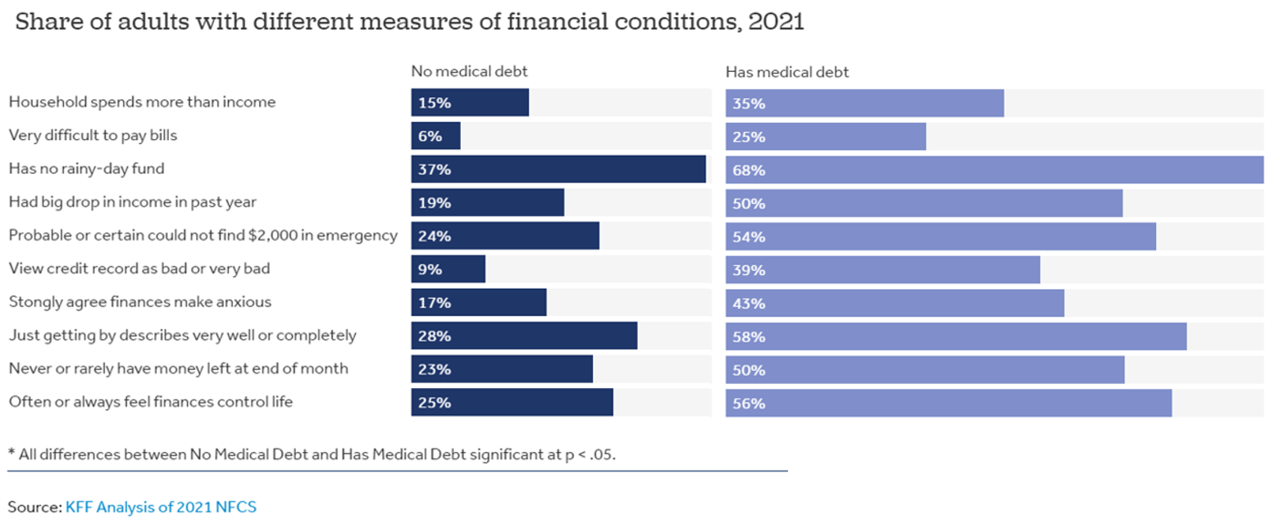
How financially vulnerable are people with medical debt in the U.S.? Significantly more, statistically speaking, we learn from the latest survey data revealed by the National Financial Capabilities Study (NFCS) from the FINRA Foundation. The Kaiser Family Foundation and Peterson Center on Healthcare analyzed the NFCS data through a consumer health care financial lens with a focus on medical debt. Financial distress takes many forms, the first chart inventories. People with medical debt were most likely lack saving for a “rainy day” fund, feel they’re “just getting by” financially, feel their finances control their life, and
The Wellness Market Shaped by Health at Home, Wearable Tech, and Clinical Evidence – Thinking McKinsey and Target

Target announced that the retail chain would grow its aisles of wellness-oriented products by at least 1,000 SKUs. The products will span the store’s large footprint, going beyond health and beauty reaching into fashion, food, home hygiene and fitness. The title of the company’s press release about the program also included the fact that many of the products would be priced as low as $1.99. So financial wellness is also baked into the Target strategy. Globally, the wellness market is valued at a whopping $1.8 trillion according to a report published last week by McKinsey. McKinsey points to five trends
The Trust-Innovation Gap – Welcome to the 2024 Edelman Trust Barometer

If it’s January, it’s Davos-time — that is the annual meeting of the World Economic Forum convening global experts and passionistas focused on big ideas and challenges facing us mere humans living on Planet Earth. Parallel with the WEF is the annual publication of the 2024 Edelman Trust Barometer, now in its 24th year, focusing on global citizens’ concerns that unite people around the world. For the 2024 study, Edelman’s team fielded the survey in November 2023, collecting input from over 32,000 people living in 28 countries. About 1,150 interviews (plus or minus) were done in each nation which included
Access to Technology Is the New Pillar for Well-Being: CES & the UN Partner for Human Security for All

In kicking off #CES2024, CTA’s researchers noted the acceleration of global connectivity, with gaps in peoples’ ability to connect depending where they live: by region, the percent of people connected to the internet today are, according to CTA’s data, 92% in the U.S. 87% in the E.U. 76% in Latin America 73% in China 55% in Nigeria 46% in India. Such gaps in connectivity threaten peoples’ individual well-being, but also social and political stability that impacts the entire world’s security. And not to overlook, as well, the promise of AI to do good at scale at the enterprise-level, globally.
The Health Consumer in 2024 – The Health Populi TrendCast
At the end of each year since I launched the Health Populi blog, I have put my best forecasting hat on to focus on the next year in health and health care. For this round, I’m firmly focused on the key noun in health care, which is the patient – as consumer, as Chief Health Officer of the family, as caregiver, as health citizen. As my brain does when mashing up dozens of data points for a “trendcast” such as this, I’ll start with big picture/macro on the economy to the microeconomics of health care in the family and household,
An Extraordinary Life and Voice: A Call-to-Action from Casey Quinlan, featured in the Journal of Participatory Medicine

It is about time that a healthcare journal features examples of patient-leaders who have pioneered activism, innovation, and The first exemplar in this vein is Casey Quinlan, whom we lost all-too-soon earlier this year on 24th August. A team of her appreciative colleagues and friends wrote up the first in a new series called “Extraordinary Lives” published in the Journal of Participatory Medicine (JPM) titled “An Extraordinary Voice Expressed Through Humor: A Tribute to Casey Quinlan.” I played a minor role in getting this essay to the finish line, and am grateful to have had the opportunity to do so
In 2024 U.S. Consumers Will Mash Financial Resolutions With Those For Physical Health and Mental Health, Fidelity Finds

One-third of U.S. consumers feel in worse financial shape now than in 2022, with inflation a top concern, discovered in the 2024 New Year’s Financial Resolutions Study from Fidelity Investments. In this 15th annual update of Fidelity’s research into Americans’ New Year’s resolutions for financial health, we learn the mantra that 2024 will be the year of living practically, opening new chapters for saving and paying down debt. Fidelity conducted an online poll among 3,002 U.S. adults 18 and over in October 2023 to gauge peoples’ perspectives on personal finances, and well-being currently and into 2024. This
Inflation and the cost of health care top U.S. voters’ issues for 2024 elections
The cost of living ranks top in U.S. voters’ minds among many issues Americans are feeling and following in late 2023. A close second in line is affordability of health care, as consumers’ household budgets must make room for paying medical bills — with prescription drug costs also very important as a discussion topic for 2024 Presidential candidates, we learn from the latest KFF Health Tracking Poll published 1 December. The monthly study focused on U.S. voters’ top issues and perspectives on the health system and care approaching the new year of 2024. KFF fielded the study among 1,301 U.S.
The Consumerization of AI in Healthcare – The Early Days of AI-Trust
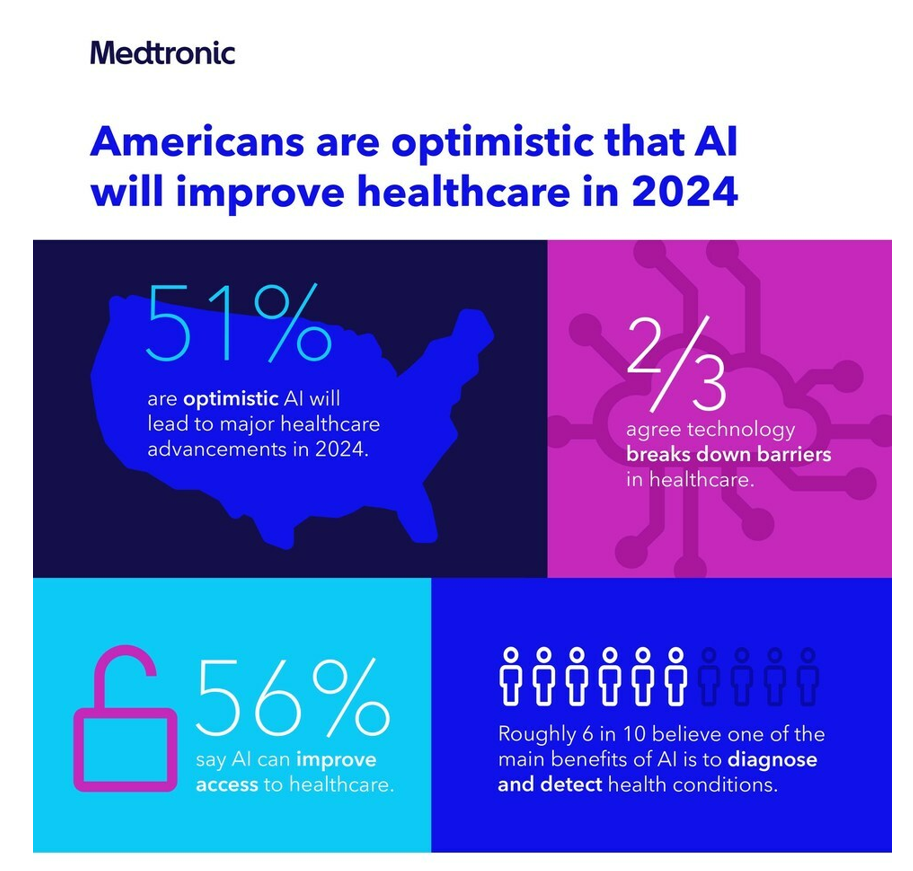
Most people in the U.S. are bullish on the role AI will play in health care in 2024, especially to lower access barriers to care and to diagnose and detect health conditions. Two new studies point to the consumerization of AI in healthcare, from Medtronic and Deloitte. This post weaves their findings together and suggests some planning points for 2024. Medtronic collaborated with Morning Consult to poll 2,213 U.S. adults in late September 2023 to gauge peoples’ perspectives on AI and health care. With such optimism among health consumers comes some
Healthcare Bills, Affordability, and Self-Rationing Care Will Continue to Challenge U.S. Health Consumers in 2024
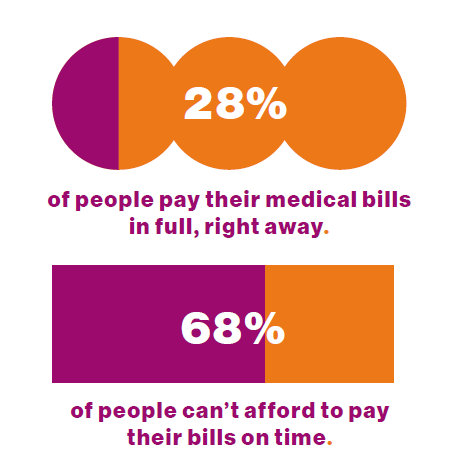
Two-thirds of U.S. consumers say they can’t afford to pay their medical bills on-time, based on the 2023 Consumer Survey from Access One, a financial services company focused on healthcare payments. The report’s title page asks the question, “What options do consumers really want for paying healthcare expenses?” The survey report responds to that question, finding out that nearly one-half of patients have taken some kind of action to reduce their medical expenses. Furthermore, one-third of consumers are not confident they could pay a medical bill of $500 or more. Access One fielded
“My Doctor’s Office” Should Accept Wearable Tech Health Data, Most Patients Say

“Do personal health trackers belong in the doctor’s office?” Software Advice wondered. “Yes,” the company’s latest consumer survey found, details of which are discussed in a report published on their website. Unique to this study is the patient sample polled: Software Advice surveyed 876 patients in September 2023 to gauge their perspectives on wearable tech and health. Note that the patient sample was limited to consumers who had seen a health care provider in the past two years and who also owned and used a personal wearable health device such as an Apple Watch or Fitbit. Thus, the responses shared
How Ahold-Delhaize Connects the Grocery, Climate Change, ESG and Consumers’ Health

In the food sector, “the opportunity for us and the role that we play is to connect climate and health,” Daniella Vega of Ahold Delhaize told Valerio Baselli during the Morningstar Sustainable Investing Summit 2023. In a conversation discussing the importance of non-financial metrics in companies’ ESG efforts, Vega connected the dots between climate change, retail grocery, and consumers’ health and well-being. Vega is the Global Senior Vice President, Health & Sustainability, with Ahold Delhaize— one of the largest food retail companies in the world. Based in the Netherlands, the company operates mainly in
Money and Mental Health in the U.S. – How Difficulty Paying Medical Bills Can Hurt Healing and Well-Being

There is growing evidence on the connection between people’s financial health and their mental health, explored and explained in Understanding the Mental-Financial Health Connection, a study published by the Financial Health Network. Keep that relationship in mind in the context of a new forecast from Kaiser Family Foundation estimate the 2023 cost for employer-sponsored insurance for a family to reach nearly $24,000 in 2023. That cost is a 7% increase over last year, and is expected to be split with companies covering $17K (about 70%) and employees about $6600 (roughly 30%). KFF heard that
Health Care Finance Leaders Look to Cut Costs and Improve Patients’ Financial Experience — Think AI and Venmo
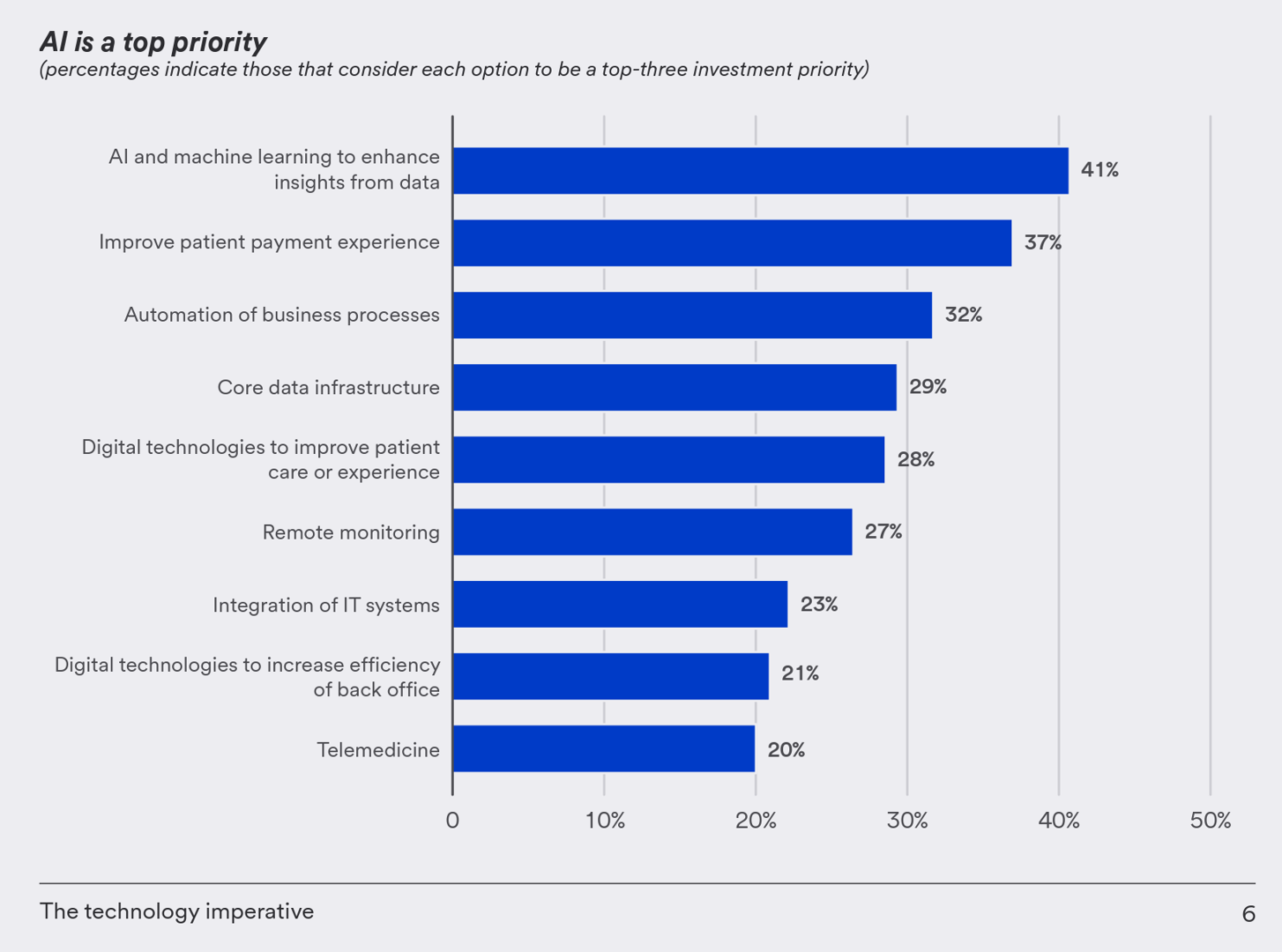
One half-of health care financial leaders plan to invest in technology to cut costs — and most believe that AI has the potential to re-define the entire finance function as they look to Leading the transformation, a study conducted by U.S. Bank among U.S. health finance leaders thinking about emerging technologies. U.S. Bank fielded a survey among 200 senior health care financial leaders in the U.S., 30% of whom were group CFOs, 20% regional/divisional CFOs, 25% senior managers, and the remaining various flavors of financial managers. All respondents were responsible for at least $100
Food-As-Medicine Grows Its Cred Across the Health/Care and Retail Ecosystem
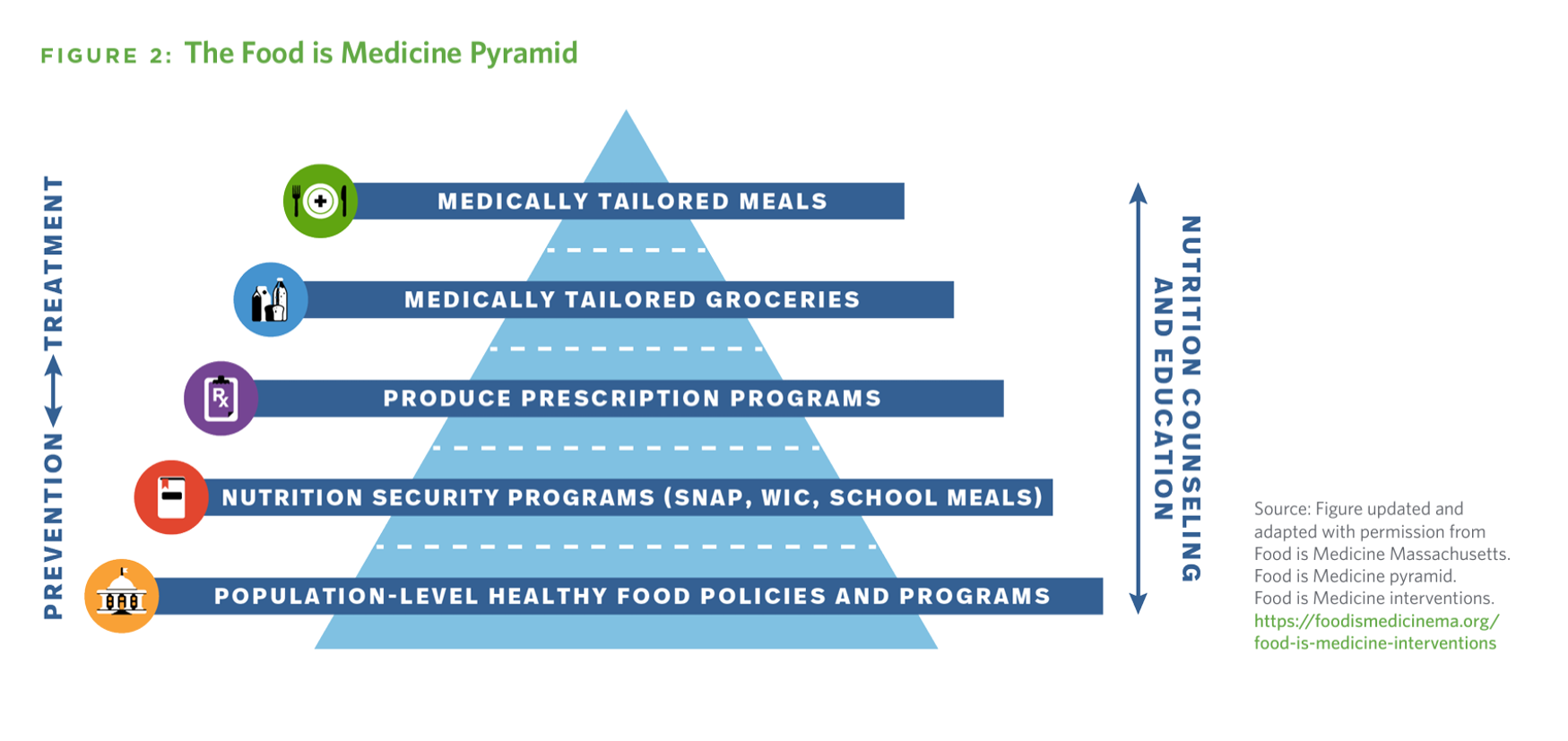
In the nation’s search for spending smarter on health care, the U.S. could save at least $13 billion a year through deploying medically-tailored meals for people enrolled in Medicare, Medicaid, and private insurance programs, according to the True Cost of Food, research published by the Tufts School of Nutrition Science and Policy collaborating with The Rockefeller Foundation. It’s been one year since the White House convened the Conference on Hunger, Nutrition, and Health, kicking off the Biden Administration’s national strategy to improve health citizens’ access to healthy food as a matter of public health and economic security.
The 2023 Health Economy – The Evolving Primary Care and Retail Health Convergence Through Trilliant Health’s Lens
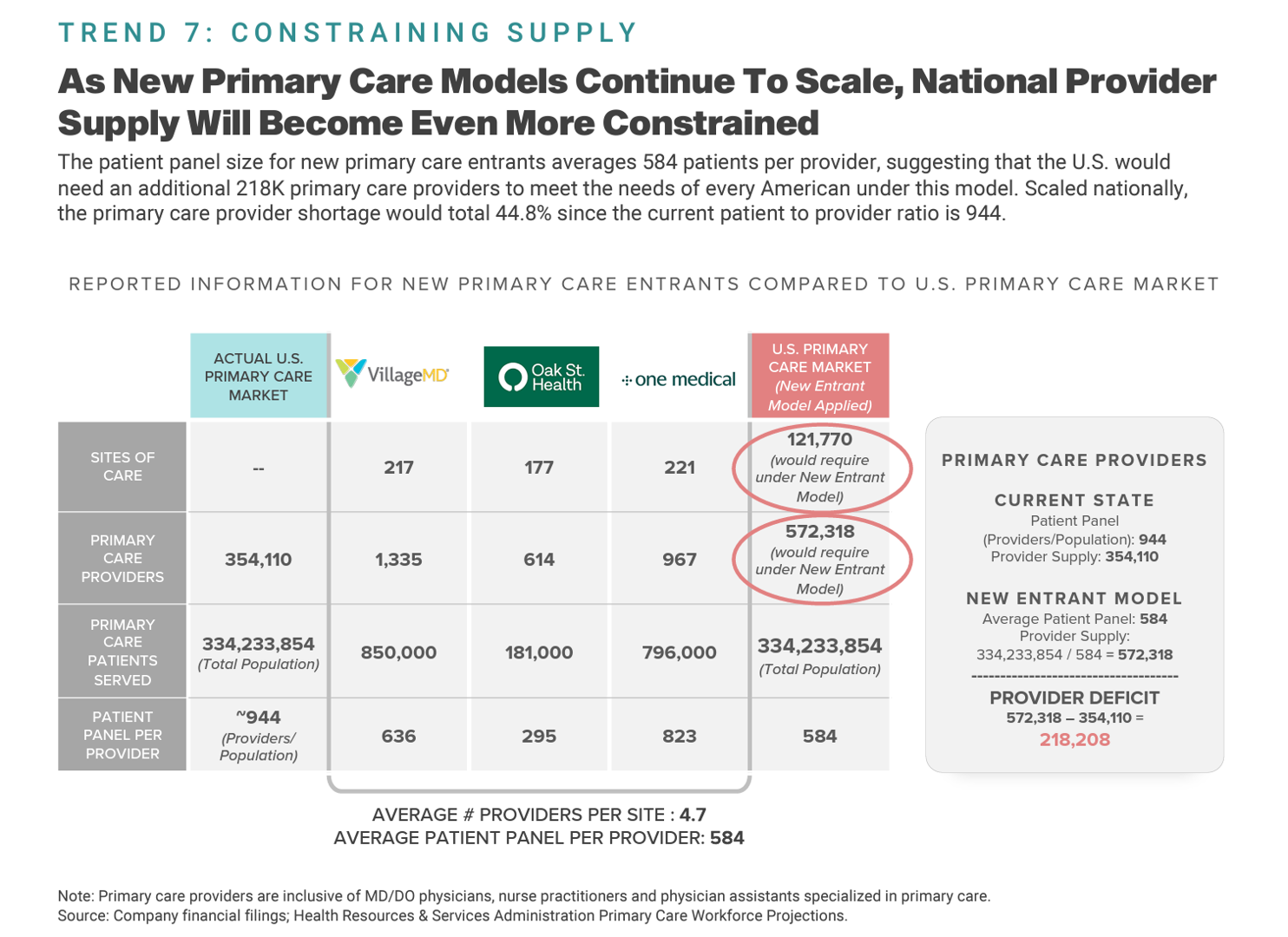
In U.S. health care’s negative-sum game, stakeholders who survive and win that game will have to deliver value-for-money, we learn from Trilliant Health’s 2023 Trends Shaping the Health Economy Report. “Report” is one word for this nearly 150-page compendium of health care data that is an encyclopedic treasure trove for health service researchers, marketers, strategists, journalists, and those keen to explore questions about the current state of health care in America. As Sanjula Jain points out in the Report’s press release, the publication resembles another huge report many of us appreciated for
The Healthcare Financial Experience is a Stressful One: the Convergence of our Medical, Retail, and Financial Lives

One in two consumers in the U.S. feel their well-being or healing was negatively impacted by difficulty paying for their medical care. Welcome to the convergence of patients’ health care life with financial and retail lives, we learn from the 2024 Healthcare Financial Experience Study from Cedar. And that patient’s positive clinical experience can absolutely reverse the consumer’s perception of the provider, noted by this quote from OSU’s Chief Financial Officer Vincent Tammaro: “We’ve cured you of your ailment, but we’ve harmed you financially.” That’s a form of financial toxicity that
Slip Slidin’ Away: the Reputations of Pharma and Healthcare in the U.S. Decline in the Latest Gallup Poll
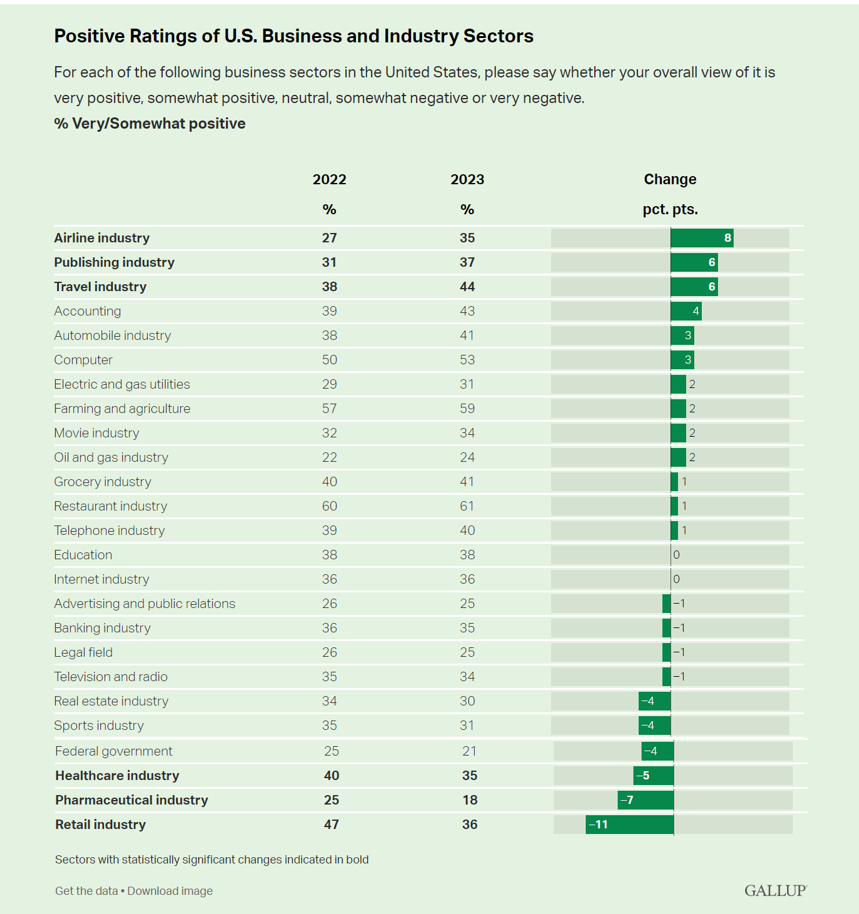
Oh, how quickly people forget…and slow to forgive. U.S. consumers’ positive views for healthcare, pharma and retail have significantly fallen in just one year, the latest annual Gallup poll of industry rankings in America found as of August 2023. This stat for the pharma industry was the lowest Gallup ever recorded for the sector since 2001. I can’t help hearing Paul Simon’s lyrics to Slip Slidin’ Away….”you know the nearer your destination, the more you’re slip slidin’ away” when it comes to health citizens’ perceptions of pharma and the healthcare
“Healthcare Isn’t Healthy:” the Global Challenge of Health Equity, and Calls-to-Action
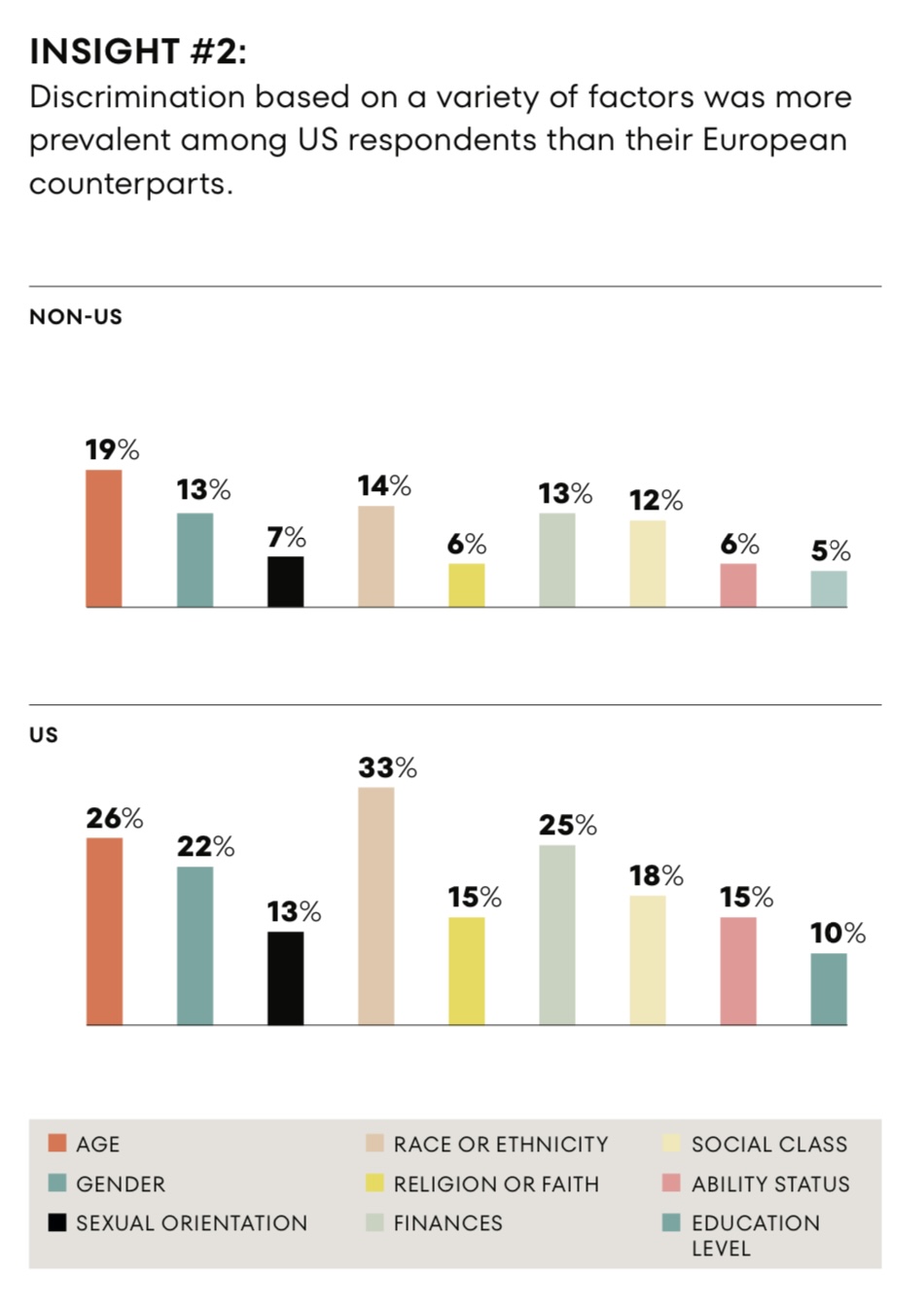
Discrimination in health care is reported by more people in the U.S. than in Germany, Spain, or the U.K., we learn in the research reported in The Intersection of Health Equity in Communities & Business Strategy: A Call-to-Action, from Omnicomm PR Group (OPRG) and Atlantic Insights. The study was conducted among 6,000 people living in Germany, Spain, the United Kingdom and the United States, fielding 1,500 interviews in each of the four countries in March 2023. The U.S. survey sample included 375 people identifying as Black, White, Hispanic, or
The Clinician of the Future: A Partner for Health, Access, Collaboration, and Tech-Savviness

One-half of clinicians working in the U.S., doctors and nurses alike, are considering leaving their current role in the next two to three years. That 1 in 2 clinicians is significantly greater than the global 37% of physicians and nurses thinking about leaving their roles in the next 3 years, according to the report Clinician of the Future 2023 from Elsevier. Elsevier first conducted research among doctors and nurses for the Clinician of the Future report in 2022, following up this year’s survey research online among 2,607 clinicians working around the world: Elsevier polled
For Public Health, U.S. Consumers See Opioids, Obesity, and Guns Top 3 Public Health Threats – But Lowering Healthcare & Drug Costs is Job 1 for Government
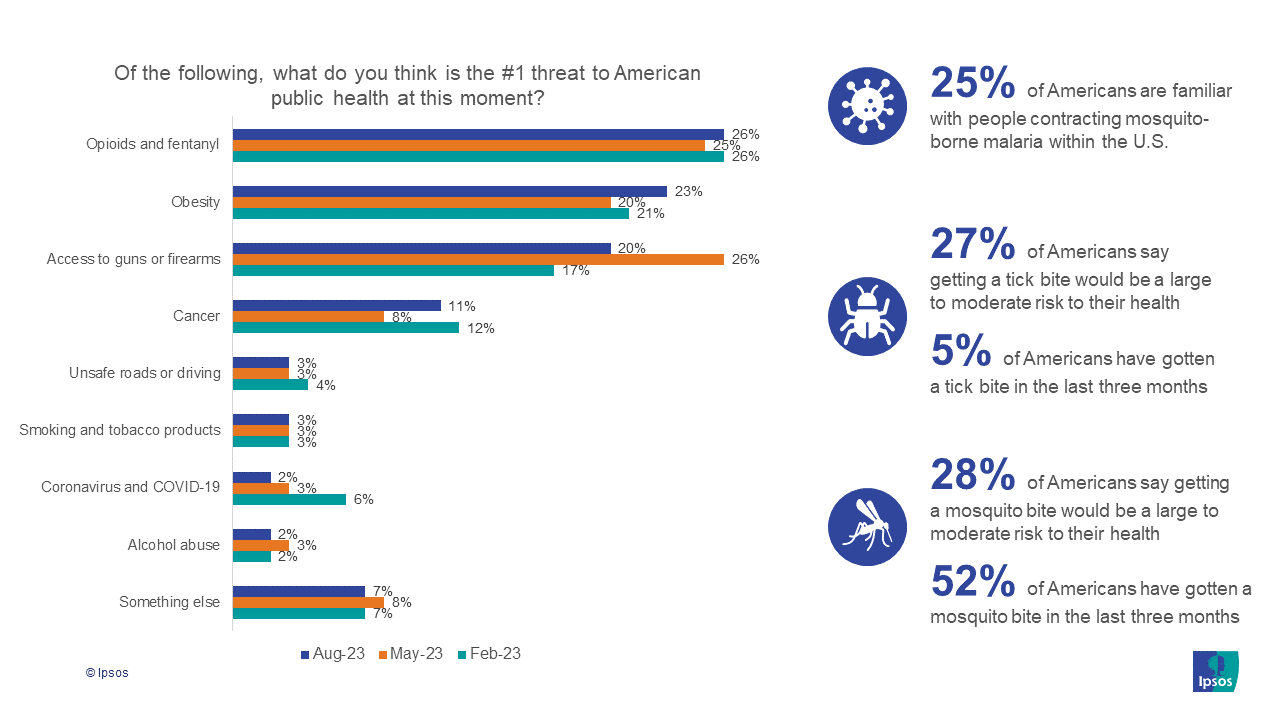
Americans cite opioids and fentanyl, obesity, and access to guns and firearms as the top three public health challenges this summer of 2023, according to the new Axios/Ipsos American Health Index. As for government priorities dealing with public health, though, U.S. health citizens say the top priority should be lowering the costs of health care and prescription drugs. Once again, we see evidence that U.S. consumers bundle their financial wellbeing — in this instance, costs of medical services and medicines — into peoples’ overall sense of health for themselves as individuals and for
Personalizing Health Means Personalizing Health Insurance for Patient-Members – Learning from HealthEdge

As patients assume more financial skin in their personal healthcare, they take on the role of demanding consumer, or “impatient patients.” HealthEdge’s latest research into health consumers’ perspectives finds peoples’ satisfaction with their health insurance plans lacking, with members seeking easier access their personal health information, high levels of service, and rewards for healthy behaviors. Health plans would also boost consumers’ satisfaction by channeling patients’ access to the kinds of medical providers that align with consumers’ preferences and personal values, and by personalizing information to steer people toward lower-cost care.
Pharmacy Plays a Growing Role in Consumers’ Health@Retail – J.D. Power’s 2023 Rankings
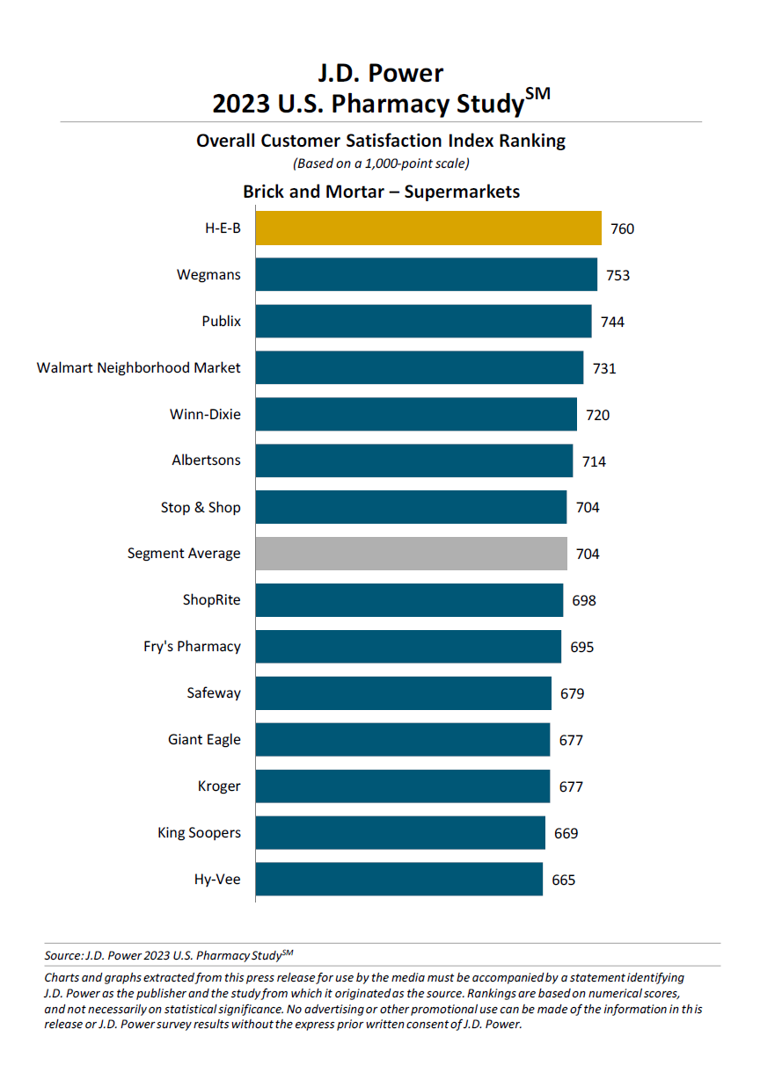
“Brick-and-mortar pharmacies forge meaningful connections with customers” through conversations between pharmacists and patients, “on a first-name basis.” This quote comes from Christopher Lis, managing director of global healthcare intelligence at J.D. Power who released the company’s annual 2023 U.S. Pharmacy Study today, the 15th year the research has been conducted. Each year, J.D. Power gauges U.S. consumers’ views on retail pharmacies in four channels: brick and mortar chain drug stores, brick and mortar mass merchandisers, brick and mortar supermarkets, and mail order. Across all four channels, the
Cost Trumps Quality of Health Care for Consumers As Their Experience Has Eroded
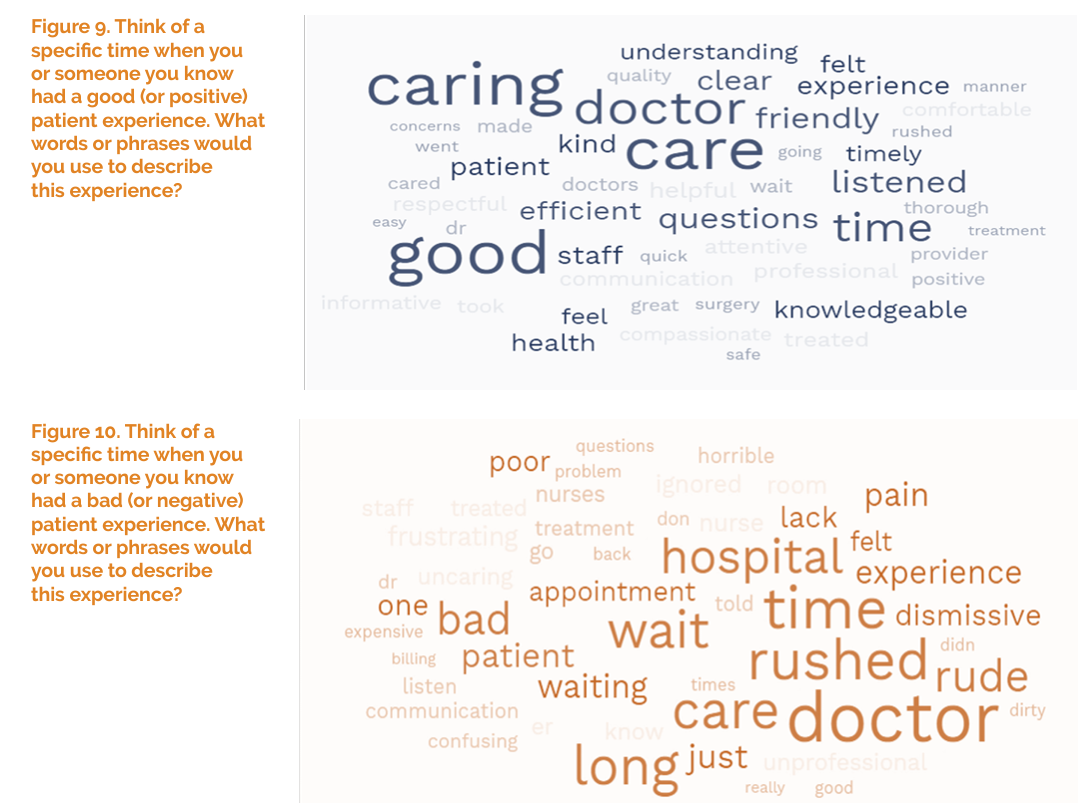
Patients’ perceptions of health care quality and experience have fallen in the three years since 2020, based on a July 2023 update from The Beryl Institute – Ipsos Px Pulse study. Start with health care quality, which 58% of U.S. adult patients ranked as “very good or good” in June 2020. The percent of health consumers evaluating their healthcare quality as very good or good fell to 41% of people in June 2023, an erosion of 17 percentage points, shown in the first chart. Next, consider patients’ ratings on their care experience,
GNC Offers “Free Healthcare” — Telehealth, Generic Meds, and Loyalty in the Retail Health Ecosystem

The retail health landscape continues to grow, now with GNC Health offering a new program featuring telehealth and “curated set” of 40+ generic prescription drugs commonly used in urgent care settings. The services are available to members of GNC’s new-and-improved loyalty program, GNC PRO Access, which is priced at a fixed fee of $39.99 for one year’s membership. This is available to consumers 18 years of age and older. “As a trusted brand in the health and wellness space, we are thrilled to expand our efforts in helping our customers Live Well by offering
Patients, Nurses and Doctors Blame Health Insurers for Increasing Costs and Barriers to Care
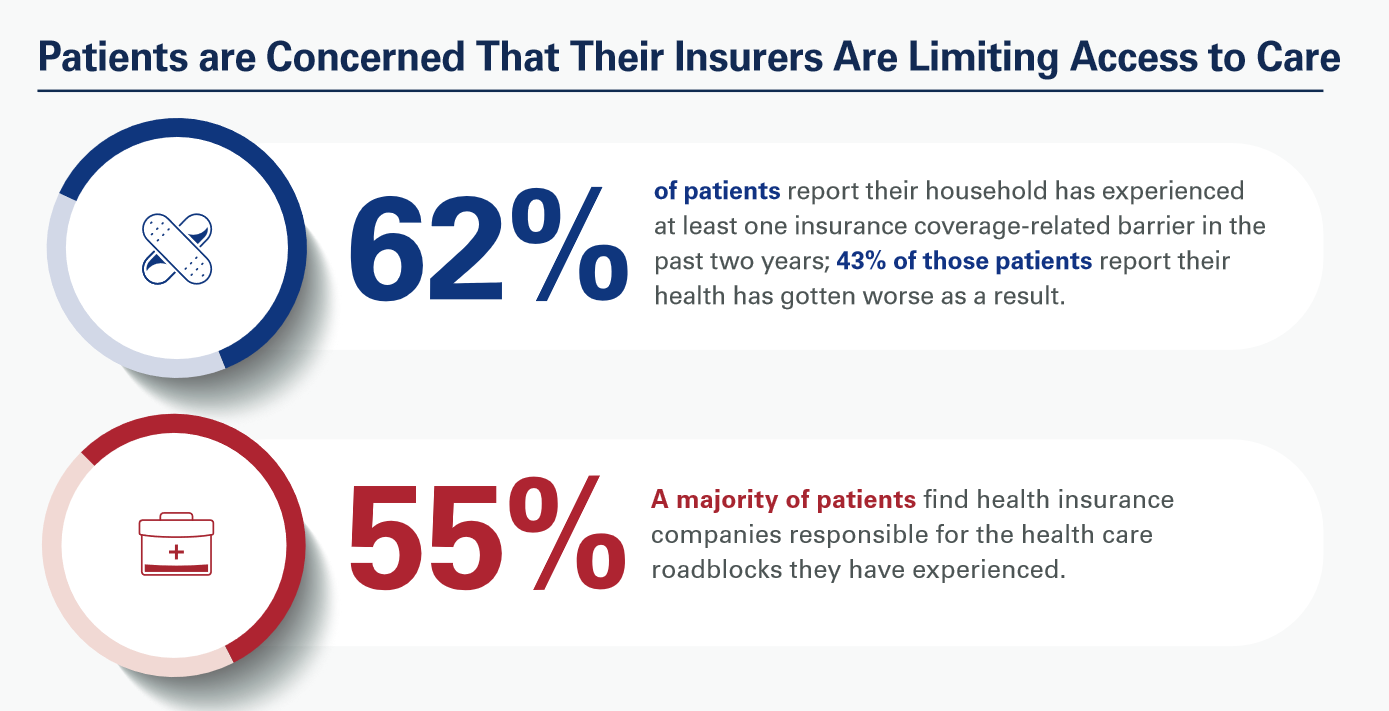
Most patients, nurses and doctors believe that health insurance plans reduce access to health care which contributes to clinician burnout and increases costs, based on three surveys conducted by Morning Consult for the American Hospital Association (AHA). Most patients have experienced at least one health insurance related barrier in the past two years, and 4 in 10 of those people said their health got worse as a result of that care-barrier. “These surveys bear out what we’ve heard for years — certain insurance companies’ policies and practices are reducing health care access and making
Happy 75th Birthday, NHS – Through A U.S. Health Care Lens

The UK’s National Health Service (NHS) turns 75 today. The NHS was the brainchild of Minister of Health Aneurin Bevan; he wrote in a statement to doctors and nurses in The Lancet on July 3, 1948, “My job is to give you all the facilities, resources, apparatus and help I can, and then to leave you alone as professional men and women to use your skill and judgement without hindrance.” This week in The Lancet, the editors assert, “The founding principles of the NHS put into practice 75 years ago are at risk of
The Cost of Treating Patients is On the Rise: PwC Goes What’s Behind the 2024 Medical Spending Numbers

Health care cost trend will spike up another percentage point to 7.0% in 2024, according to the annual report from the PwC Health Research Institute, Medical cost trend: Behind the numbers 2024. Every year, the PwC HRI team goes behind those numbers to assess cost inflators and deflators which underpin annual medical inflation. As the first line chart illustrates, the peak of medical trend in the last 18 years was in 2007 when the U.S. saw double-digit cost growth of nearly 12%. Here’s a link to PwC’s 2007 study looking behind the
The Latest KFF Poll on Consumer Experiences with Health Insurance Speaks Volumes About Patients’ Administrative Burden
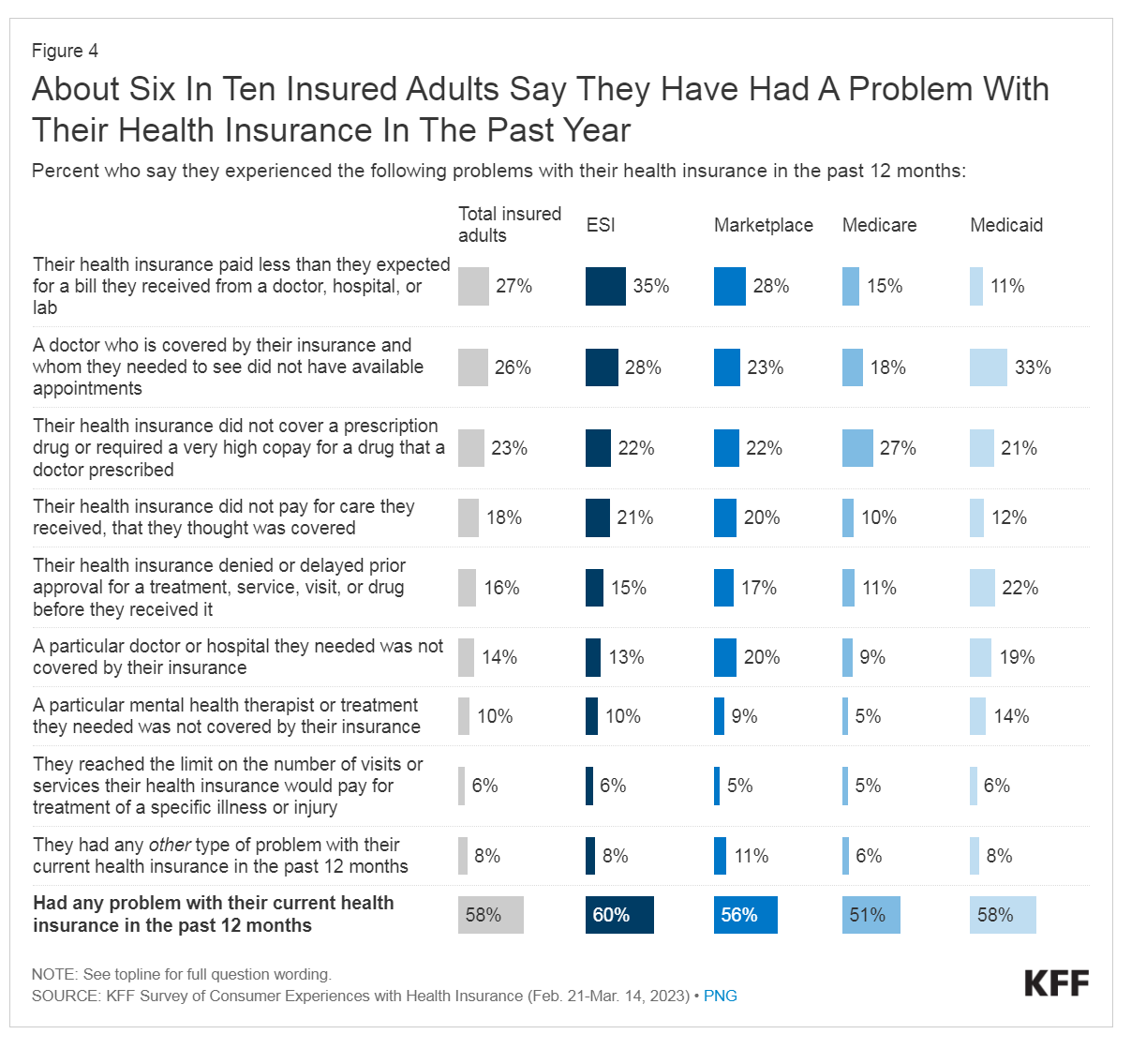
People love being health-insured, but their negative experiences with health plans create serious burdens on patients-as-consumers. And those burdens impact even more people who are unwell than healthier folks. The 2023 Kaiser Family Foundation Survey of Consumer Experiences with Health Insurance updates our understanding of and empathy for insured peoples’ Patient Administrative Burdens (PAB). For this study, KFF polled 3,605 U.S. adults 18 and over in February and March 2023 who had health insurance across different plan types. Over the past several years, I’ve come to appreciate the concept of PAB by listening to and learning from colleagues Dr, Grace
The State of Healthcare in America, State-By-State
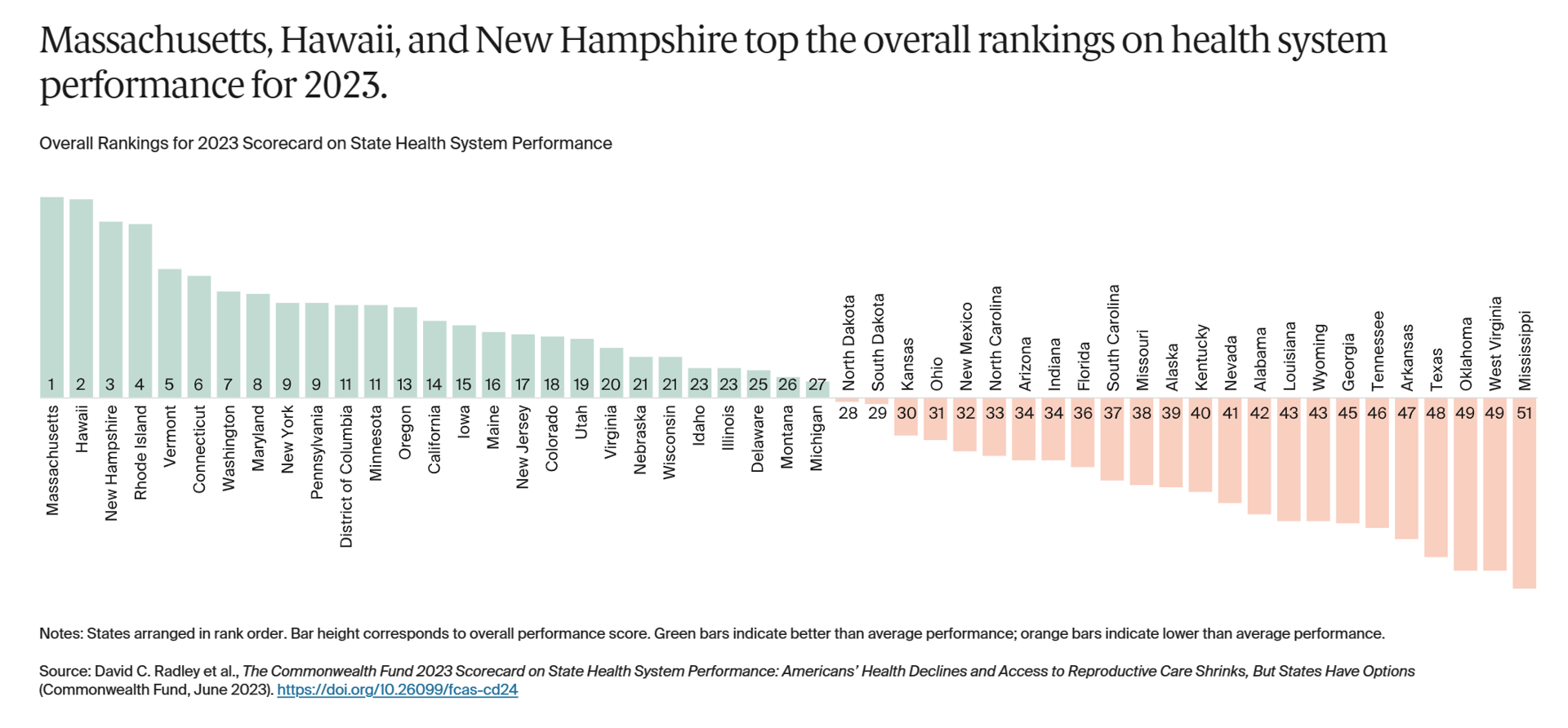
If you live in Massachusetts, Hawaii, and New Hampshire, you win a kind of state lottery for public health and well-being, based on this year’s read of the 2023 Scorecard on State Health System Performance from The Commonwealth Fund. Here’s a picture of the annual study’s top-line findings, a roster of the fifty U.S. states ranked by a mash-up of health system indicators. As Annie Burkey of FierceHealthcare succinctly summed it up, the “Commonwealth Fund gives healthcare in southeastern states failing grades across the board.” I’ll give you more details about the Top and Bottom
Patients-As-Health Care Payers Define What a Digital Front Door Looks Like
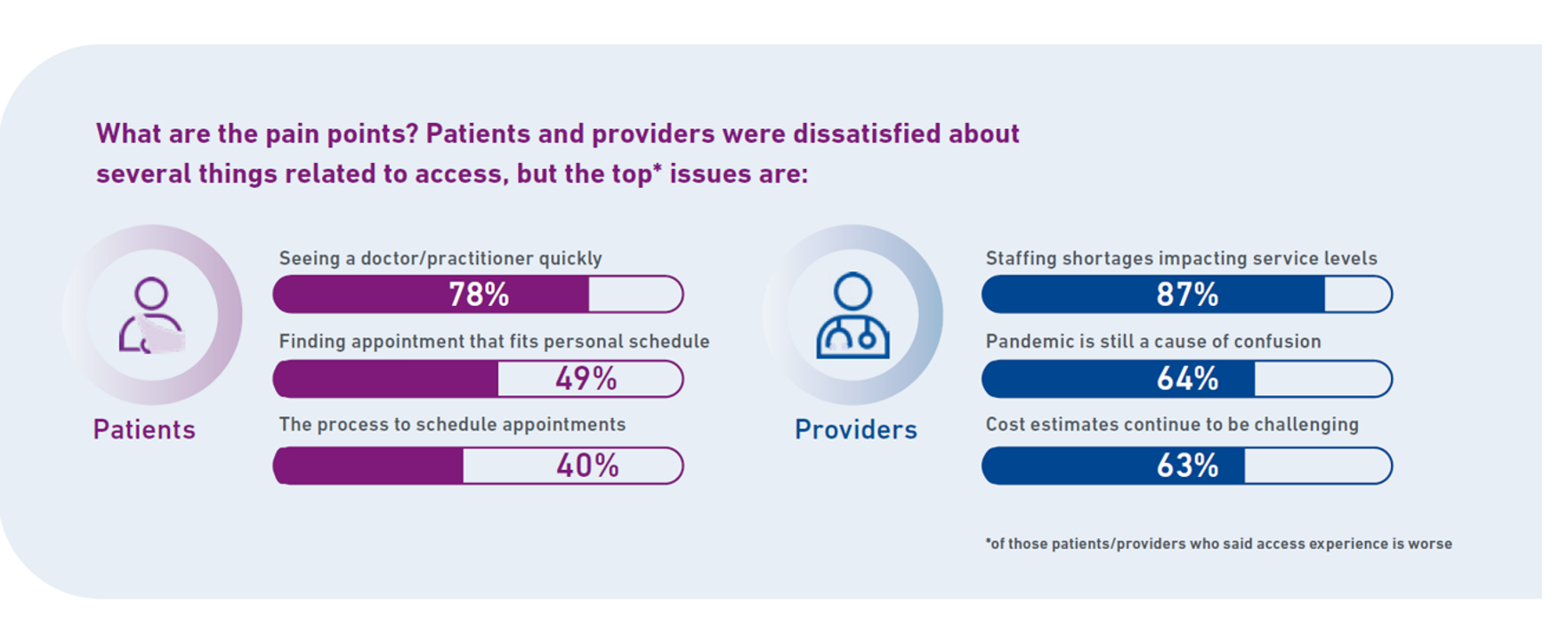
In health care, one of the “gifts” inspired by the coronavirus pandemic was the industry’s fast-pivot and adoption of digital health tools — especially telehealth and more generally the so-called “digital front doors” enabling patients to access medical services and personal work-flows for their care. Two years later, Experian provides a look into The State of Patient Access: 2023. You may know the name Experian as one of the largest credit rating agencies for consumer finance in the U.S. You may not know that the company has a significant footprint
Consumers and Cancer: 3 Patient-Focused Charts From IQVIA on the State of the Oncology in 2023 – and Introducing CancerX
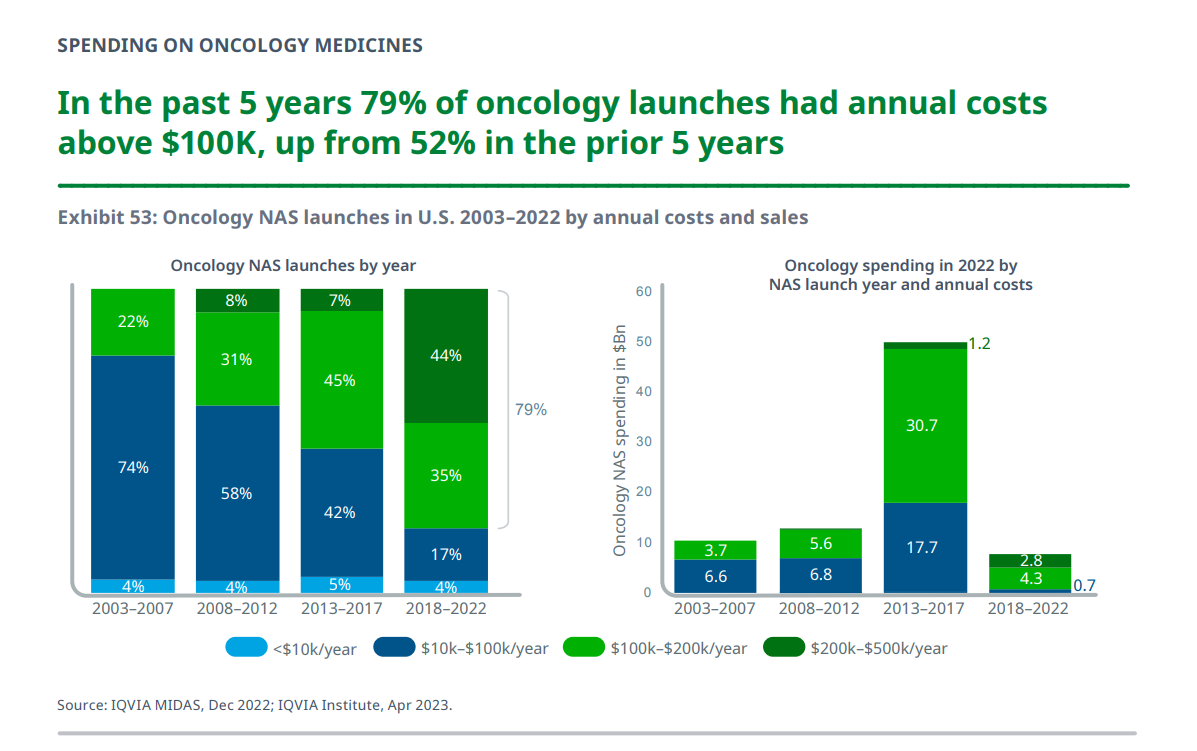
It’s time for the annual ASCO conference, currently convening the American Society for Clinical Oncology in Chicago. Starting 2nd June, there have been dozens of positive announcements updating research and therapies bringing hope to the 2 million new patients who will be diagnosed with cancer in the U.S. in 2023, and millions of more people worldwide. Just in time for #ASCO2023, the IQVIA Institute published their annual report on Global Oncology Trends 2023 – Outlook to 2027, an update featuring pipelines, therapy approvals, research updates, costs of oncology products, and patients.
Searching for Health/Care Touchpoints in the 2023 Axios Harris Poll 100
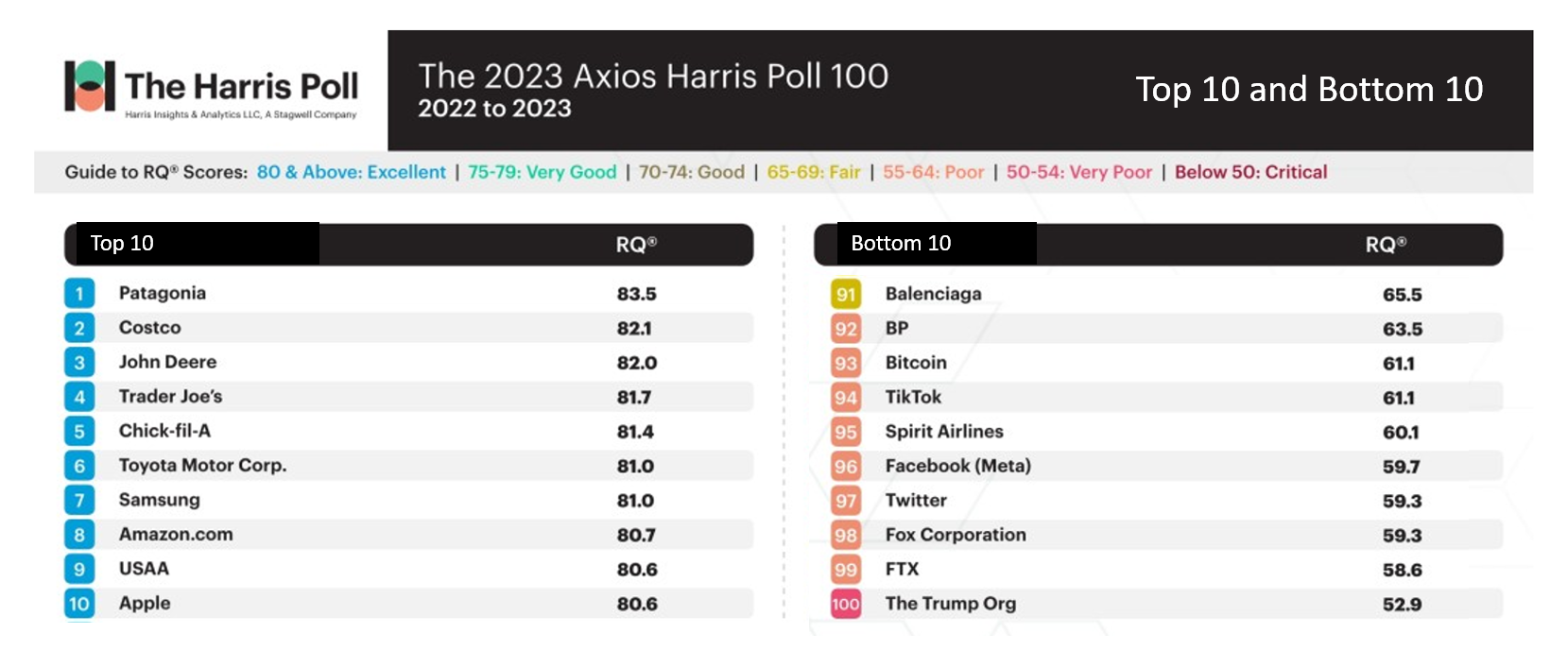
Patagonia, Costco, John Deere, and Trader Joe’s are loved; Twitter, Fox Corp., FTX and The Trump Organization? Not so much. Welcome to 2023 Axios Harris Poll 100 list of companies U.S. consumers rate from excellent in terms of reputation to very poor and, one in particular, “critical.” Exploring the list, we can find insights into consumers’ preferred touchpoints for health, health care, and well-being curated in their daily lives. In this, today’s, Health Populi blog, I consider The 2023 Axios Harris Poll 100 reputation rankings in light of what we learned from the Morning Consult Most Trusted Brands 2023 study
What $31,065 Can Buy You: a Toyota Corolla Cross Hybrid, a Year at Gnomon School, or Healthcare for a Family of 4 in America
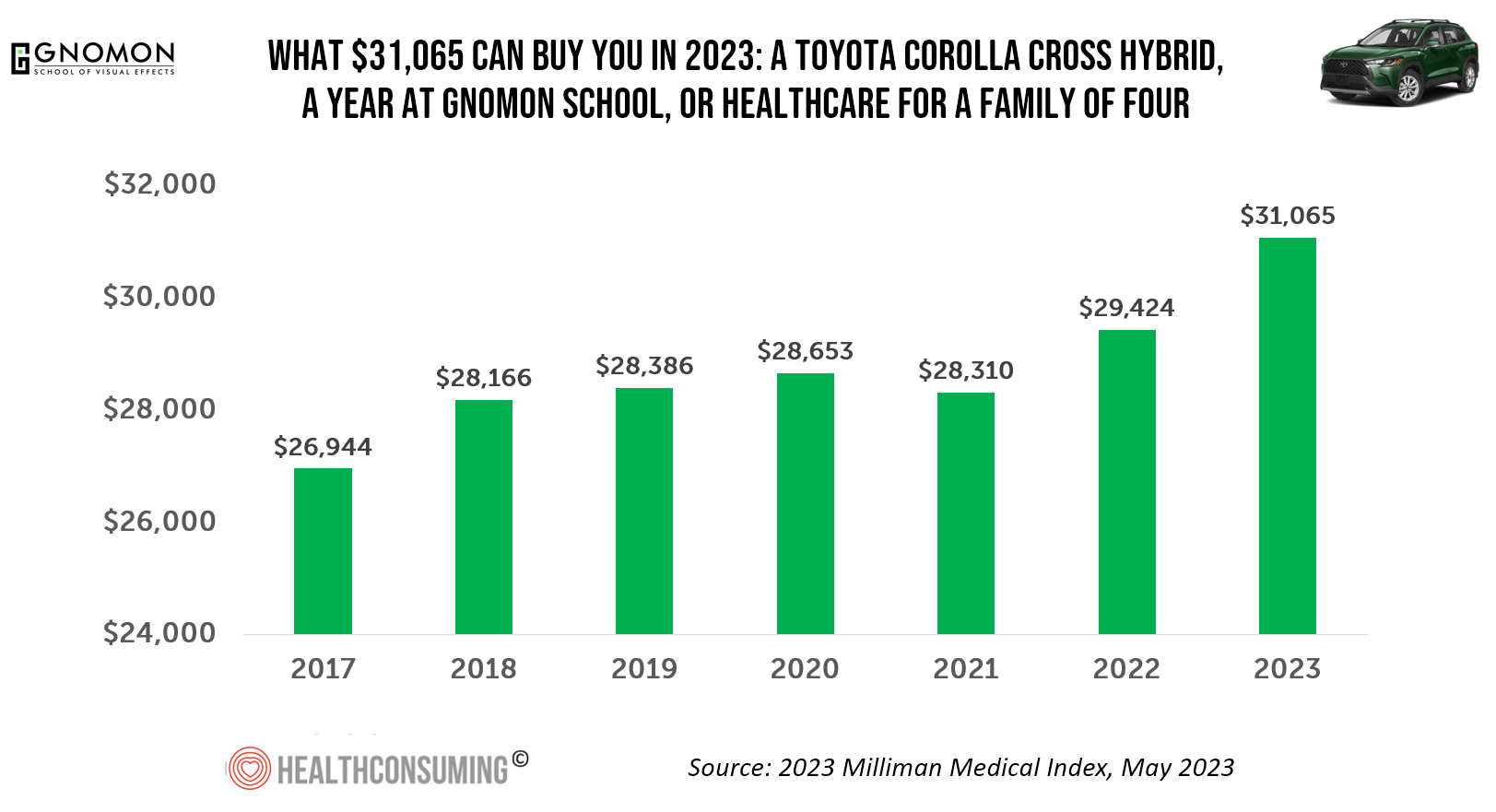
“Healthcare costs came roaring back in 2021” after falling in 2020. In 2023, that roaring growth in health care costs continues with expected growth of 5.6%. For 2023, you could take your $31K+ and buy a Toyota Corolla Cross Hybrid auto, fund a year at the Gnomon School in Hollywood toward a degree in animation or game design, or buy healthcare for your family of 4. Welcome to this year’s annual look at health care costs for a “typical” U.S. family explained in the 2023 Milliman Medical Index (MMI).
Our Mental and Emotional Health Are Interwoven With What We Eat and Drink – Chewing On the IFIC 2023 Food and Health Survey
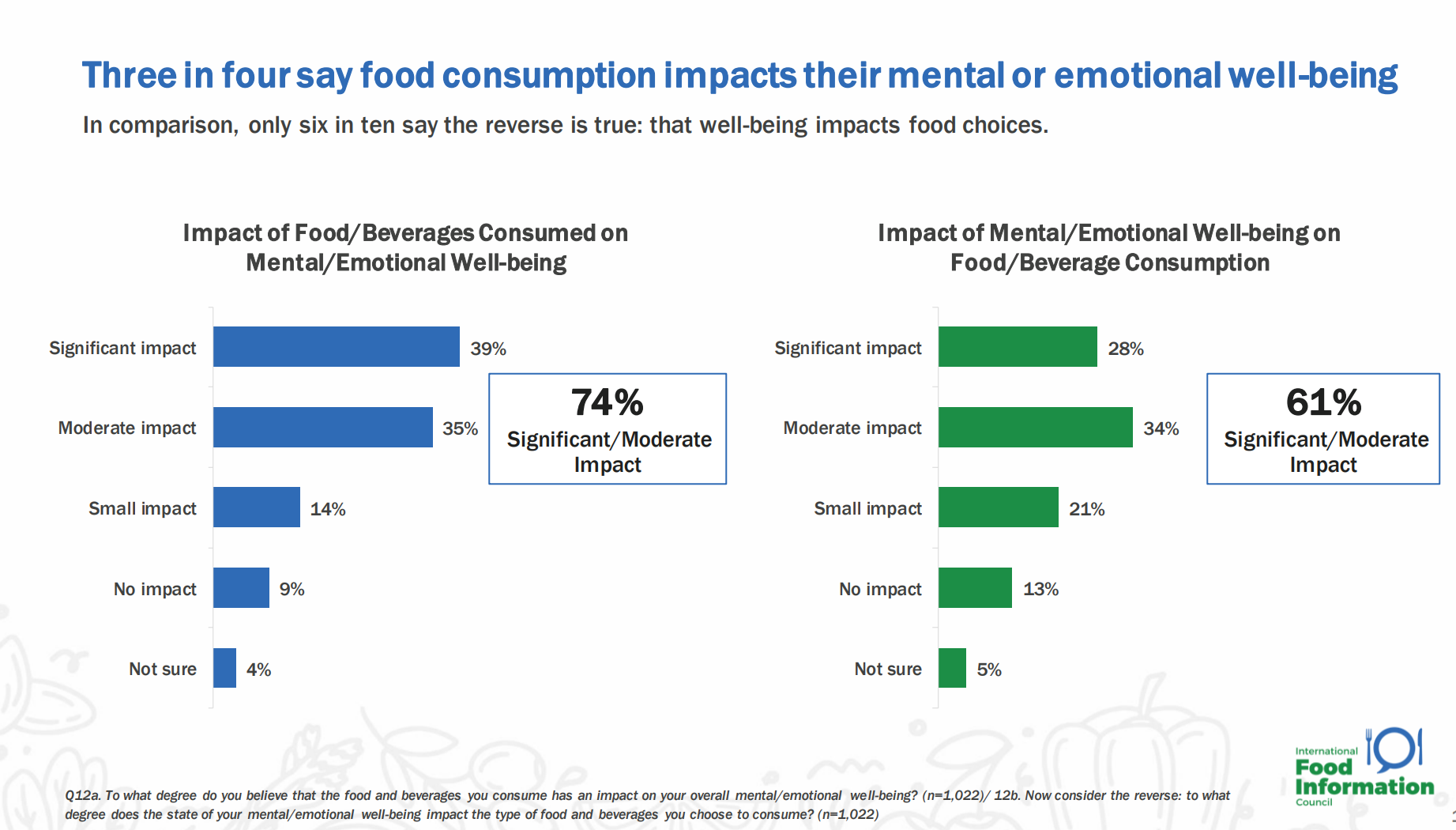
As most Americans confess to feeling stressed over the past six months, peoples’ food and beverage choices have been intimately connected with their mental and emotional well-being, we learn from the 2023 Food & Health Survey from the International Food Information Council (IFIC). For this year’s study, IFIC commissioned Greenwald Research to conduct 1,022 interviews with adults between 18 and 80 years of age in April 2023. The research explored consumers’ perspectives on healthy food, the cost of food, approaches to self-care through food consumption, the growing role of social media in the food system, and the influence of sustainability
Retail Clinics’ Growing Role in Health Care and Prescription Drug Sales
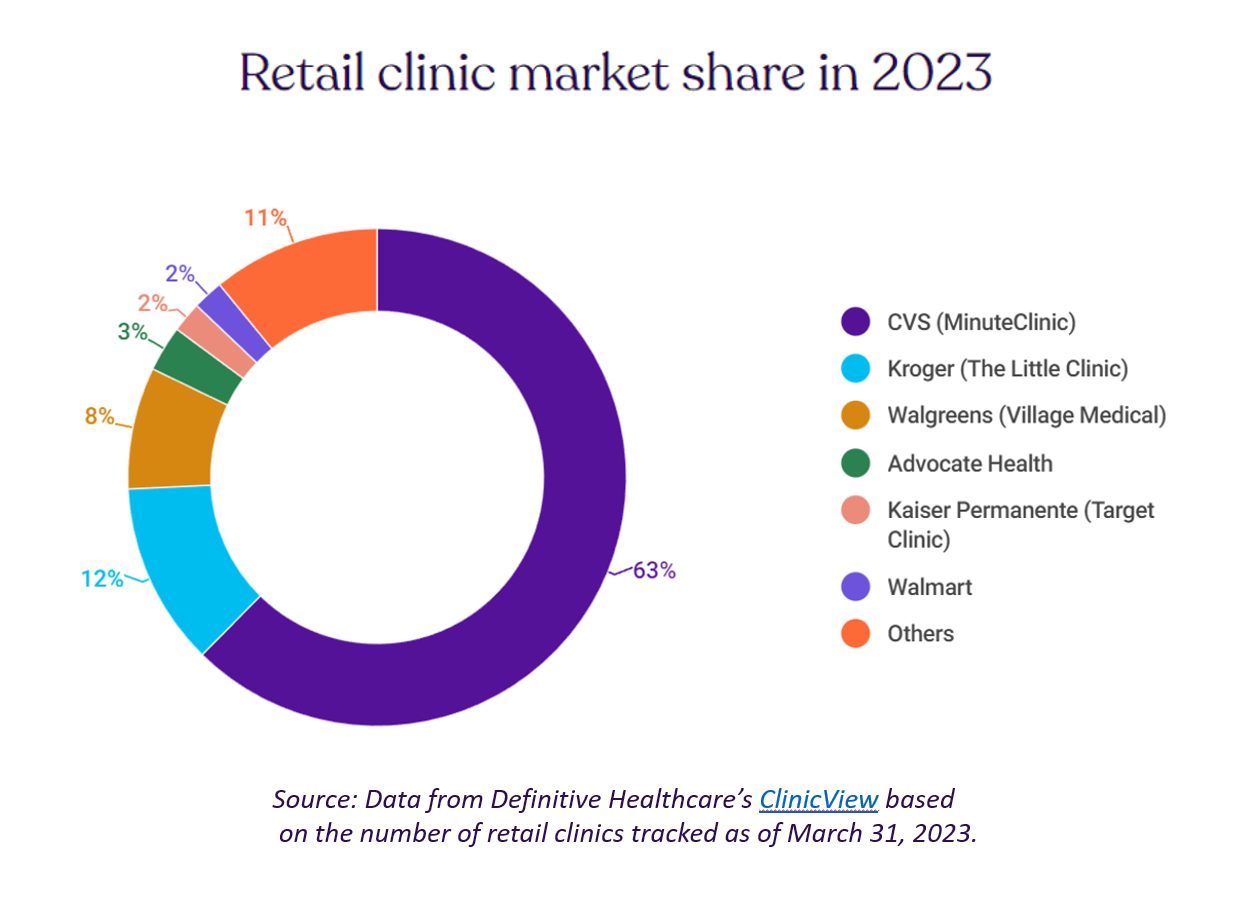
“It seemed like an odd pairing: shampoo and a throat swab,” observes a new report on the growth of retail health from Definitive Healthcare. But retail clinics are no longer, as the paper explains, “an experiment of a few grocery stores….they’re becoming a major force in the U.S. healthcare system,” asserts the thesis of Retailers in healthcare: A catalyst for provider evolution. While the use of emergency departments fell by 1% in the past five years, the use of retail clinics expanded by 70%, Definitive Healthcare calculated. Most retail clinics are owned by
Medical Debt: “The Debt of Necessity” – A Current U.S. Picture from the CFPB

On April 11, 2023, three of the largest U.S. consumer credit rating companies — Equifax, Experian and TransUnion — planned to remove medical bill collections that were under $500 from consumers’ credit reports. The Consumer Financial Protection Bureau (CFPB) calculated that these medical bill “erasures” under $500 impacted nearly 23 million consumers and eliminated medical collections totally for 15.6 million people in the U.S. according to CFPB’s recently-published Data Point report. For some context, it’s useful to know that the CFPB was created as part of the Dodd-Frank Wall Street Reform and Consumer Protection Act passed by Congress and signed
Getting Health Care at a Retail Pharmacy vs a Retail Store: Consumers May Be Favoring the Pharmacist Versus the Retailer
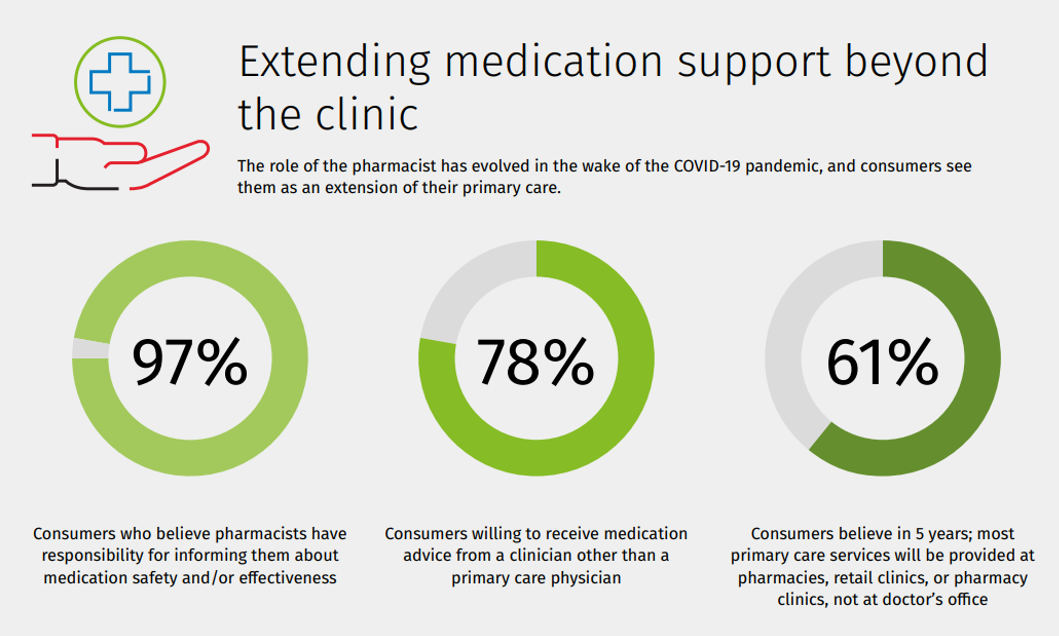
Not all “retail health” sites are created equal, U.S. consumers seem to be saying in a new study from Wolters Kluwer Health, the company’s second Pharmacy Next: Consumer Care and Cost Trends survey. Specifically, consumers have begun to differentiate between health care delivered at a retail pharmacy versus care offered at a retail store — such as Target or Walmart (both named as sites that offer “health clinics in department stores” in the study press release). While 58% of Americans were likely to visit a local pharmacy as a “first step” when faced with a non-emergency medical situation and 79%
Virtual Health Care Can Reduce Carbon Emissions: the Environmental ROI on Telehealth
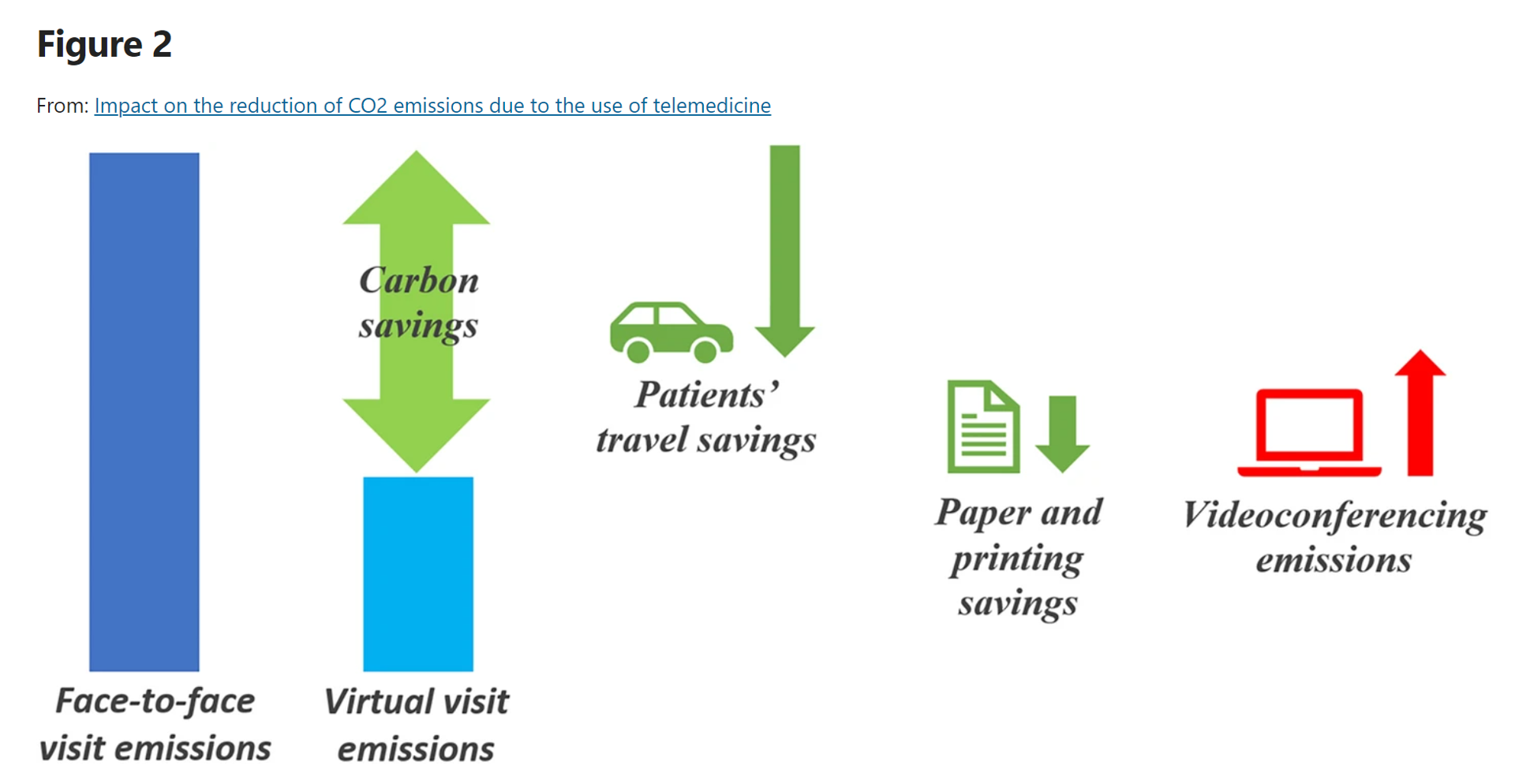
As implemented in the COVID-19 era and its immediate wake, the most obvious environmental benefits offered by telehealth visits replacing in-person patient encounters have been achieved through reduced patient travel, considering The Role of Virtual Consulting in Developing Environmentally Sustainable Health Care, a systematic literature review published in the Journal of Medical Internet Research. This study, led by researchers at the University of Oxford, UK, and the University of Oslo, Norway, identified over 1,600 scientific papers, narrowing the most rigorous and relevant to 23 papers focusing on virtual consulting and carbon emissions. This is an important question for two major
A Public Health Wake-Up Call: Reading Between the Lines in IQVIA’s 2023 Use of Medicines Report
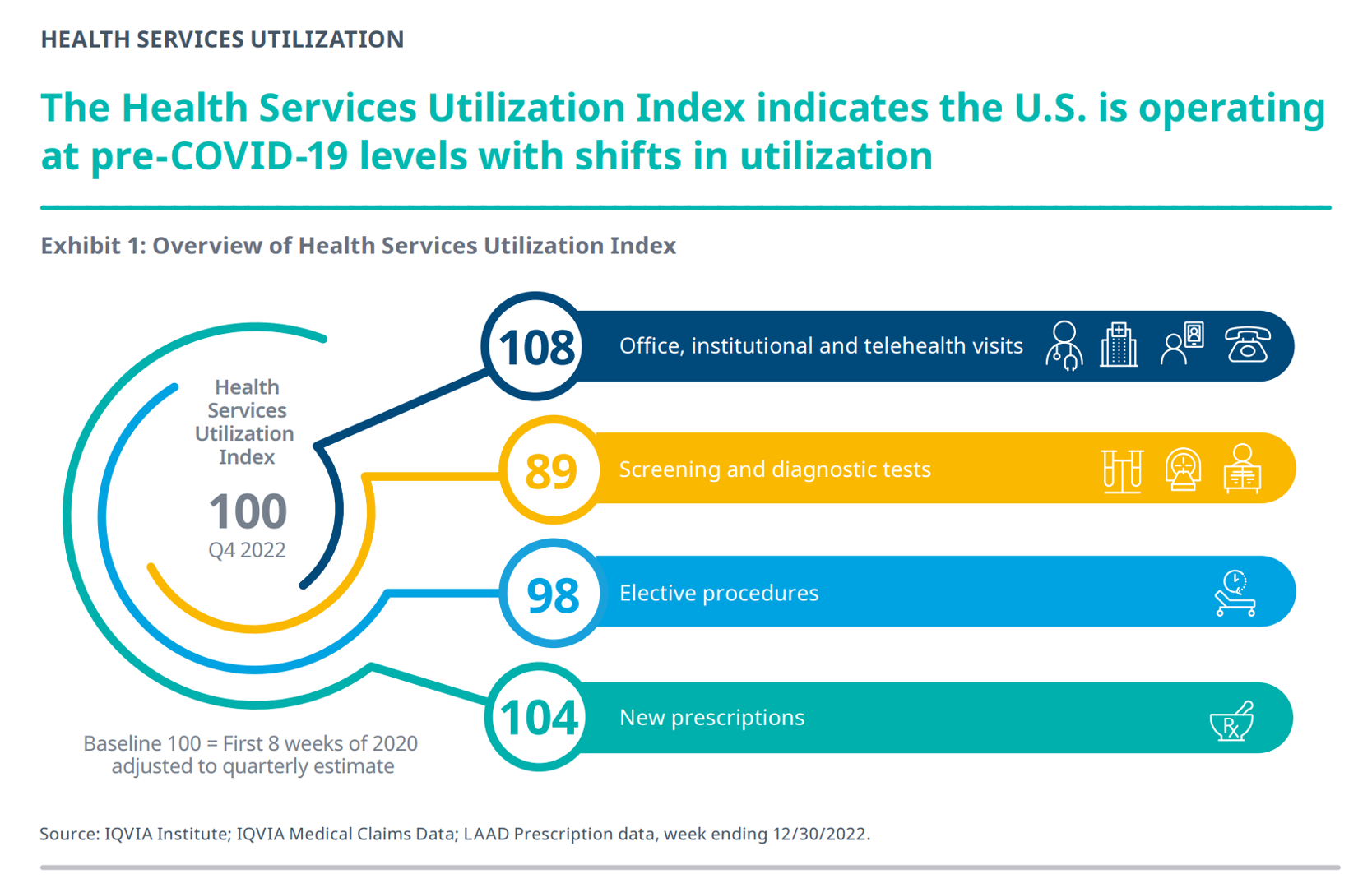
Reviewing the annual 2023 report from the IQVIA Institute for Human Data Science discussing The Use of Medicines in the U.S. is always a detailed, deep, and insightful dive into the state of prescription drugs. It’s a volume speaking volumes on the current picture of prescribed meds, spending and revenues, health care utilization trends, and a forecast looking out to 2027. In my read of this year’s review, I see a flashing light for U.S. health care: “Wake up, public health!” I’ve pulled out a few of the data points that speak to me about population health, prevention and early
Thinking Pharma on a Friday: Europe’s Big Reforms for a Health Union & the U.S. 50-State Fragments

The COVID-19 pandemic re-shaped European Union leaders to reimagine healthcare, public health, and health citizenship in the EU. Welcome to #HealthUnion, the hashtag that the European Commission has adopted with the vision of assuring access to medicines for all people living in the 27-nation EU area — regardless of socioeconomic status. On 26th April 2023, the EC unveiled the most significant reforms for the region’s pharmaceutical industry in twenty years. It’s really a package or “toolkit” in the words of EC Health and Food Safety Commissioner Stella Kyriakides for addressing several strategic health pillars
Health Care Financing: How Inflation and Health Care Prices Could Hit the U.S. Consumer
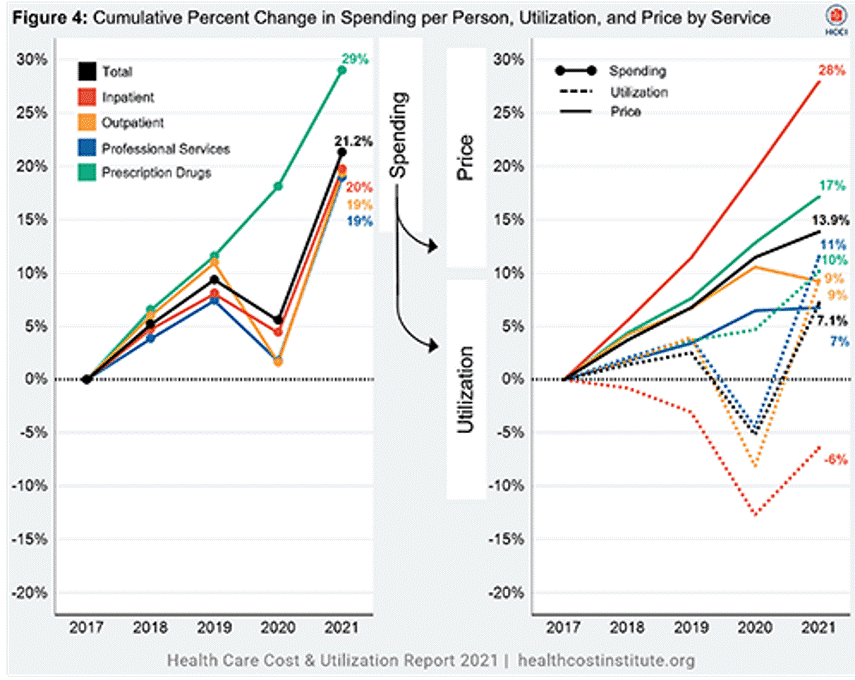
In the U.S. in 2021, per person health care spending increased by nearly 15%, reversing 2020’s spending decline of 3.5% in the first year of the COVID-19 pandemic. The latest Health Care Cost and Utilization Report from the Health Care Cost Institute (HCCI) details health spending in 2021, dissecting the change in terms of utilization of services and prices by category. That’s a big rise over consumers’ household inflation for food, energy, and other kitchen-table considerations, prompting me to look for additional context from a recent paper published by the OECD on Health care financing in times of high inflation,
Consumers Expect Every Company to Play a Meaningful Role in “My Health” – New Insights from the 2023 Edelman Trust Barometer

People have expanded their definitions of health in 2023, with mental health supplanting physical health for the top-ranked factor in feeling healthy. Welcome to the Edelman Trust Barometer Special Report: Trust and Health, released this week, with striking findings about how the economic, post-pandemic life, pollution and climate change all feed mis-trust among citizens living in 13 countries — and their eroding trust for health care systems. While these factors vary by country in terms of relative contribution to citizen trust, note that in the U.S., social polarization plays an outsized role in factors that “make us
“Your care, your way:” Learning from the Philips Future Health Index 2023

Consider the key drivers of supply and demand in health care, globally, right now: On the medical delivery supply side, the shortage of staff is a limiting factor to continuing to deliver care based on the usual work-flows and payment models. On the demand side, patients are taking on more demanding roles as consumers with high expectations for service, convenience, and safe care delivered closer to home — or at home. This dynamic informs The Future Health Index 2023 report from Philips, launched this week at HIMSS 2023. This is the eighth annual global FHI report, with detailed country-specific analyses to
Don’t Mess with Medicare and Medicaid, Washington: They Remain Popular with Americans Across Party ID
A majority of the U.S. public does not want politicians to “up-end” government-funded health programs, according to the Kaiser Family Foundation’s March 2023 Health Tracking Poll. Social Security, Medicare, and Medicaid all garner most partisans’ support whether identifying as Democrat, Independent, or Republican, KFF found in their monthly poll of U.S. voters ages 18 and over. The survey was conducted online and by telephone among 1,271 U.S. adults between March 14-23, 2023. Among all the important findings in this well-timed poll, I’ll point to the issue of public
The Patient Is Still the Payor – And May Skip Paying for Prevention (Eyes on the ACA & Texas)
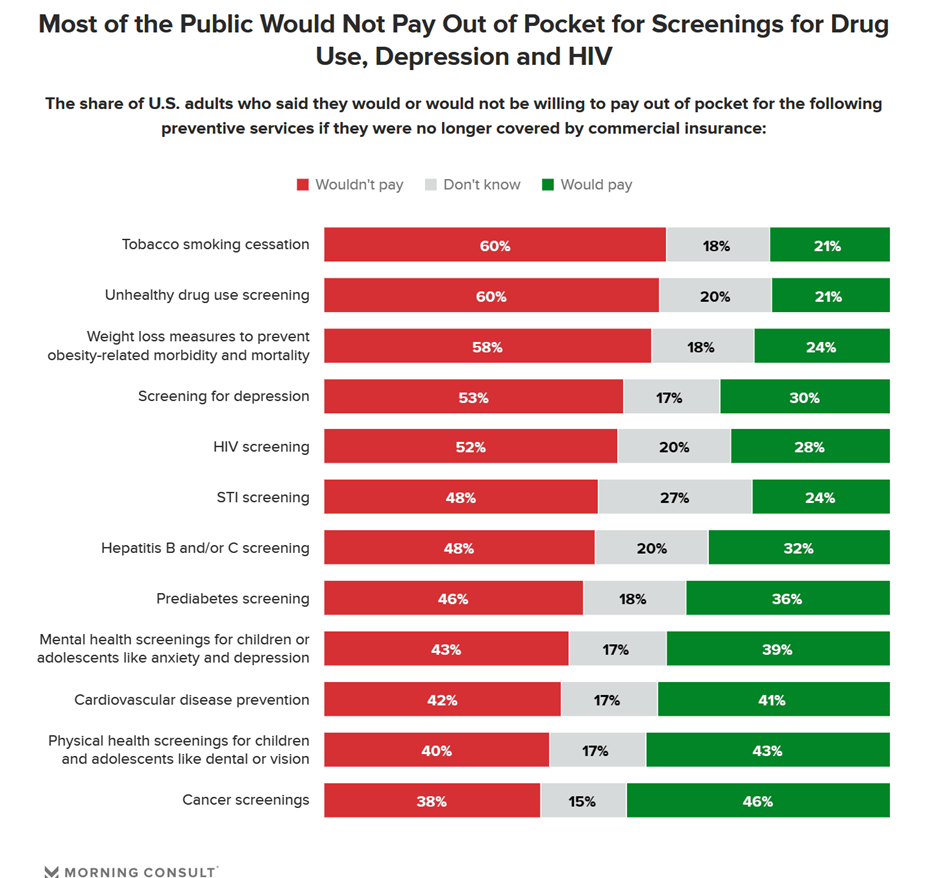
Many health citizens in the U.S. would likely skip receiving preventive health care services if the Affordable Care Act’s (ACA) coverage for them goes away, a Morning Consult survey found. The first chart illustrates the top-line of this research: that most U.S. adults would not pay out of pocket for several preventive services including tobacco cessation, drug use screening, weight loss measures to prevent obesity-related illnesses, as well as screening for depression or HIV. One of the key benefits embedded in the ACA was “free” without co-pay shares for preventive care. These
We Are All Health Consumers Now – Toluna’s Latest Look at Consumers’ Health & Well-Being
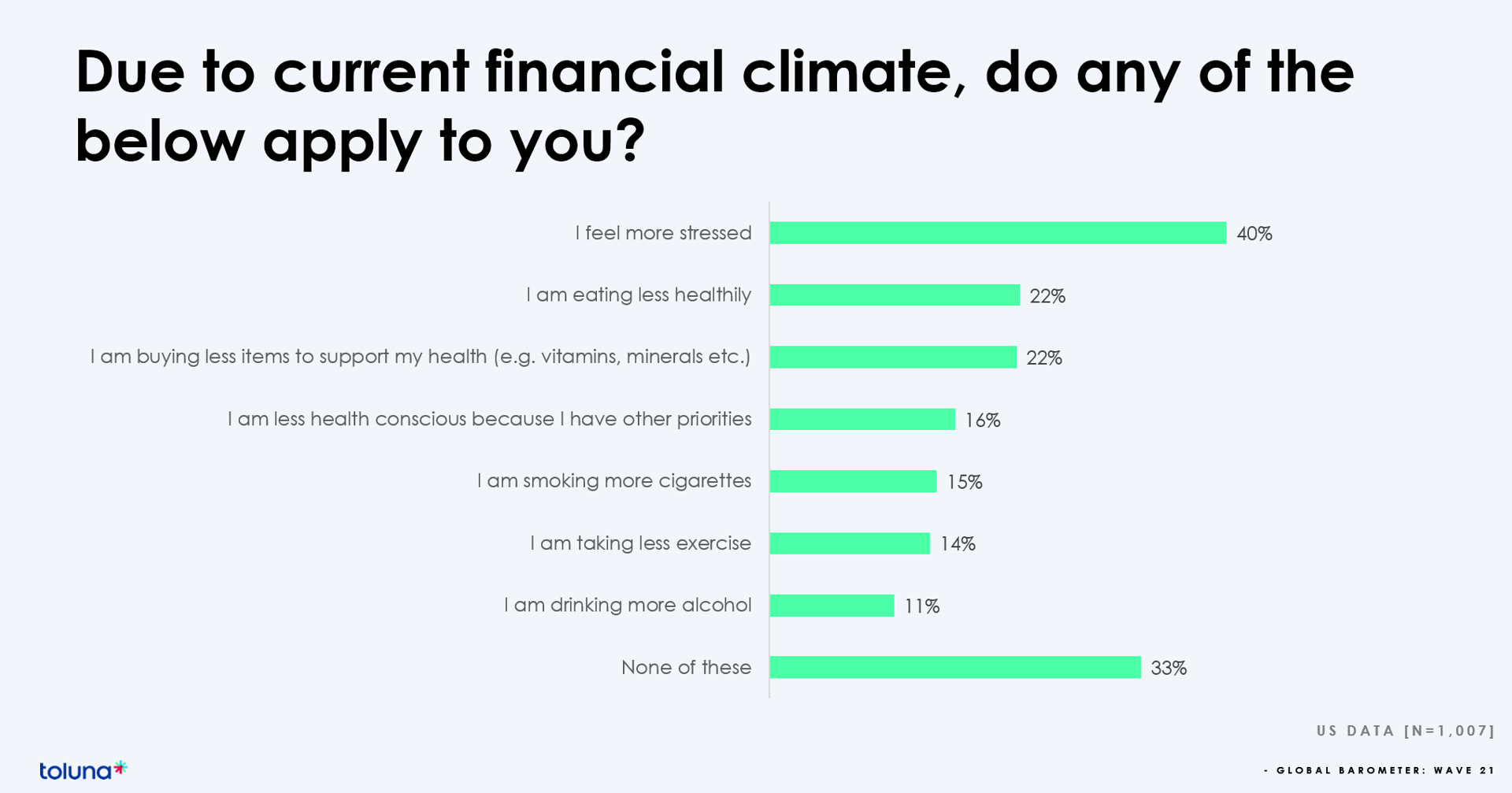
The challenging financial climate at the start of 2023 is impacting how people, globally, are perceiving, managing, and spending money on health and well-being, based on the latest (Wave 21) Global Consumer Barometer survey conducted by Toluna, a sister company of Harris Interactive. Globally, one-third of health citizens the world over are confronting greater stress levels due to the higher cost of living in their daily lives. One in two people say that rising cost of living is negatively impacting their health and well-being. On the positive side, one in three people believe
People Using Health Apps and Wearable Tech Most Likely Track Exercise and Heart Rate, Sleep and Weight – But Cost Is Still A Barrier
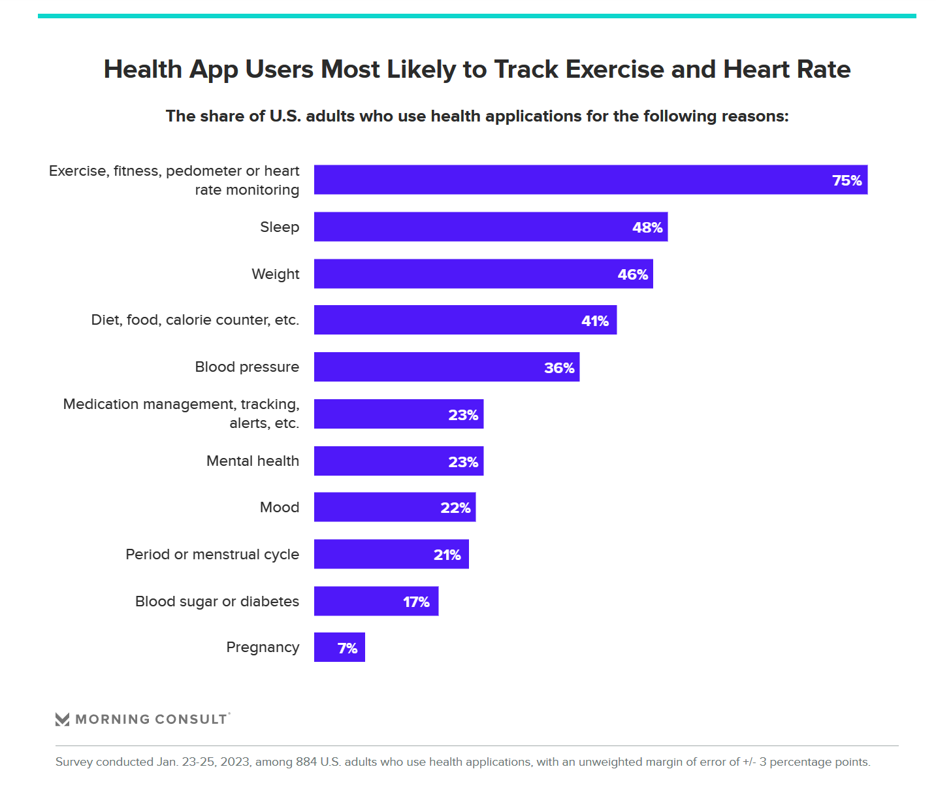
Over one in three U.S. consumers use a health app or wearable technology device to track some aspect of their health. “The public’s use of health apps and wearables has increased in recent years but digital health still has room to grow,” a new poll from Morning Consult asserts, published today. Among digital health tech users, most check into them at least once every day in the past month. One in four use these tech’s multiple times a day, the first pie chart illustrates. Eighteen percent of people use their digital
The American Hospital Association Looks at Retail and Tech Health Care Disruptors

Ever since Clayton Christensen explained the concept of disruptive innovation in 1995, health care became one of the poster children emblematic of an industry ripe for disruption. Nearly 30 years later, disrupting health care continues to be a theme which, in 2023, seems open for those slow-moving tectonic driving forces to finally re-form and re-imagine health care delivery. So in today’s Health Populi we turn to a new report, Health Care Disruption 2023 Outlook, part of AHA’s “The Buzz” market scan initiative. The American Hospital Association is taking disruption seriously right here, right now, as the U.S. hospital sector is
The Reputation of Pharma Among U.S. Consumers Is Tied More to Pricing Than to Innovation
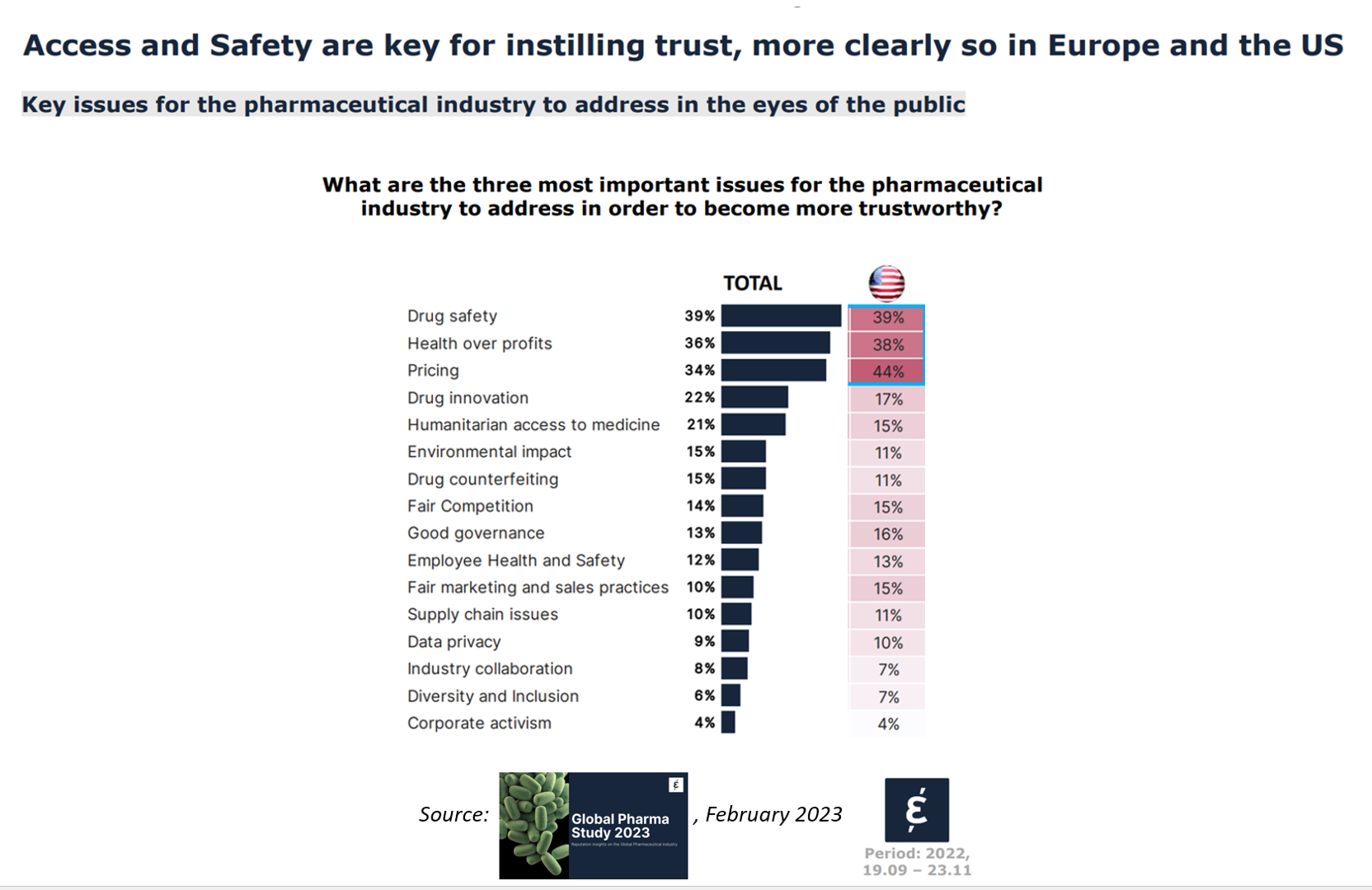
In the U.S., price and the cost of medicines is tied to how people feel about the pharma industry, evidenced in the Global Pharma Study 2023 from Caliber. Caliber, a reputation and corporate strategy consultancy, fielded survey research among over 17,000 health consumers including U.S. adults between 18 and 75 years of age as well as health citizens living in Brazil, China, France, Germany, Japan, and the UK. Caliber assessed the reputation of 16 industries, globally, finding that pharma ranked 10th among the 16, just below automotive and just above chemicals (and well
The US Healthcare System Outspends and Underperforms While Most People Live Paycheck to Paycheck
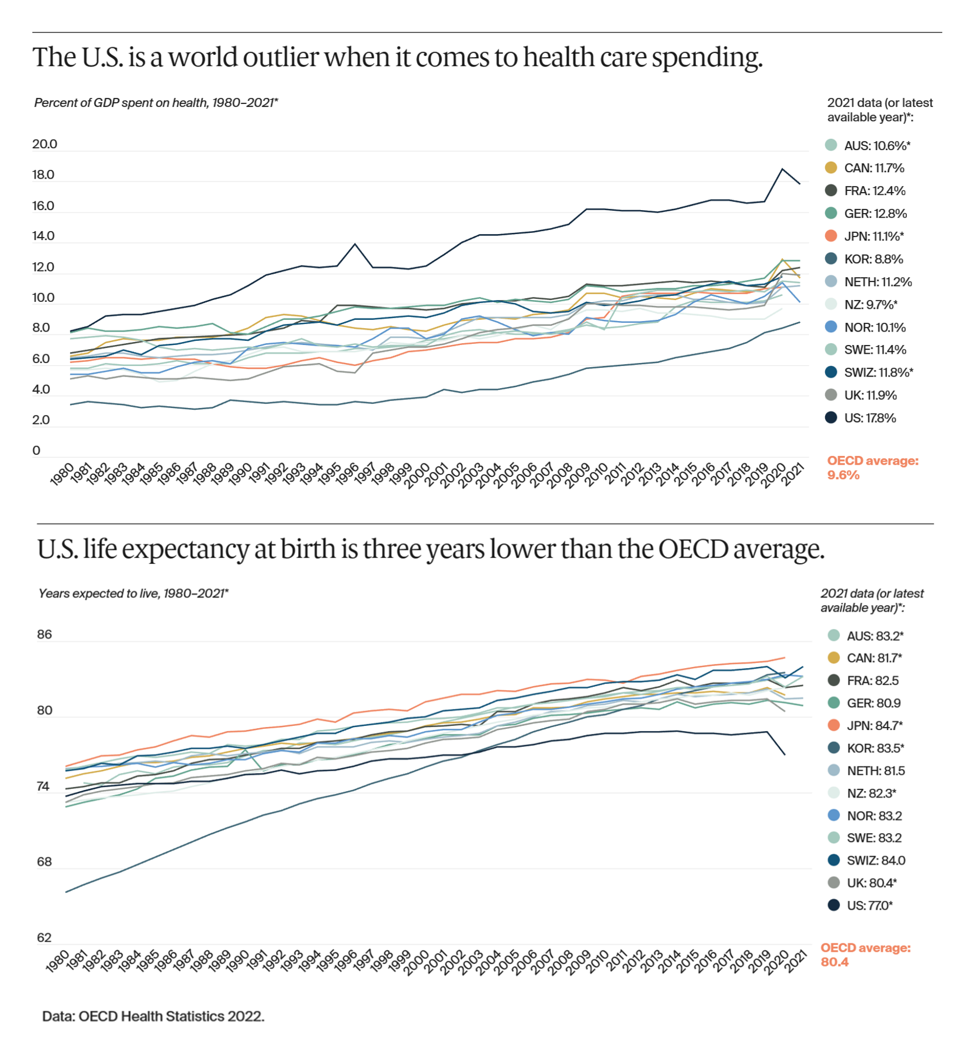
The U.S. is an outlier in the world for high health care spending, as well as in low achievement for life expectancy at birth — 3 years less than that in peer OECD countries — discussed in U.S. Health Care from a Global Perspective, 2022: Accelerating Spending, Worsening Outcomes, the latest look into American health system performance in a global context from The Commonwealth Fund. Another study published in JAMA this week talks about the Organization and Performance of US Health Systems, calling out the fact that, “Small quality differentials combined with large price differentials suggests that health systems have
Quick, Accessible, Inexpensive Health Care – A Retail Health Update from Amazon and Dollar General

Two announcements this week add important initiatives to patients’ growing choices that speak to their consumer-sides’ sense of value and personal healthcare cost-containment: Amazon launched RxPass, a generic medicines subscription service; and, Dollar General promoted its mobile health service powered by DocGo on demand for health visits, “right outside the store.” These two programs come from outside of the legacy health care system of so-called incumbents — hospitals, health systems, health insurance — leveraging two brand-names beloved to many consumers for convenience, price transparency, and sheer cost. First, check out Amazon Pharmacy’s RxPass. Amazon
Integration is the New Innovation for Healthcare in 2023: Reflections on CES2023 and JPM2023

The peak of venture investment for digital health was in 2020 and 2021, precipitously declining later in 2022. And the outlook for 2023 is practical and Show-Me: that is, demonstrate clinical outcomes and return-on-investment before “I” (for investors) can take a leap of faith to spend a dollar, a Yen, a Euro, or British pound on a shiny new-new healthcare thing. If it’s January, then CES and JP Morgan convene their influential annual meetings which feature health technology for globally engaged health industry stakeholders — investors, surely, but also providers, innovators, analysts, and insurers. In my January
Record Numbers of People in the U.S. Putting Off Medical Care Due to Cost – A New “Pink Tax” on Women?
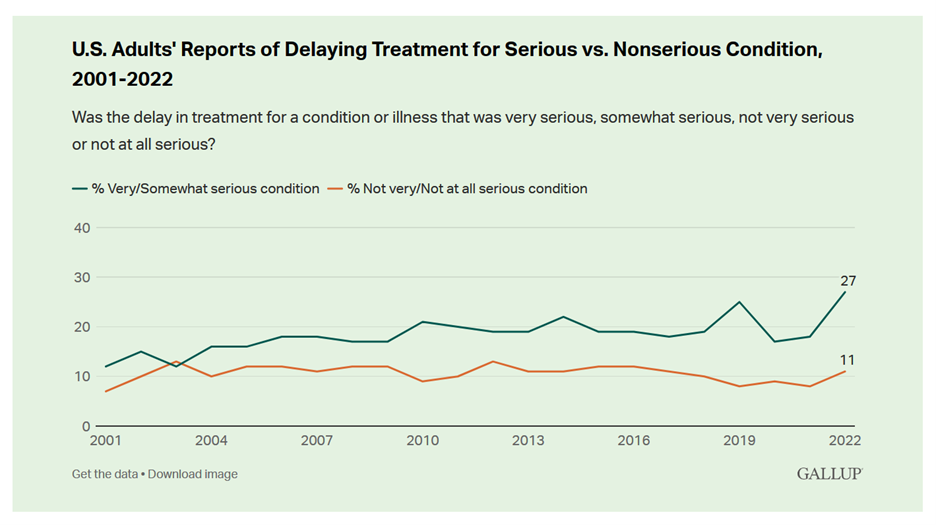
More people in the U.S. than ever have put off medical care due to cost, according to Gallup’s latest poll of patients in America. Gallup conducted the annual Health and Healthcare poll U.S. adults in November and December 2022. This was the highest level of self-rationing care due to cost the pollster has found since its inaugural study on the topic in 2001. This was also the most dramatic year-on-year increase of postponing treatment due to cost in the study’s history. Note the substantial difference in women avoiding
In 2023, We Are All Health Consumers in Search of Value

Every health/care industry stakeholder will be in search of value in 2023, I explain in my latest post written on behalf of Medecision. In this essay, I forecast what’s ahead for hospitals, digital health innovators and investors, employers, pharma, and patients-as-consumers — all firmly focused on value in the new year. “Inflation may make consumers and the healthcare system sicker,” Deloitte expects, signaling a sort of “unrest” for the healthcare ecosystem. One of the most telling data points I include in my assessment of 2023 comes from GSR Ventures, which polled major health care investors on
When Household Economics Blur with Health, Technology and Trust – Health Populi’s 2023 TrendCast

People are sick of being sick, the New York Times tells us. “Which virus is it?” the title of the article updating the winter 2022-23 sick-season asked. Entering 2023, U.S. health citizens face physical, financial, and mental health challenges of a syndemic, inflation, and stress – all of which will shape peoples’ demand side for health care and digital technology, and a supply side of providers challenged by tech-enabled organizations with design and data chops. Start with pandemic ennui The universal state of well-being among us mere humans is pandemic ennui: call it languishing (as opposed to flourishing), burnout, or
Dollar General & CHPA Collaborate to Bolster Health Consumers’ Literacy and Access for OTC Pain Meds and Self-Care

Health is “made” where we live, work, play, pray, learn….and shop. I spend a lot of time these days in the growing health/care ecosystem where retail health is broadening to address social determinants and drivers of health – namely food, transportation, broadband access, education, environment, and financial wellness – all opportunities for self-care and health engagement. For many years, I have followed the activities of CHPA, the Consumer Healthcare Products Association, and have participated in some of their conferences. Their recent announcement of a collaboration with Dollar General speaks to the growing role of self-care for all people.
Show Me The Evidence and The ROI: Digital Health Investing in 2023 via GSR Ventures
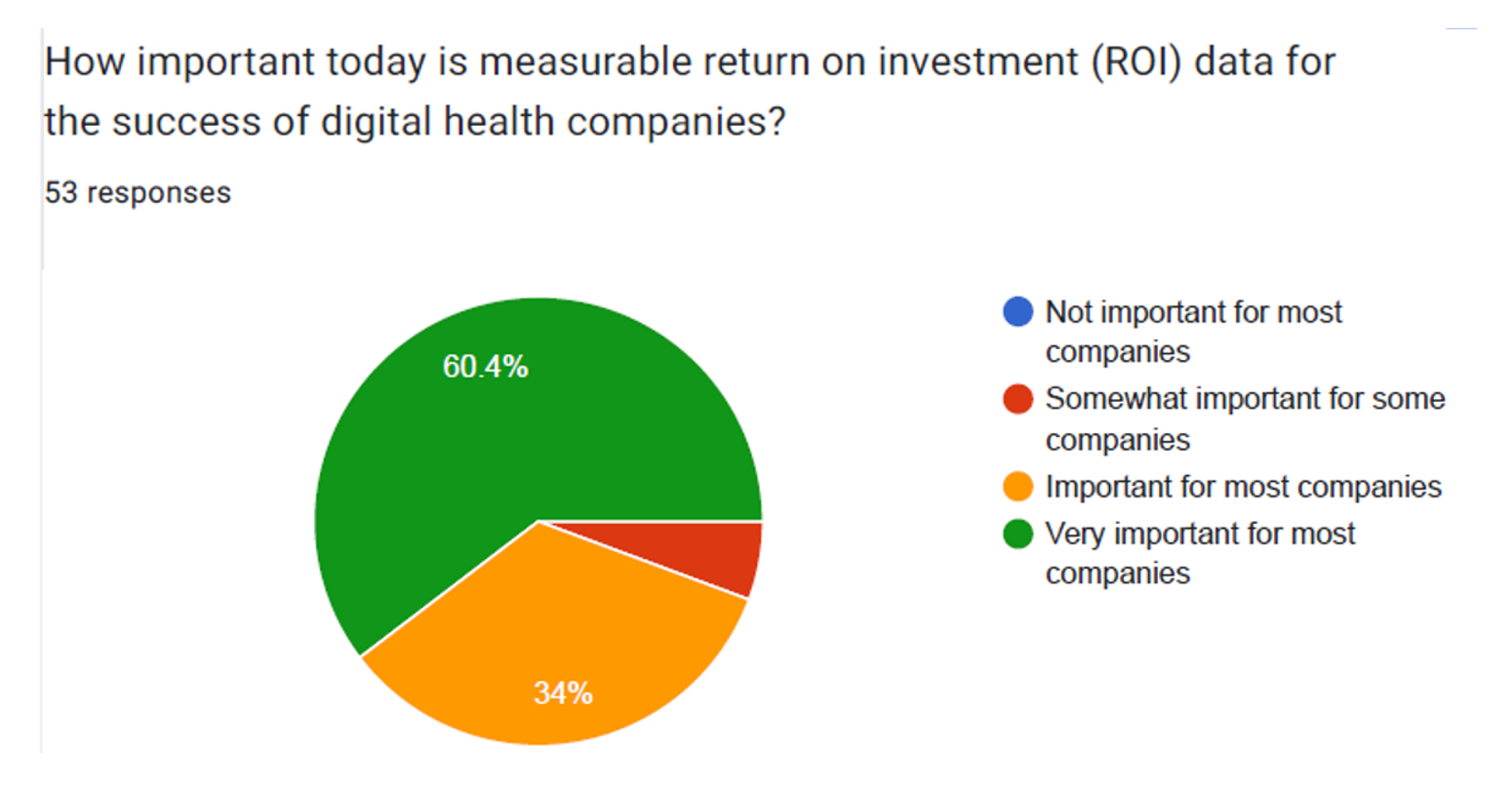
With valuations of digital health companies expected to decline in 2023, investors in the sector are Missourian in spirit in “Show Me” mode: here, it’s all about the clinical evidence and ROI, according to a survey from GSR Ventures. conducted among over 50 major digital health venture capital investors. Most of the 50+ responses to the survey expect that in 2023, valuations for digital health companies will decrease by over 20%: that’s a net of 83% including 60% expecting valuations to fall 20-40%, and 23% anticipating declines of over 40% of valuations in the next
Consumers Are Feeling Their Healthcare Cost of Living – Research from Qualtrics
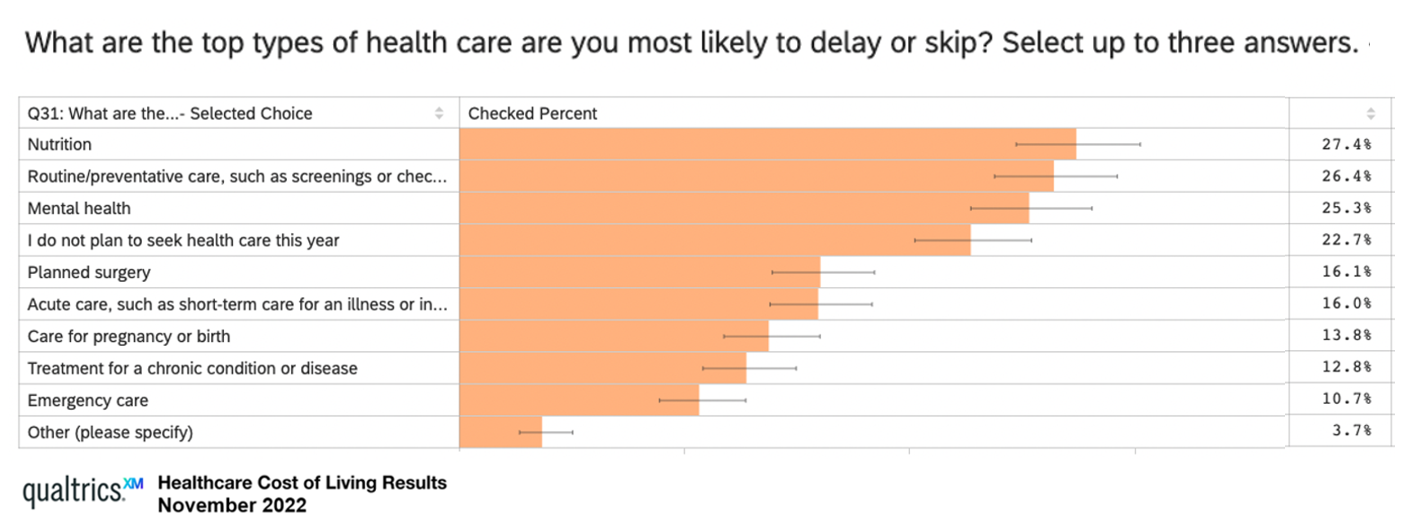
Rising costs are the #1 reason U.S. health consumers are avoiding or delaying health care, replacing concerns about COVID-19, based on survey research from Qualtrics. The company’s Healthcare Cost of Living survey research learned that 48% of U.S. adults chose to defer health care in 2022, split by 31% of consumers skipping care due to cost concerns, and, 17% of people delaying care who had concerns about the coronavirus. Note the types of care delayed or skipped: Over 27% of people delayed care related to nutrition 26% delayed routine or preventive care, such as screenings or
The Food-Finance-Health Connection: Being Thankful, Giving Thanks
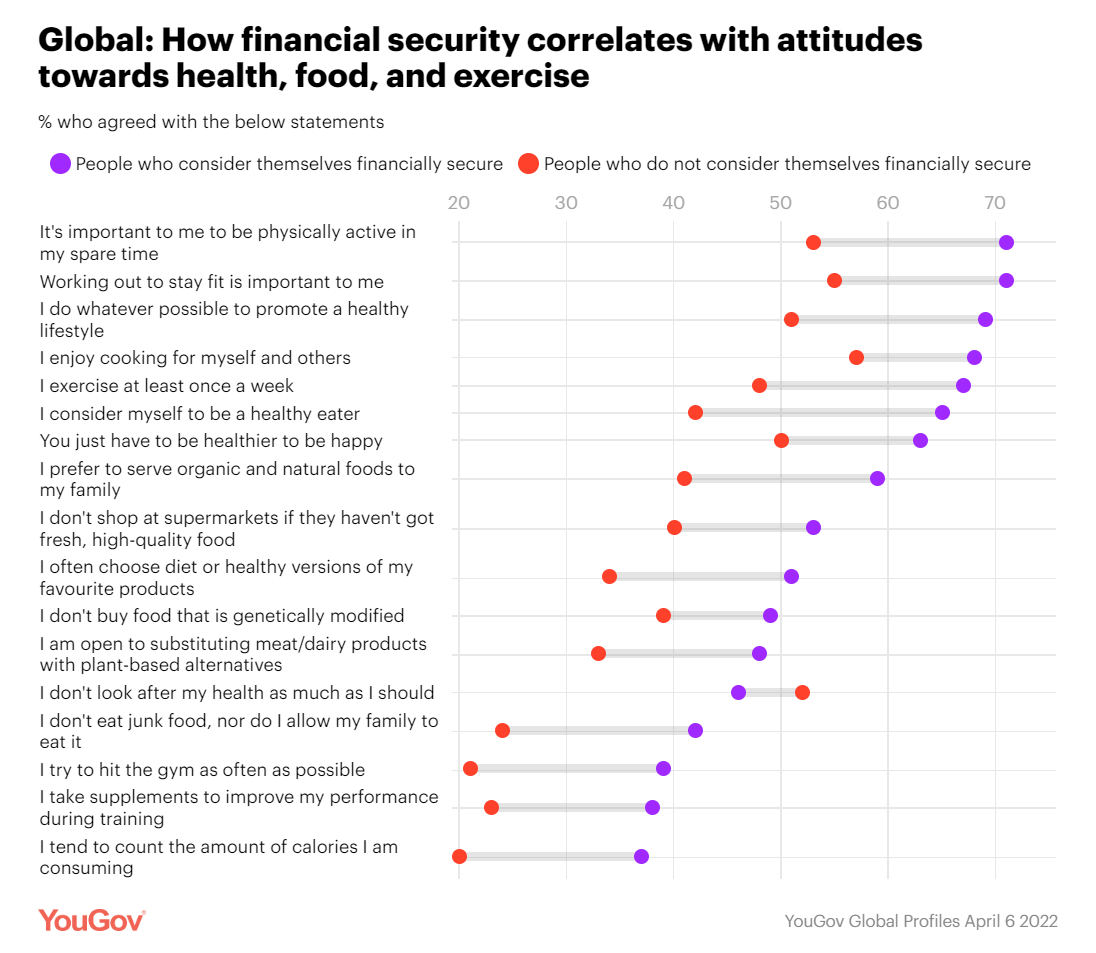
Food features central in any holiday season, in every one’s culture. For Thanksgiving in the United States, food plays a huge role in the history/legend of the holiday’s origins, along with the present-day celebration of the festival. At the same time, in and beyond the U.S., families’ finances will also be playing a central role in dinner-table conversations, shopping on the so-called “Black Friday” retail season (which has extended long before Friday 25th November), and in what’s actually served up on those tables. Let’s connect some dots today on food, finance and health as we enter the holiday season many
Men Work in Retirement for Healthy Aging; Women, for the Money – Transamerica Looks at Retirement in 2022
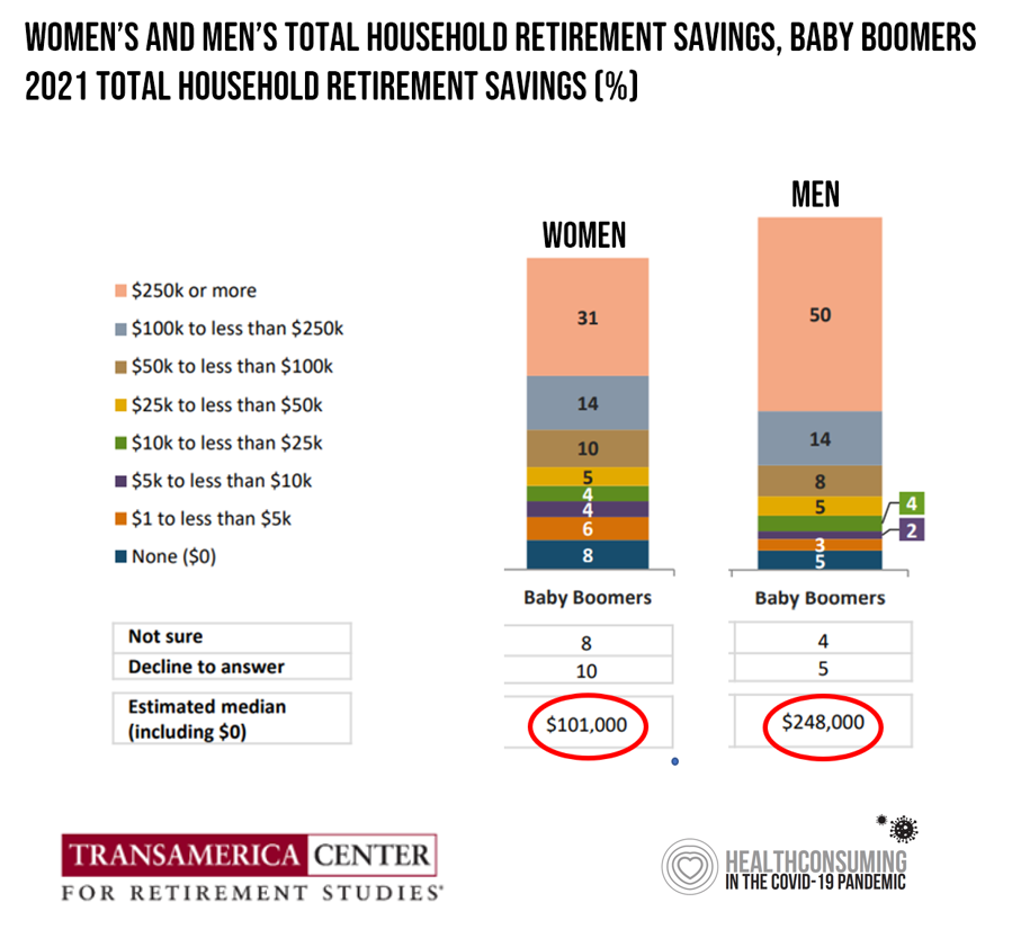
Due to gender pay gaps, time away from the workforce for raising children and caring for loved ones, women in the U.S. face a risky retirement outlook according to Emerging from the COVID-19 Pandemic: Women’s Health, Money, and Retirement Preparations from the Transamerica Center for Retirement Studies (TCRS). As Transamerica TCRS sums up the top-line, “Societal headwinds are undermining women’s retirement security.” Simply said, by the time a woman is looking to retire, she has saved less than one-half of the money her male counterpart has put away for aging after work-life. The
In Search of Clinical Effectiveness, But “Investment Exuberance?” Not So Much. Insights From FINN Partners and Galen Growth at HLTH 2022

While venture funding for digital health technology declined globally by 35% in the first three quarters of 2022 compared with 2021, this marks a “return to normal” based on the assessment in the Global State of Digital Health Report from FINN Partners and Galen Growth, published today and launched during the HLTH 2022 conference. The report analyzes data from over 12,000 digital health ventures tracked by Galen Growth’s HealthTech Alpha platform. The first chart illustrates the change in venture funding by therapeutic area, showing downturns in four of the five areas called
Thinking Value-Based Health Care at HLTH 2022 – A Call-to-Action

The cost of health insurance for a worker who buys into a health plan at work in 2022 reached $22,463 for their family. The average monthly mortgage payment was $1,759 in mid-2022. “When housing and health both rank as basic needs in Maslow’s hierarchy, what’s a health system to do?” I ask in an essay published today on Crossover Health’s website titled Value-Based Care: Driving a Social Contract of Trust and Health. The answer: embrace value-based care. Warren Buffett wrote Berkshire Hathaway shareholders in 2008, asserting that, “Price is what you pay. Value
$22,463 Can Get You a Year of College in Connecticut, a Round of Ref Work in the Stanley Cup Playoffs, or Health Benefits for a Worker’s Family
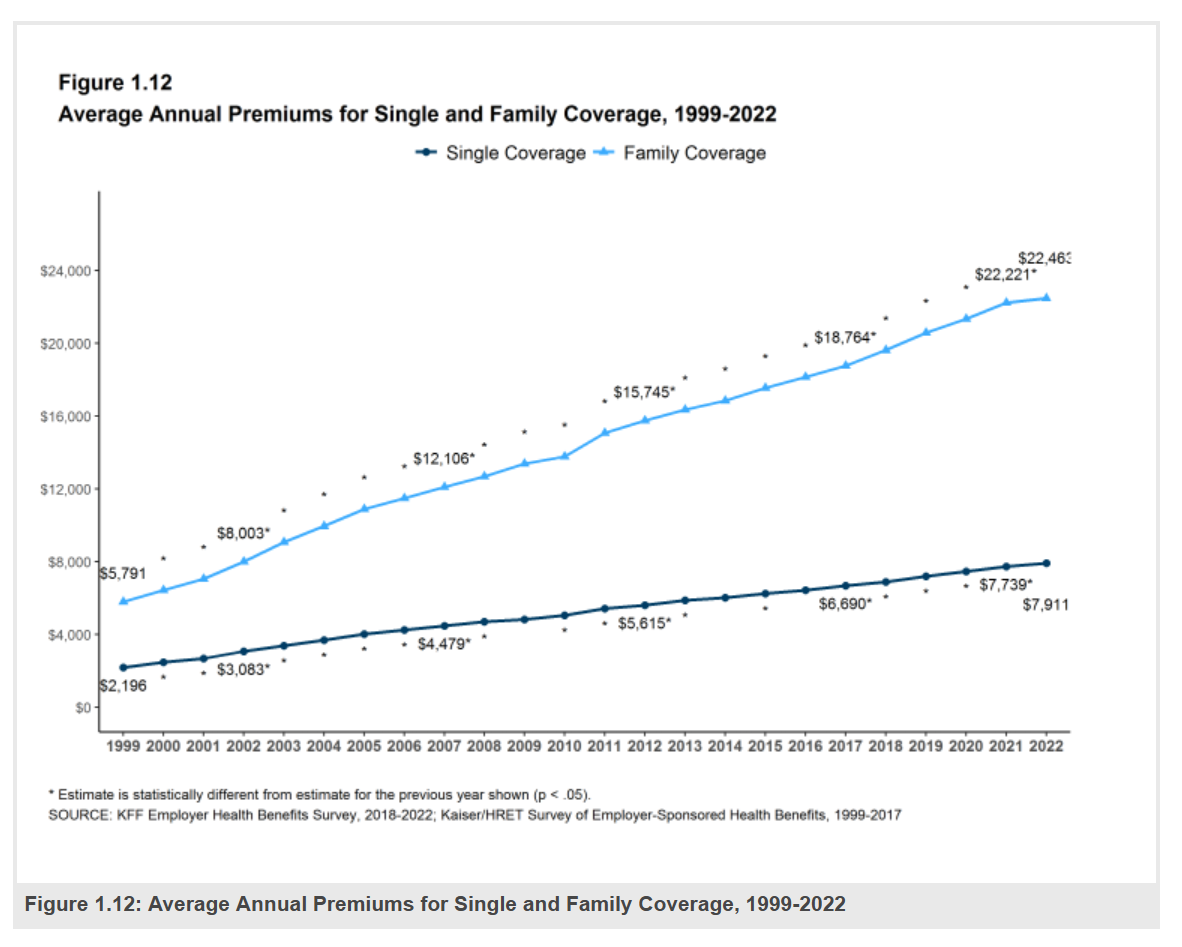
Employers covering health insurance for workers’ families will face insurance premiums reaching, on average, $22,463. That is roughly what a year at an independent college in Connecticut would cost, or a round of pay for a ref in the Stanley Cup playoffs. With that sticker-shock level of health plan costs, welcome to the 2022 Employer Health Benefits Survey from Kaiser Family Foundation, KFF’s annual study of employer-sponsored health care. Each year, KFF assembles data we use all year long for strategic and tactical planning in U.S. health care. This mega-study looks at
How Will the “New” Health Economy Fare in a Macro-Economic Downturn?

What happens to a health care ecosystem when the volume of patients and revenues they generate decline? Add to that scenario a growing consensus for a likely recession in 2023. How would that further impact the micro-economy of health care? A report from Trilliant on the 2022 Trends Shaping the Health Economy helps to inform our response to that question. Start with Sanjula Jain’s bottom-line: that every health care stakeholder will be impacted by reduced yield. That’s the fewer patients, less revenue prediction, based on Trilliant’s 13 trends re-shaping the U.S. health
Health in the 2022 U.S. Midterm Elections – Women, Prescription Drugs, and Who Shows Up to Vote

On Tuesday November 8, 2022, health and medical issues will be on many U.S. voters’ minds as they enter voting booths to select representatives for the House and the Senate, along with some states’ ballots addressing specific healthcare issues. Health policy experts from Manatt, Phelps & Phillips, AARP, and the United States of Care recently shared perspectives on the health care issues on voters’ and policy makers’ minds for the 2022 midterm elections. This post synthesizes their analyses as we lead up to what will be a pivotal election for Americans’ public health, individual well-being, and access to care.
The Patient as Prescription Drug Payer – The GoodRx Playbook

Patients have more financial skin-in-their-healthcare-games facing high-deductibles and direct out-of-pocket costs for medical bills…including prescription drugs. I collaborated with GoodRx on a “yellow paper” discussing The Health Consumers as Payer, with implications and calls-to-action for pharma and life science companies. You can download the paper at this link. The report is intended to be a playbook for understanding patients’ growing role as consumers and health care payers, providing insights into peoples’ home economic mindsets and how these impact a patient’s adherence to medication based on cost and perceived value. With inflation facing household
Health Care Costs Are a Driver of Health Across All of America – Especially for Women
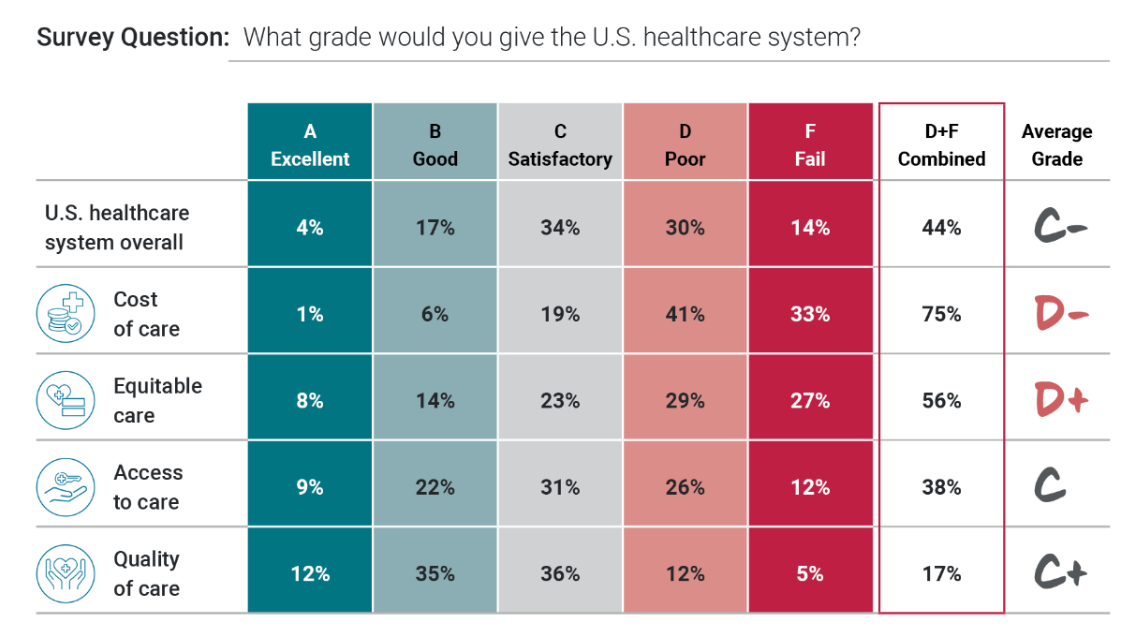
Three in four people in America grade health care costs a #fail, at grade “D” or lower. This is true across all income categories, from those earning under $24,000 a year to the well-off raking in $180K or more, we learn in Gallup’s poll conducted with West Health, finding that Majorities of people rank cost and equity of U.S. healthcare negatively. Entering the fourth quarter of 2022, several studies were published in the past week which reinforce the reality that Americans are facing high health care costs, preventing many from seeking necessary medical services, and hitting under-served health citizens even harder
Connected Wellness Growing As Consumers Face Tighter Home Economics

“Consumers are using the Internet to take their health into their own hands,” at least for 1 in 2 U.S. consumers engaging in some sort of preventive health care activity online in mid-2022. The new report on Connected Wellness from PYMNTS and Care Credit profiles American health consumers’ use of digital tools for health care promotion and disease prevention. The bottom-line here is that the most connected 10% of consumers were 1.65 times more likely to be engaged in preventive digital health activities than the average person. Peoples’ engagement with digital health
Health Consumers Want More Support from Healthcare – At Retail Experience Levels

As consumers learn to appreciate and patronize retail touchpoints, entertainment, and financial management via omnichannel platforms, patients and health citizens are seeking more enchanting service levels for their health care. The latest view on patient preferences from Kaufman Hall is out in the firm’s annual 2022 State of the Healthcare Consumer Report. Every year, this go-to report divines how U.S. patients continue to morph into health/care consumers. This year’s top-line is that peoples’ expectations of health care service providers exceed what those providers, health plans, and suppliers (like pharma) are serving up —
Remember the Social Determinants of Health When Prescribing Drugs
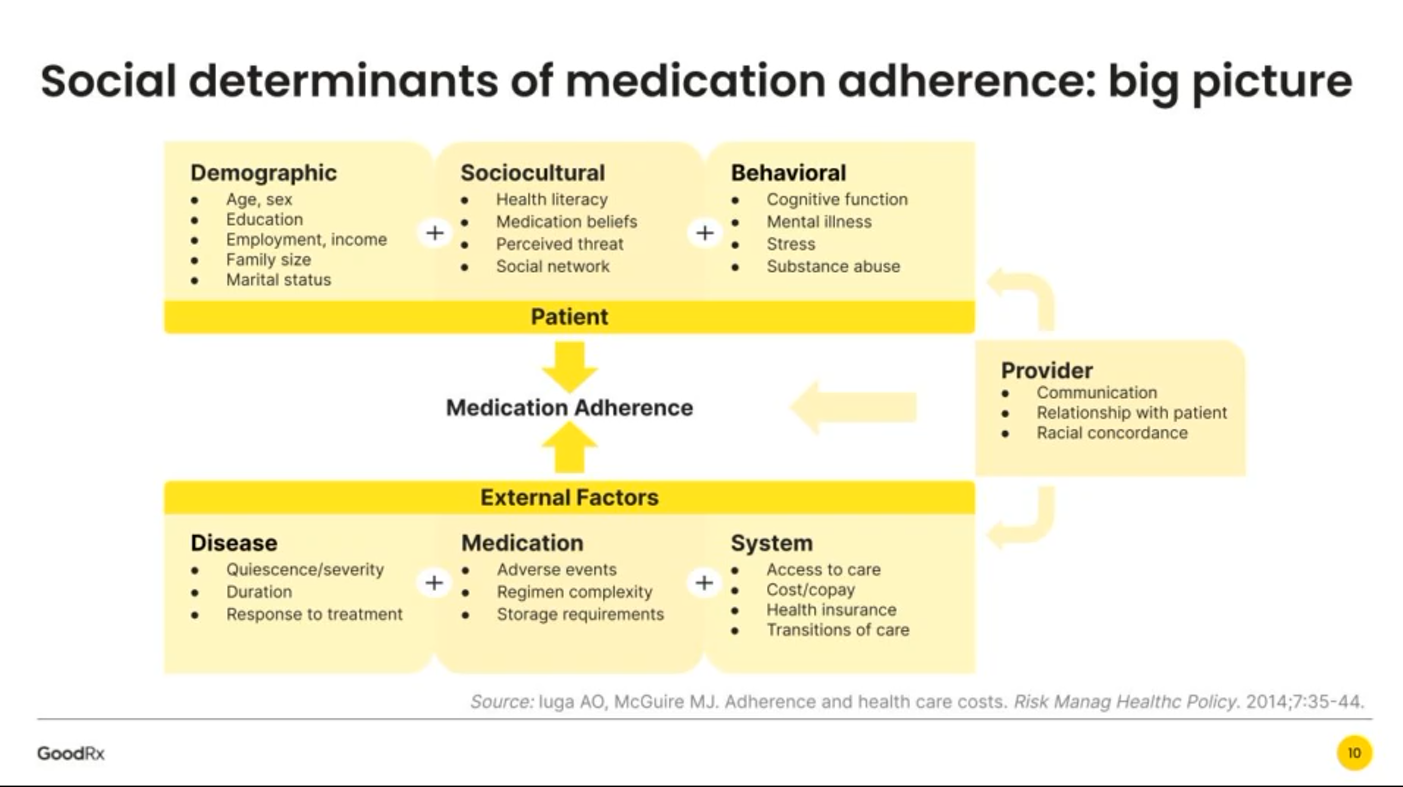
Thinking about the social determinants of prescription drugs, how people take medicines in real life in my latest post in Medecision’s Liberate Health blog. I had one of those special lightbulb moments when listening to Mauricio Gonzalez-Arias, M.D. of NYC Health + Hospitals and Suvida Healthcare discussing medication adherence and what prevents us from taking our meds as prescribed. His discussion on social determinants’ role in shaping our relationship with prescriptions was powerful, and the jumping off point for this essay. Medication adherence is a challenge that fiscally costs the
The Patient As the Payer: Self-Pay, Bad Debt, and the Erosion of Hospital Finances
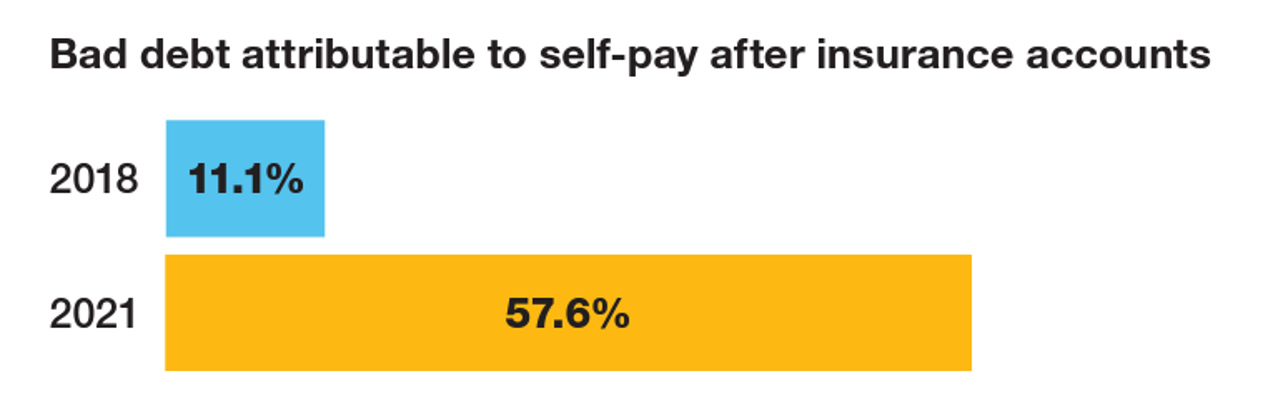
“The odds are against hospitals collecting patient balances greater than $7,500,” the report analyzing Hospital collection rates for self-pay patient accounts from Crowe concludes. Crowe benchmarked data from 1,600 hospitals and over 100,00 physicians in the U.S. to reveal trends on health care providers’ ability to collect patient service revenue. And bad debt — write-offs that come out of uncollected patient bill balances after “significant collection efforts” by hospitals and doctors — is challenging their already-thin or negative financial margins. The first chart quantifies that bad debt attributable to patients’ self-pay payments
Gallup Reveals Americans’ Views on Industry Are the Lowest Since 2008 – Implications for Healthcare and Pharma
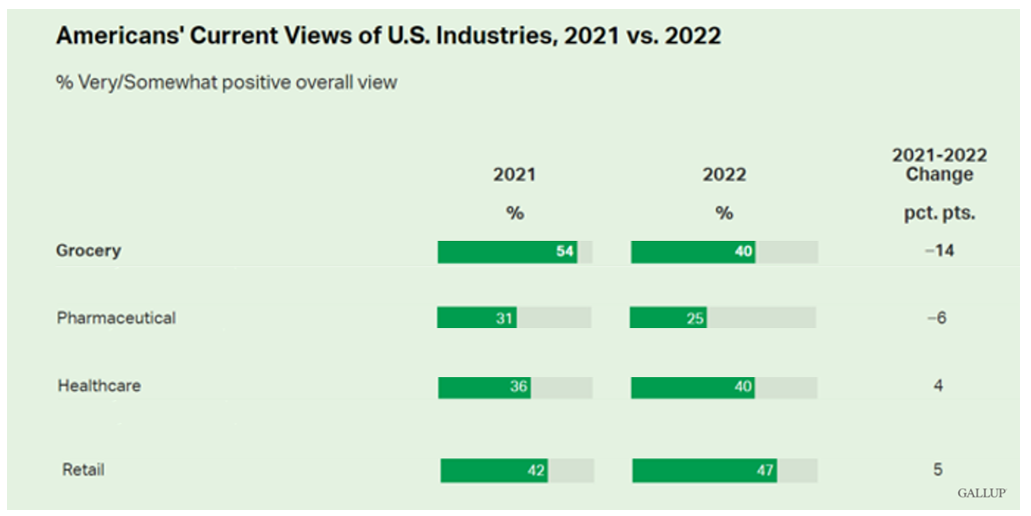
Americans’ positive views of 25 industries in the U.S. have declined in the past year. In their latest look into consumers’ views on business in America, Gallup found that peoples’ ratings on business fell to their lowest ratings overall since 2008. Peoples’ highest ratings of industry in American occurred in 2017 when nearly 50% of people gave business a very or somewhat positive grade. The year-on-year decline from 2021 find oil and gas at the lowest level of positivity, advertising/PR, legal, the Federal government, and pharma at the bottom of the ratings.
Most Consumers Are Health and Wellness Consumers Even in Hard Financial Times, Accenture Finds
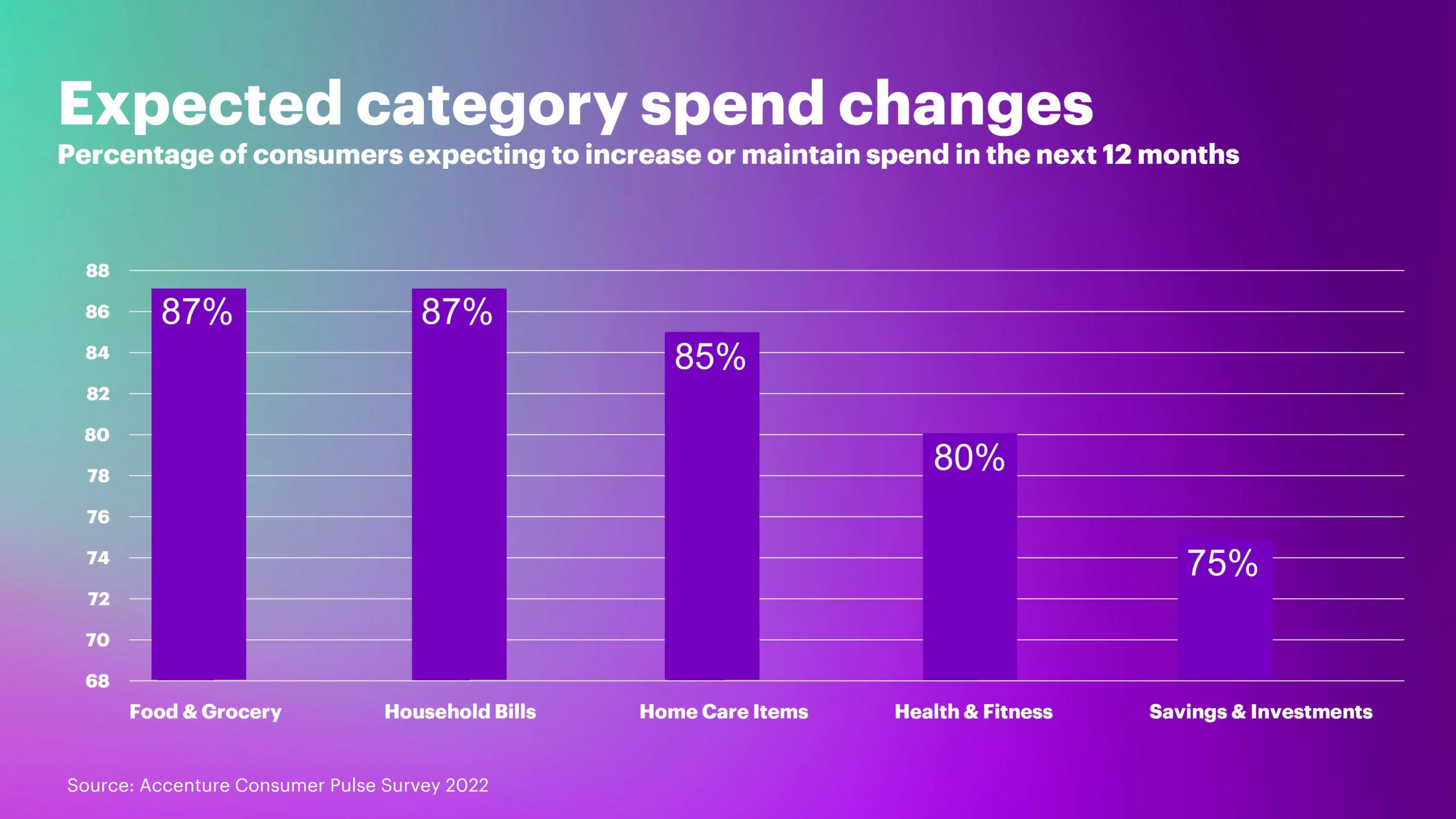
Consumers consider health and well-being as an “essential” household spending category based on new research from Accenture. Accenture polled over 11,000 consumers in 17 countries, considering how people are faring amid “widespread uncertainty and personal financial strains,” in the firm’s words. While two in three consumers feel financially stressed, 4 in 5 intend to grow or hold their personal spending on health and fitness steady in the next year. The first chart graphs data from Accenture’s global survey. In the U.S., more granularly, 26% of consumers intend to increase spending on health and wellness





 Interviewed live on BNN Bloomberg (Canada) on the market for GLP-1 drugs for weight loss and their impact on both the health care system and consumer goods and services -- notably, food, nutrition, retail health, gyms, and other sectors.
Interviewed live on BNN Bloomberg (Canada) on the market for GLP-1 drugs for weight loss and their impact on both the health care system and consumer goods and services -- notably, food, nutrition, retail health, gyms, and other sectors. Thank you, Feedspot, for
Thank you, Feedspot, for  As you may know, I have been splitting work- and living-time between the U.S. and the E.U., most recently living in and working from Brussels. In the month of September 2024, I'll be splitting time between London and other parts of the U.K., and Italy where I'll be working with clients on consumer health, self-care and home care focused on food-as-medicine, digital health, business and scenario planning for the future...
As you may know, I have been splitting work- and living-time between the U.S. and the E.U., most recently living in and working from Brussels. In the month of September 2024, I'll be splitting time between London and other parts of the U.K., and Italy where I'll be working with clients on consumer health, self-care and home care focused on food-as-medicine, digital health, business and scenario planning for the future...